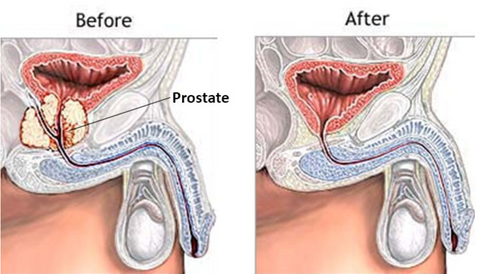
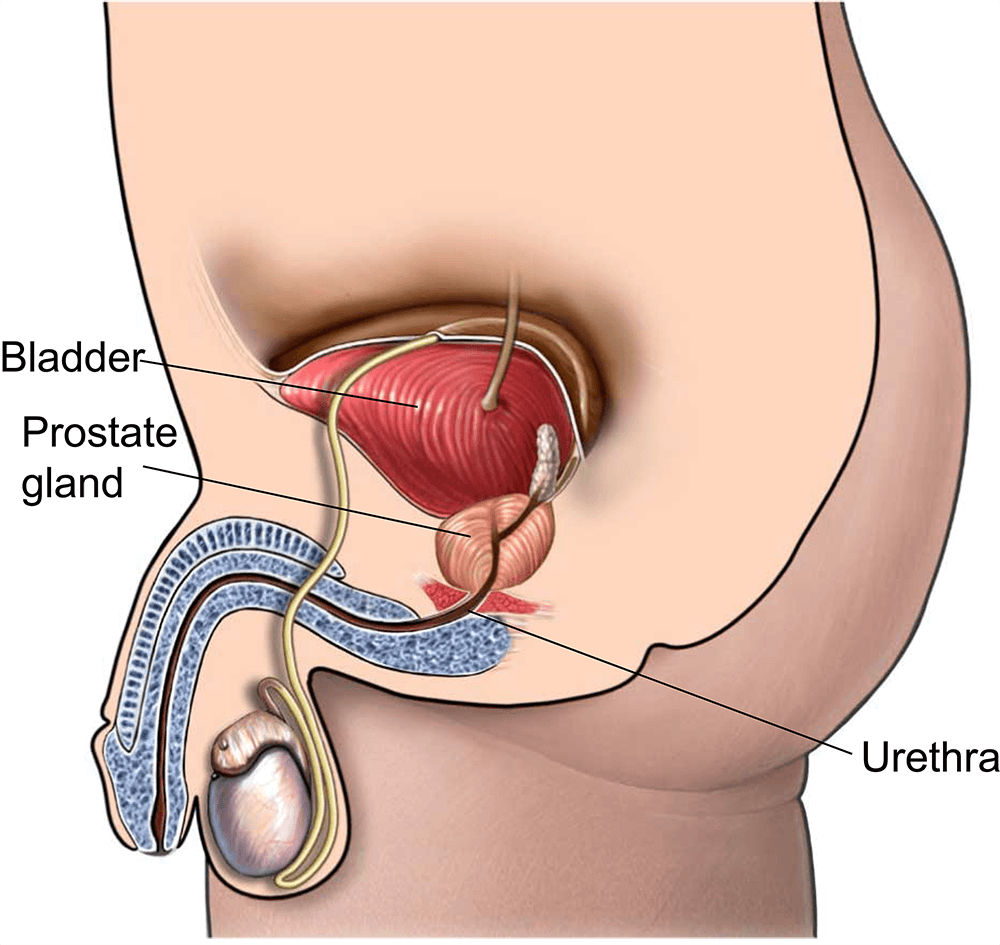
Short answer: urinary incontinence tops the list. It affects roughly onethird of men in the weeks after the surgery and can linger for months if not addressed. The good news? With the right tricks, support, and a bit of patience, most folks regain control and get back to their normal lives.
Quick Summary
Whats the main issue?
After a prostatectomy the bladdersphincter complex often needs time to relearn how to hold urine. This postprostatectomy urinary incontinence can be stresstype (leakage with cough or sneeze), urgetype (sudden need to go), or a mix of both.
