Imagine youre sitting in a radiology suite, the machine humming softly, while a patient anxiously waits for answers. You know that the images you acquire today could shape the entire treatment plan tomorrow. Thats the power of a cervical cancer staging radiology assistant a trusted sidekick that helps turn raw scans into clear, actionable stages.
Why Use a Radiology Assistant
First off, what exactly does a radiology assistant do when we talk about cervical cancer? In plain language, its a combination of standardized protocols, checklists, and communication tools that make sure every MRI, every report, and every multidisciplinary discussion is consistent and reliable. Think of it as the wellorganized friend who always remembers to bring the right charger, the correct notes, and the big picture.
From the moment a patient steps into the department, the assistant guides the whole workflow: confirming the clinical question, preparing the patient, selecting the optimal sequences, and finally delivering a structured report that speaks the same language as the surgeon, oncologist, and pathologist. When you have a clear, repeatable process, you reduce errors, speed up decisionmaking, and, most importantly, give patients the confidence that their care is in capable hands.
Current Staging Systems
| System | Year | Role of Imaging | Key MRI Findings |
|---|---|---|---|
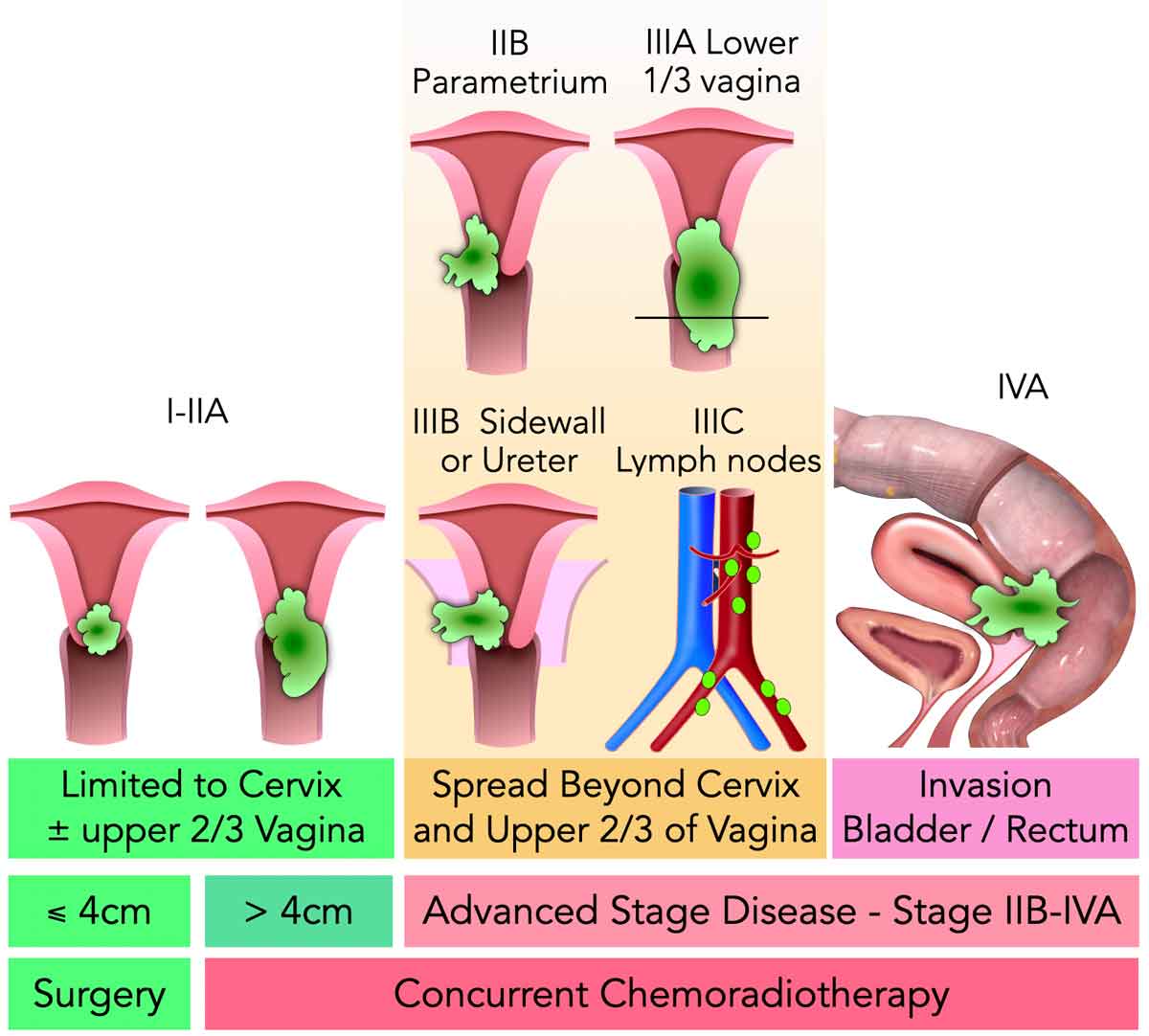
| FIGO (revised) | 2018 | Allows crosssectional imaging (MRI, CT, PET) to supplement clinical exam | Tumor size, parametrial invasion, vaginal/uterine extension, nodal status |
| TNM (8th/9th) | 2017 / 2022 | Provides detailed T, N, Mcategories for research and planning | Same MRI criteria plus distant metastasis detection |
So, why do we bother with both FIGO and ? The answer is simple: surgeons love FIGO because it ties directly to operative decisions, while researchers and medical oncologists lean on TNM for its granularity. A good radiology assistant knows which system the referring team prefers and tailors the report accordingly no extra guesswork needed.
