Did you know that up to87% of men notice some urinary leakage after a radical prostatectomy? Its a startling number, but its just the tip of the iceberg when it comes to what you might experience after surgery. In the next few minutes Ill walk you through the most common side effects, how long they usually last, and what you can actually do to stay in control of your life.
Quick Summary Table
| SideEffect | Typical Onset | Average Duration | LongTerm Persistence | FirstLine Management |
|---|---|---|---|---|
| Urinary Incontinence | ImmediateWeeks | 312months (most improve) | 510% require pads longterm | Pelvicfloor physio, fluid timing |
| Erectile Dysfunction | WeeksMonths | 624months (varies) | Up to 30% chronic | Medications, devices, counseling |
| Dry Orgasm / Reduced Sensation | Immediately after surgery | Usually permanent | Permanent | Lubricants, altered stimulation |
| Infertility | Instantaneous | Permanent (unless sperm banking) | Permanent | Sperm banking preop |
| Lymphedema | WeeksMonths (if nodes removed) | Variable | May be chronic | Compression, lymphatic massage |
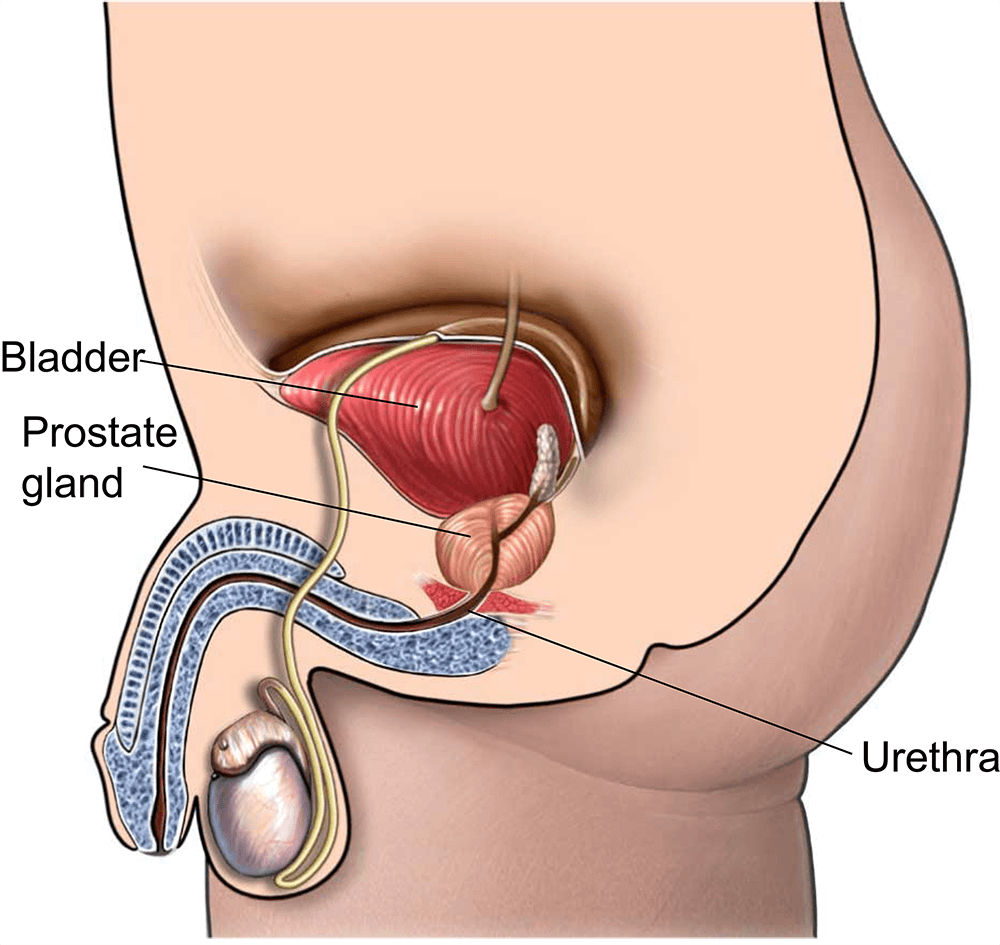
Urinary Incontinence Overview
Lets start with the one most men ask about first: leaks. After a radical prostatectomy the sphincter that controls urine flow can be a bit shaky. You might notice occasional dribbles, urgency, or nighttime trips to the bathroom.
