Wondering why that stubborn morning neck stiffness feels different for you than it does for the guys you know? Youre not alone. Most women with spondylitis notice a mix of back, hip, and even peripheral joint pain that can creep up before you even have your coffee. The good news? Theres a clear, stepbystep plan that blends medicine, movement, and mindful lifestyle tweaks to keep the pain at bay and protect your spine for the long haul.
Below, Ill walk you through everything you need to knowwhat to look for, which treatments actually work, and how to stay in control of your health without feeling overwhelmed. Think of it as a friendly chat over tea, with a sprinkle of science to back it up.
Female Spondylitis Symptoms
What symptoms appear most often in women?
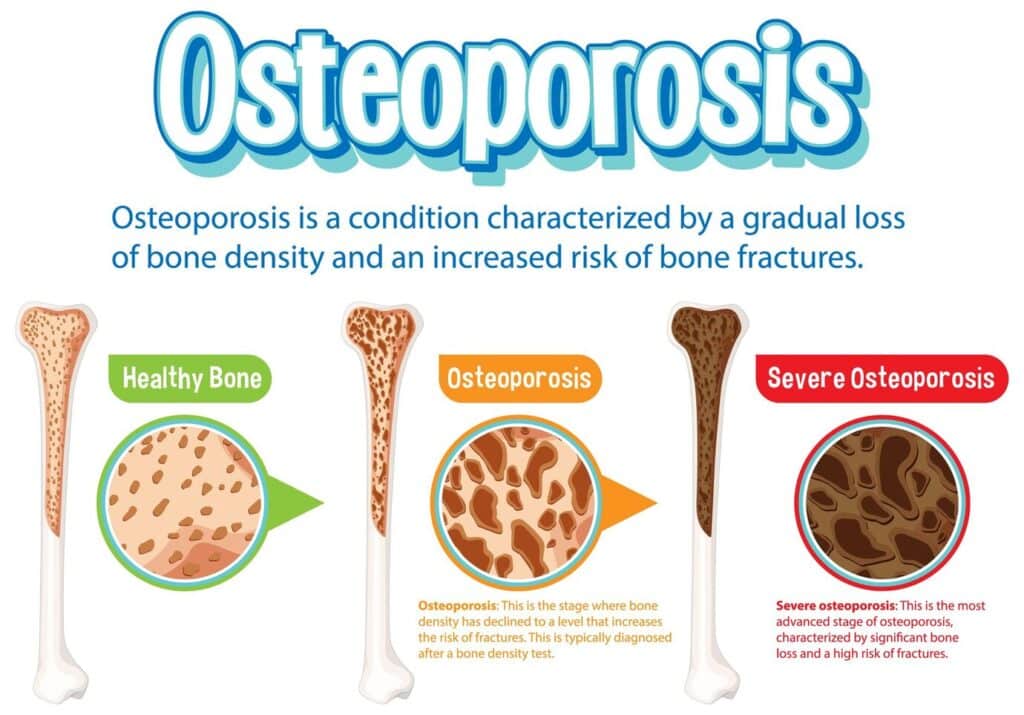
While spondylitis can affect anyone, women tend to experience a slightly different symptom pattern. Common signs include:
- Persistent lowerback or hip pain that worsens after periods of inactivity.
- Morning stiffness lasting more than 30minutes, often easing after gentle movement.
- Peripheral joint involvementknees, shoulders, or even the elbows may feel achy.
- Fatigue that feels more brainfog than just tiredness, sometimes accompanied by mood swings.
These clues are especially useful because they differ from the classic young male with severe back pain stereotype that many textbooks highlight.
How does HLAB27 influence symptoms in females?
HLAB27 is a genetic marker that shows up in a large chunk of spondylitis patients. In women, its presence often means an earlier onset and a higher chance of extraspinal pain, such as in the hips or peripheral joints. Studies from the suggest that around 70% of HLAB27positive women report hip pain as a primary complaint.
QuickReference: HLAB27 Positive vs. Negative
| Feature | HLAB27 Positive | HLAB27 Negative |
|---|---|---|
| Typical Onset Age | Late teensearly 20s | Mid20s30s |
| Hip Involvement | High (60%+) | Moderate |
| Morning Stiffness Duration | >30min | Variable |
| Family History | Common | Less common |
How to differentiate spondylitis from other back problems?
Its easy to mislabel that nagging ache as just a bad posture day. Heres a quick selfscreen:
- Is the pain worse after resting and better after light activity? Spondylitis.
- Do you feel pain in the buttock area that radiates to the thigh? Look for sacroiliac involvement.
- Is there persistent swelling in a peripheral joint (e.g., knee)? Could signal extraspinal disease.
If you tick two or more of these boxes, its worth booking an appointment with a rheumatologist. Early diagnosis makes a world of difference.
First Line Treatments
Why NSAIDs are the cornerstone
Nonsteroidal antiinflammatory drugs (NSAIDs) are usually the first prescription because they target the inflammation that fuels the pain. Common choices include ibuprofen, naproxen, and the COX2 selective celecoxib. For most women, a lowtomoderate dose taken with food does the trick.
However, be mindful of the risks: gastrointestinal irritation, increased cardiovascular strain, andin rare caseskidney issues. Discuss any history of ulcers or heart disease with your doctor before committing to longterm use.
When corticosteroids become necessary
Corticosteroid bursts can calm a sudden flare, especially if NSAIDs arent enough. Oral prednisone for a short 12week stint, or a targeted injection into an inflamed sacroiliac joint, can bring relief fast. But remember, steroids are a quick fixtheyre not meant for continuous control because of sideeffects like bone thinning and mood swings.
