Ever caught yourself staring at an odd, warty bump in your mouth and wondering, Is this something serious? Youre not alone. Many of us notice strange changes in our bodies and hope theyll just disappear, but when it comes to a lesion that could be verrucous carcinoma, knowing how doctors stage it can change everythingfrom peace of mind to the treatment plan youll follow.
Heres the straightup answer: verrucous carcinoma is staged using the same TNM system most cancers use, and while its often lowgrade, understanding the stage helps your medical team decide the safest, most effective path. Lets walk through what that looks like, why it matters, and what you can do next.
Quick Overview
What Is Verrucous Carcinoma?
Think of verrucous carcinoma as the gentle giant of the oral cancer family. Its a slowgrowing, warty tumor that looks a bit like a cauliflower, usually appearing in the mouth, on the skin, or even in the genital area. Pathology outlines describe it as a welldifferentiated variant of squamous cell carcinomameaning the cells look more like normal tissue, which is why it tends to stay put and rarely spreads.
Typical Locations
When we talk about verrucous carcinoma oral cases, the tongue, floor of the mouth, and buccal mucosa get the most love (or trouble). Outside the mouth, you might see it on the skin of the feet or the penis, each with its own quirks.
Why Staging Matters
Does Staging Affect Prognosis?
Absolutely. Even though most verrucous carcinomas are lowgrade, knowing the stage tells doctors whether the tumor is confined to the surface or has nudged into deeper tissues or nearby lymph nodes. That knowledge directly influences the odds of a successful outcome.
Balancing Benefits and Risks
Staging isnt about scaring you with extra tests; its about tailoring care. Overtesting can feel invasive, but undertesting might miss hidden spread. Finding that sweet spotknowing when a CT scan or an MRI is truly neededkeeps you safe without the unnecessary hassle.
TNM System
What Do T, N, and M Stand For?
In the TNM world, T measures the primary tumors size and depth, N checks the nearby lymph nodes, and M looks for distant metastasis. For verrucous carcinoma, the same rules apply, but with a few nuances.
How Is T Staged?
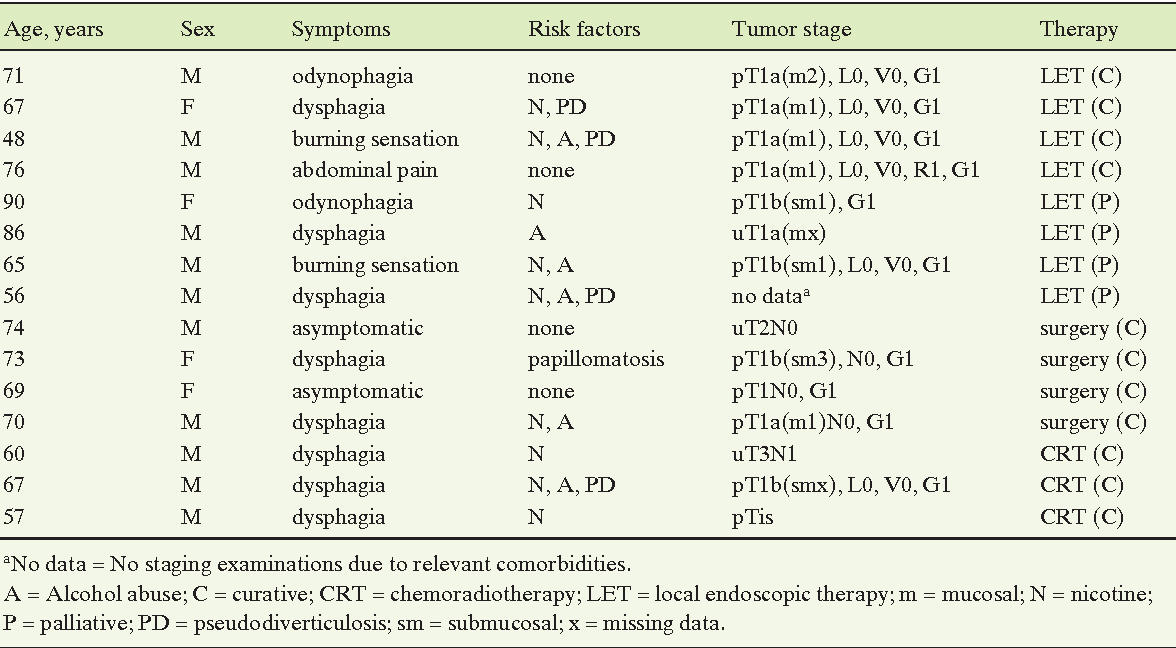
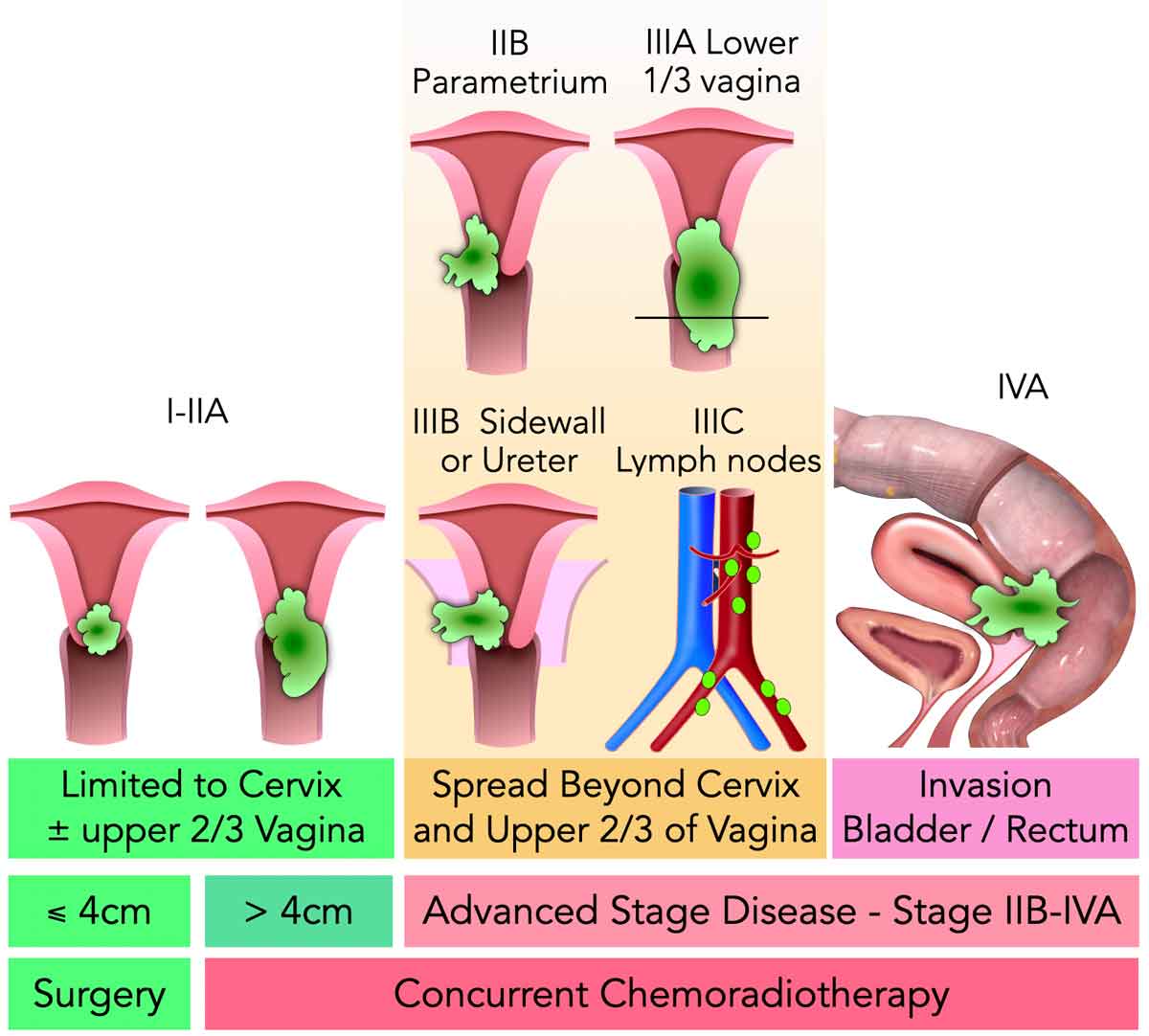
T1: Tumor 2cm, confined to the mucosa.
T2: >2cm but 4cm, still limited to submucosa.
T3: >4cm or invading deeper muscles.
T4: Invades adjacent structures (e.g., bone).
For superficial, exophytic lesions, you might see Ta (noninvasive).
When Are Nodes Positive?