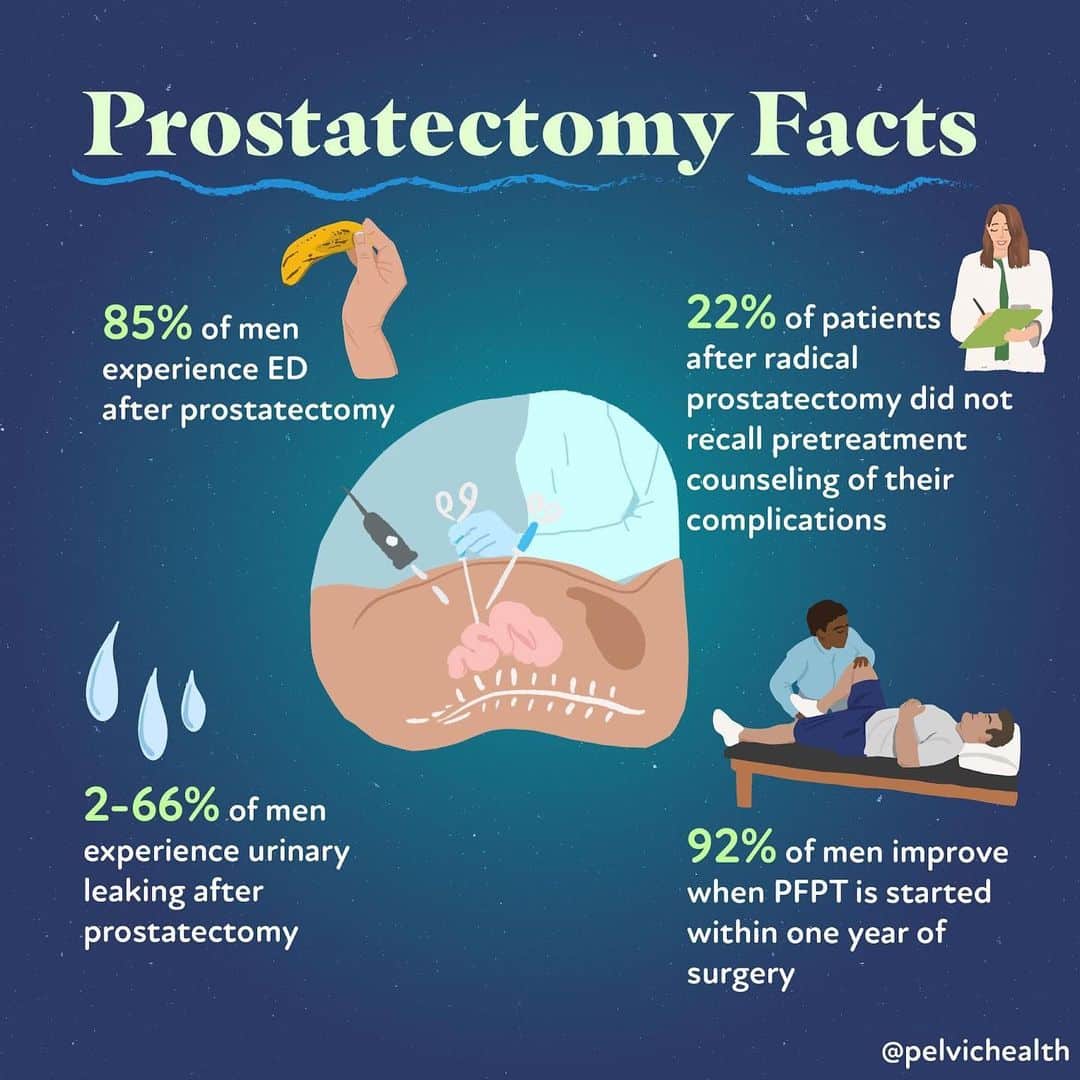
How common is it?
Studies from the Mayo Clinic and the American Urological Association show that 3040% of men experience some level of leakage during the first three months, while about 1015% still have persistent symptoms after a year.
