What Is DAN?
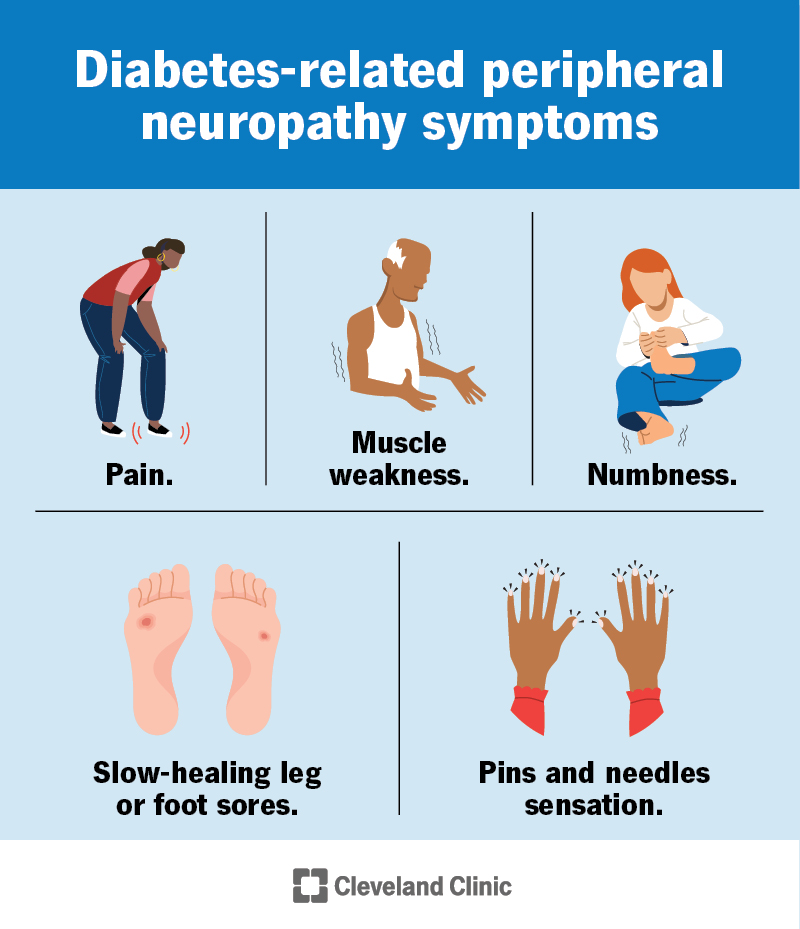
In plain English, DAN is a type of nerve damage that hits the part of the nervous system that automatically controls things you dont think about: heart rate, digestion, bladder function, sweating, and even eye response. Its different from the tingly peripheral neuropathy that usually shows up in your feet and hands. While peripheral neuropathy is like a staticfilled telephone line, DAN is more like a broken thermostatyour bodys internal regulations start to glitch.
Definition and Scope
Medical researchers define autonomic neuropathy as a dysfunction of the autonomic nervous system caused by sustained high blood glucose. It can appear after 1015 years of type2 diabetes, but it sometimes shows up earlier, especially if blood sugar control has been inconsistent.
Why It Matters
These symptoms arent just annoying; they can lead to serious complications like sudden fainting, dangerous drops in blood pressure, or even lifethreatening heart rhythm problems. Knowing the early signs gives you a chance to intervene before the issues spiral.
Core Symptom Checklist
Lets get straight to the heart of the matter. Below is a quickreference table that lists the systems affected, typical symptoms, and a reallife example you might recognize.
| System | Typical Symptom | Everyday Example |
|---|---|---|
| Cardiac | Resting tachycardia, orthostatic hypotension | My heart feels like its sprinting even when Im just watching TV. |
| Gastrointestinal | Constipation, gastroparesis, nausea | Food sits in my stomach for hours; I feel full after just a bite. |
| Genitourinary | Erectile dysfunction, urinary urgency or retention | I cant finish a bathroom break without feeling an urgent need to go again. |
| Sweat & Skin | Too much or too little sweating | My hands are either constantly clammy or completely dry. |
| Vision | Abnormal pupil response, dry eyes | Bright lights glare and my eyes feel gritty. |
What Are the First Signs?