Any palpable or imagingdetected lymph node larger than 1cm in the short axis bumps the N category up to N1 (single ipsilateral node). Multiple or contralateral nodes move you to N2 or N3.
Is Metastasis Common?
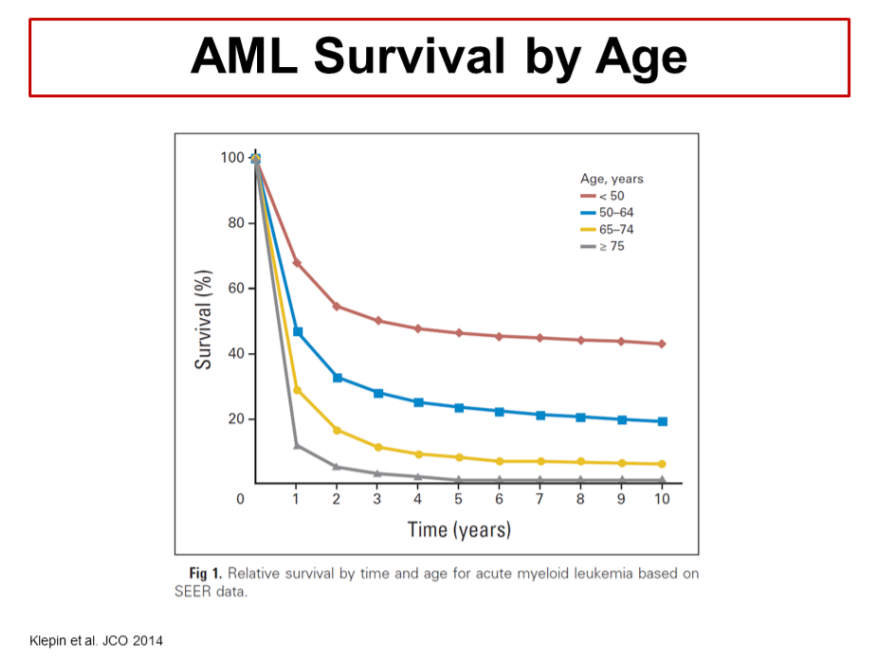
Rare. Most studies, including data from the SEER program, show verrucous carcinoma rarely jumps to distant sites. Thats why many patients stay in the M0 bucket.
| Stage | T | N | M | Overall Stage |
|---|---|---|---|---|
| Stage I | T1T2 | N0 | M0 | I |
| Stage II | T3 | N0 | M0 | II |
| Stage III | T4 | N0N1 | M0 | III |
| Stage IV | Any T | Any N | M1 | IV |
Staging by Site
Oral Staging Specifics
The oral cavity follows the classic AJCC rules, but clinicians pay extra attention to bone involvement because that can shift a T3 to a T4 overnight.
Skin Staging
Cutaneous verrucous carcinoma often stays superficial, so youll see more Ta or T1 designations unless theres deep dermal invasion.
Genital Staging
Penile or vulvar lesions are staged similarly, yet the anatomical complexities (like corpora cavernosa involvement) can bump the T category higher.
Clinical vs. Pathologic Staging
Whats the Difference?
Clinical staging relies on what the doctor sees and the imaging results before any surgery. Pathologic staging, on the other hand, comes from the actual tissue removed during biopsy or resectiongiving a crystalclear picture.
When Is a Biopsy Required?
Any suspicious warty lesion deserves a biopsy. The pathology report confirms whether youre dealing with a verrucous carcinoma and provides the definitive T measurement.
RealWorld Example
Imagine a 58yearold man who notices a slowgrowing ulcer on his tongue. Clinical exam suggests a T2 lesion, but the biopsy reveals deeper muscle invasion, upgrading it to T3. That shift changes his treatment plan from a simple excision to surgery plus a brief course of adjuvant therapy. If the team is considering the broader pelvic or systemic implications, they may also review guidance on related cancers such as prostate cancer outlook to help plan surveillance strategies in older patients with multiple risks.
Treatment Options
Surgery: The Gold Standard
Because verrucous carcinoma rarely spreads, removing the tumor with clear margins is often enough. For oral lesions, a partial glossectomy or mandibulectomy might be performed depending on size.
Radiation: A Cautious Approach
Radiation can be a doubleedged sword. While it can shrink tumors, theres a documented risk of the lesion transforming into a more aggressive squamous cell carcinomaa phenomenon called anaplastic transformation. Thats why many specialists reserve radiation for unresectable cases or after surgery when margins are close.
