Finding the right pill (or pillfree) path to calm the storm inside can feel like looking for a flashlight in a blackout. If youre wondering which meds actually help PTSD, the two drugs most clinicians recommend are paroxetine and sertraline both SSRIs backed by NHS and VA guidelines. They can ease flashbacks, nightmares and anxiety, but theyre not a magic bullet.
In the next few minutes well walk through what each medication does, how to weigh benefits vs. sideeffects, and what options exist when the firstline drugs dont fit your life. Think of this as a friendly chat with a trusted healthcoach, not a dry textbook.
Quick Overview
PTSD (PostTraumatic Stress Disorder) isnt just having bad memories. Its a fullbody response that can include intrusive thoughts, hypervigilance, sleep disruptions, and intense anxiety. Medications are one tool in the toolbox, often paired with therapy such as CBT or EMDR. Below is a snapshot of the main drug families and when theyre usually considered:
- Firstline: SSRIs (paroxetine, sertraline) approved by the FDA, EMA, and NHS for PTSD.
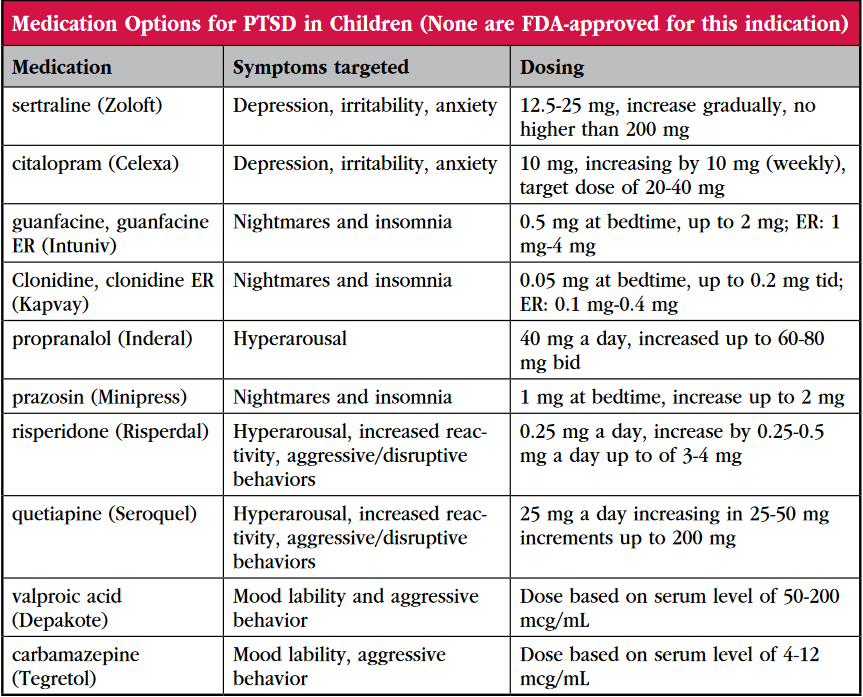
- Secondline / adjunct: SNRIs (venlafaxine), atypical antipsychotics (risperidone, quetiapine), and alphablockers (prazosin for nightmares).
- Emerging options: MDMAassisted therapy, prazosin for complex PTSD, and lowdose ketamine in research settings.
Choosing the best medication for PTSD and anxiety depends on your specific , your overall health, and how you react to the first pill you try.
FirstLine Options
When doctors talk about the best medication for PTSD, they almost always start with the two SSRIs that have the strongest evidence base.
Which SSRIs are FDA/EMAapproved for PTSD?
Paroxetine (brand name Paxil) and sertraline (Zoloft) received formal approval because largescale trials showed them to reduce core PTSD symptoms by roughly 3040% after 812 weeks. They work by increasing serotonin levels, which helps regulate mood, anxiety, and intrusive thoughts.
What about SNRIs like venlafaxine?
