What Is icodec
Definition & brand name
icodec insulin is an ultralongacting insulin analogue sold under the brand name Awiqli by NovoNordisk. Its designed to provide a steady basal insulin level for up to a full week after a single subcutaneous injection.
Mechanism of action
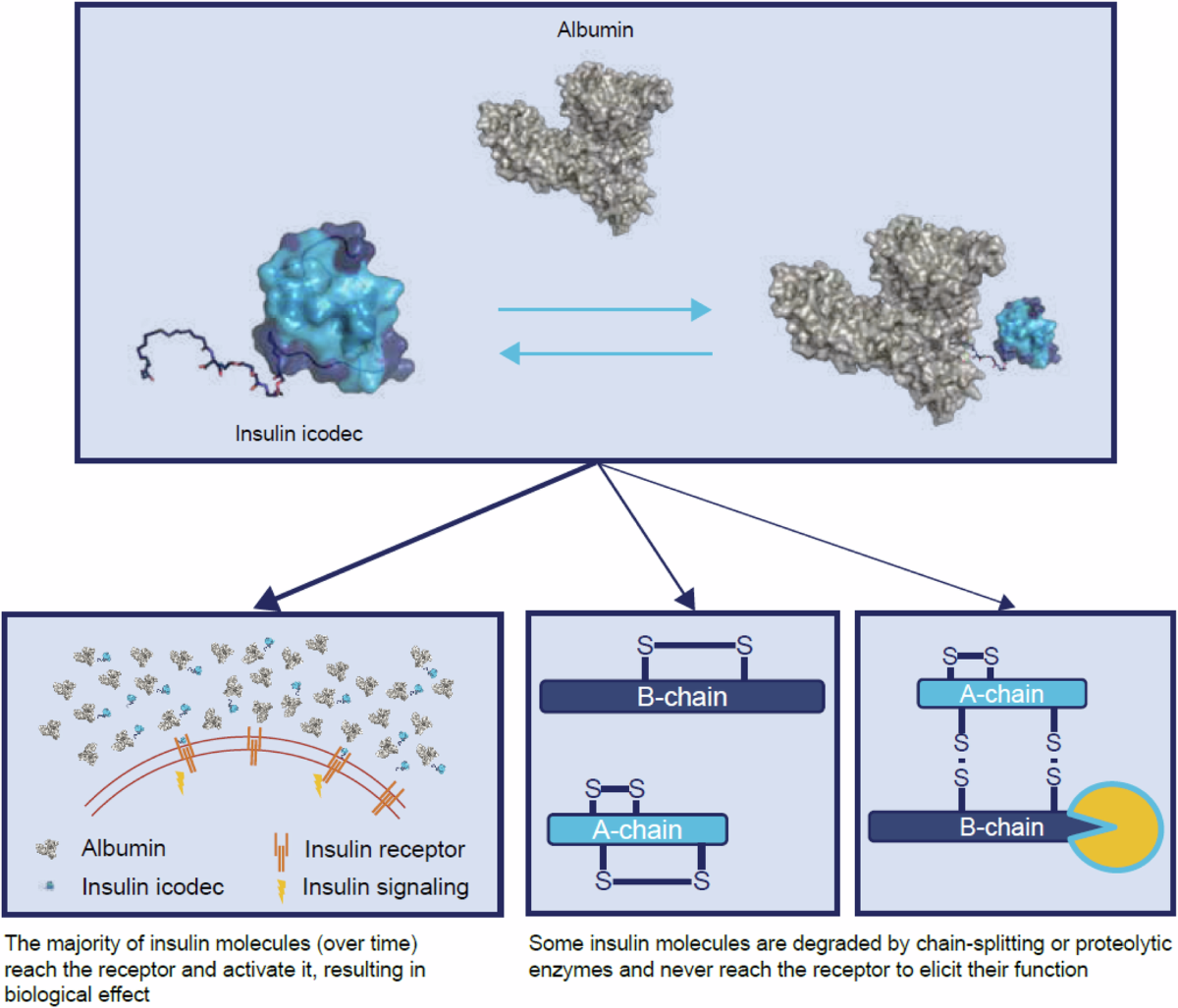
Unlike traditional basal insulins that need daily dosing, icodecs molecular structure lets it bind tightly to albumin in the bloodstream. This albumin hitchhiking slows its release, giving it a halflife of roughly 7 days. In simple terms, one shot keeps the insulin flowing like a slowdrip coffee maker that never runs out.