Systemic Therapy
Chemotherapy and targeted agents have limited roles; most patients do just fine with surgery alone. When used, its usually in a multimodal setting for advanced stages.
Decision Tree (StageBased)
Stage III: Surgery alone.
Stage III: Surgery + possible adjuvant radiation if margins are close.
Stage IV: Multidisciplinary approachsurgery, radiation, and perhaps systemic therapy.
Early Symptoms
What to Watch For?
A painless, white or pinkish plaque that slowly enlarges.
A warty, cauliflowerlike mass that may bleed when scraped.
Difficulty swallowing or a feeling that something is stuck in the throat.
If any of these pop up and linger for more than two weeks, its time to see a professional.
Timeline from Lesion to Diagnosis
Because the growth is slow, many patients wait months before seeking help. Early detection, however, can keep the stage low and the treatment simple.
Imaging & Diagnostic Tools
CT, MRI, PET: When Do They Help?
CT scans are great for bone involvement, MRI excels at softtissue depth, and PET is reserved for suspected distant spread (rare in verrucous carcinoma).
Ultrasound for Nodal Assessment
Highfrequency ultrasound can pinpoint suspicious lymph nodes without radiation exposureperfect for patients who need a quick N check.
StepbyStep Staging Journey
1. Clinical exam 2. Imaging (CT/MRI) if T3 or N1 3. Biopsy 4. Pathology report 5. Final TNM assignment 6. Treatment planning.
Frequently Asked Questions (FeaturedSnippet Ready)
Is verrucous carcinoma dangerous?
Its lowgrade and rarely metastasizes, but if left untreated it can cause local destruction, affecting speech, swallowing, and quality of life.
Can it be staged like other oral cancers?
Yesdoctors use the same AJCC/TNM criteria, with occasional tweaks for the tumors warty nature.
Do all patients need a CT scan?
No. Imaging is usually reserved for larger lesions (T3) or when lymph nodes feel abnormal.
What does Ta mean?
Ta denotes a noninvasive, exophytic tumor that hasnt breached the epitheliumcommon in early verrucous lesions.
Are pictures useful for selfdiagnosis?
Pictures can raise awareness, but only a clinicians exam and biopsy can confirm the diagnosis and stage.
Case Studies (Experience in Action)
Case1: EarlyStage Oral VC
John, 45, noticed a small, painless bump on his tongue. A biopsy confirmed a T1N0M0 lesion. He underwent a simple excision with clear margins. Six months later, hes back to enjoying spicy foods with no recurrence.
Case2: Advanced Penile VC
Mike, 62, presented with a large ulcerating mass on the penis. Imaging revealed T4N1M0 disease. He required partial penectomy plus adjuvant radiation. At twoyear followup, theres no evidence of spread, and he reports a good quality of life after reconstructive surgery.
Authoritative Sources & Further Reading
Trusted Guidelines
For the most uptodate staging criteria, see the . Its the gold standard that oncologists worldwide rely on.
Key Studies
Research published in the Journal of Oral Pathology highlights the low metastasis rate of verrucous carcinoma and underscores the importance of clear surgical margins. Another study in Head & Neck Oncology discusses the rare risk of anaplastic transformation after radiation.
Conclusion
Understanding verrucous carcinoma staging isnt just academicits the compass that guides every decision from diagnosis to recovery. While most lesions stay lowgrade and manageable, knowing the exact stage lets you and your medical team choose the safest, most effective plan and avoid unnecessary procedures.
If you spot a persistent warty growth, dont wait. Schedule an appointment, get a biopsy, and ask your doctor about the stage. Knowledge empowers you to take charge of your health, and with the right information, youre already halfway to the best outcome.
FAQs
What is verrucous carcinoma staging?
Verrucous carcinoma staging uses the TNM system to assess tumor size, lymph node involvement, and distant spread.
How does staging affect treatment?
Staging guides treatment decisions, helping doctors choose surgery, radiation, or other therapies based on cancer extent.
Is verrucous carcinoma staging different from other cancers?
No, it follows the same TNM system as other oral cancers, with minor adjustments for its unique growth pattern.
Can verrucous carcinoma spread to lymph nodes?
It rarely spreads to lymph nodes, but staging checks for any possible involvement to ensure accurate treatment.
What does Ta mean in verrucous carcinoma staging?
Ta indicates a noninvasive, exophytic tumor that hasn’t invaded deeper tissues, common in early-stage lesions.