Venlafaxine (Effexor) blocks the reuptake of both serotonin and norepinephrine. Its especially helpful when anxiety and depressive symptoms are tightly woven together a common picture in complex PTSD medication scenarios. The tradeoff? A higher chance of increased blood pressure, so routine monitoring is key.
How do these meds help specific symptoms?
- Nightmares: Both SSRIs can dampen the intensity, but many patients need a dedicated sleep aid like prazosin.
- Flashbacks: Consistent dosing reduces the frequency; adjunctive lowdose antipsychotics sometimes help when flashbacks remain vivid.
- Hyperarousal: SSRIs calm the nervous system over time, often making other therapies more effective.
What are the most common sideeffects?
Every medication comes with a price tag of sorts. Below is a quick reference you can download later (see the table at the end of the article). In general, expect:
- Nausea or stomach upset (often eases after a few days)
- Sexual dysfunction a frequent complaint that many people quietly endure
- Weight changes some gain, some lose
- Sleep disturbances paradoxically, some feel more awake at night
Do you have any quickstart tips for minimizing sideeffects?
Take the pill with food, start at the lowest possible dose, and increase gradually (start low, go slow). Keep a simple symptom diary note both improvements and any new aches. If something feels off, call your prescriber before you make any changes.
Alternative Choices
SSRIs work great for many, but theyre not a onesizefitsall. Below is a rundown of what clinicians reach for when the first line doesnt hit the mark.
What meds are used when SSRIs dont work?
Atypical antipsychotics such as risperidone or quetiapine are often added to blunt severe flashbacks or agitation. Theyre not firstline because of metabolic sideeffects, but in a carefully monitored plan they can be a lifesaver.
Can mood stabilizers help?
If you have cooccurring bipolar features, doctors might add lithium or valproate. The evidence is lighter, but they can smooth out mood swings that otherwise sabotage therapy progress.
Any promising newer options?
Prazosin has earned a spot as the goto for PTSD medication nightmares, especially in veteran populations. A showed that nightly doses of 515mg cut nightmare frequency by half.
MDMAassisted psychotherapy is still in Phase3 trials, but early data suggest it may drastically reduce avoidance symptoms when combined with guided therapy. Keep an eye on the updates if youre curious about the frontier.