MRI Protocol Checklist
Lets walk through the MRI protocol that the assistant makes sure we never miss. Picture yourself setting up the scanner; the checklist pops up on your screen, and you tick each box with confidence.
- Patient preparation: A comfortably full bladder, bowel prep if needed, and an antiperistaltic agent for those wiggly patients.
- Core sequences:
- T2weighted sagittal outlines the uteruscervix relationship.
- T2weighted axial and oblique shows parametrial invasion and stromal depth.
- Diffusionweighted imaging (DWI) highlights highcellularity tumor and suspicious nodes.
- Dynamic contrastenhanced (DCE) separates tumor from postradiation fibrosis.
- Reporting template: A clean structure Clinical Info Technique Findings Staging (FIGO/TNM) Impression. This template follows the , which many centers have adopted as a gold standard.
Following this checklist not only speeds up scan acquisition but also produces reports that are instantly usable by the tumor board. When every radiologist speaks the same language, the whole team moves forward together.
Interpreting MRI Findings
Even the best protocol can lead to misstaging if we misinterpret the images. Here are a few common pitfalls and how our radiology assistant helps sidestep them.
Overstaging: Edema vs. Parametrial Invasion
Its easy to mistake postprocedural swelling for true tumor spread. The assistant reminds us to crosscheck DWI ADC values true invasion shows low ADC, while simple edema has higher ADC. Correlating with the clinical exam (often a firm, immobile mass) also prevents overcalling.
Understaging: Missed Small Nodes
Small, <5mm nodes can hide metastatic disease. The assistants checklist flags when to look for round shape, loss of fatty hilum, or high signal on DWI. If doubt lingers, a PETCT can be ordered thats built into the nextstep portion of the report.
Artifacts That Trick the Eye
Motion, susceptibility, and even the coil placement can create ghosting that mimics tumor. The assistant prompts us to repeat a breathhold sequence or use parallel imaging, saving time and avoiding unnecessary alarm.
Having these guardrails in place means we deliver more accurate FIGO or and fewer secondlook scans that waste everyones precious time.
Beyond Cervical Cancer
Once youve mastered cervical cancer staging, the same radiology assistant framework slides seamlessly into other gynecologic malignancies.
Endometrial Cancer Staging Radiology
Endometrial cancer shares many MRI sequences with cervical cancer T2, DWI, and DCE but the landmarks shift to the endometrium and myometrium. The assistants checklist simply swaps parametrial for myometrial invasion depth and adds a column for cervical stromal involvement when needed. This crossapplication demonstrates the assistants versatility and the radiologists breadth of expertise.
Other Pelvic Tumors
Whether its ovarian carcinoma or vaginal melanoma, the core principle stays the same: standardized imaging, clear communication, and a structured report. By expanding the assistants scope, you become the goto imaging partner for the entire gynecologic oncology team.
Practical Resources
Want to start using a radiology assistant today? Heres a quick toolbox you can download and adapt:
- PDF Checklist: A printable Cervical Cancer MRI Staging Checklist that mirrors the Radiology Assistants format.
- Suggested Reading:
- Radiology Assistant Cervical Cancer MR Staging (2023).
- Radiopaedia Cervical cancer (staging) regularly updated.
- WHO/FIGO Official .
- Recent peerreviewed article: Imaging in Carcinoma Cervix and Revised 2018 FIGO Staging System (PMCID8590564).
- Continuing Education: ESUR and ACR webinars on pelvic MRI they often include live demonstrations of the radiology assistant workflow.
All these sources are from reputable societies or peerreviewed journals, ensuring the information you pass on is trustworthy and uptodate.
Conclusion
Bringing a cervical cancer staging radiology assistant into your practice isnt a fancy gadget; its a mindset. It means choosing the right MRI protocol, interpreting images with a calibrated eye, and delivering reports that speak the same language as your surgical and oncology colleagues. By following the checklists, embracing both FIGO and TNM perspectives, and leaning on reliable resources, youll help patients move from uncertainty to a clear, personalized treatment path.
Ready to give your radiology team a friendly boost? Download the checklist, join an upcoming webinar, or simply reach out to a colleague whos already using the assistant. Together, we can make every scan count and every staging decision feel a little less daunting for everyone involved.
For clinicians coordinating cancer care who are also managing patients with prostate concerns, concise guidance on prostate cancer outlook can help align expectations across disciplines and improve multidisciplinary planning.
FAQs
What is a cervical cancer staging radiology assistant?
A cervical cancer staging radiology assistant is a structured protocol or checklist that guides radiologists in acquiring and reporting MRI findings for cervical cancer staging.
Why is MRI important in cervical cancer staging?
MRI provides detailed images of tumor size, parametrial invasion, and spread to nearby organs, which are critical for accurate cervical cancer staging and treatment planning.
What should be included in a cervical cancer MRI report?
A cervical cancer MRI report should include tumor size, parametrial and vaginal invasion, distance to internal os, nodal status, and any distant spread or complications.
How does a radiology assistant improve cervical cancer staging?
A radiology assistant ensures standardized imaging, reduces errors, and promotes clear communication among the oncology team for better patient outcomes.
Can a radiology assistant be used for other gynecologic cancers?
Yes, the same radiology assistant framework can be adapted for endometrial, ovarian, and other pelvic cancers to maintain consistency in staging and reporting.