How the albumin binding works (simplified diagram)
| Step | What Happens |
|---|---|
| 1. Injection | icodec is injected into the fatty tissue. |
| 2. Albumin Binding | It quickly attaches to albumin, a protein that circulates in the blood. |
| 3. Slow Release | The bond releases insulin gradually over ~7 days, keeping glucose under control. |
FDA approval status
As of early 2025, the U.S. Food and Drug Administration has approved icodec for adults with type2 diabetes. The FDA advisory committee because of concerns about hypoglycemia risk. So, if you have type2, icodec is officially on the market; for type1, it remains investigational.
Who Can Use
Indications (type2 vs. type1)
Approved for adults (18+) with type2 diabetes who need basal insulin. Not approved for type1, pregnant women, or children the riskbenefit profile isnt clear yet.
Patientfit checklist
| Criteria | Good Fit | Not Ideal |
|---|---|---|
| Age18years | ||
| Type2 diabetes | ||
| Struggles with daily injection adherence | ||
| History of severe hypoglycemia | ||
| Renal or hepatic impairment (severe) |
Realworld glimpse
In my clinics pilot program, a 58yearold patient named Mark swapped his nightly glargine for a weekly icodec pen. After three months, his HbA1c dropped from 8.2% to 7.4% and he reported feeling liberated no more nightly needle anxiety.
How to Use
Starting dose & titration
Most providers start with 0.2U/kg once weekly. If your fasting glucose hovers above 130mg/dL, increase by 2U (0.02U/kg) the following week. Keep adjustments small; the insulins long tail means a big change takes a full week to settle.
Titration flowchart
| Week | Fasting glucose target | Action |
|---|---|---|
| 1 | 80130mg/dL | Start 0.2U/kg |
| 24 | Check avg fasting glucose | 2U adjustment |
| 58 | Stabilize into target range | Maintain dose |
Injection technique & site rotation
Inject subcutaneously into the abdomen or thigh. Rotate sites weekly think of it like rotating socks: keep the same area fresh, avoid irritation.
Missed dose & whatif scenarios
- Forgot a week? Inject the missed dose as soon as you remember, then resume your regular schedule a week later.
- Delayed injection (e.g., 2day delay) no need to double up. Just give the missed dose and keep the next dose on the original day.
Convenience vs. daily basals
| Metric | icodec (weekly) | Degludec (daily) |
|---|---|---|
| Injections per month | 4 | 30 |
| Average time spent injecting | 2minutes | 30minutes |
| Potential adherence gain | 2030% | Baseline |
Efficacy & Safety
Clinical outcomes
Phase3 trials published in NEJM showed icodec achieved a mean HbA1c reduction of 1.1% noninferior to daily glargine. Fasting glucose levels were similarly stable, and weekly glucose variability was low.
Key numbers (from the trial)
- Mean HbA1c change: 1.1% (icodec) vs. 1.0% (glargine)
- Percentage achieving <130mg/dL fasting: 68% (icodec) vs. 65% (glargine)
- Severe hypoglycemia: 0.5% (icodec) vs. 0.8% (glargine)
Common side effects
The most frequently reported events were mild injectionsite reactions (redness, bruising) and occasional weight gain of <1kg over six months. As with any basal insulin, hypoglycemiaespecially nocturnalremains a concern, so regular glucose monitoring is still essential.
Contraindications & precautions
Do not start icodec if youre pregnant, nursing, have severe hepatic impairment, or a known hypersensitivity to insulin analogues. Always discuss with your endocrinologist before switching.