How do clinicians decide which secondline drug fits?
Think of it as a decision tree. If the primary symptom is nightmares prazosin. If flashbacks dominate lowdose antipsychotic. If anxiety is overwhelming and SSRIs feel flat SNRI or add an anxiolytic under strict supervision.
What about complex PTSD medication approaches?
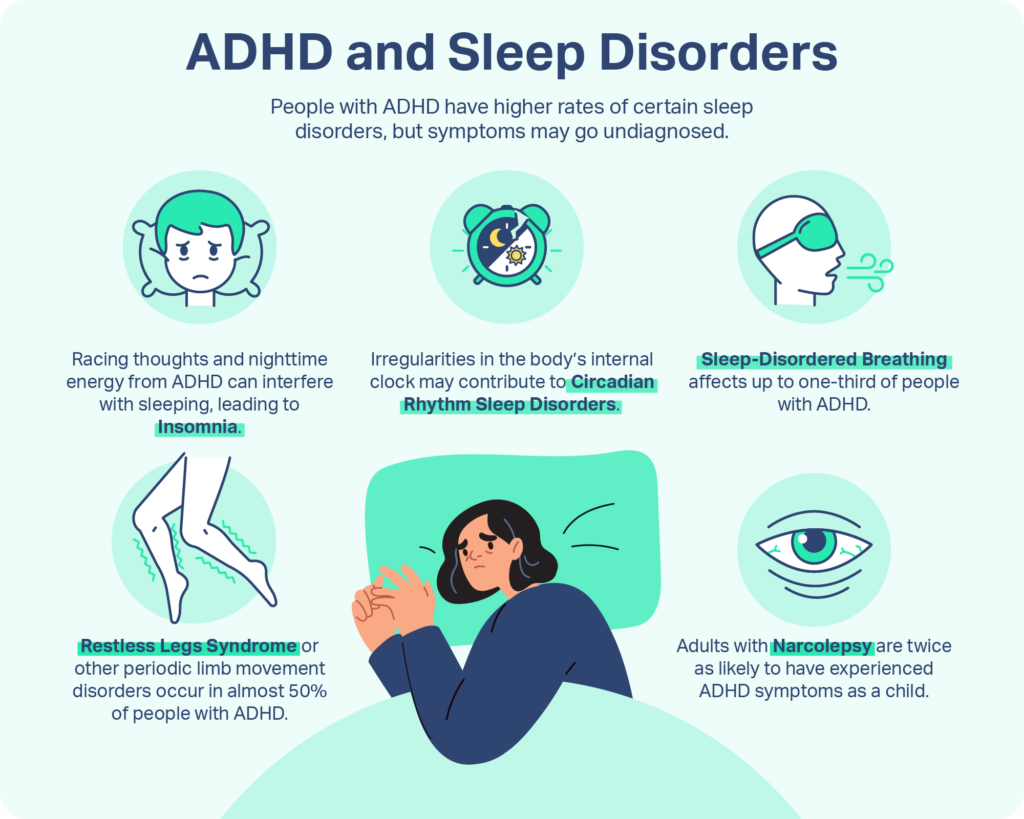
Complex PTSD often includes chronic trauma, emotional dysregulation, and interpersonal difficulties. In practice, many clinicians blend an SSRI with prazosin for sleep and a lowdose atypical antipsychotic for affect regulation. The key is close followupusually every 46 weeks. For patients exploring how past trauma and attention difficulties interact, resources on ADHD and trauma can help clinicians shape a combined treatment plan.
Nightmares & Flashbacks
These two symptoms are why many people search for PTSD medication nightmares or best medication for PTSD flashbacks. Lets unpack the science and the realworld tricks that actually make a difference.
Best medication for PTSD nightmares?
Prazosin, an alpha1 blocker originally made for blood pressure, relaxes the brains fear circuitry during REM sleep. Start low (12mg at bedtime) and titrate up; most patients see improvement within two weeks. Sideeffects are usually mild (dizziness on standing) and disappear once the dose stabilizes.
Best medication for PTSD flashbacks?
While SSRIs reduce overall intrusion frequency, some people need a targeted boost. A low dose of risperidone (0.250.5mg) taken when flashbacks loom can blunt the surge of cortisol and dampen the memorys vividness. Always combine this with psychotherapy; medication alone rarely eradicates the underlying trauma.
Whats the best medication for PTSD and anxiety combo?
Sertraline is often preferred because it has a relatively mild sideeffect profile and also treats generalized anxiety. Pair it with CBT and you have a twopronged attack: the drug stabilizes the chemistry, and the therapy reshapes the thought patterns.
Can medication alone stop flashbacks?
Rarely. Flashbacks are stored memories; medication can lower the brains excitability, but you still need a safe space to process them. Think of medication as the foundation and therapy as the house you build on top.
Is there a PTSD medication list you can download?
Below is a concise table you can copy into a spreadsheet or print out. Feel free to edit the columns to match what your prescriber recommends.