Often the first clue is a subtle dizziness when you stand up too quickly (orthostatic hypotension). You might dismiss it as just being tired, but repeated episodes are a red flag. Another early signal is a sudden, unexplained change in bowel habitsespecially persistent constipation that doesnt improve with diet.
How Long Can You Live With It?
Living with autonomic neuropathy doesnt necessarily mean a shortened lifespan. With proper management, many people maintain a good quality of life for decades. The key is early detection and consistent care. Ignoring symptoms, however, can increase the risk of cardiovascular events and hospitalizations, which can impact longevity.
How Is Diagnosed?
Getting a definitive diagnosis usually involves a combination of clinical history, simple bedside tests, and sometimes specialized studies. Your doctor will want to rule out other causes first, so be ready to share every odd feeling youve noticed.
Standard Tests
- Heartrate variability (HRV): Measures how your heart rate changes with breathing. Low variability can hint at cardiac autonomic neuropathy.
- Tilttable test: You lie on a table that tilts upward; blood pressure and heart rate are monitored for abnormal drops.
- Gastric emptying study: A small amount of radioactive material tracks how quickly food leaves your stomach.
- Sweatspot test: A small chemical patch measures sweat production on your forearm.
StepbyStep Office Visit
When you walk into the clinic, expect a quick blood pressure check while youre lying down, then again after you stand up. The doctor may ask you to sip a glass of water and measure your heart rate before and after, to spot any irregularities. If something looks off, theyll likely refer you to a neurologist or a gastroenterologist for the more specialized tests mentioned above.
How Is Autonomic Neuropathy Diagnosed?
According to a review by the , diagnosis hinges on symptom patterns plus objective test results. No single test can prove DAN, but a combination that matches your clinical picture is usually enough for a solid diagnosis.
Managing and Treating
Think of treatment as a threepart orchestra: lifestyle changes, medication, and supportive therapies. Each instrument matters, and together they can bring your body back into a smoother rhythm.
Lifestyle First
BloodSugar Control: Tight glycemic management remains the cornerstone. Even modest reductions in HbA1c can slow nerve damage progression.
Balanced Diet: Small, frequent meals help prevent gastroparesis spikes. Focus on fiber, lean protein, and lowglycemic carbsfoods such as strawberries can be part of a lowglycemic approach to help manage overall blood glucose; for more on how specific foods affect sugars see strawberries blood sugar. Stay hydrateddehydration worsens bloodpressure swings.
Exercise: Lowimpact activitieswalking, swimming, or gentle yogaimprove circulation and autonomic tone. Start slow; even a 10minute stroll each day can make a difference.
Medication Toolbox
- Midodrine: Raises blood pressure in people with orthostatic hypotension.
- Prokinetics (e.g., metoclopramide): Speed up gastric emptying for gastroparesis.
- PDE5 inhibitors: Help with erectile dysfunction caused by autonomic dysfunction.
- Fludrocortisone: Increases blood volume, useful for chronic low blood pressure.
Always discuss medication side effects with your provider. Some drugs can interact with insulin or other diabetes meds, so a coordinated approach is essential.
Can Diabetic Neuropathy Be Reversed?
Current research suggests that while we cant fully reverse longstanding nerve damage, we can halt its progression and even improve some symptoms. A 2023 study presented at the American Diabetes Association conference showed that intensive glucose control combined with lifestyle interventions led to modest but meaningful improvements in autonomic function scores. The takeaway? Your actions today can still rewrite tomorrows health story.
Complementary Approaches
Physical therapy can teach you safe ways to improve balance and reduce fall risk. Stressreduction techniqueslike mindfulness, breathing exercises, or even a short daily meditationcan calm the autonomic system and help stabilize heart rate.
Frequent Patient Questions
What Are the 5 Main Symptoms of Diabetic Neuropathy?
While diabetic neuropathy broadly covers many nerve issues, the five hallmark signs often include:
- Persistent numbness or tingling in feet/hands.
- Sharp, burning pain that worsens at night.
- Loss of balance or frequent falls.
- Digestive disturbances (constipation or diarrhea).
- Changes in sweating or temperature regulation.
When any of these overlap with autonomic signs, its a strong hint to explore DAN further.