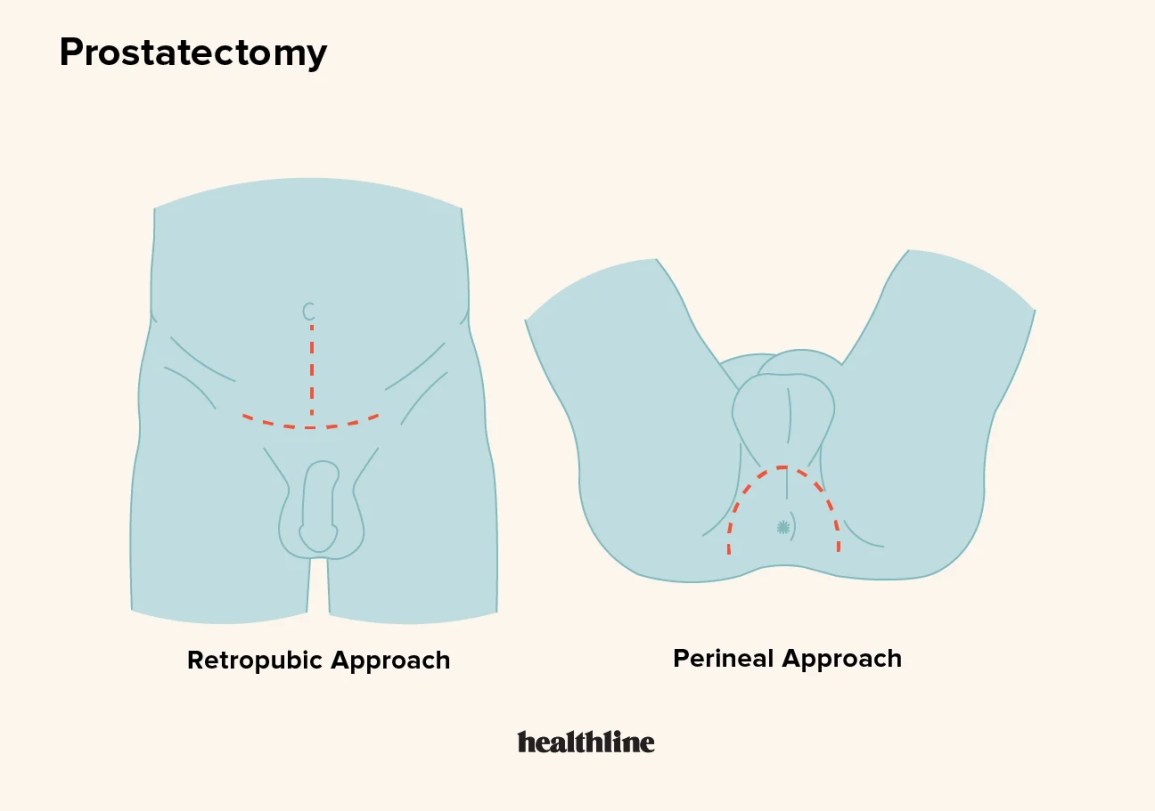
Which surgery type matters?
| Surgery | Incontinence Rate (first 3 months) |
|---|---|
| Open radical prostatectomy | 35% |
| Laparoscopic prostatectomy | 32% |
| Robotassisted prostatectomy | 28% |
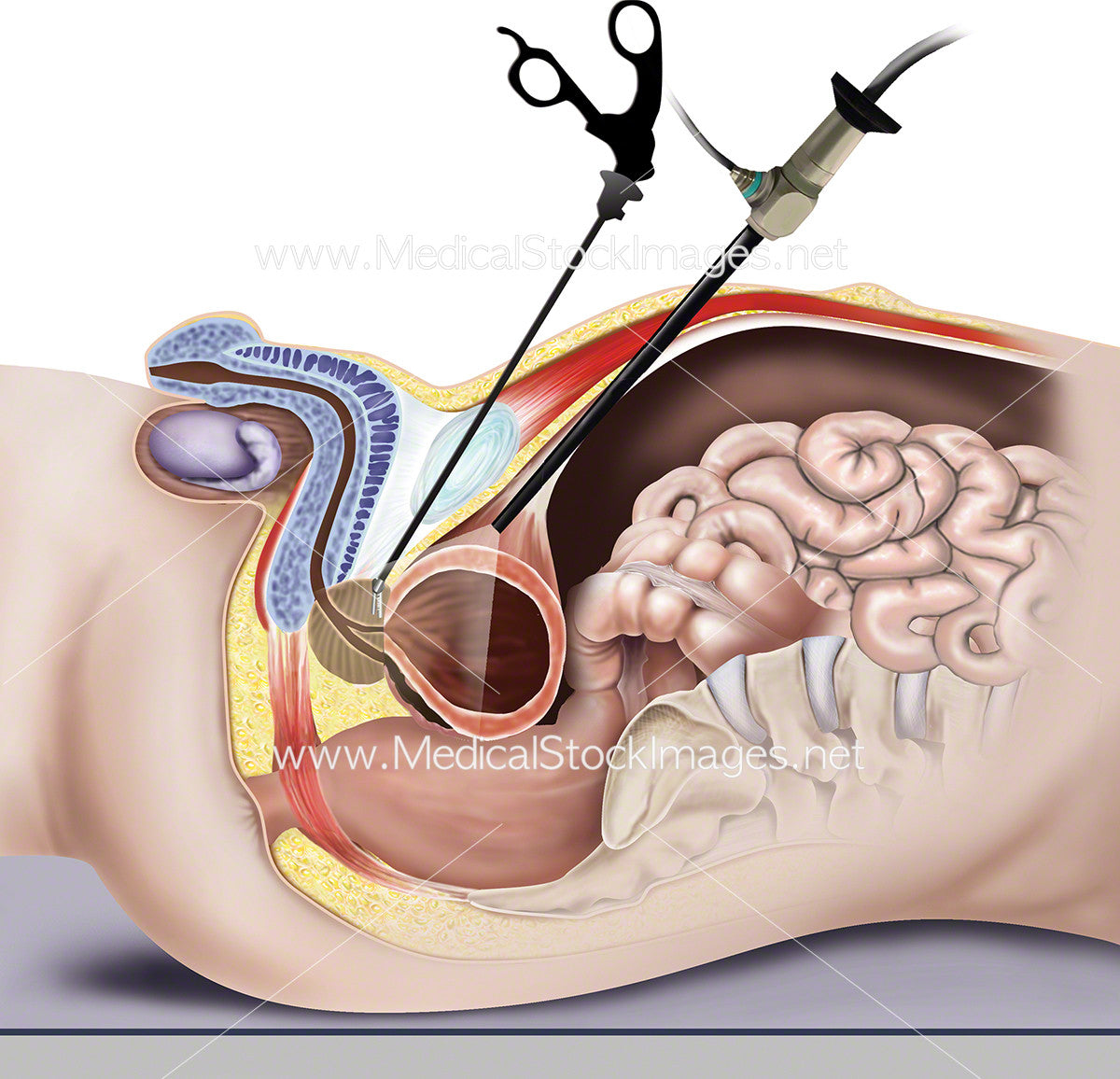
Robotic approaches tend to spare a bit more of the surrounding tissue, which can translate into slightly lower early leakage rates, but the difference isnt dramatic.
Expert voice
Urinary leakage after prostate surgery is expected, not a failure, notes Dr. Sarah Mitchell, a urologist at . Most men improve with time, pelvicfloor training, and proper followup.
Physiology Behind Leak
Where does the problem start?
The prostate sits just below the bladder, hugging the urethra and supporting the internal sphincter. When the gland is removed, the surgeon must reconnect the bladder to the urethra and often has to cut through or stretch the surrounding muscles.
What gets damaged?
- External sphincter muscles the main gatekeeper that stays closed until you decide to pee.
- Pelvic floor support a hammock of muscles that stabilizes the bladder and urethra.
- Nerve pathways signals that tell the brain when the bladder is full.
Why does it matter?
When any of those pieces are weakened, the coordination between fill and hold gets thrown off. Imagine trying to keep a garden hose shut with a leaky clamp a little pressure, and water bursts out.
Realworld illustration