DMARDs and biologics: slowing the disease
Traditional diseasemodifying antirheumatic drugs (DMARDs) like sulfasalazine have modest benefit for axial disease, but the real gamechangers are biologics. TNF inhibitors (e.g., etanercept, adalimumab) and newer IL17 blockers (secukinumab) have strong evidence of halting spinal fusion progression.
According to the , about 6070% of patients on biologics report a significant drop in pain within the first three months.
Comparison Chart: Medication Options
| Option | Onset of Relief | Typical SideEffects | Cost (US$) |
|---|---|---|---|
| NSAIDs | HoursDays | GI upset, cardiovascular risk | Low |
| Corticosteroids | DaysWeeks | Weight gain, mood swings, bone loss | Moderate |
| Traditional DMARDs | WeeksMonths | Liver enzymes, blood count changes | Moderate |
| Biologics (TNF/IL17) | Weeks | Infection risk, injection site reactions | High |
NonPharmacologic Therapies
Exercise: the prescription you can do at home
Movement may sound counterintuitive when youre stiff, but lowimpact exercise is the single most effective nondrug tool. A routine that mixes core strengthening, gentle stretching, and aerobic activity keeps the spine supple and reduces flareups.
Heres a simple 4week starter plan (feel free to swap days based on your schedule):
Weeks12: Foundation
- CatCow stretch 2minutes, 3times a day.
- Seated hip openers 30seconds per side.
- Brisk walk 20minutes, 4days/week.
Weeks34: Build Strength
- Modified plank hold 1530seconds, 3sets.
- Standing glute bridges 10 reps, 3sets.
- Swimming or cycling 30minutes, 3days/week.
Consistency matters more than intensity. Even a short daily habit can cut morning stiffness by up to 40% (data from the ).
Physical therapy and manual therapy
A qualified physio will tailor stretches to your hipsacroiliac area, improve posture, and teach safe lifting mechanics. Manual techniqueslike myofascial releasecan temporarily ease muscle guarding, making your home exercises more effective.
Complementary approaches
Yoga, acupuncture, and therapeutic massage have modest evidence for pain reduction. The key is to choose evidencebased styles that emphasize spinal alignment and avoid deep twists that could aggravate inflamed joints. If youre curious, try a beginners Gentle Yoga for Back Care class and see how your body responds.
Managing Risks & Monitoring
Regular labs and imaging
Because many of the medications affect liver function or blood counts, routine blood work every 36months is standard. Creactive protein (CRP) and erythrocyte sedimentation rate (ESR) help track disease activity, while an MRI of the sacroiliac joints is the goldstandard for confirming early inflammation.
Lifestyle factors that influence outcomes
- Weight management: Extra pounds add mechanical stress to the spine.
- Smoking cessation: Smoking accelerates spinal fusion; quitting can improve treatment response.
- Sleep hygiene: A supportive mattress and consistent sleep schedule aid recovery.
When surgery or advanced interventions become an option
Only a minority of women reach the point where spinal fusion or hip replacement is necessary. Indications include severe, fixed deformity, refractory pain despite optimal medical therapy, or progressive loss of mobility. Your rheumatologist will evaluate imaging trends and functional scores before recommending any surgical route.
Quick Reference Resources
Below are some handy tools you can download or bookmark right now:
- Symptom Tracker PDF: A printable onepage checklist to log pain, stiffness, and medication effects.
- AskYourDoctor Script: Five concise questions (e.g., How does my HLAB27 status affect my treatment plan?) to bring to your next appointment.
- Credible Sources: , , , and the for uptodate guidelines.
Conclusion
Living with spondylitis as a woman can feel like navigating a maze of pain, confusing symptoms, and an avalanche of treatment options. The reality, though, is far more manageable than it appears. By recognizing the distinct femalespecific signs, partnering with a rheumatologist for tailored medication, and committing to a regular, lowimpact exercise regimen, you can dramatically reduce flareups and protect your spine for years to come.
Take one step today: download the symptom tracker, schedule that rheumatology appointment, or simply add a 10minute stretch to your morning routine. You deserve a life where pain doesnt dictate the daylets work together to make that happen. For guidance on treatment goals and what remission can look like, review the ankylosing spondylitis remission criteria as part of your longterm plan.
FAQs
What early signs should women watch for with spondylitis?
Common early clues include persistent lower‑back or hip pain that improves with movement, morning stiffness lasting >30 minutes, peripheral joint aches (knees, shoulders), and a lingering “brain‑fog” fatigue.
How does being HLA‑B27 positive change treatment for females?
HLA‑B27‑positive women often develop symptoms at a younger age and are more likely to have hip or peripheral joint involvement, so doctors may start biologic therapy earlier to prevent structural damage.
Are NSAIDs safe for long‑term use in women with spondylitis?
NSAIDs are effective first‑line agents, but long‑term use can increase risk of gastrointestinal irritation, cardiovascular events, and kidney issues. Regular monitoring and using the lowest effective dose with food is recommended.
What kind of exercise is best for women dealing with spondylitis?
Low‑impact activities such as walking, swimming, cycling, and gentle core‑strengthening routines (e.g., modified planks, cat‑cow stretches) help maintain spinal flexibility without over‑loading inflamed joints.
When should I consider moving to biologic therapy?
If pain and stiffness persist despite NSAIDs, short courses of steroids, and physical therapy, or if imaging shows progressive inflammation, a rheumatologist may recommend TNF‑α inhibitors or IL‑17 blockers as the next step.