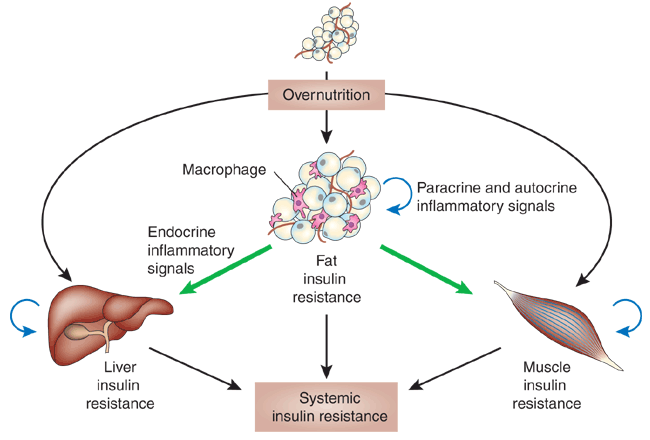
Preventing stress-induced insulin resistance requires understanding how stress affects glucose metabolism. When under stress, the body releases cortisol and adrenaline, which can elevate blood sugar levels by reducing insulin's ability to move glucose into cells. This can lead to
diabetic autonomic neuropathy and other complications if not managed properly. Managing stress can help mitigate these effects; techniques like mindfulness-based stress reduction have shown significant benefits in reducing fasting glucose levels, which is crucial for people with conditions like
diabetic nerve damage.To manage stress-induced diabetes, adopting a lifestyle that includes regular exercise, balanced nutrition, and stress-reduction techniques is essential. High-intensity interval training (HIIT) and steady-state cardio can improve insulin sensitivity, while focusing on low-glycemic, high-fiber foods can help stabilize blood sugar levels. Additionally, incorporating stress-management tools like 5-2-5 breathing and micro-walks can help reduce cortisol spikes. These habits, combined with a focus on nutrition and activity, can create a feedback loop that reinforces overall health.For those with
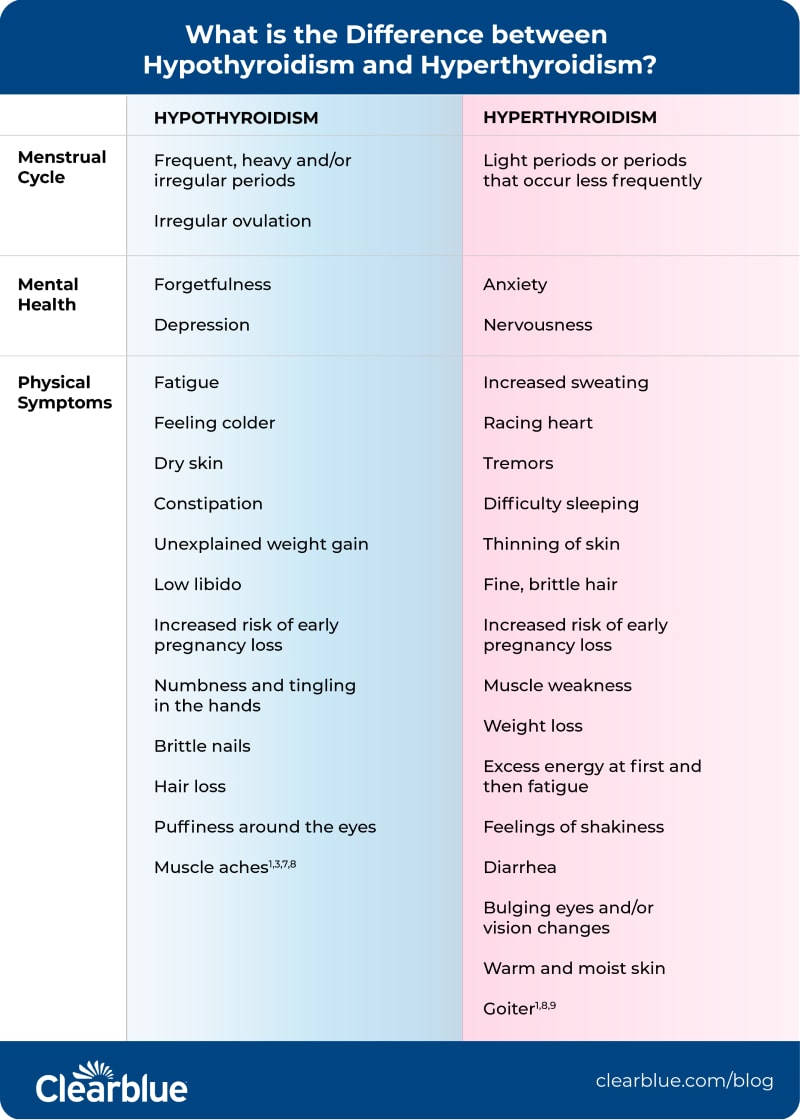
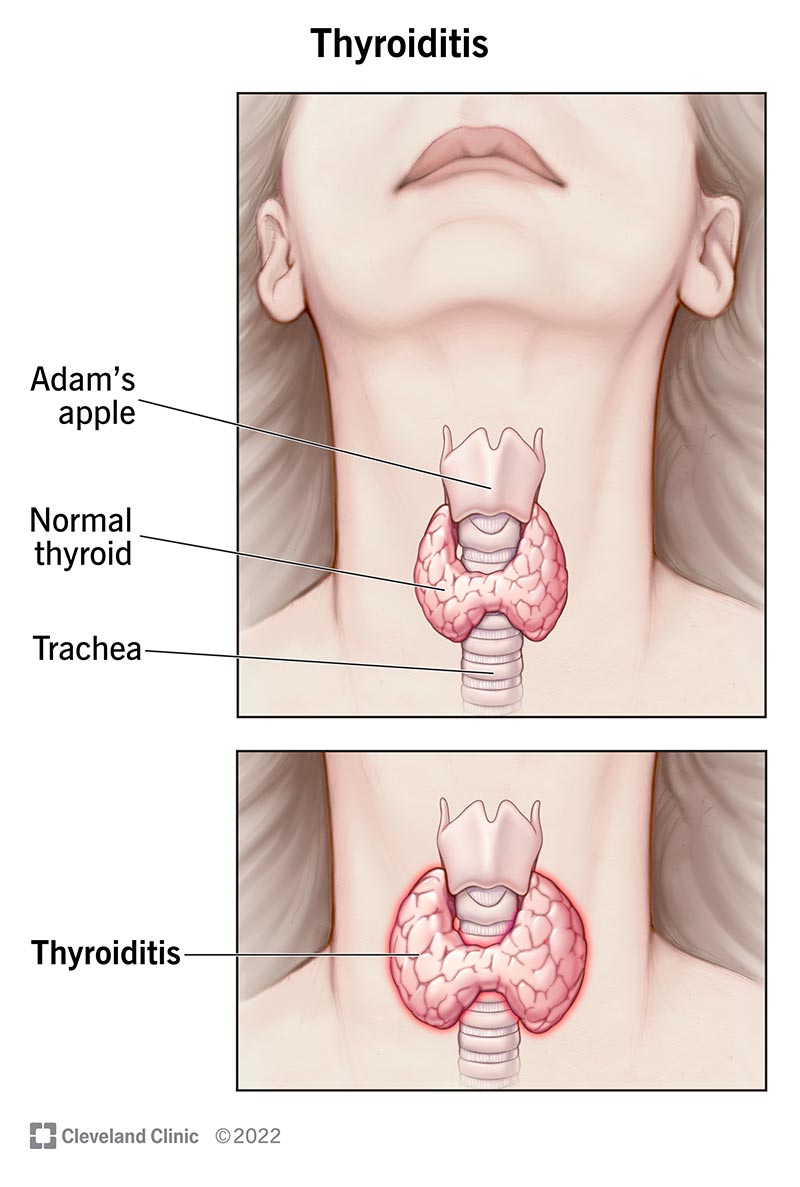
primary hypothyroidism, managing stress is also important because it can exacerbate symptoms. Hypothyroidism is treated with hormone replacement therapy, typically involving medications like levothyroxine, but stress management remains crucial for overall well-being. Understanding the differences between treatments, such as comparing