| Drug | Class | Typical Dose | Main Use | Key SideEffects |
|---|---|---|---|---|
| Paroxetine | SSRI | 2060mg daily | General PTSD symptoms | Nausea, sexual dysfunction, weight gain |
| Sertraline | SSRI | 50200mg daily | PTSD + anxiety | Insomnia, diarrhea, dizziness |
| Venlafaxine | SNRI | 75225mg daily | PTSD with strong depressive component | Increased BP, sweating, headache |
| Prazosin | Alpha1 blocker | 115mg at bedtime | Nightmares & sleep disruption | Dizziness, fainting (first dose) |
| Risperidone | Atypical antipsychotic | 0.252mg daily | Flashbacks, agitation | Weight gain, metabolic changes |
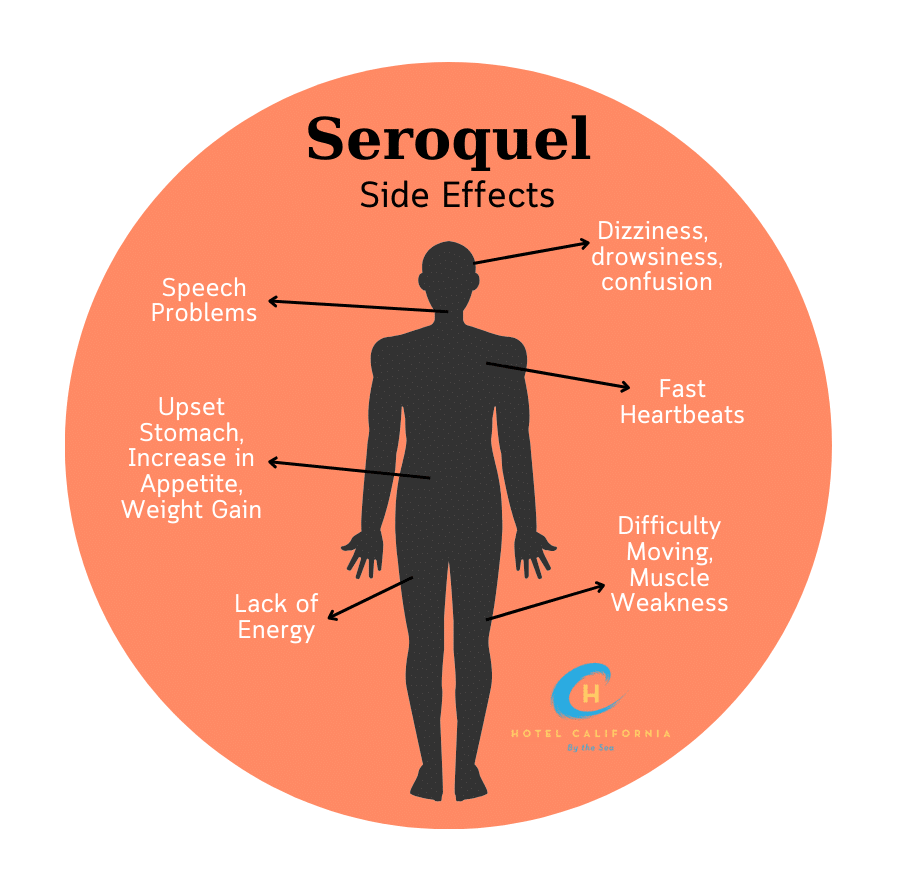
| Quetiapine | Atypical antipsychotic | 25150mg nightly | Sleep aid, anxiety | Sedation, dry mouth |
SideEffect Management
Every bump on the road deserves a warning sign. Understanding PTSD medication side effects lets you catch problems early and keep the treatment journey smooth.
What are the most concerning sideeffects?
While most patients tolerate SSRIs well, a few red flags demand immediate attention:
- Suicidal thoughts: Especially in people under 24years old. Any sudden mood shift should be reported.
- QT prolongation: Certain antipsychotics can affect heart rhythm. An EKG is often ordered before starting or increasing doses.
- Severe allergic reaction: Swelling, rash, or difficulty breathing call emergency services.
How to handle insomnia or weight gain?
Take the medication in the morning if its making you wired at night. Pair it with simple sleep hygiene: dim lights an hour before bed, limit caffeine, and consider a calming tea. For weight changes, a short walk after meals or a gentle strength routine can offset the metabolic drift.
Can PTSD meds interact with other prescriptions?