Studies from the show that anywhere from 0% to 87% experience some degree of leakage, largely depending on the surgical technique and your preoperative pelvicfloor strength. The good news? 90% of men regain nearnormal control within a year with proper rehab.
Management Tips
- Pelvicfloor physio: Think Kegels, but guided by a therapist who can teach you the right pushandhold rhythm. A typical program runs 12weeks, with success rates around 70% for moderate cases.
- Fluid tweaks: Cut back on caffeine and carbonated drinks, especially after dinner. Keep a water bottle handy, but sip rather than gulp.
- Surgical rescue: For the stubborn 510% who keep needing pads, options like a urethral sling or an artificial urinary sphincter can restore confidence.
Erectile Dysfunction Overview
Another big worry is not being able to rise to the occasion. Nervesparing techniques aim to protect the cavernous nerves that run alongside the prostate, but the reality is that erectile dysfunction (ED) can still happen in anywhere from 11% to 87% of cases.
Why such a wide range? It depends on the surgeons experience, the stage of cancer, and whether you had a robotic or open approach. According to a comprehensive review in , men who undergo roboticassisted surgery often see a slightly faster return of erections, but longterm ED rates balance out.
Treatment Pathways
- PDE5 inhibitors: Viagra, Cialis, and their siblings work for many men, especially if the nerves werent completely severed.
- Vacuum erection devices: A noninvasive option that can be a bridge while waiting for nerve recovery.
- PENILE implants: For those whove tried everything else, a surgically placed device can bring back spontaneity.
- Emotional support: Open communication with your partner and, if needed, a counselor can ease the psychological strain.
Changes in Sexual Health
Even if you regain erections, the quality of orgasm often shifts. Most men notice dry orgasmsno ejaculateand a sometimesduller sensation. Some describe a subtle shortening of the penis, which is mostly a visual effect rather than a functional one.
These changes are usually permanent, but they dont have to signal the end of a satisfying sex life. Many couples discover new techniquesdifferent positions, extended foreplay, or simple lubricantsthat bring back pleasure.
Coping Strategies
- Use a highquality waterbased lubricant to enhance sensation.
- Experiment with stimulation that doesnt rely on ejaculatory pressure (e.g., perineal massage).
- Focus on intimacy beyond penetrationcuddling, kissing, shared fantasies.
Fertility Impact Overview
One side effect you cant ignore: after the prostate is gone, so is the seminal fluid. If you were hoping for children, this is a permanent change unless youve banked sperm beforehand.
Many urology centers now discuss sperm banking during the preop consult. Its a quick, painless processcollect a sample, freeze it, and keep it for future IVF or ICSI. If you missed that window, youll need to explore donor options or adoption.
Lymphedema Risk Overview
When surgeons also remove pelvic lymph nodes (common in higherrisk cancers), you open the door to lymphedemaswelling in the legs, groin, or lower abdomen. Its not as dramatic as in breast cancer patients, but it can be uncomfortable and, in rare cases, lead to infection.
Prevention & Care
- Wear graduated compression stockings during the first few months.
- Gentle lymphatic massage from a certified therapist can move fluid out of the affected area.
- Stay activewalks, swimming, or light cycling keep the lymph system humming.
Other Less Common Effects
Beyond the big four, you might notice:
- Bowel changes: Occasionally, a temporary loose stool or urgency appears, especially if the rectum was manipulated.
- Pain: Some men report lingering pelvic discomfort for months. Most of it fades with physical therapy.
- Hormonal shifts: Removing the prostate doesnt affect testosterone directly, but recovery can feel off due to stress and altered sleep.
Curious about how a robotic approach compares? A metaanalysis in suggests robotic prostatectomy may lead to slightly lower early urinary leakage and a quicker return to normal activities, though longterm erectile outcomes line up with open surgery.