Armour vs levothyroxine, can help individuals make informed decisions about their care and manage their condition more effectively. Incorporating stress-reduction techniques into daily routines can significantly improve insulin sensitivity and overall health, reducing the risk of complications associated with both diabetes and hypothyroidism. Regular exercise and a balanced diet are key components of this approach, helping to maintain stable blood sugar levels and prevent long-term health issues. If stress persists, it may be beneficial to explore additional stress management techniques like cognitive behavioral therapy (CBT) for stress.
FAQs
How does stress cause blood sugar to rise?
Stress releases cortisol and adrenaline, which signal the liver to release more glucose and make muscle cells less responsive to insulin, leading to higher blood sugar.
Can stress raise blood sugar in type 1 diabetes?
Yes. Even with injected insulin, cortisol can temporarily overwhelm insulin action, causing rapid spikes in glucose levels.
What are quick ways to lower stress‑induced glucose spikes?
Practice 5‑2‑5 breathing, take micro‑walks, stay hydrated, and add a short mindfulness or relaxation break to reduce cortisol within minutes.
How much can chronic stress increase A1C?
Long‑term high stress can raise HbA1c by about 0.3‑0.5 %, reflecting a measurable increase in average blood glucose over months.
When should I see a doctor for stress‑related high blood sugar?
If fasting glucose stays above 100 mg/dL or you notice persistent spikes despite lifestyle changes, schedule a medical evaluation for possible treatment.