Gastrointestinal Autonomic Neuropathy Symptoms
Beyond the usual constipation, you might experience early satiety (feeling full after a few bites), unexplained weight loss, or a bloat sensation that doesnt go away. Some people describe it as a slowmotion after meals, as if the food is moving through a tunnel clogged with traffic.
Cardiac Autonomic Neuropathy Symptoms
Sudden heart palpitations, an unusually high resting heart rate, or a drop in blood pressure when you stand up are classic red flags. If you ever feel lightheaded after sitting for a while and then standing, thats orthostatic hypotension screaming for attention.
How Is Autonomic Neuropathy Diagnosed?
As mentioned earlier, a mix of HRV testing, tilttable studies, and symptom mapping usually does the trick. The emphasizes that a thorough clinical exam paired with targeted tests is the gold standard.
Autonomic Neuropathy Treatment
Treatment is personalized. For some, adjusting insulin timing and adding a lowdose midodrine brings blood pressure back to a safe range. For others, the key lies in dietary tweaks and a consistent exercise routine. The common thread? Ongoing communication with your healthcare team.
Balancing Benefits Risks
Understanding both sides of the coin helps you make informed choices. The upside of early detection is clear: you can prevent emergencies, keep your energy levels steadier, and reduce the need for hospital visits. The downside of ignoring symptoms? More frequent falls, severe dehydration from gastrointestinal slowdown, or even heart rhythm disturbances that could land you in the ER.
Benefits of Early Detection
Studies show that patients who receive a diagnosis within the first year of symptom onset have a 30% lower rate of cardiovascular complications over five years. Early interventions also mean fewer medication side effects because you can start with lifestyle strategies.
Risks of Ignoring Symptoms
When autonomic nerves malfunction, your body cant regulate temperature, blood pressure, or digestion properly. This can lead to dangerous scenarios: a fainting episode while driving, severe constipation causing bowel obstruction, or uncontrolled bloodpressure spikes that increase stroke risk.
Cost Comparison (Quick Look)
Routine screening (a few office visits and basic tests) typically costs a few hundred dollars annually. In contrast, an emergency admission for a fainting spell or severe gastroparesis can run into thousands. Investing a little time and money now can save big headachesand billslater.
Quick Takeaway Checklist
- Be alert for a racing heart at rest, dizziness on standing, or persistent constipation.
- Schedule a checkup if any of the core symptoms appear; early testing is key.
- Maintain tight bloodsugar controlsmall HbA1c drops make a huge difference.
- Adopt a balanced diet with frequent, small meals and stay wellhydrated.
- Add gentle exercise and stressrelief practices to your daily routine.
- Talk to your doctor about medication options if lifestyle changes arent enough.
- Stay connected with a diabetes support communityshared stories help you feel less alone.
Living with diabetic autonomic neuropathy isnt a solo journey. By recognizing the signs, seeking the right diagnosis, and embracing a proactive treatment plan, you can keep your bodys automatic systems humming smoothly. Got questions or personal experiences to share? Drop a comment belowlets keep the conversation going. Your voice might be the one that helps someone else feel heard and empowered.
FAQs
What are the most common diabetic autonomic neuropathy symptoms?
Typical signs include a racing heart at rest, dizziness when standing (orthostatic hypotension), persistent constipation or gastroparesis, abnormal sweating, and urinary problems.
How can I tell if my dizziness is related to autonomic neuropathy?
If you feel light‑headed or faint shortly after standing up, especially if it happens repeatedly, it may be orthostatic hypotension—a common autonomic symptom in diabetes.
Is there a simple test doctors use to diagnose autonomic neuropathy?
Doctors often start with heart‑rate variability and blood‑pressure measurements while you change positions; more detailed studies like tilt‑table testing or gastric emptying scans may follow.
Can lifestyle changes improve diabetic autonomic neuropathy symptoms?
Yes. Tight blood‑sugar control, small frequent meals, regular low‑impact exercise, and staying well‑hydrated can slow progression and relieve many symptoms.
Are there medications that help with the autonomic effects of diabetes?
Medications such as midodrine for low blood pressure, prokinetics for gastroparesis, and PDE‑5 inhibitors for erectile dysfunction are commonly prescribed when lifestyle measures aren’t enough.