Types of Prostatectomy
| Procedure | SideEffect Profile | Typical Recovery | Who Chooses It? |
|---|---|---|---|
| Open Radical Prostatectomy | Higher early incontinence, similar longterm ED | 46weeks hospital stay | Surgeons with extensive experience, large tumors |
| RoboticAssisted Laparoscopic | Lower early leakage, comparable ED | 23days hospital stay | Patients seeking minimally invasive option |
| Simple (Partial) Prostatectomy | Fewer sexual/urinary issues | Shorter stay | Benign enlargement, not cancer |
| Transurethral Resection (TURP) | Different set of urinary symptoms | Outpatient | Benign hyperplasia, not curative for cancer |
Understanding these four types helps you ask the right questions when youre in the doctors office. Will a robotic approach reduce my risk of leakiness? or If Im older, does open surgery give me better cancer control? are the kinds of conversations that lead to shared decisionmaking.
Real Patient Experiences
Prostate Surgery Ruined My LifeOr Did It?
Mark, a 58yearold accountant, wrote that two months after his surgery he was borderline embarrassed to leave the house because of sporadic leaks. He started a pelvicfloor program, cut down on his daily coffee, and within eight months was back to golfing without a single pad. I thought the surgery ended my independence, he says, but the rehab gave me a new sense of control.
Expert Insight
Dr. Elena Ramirez, a urologist with 20years of experience, stresses that patients who get realistic expectations and early physiotherapy are far more satisfied, even if a side effect persists. She recommends every man schedule a followup with a specialized pelvicfloor therapist within four weeks postop.
Managing Side Effects Effectively
Lifestyle & Nutrition
What you put in your mouth can aggravateor sootheyour bladder. Aim for:
- Lowcaffeine drinks (herbal tea, water).
- Avoiding spicy, acidic foods that can irritate the urinary tract.
- Staying hydrated, but spacing fluid intake to reduce nighttime trips.
Medical & Surgical Interventions
If simple measures dont cut it, theres a toolbox of options:
- Prescription meds for overactive bladder (mirabegron, anticholinergics).
- Urethral slings or artificial sphincters for stubborn incontinence.
- ED devicespills, vacuums, or implantsas discussed earlier.
Psychological Support
Feelings of frustration, shame, or loss are normal. Talk therapy, support groups, or online forums can provide a sense of community. Remember, youre not alonemany men walk this path and emerge stronger.
Bottom Line Summary
Radical prostatectomy can feel like stepping onto a roller coaster that you never signed up for. The ride includes urinary leakage, changes in sexual function, permanent infertility, and occasional swelling, but the good news is that most of these side effects are manageable, and many improve dramatically with time, therapy, and the right mindset.
What matters most is staying informed, voicing your concerns early, and partnering with a medical team that respects your goals. If youre facing surgery, ask about nervesparing options, pelvicfloor rehab, and sperm bankingknowledge is the first step toward reclaiming control. For detailed tips on improving recovery after surgery, consider resources on prostatectomy recovery to plan your rehab.
Whats your biggest worry about prostate surgery? Have you or a loved one gone through it? Share your story in the comments; together we can turn anxiety into empowerment.
FAQs
What is the typical recovery time for urinary incontinence after radical prostatectomy?
Most men see significant improvement within 3–12 months, with about 90% regaining near‑normal control by one year.
Can erectile function be restored after a nerve‑sparing prostatectomy?
Yes, many men recover erections over 6–24 months using medications, devices, or implants, especially when nerve‑sparing techniques are used.
Is infertility permanent after radical prostatectomy?
Yes, natural fertility is lost because the prostate and seminal vesicles are removed; sperm banking before surgery is the only way to preserve fertility.
How does lymphedema develop after prostate surgery?
If pelvic lymph nodes are removed, fluid can build up in the legs or groin; compression garments and lymphatic massage help manage it.
Are there long‑term sexual changes besides erectile dysfunction?
Men often experience dry orgasms and reduced sensation, which are usually permanent, but many adapt with lubricants and alternative stimulation methods.