Yes. SSRIs can increase bleeding risk when combined with blood thinners, and SNRIs can raise blood pressure when mixed with certain decongestants. Keep a master list of all meds and share it with every prescriber. A quick can be a lifesaver.
Are there longterm risks?
Longterm SSRI use has been linked in some studies to reduced bone density, especially in postmenopausal women. Regular calcium intake and weightbearing exercise help mitigate this. Metabolic sideeffects from atypical antipsychotics (high cholesterol, diabetes) also require periodic labs.
When should you ask for a medication review?
Schedule a checkin every 3months, or sooner if you notice new symptoms. Even if you feel better, a professional can confirm the dose is optimal and discuss taper plans when youre ready.
Talking to Doctor
Getting the right prescription is a conversation, not a monologue. Heres a cheatsheet of questions that make your appointment feel like a collaborative brainstorming session.
What questions should you ask your psychiatrist?
- Whats the expected timeline for improvement?
- How will we track progress rating scales, diaries, or appointments?
- What are the signs that I should call you right away?
- If sideeffects appear, can we adjust the dose before stopping?
How to discuss past medication experiences?
Bring a simple medication diary: date, dose, how you felt, any sideeffects. A onepage chart makes patterns obvious and saves time. I tried sertraline for six weeks and my anxiety dropped, but I started feeling nauseous after the third week, is a clear, actionable statement.
What if you feel the medication isnt helping?
Dont wait until youre frustrated. Ask: Can we increase the dose, try a different medication, or add a sleep aid? A stepwise plan keeps you in control.
Can you request a nondrug alternative?
Absolutely. Say, Im interested in trying EMDR alongside medication, or perhaps focusing on CBT first. The best treatment plan is the one youre comfortable committing to.
What documentation do you need for insurance?
Most insurers require a DSM5 diagnosis code (F43.10) and a written treatment plan outlining medication and therapy. Have your clinician write a brief note that you can scan and upload.
Resources & Reading
Having reliable sources at your fingertips makes the journey less lonely. Below are a few goto sites recommended by clinicians:
- NHS PTSD Treatment Page: Clear explanations of medication options and sideeffect monitoring.
- Veterans Affairs Medications for PTSD guide: Indepth data on prazosin and complex PTSD approaches.
- APA Clinical Practice Guideline: Evidencebased recommendations for combining medication and psychotherapy.
- PTSD Coach App: Free tool for tracking symptoms, medication adherence, and coping techniques.
All links above are drawn from authoritative health organizations, ensuring the information you get is accurate and uptodate.
Conclusion
Finding relief from PTSD is rarely a straight line, but with the right medication roadmap you can navigate the twists more confidently. The best PTSD medication is the one that balances symptom relief with tolerable sideeffects, and that choice should always be made together with a trusted prescriber. Keep a symptom diary, stay curious about how each pill feels, and pair medication with evidencebased therapy whenever possible.
If this guide sparked a question or you have a story to share, drop a comment below. Your experience might be the exact piece of advice someone else needs right now. And if you found this article helpful, feel free to share it with a friend whos walking a similar path were all stronger together.
FAQs
What is the best medication for PTSD?
The most recommended medications for PTSD are SSRIs like paroxetine and sertraline, which help reduce core symptoms such as flashbacks, nightmares, and anxiety.
Can medication help with PTSD nightmares?
Yes, prazosin is commonly prescribed to reduce PTSD nightmares, especially in people who do not get enough relief from SSRIs alone.
Do PTSD medications help with flashbacks?
SSRIs can reduce the frequency of flashbacks, and sometimes low-dose antipsychotics like risperidone are added for more severe or persistent flashbacks.
Are there side effects from PTSD medication?
Common side effects include nausea, sexual dysfunction, weight changes, and sleep disturbances. Most side effects improve over time or with dose adjustments.
Can I stop PTSD medication if I feel better?
Always talk to your doctor before stopping PTSD medication. Abruptly stopping can cause withdrawal symptoms or a return of PTSD symptoms.