John, 62, told me he first noticed a drip on day three after his robotic prostatectomy. I was sitting on the toilet and felt a warm trickle on my underwear, he said. It was embarrassing, but the nurse explained it was normal and gave me a simple Kegel routine.
Recognizing the Signs
When should you worry?
Most leakage is harmless, but you should call your surgeon if you notice any of these red flags:
- Sudden, forceful leakage accompanied by burning or foul odor (possible infection).
- Fever, chills, or flank pain these could signal a urinary tract infection (UTI).
- Persistent dribbling that doesnt improve after three months of pelvicfloor exercises.
Incontinence vs. infection
Both can cause urgency, but an infection often brings systemic symptoms (fever, malaise) and a cloudy or foulsmelling urine. A quick urine dipstick test at your doctors office can differentiate the two.
Selfassessment checklist
| Symptom | Likely Cause | Action |
|---|---|---|
| Leak when coughing | Stress incontinence | Start pelvicfloor PT |
| Sudden urge to go | Urge incontinence | Discuss meds with urologist |
| Burning, foul smell | UTI | See doctor for antibiotics |
| Fever/chills | Possible infection | Seek immediate care |
Questions to ask your doctor
- Is my leakage within the expected range for my surgery date?
- When should I start pelvicfloor physiotherapy?
- Do I need a catheter change to prevent infection?
Managing & Reducing Leakage
Lifestyle Tweaks (quick wins)
Small everyday changes can make a huge difference:
- Fluid timing Aim to finish most drinks two hours before bedtime.
- Limit irritants Cut back on caffeine, alcohol, and carbonated drinks, which can irritate the bladder.