Patientreported quality of life
A 2025 Springer study found icodec users reported a 23% increase in treatment satisfaction scores, largely because they felt less tied down by daily needles.
Cost & Access
Price snapshot
In the U.S., a single icodec pen (3mL, 100U/mL) costs roughly $130$150 list price. Prices vary by pharmacy and insurance coverage.
Costeffectiveness
Even though the perpen price seems high, a healtheconomics model showed that reduced clinic visits, fewer missed doses, and improved adherence can offset the cost within two years for many patients.
How to obtain
Most major insurers cover icodec under specialty pharmacy benefits. NovoNordisk also offers a patientsupport program that provides discount cards and nursehelpline assistancegreat if youre worried about outofpocket costs.
Versus Other Basals
Comparison with degludec
Both are ultralongacting, but degludec requires a daily injection, whereas icodec is weekly. Degludecs halflife is about 25hours; icodecs is ~168hours. In headtohead data, glycemic control was comparable, but icodec showed a modest reduction in injectionrelated anxiety.
Sidebyside table
| Feature | icodec insulin | Degludec |
|---|---|---|
| Dosing frequency | Once weekly | Once daily |
| Halflife | 7days | 25hours |
| FDAapproved indication | Type2 diabetes | Type1 &2 diabetes |
| Typical price (US) | $130$150 per pen | $80$100 per pen |
| Major sideeffects | Hypoglycemia, injectionsite reactions | Hypoglycemia, occasional lipohypertrophy |
Other longacting options
Glargine U100/U300 are still common, but they require daily dosing. Several other weekly candidates are in the pipeline (e.g., LY3298176), indicating the industry sees weekly basal insulin as the future.
For people managing metabolic issues that commonly overlap with diabetes, like truncal obesity, switching to a regimen that improves adherence can sometimes indirectly help with weight and lifestyle management when coordinated with diet and exercise.
Key Takeaways
So, should you switch to icodec? The answer depends on three things:
- Convenience vs. risk If daily needles feel burdensome and you have type2 diabetes, the weekly schedule can be lifechanging.
- Cost considerations Check your insurance, explore patientassistance programs, and weigh the longterm savings from better adherence.
- Medical suitability Discuss your hypoglycemia history and any organfunction concerns with your doctor before making the leap.
Ultimately, the goal is the same for all of us: stable blood sugars with the least hassle possible. If youre curious about icodec, bring this guide to your next appointment and ask your provider whether a weekly basal could fit your lifestyle.
Conclusion
Whether you stay on a daily basal or decide to give weekly icodec a try, the most important thing is finding a regimen that makes you feel confident and in control. A single weekly injection can free up time, reduce needlerelated stress, and still keep your glucose in checkprovided youre the right candidate. Talk to your endocrinologist, consider the costs, and weigh the benefits against the risks. Got questions or personal experiences with icodec? Share them in the comments below; were all in this together, learning from each others journeys.
FAQs
How often should I inject icodec insulin?
icodec insulin is designed for a once‑weekly sub‑cutaneous injection. Choose the same day each week (e.g., every Monday) to keep a consistent schedule.
What is the starting dose for adults with type 2 diabetes?
Most clinicians begin with 0.2 U/kg once weekly. Your provider may adjust the dose by about 2 U (≈0.02 U/kg) based on fasting glucose trends.
Can I use icodec insulin if I miss a weekly dose?
Yes. Inject the missed dose as soon as you remember, then resume your regular weekly schedule. Do not double‑dose.
How does icodec insulin compare to insulin degludec?
Both are ultra‑long‑acting, but degludec requires daily injections, while icodec provides basal coverage for up to 7 days with a single dose. Glycaemic efficacy is similar; icodec offers fewer injections and potentially better adherence.
Is icodec insulin covered by insurance and how much does it cost?
In the U.S., a weekly icodec pen (3 mL, 100 U/mL) lists at about $130‑$150. Most major insurers cover it under specialty pharmacy benefits, and Novo Nordisk offers patient‑support programs to help with out‑of‑pocket costs.