- Foods to avoid after prostate surgery Spicy foods, citrus, and excess salt may increase urgency for some men.
Pelvicfloor rehabilitation
Think of Kegels as a gym for your inner muscles. Heres a simple starter routine:
- Identify the muscles by stopping urine flow midstream (just for practice).
- Contract them for 5seconds, then relax for 5seconds. Aim for 10 repetitions.
- Do three sets a day, gradually increasing the hold time to 10seconds.
- After a week, add quickfire squeezes: ten rapid contractions in a row.
Most urology centers recommend beginning these exercises within 710days postop, under the guidance of a pelvicfloor physiotherapist. According to a study in the , structured physiotherapy can boost continence rates by up to 30% at three months.
Medical & device options
If lifestyle and exercises arent enough, there are proven therapies:
- Prescription meds Anticholinergics (e.g., oxybutynin) calm an overactive bladder, while duloxetine can strengthen the sphincter tone.
- External devices Urethral inserts or continence pads provide temporary protection while you heal.
- Surgical revisions Sling procedures or an artificial urinary sphincter may be offered for persistent leakage (>12months). The decision depends on severity, overall health, and personal preference.
Preventing infection & UTIs
Catheters are a doubleedged sword they help drainage but can usher bacteria in. Follow these tips:
- Keep the catheter line clean and dry; change the dressing every 48hours.
- Wash hands thoroughly before handling the bag.
- Drink plenty of water (unless fluidrestricted) to flush bacteria.
- Report any foul odor, fever, or cloudy urine immediately.
Life Expectancy Impact
Does incontinence affect survival?
No direct link exists between urinary leakage and life expectancy after prostate removal. The surgery itself, when done for cancer, aims to cure or control the disease, and survival rates are comparable to other treatments when the cancer is caught early.
Qualityoflife considerations
While the odds of living a full life remain unchanged, dealing with leakage can be emotionally taxing. Anxiety, embarrassment, and reduced social activity are common. Thats why addressing the problem early both physically and mentally matters.
Recovery timeline chart
| Stage | Typical Duration | What to Expect |
|---|---|---|
| Immediate (daysweeks) | 06weeks | Frequent dribbling, possible catheter use. |
| Transitional (13months) | 612weeks | Improvement with Kegels and PT. |
| Chronic (>6months) | >6months | Persistent leakage may need advanced treatment. |
Support & counseling
Talking to a therapist or joining a peersupport group can lift the emotional weight. Many hospitals run postprostatectomy circles where men share tips, fears, and successes. Knowing youre not alone makes a world of difference.
Expert & Source Recommendations
Who to trust?
When you search for answers, look for information from:
- Boardcertified urologists (Mayo Clinic, Harvard Health, Cancer Research UK).
- Peerreviewed journals they give you data, not anecdotes.
- Licensed pelvicfloor physiotherapists they can tailor exercises to you.
Suggested reading
For a deeper dive, check out the on postsurgical urinary issues, and the American Urological Associations guidelines on managing incontinence after prostatectomy.
Conclusion
Urinary incontinence is the most common problem after prostatectomy, but its rarely a permanent sentence. With the right mix of fluid management, pelvicfloor training, timely medical help, and emotional support, most men regain control and enjoy a normal, healthy life. If youre navigating this road, remember youre not alone your surgeon, physiotherapist, and countless others have walked it before you. Take the first step today: practice a simple Kegel, note any redflag symptoms, and reach out to your care team. Your journey to confidence starts now.
For more detailed steps on early recovery and practical tips specifically about prostatectomy recovery, consider the recovery guide that outlines timelines and rehab routines to pair with pelvicfloor therapy.
FAQs
What is the most common problem after prostatectomy?
The most common problem after prostatectomy is urinary incontinence, affecting about 30-40% of men in the first three months after surgery.
How long does urinary incontinence usually last after prostatectomy?
Urinary incontinence often improves gradually, with many men regaining continence within 6 to 12 months, though about 10-15% may have persistent symptoms after a year.
What types of urinary incontinence occur after prostatectomy?
Common types include stress incontinence (leakage with activities like coughing or sneezing) and urge incontinence (a sudden need to urinate), or a combination of both.
How can urinary incontinence be managed after prostatectomy?
Management includes lifestyle changes, pelvic-floor muscle training (Kegel exercises), medications, use of continence devices, and in some cases, surgical interventions for persistent leakage.
Does urinary incontinence after prostatectomy affect life expectancy?
No, urinary incontinence after prostatectomy does not affect life expectancy, although it can impact quality of life and emotional well-being.