Ever feel like your mind is a weathertorn fieldsometimes calm, sometimes a storm of restlessness, anxiety, or memory fog? Youre probably wondering whether past trauma is the hidden driver behind those ADHDlike moments. The short answer is yes: trauma can shape the same brain pathways that ADHD affects, and the two often walk handinhand.
In the next 1520 minutes well break down the science, point out the sneaky overlap, and give you realworld steps to get the right help. No jargon, no endless backstoryjust the info you need to make sense of whats happening inside you (or someone you love) and start moving toward relief.
Why They Connect
What does the science say?
Researchers have found that children who experience chronic stress or abuse show changes in the prefrontal cortex, amygdala, and dopamine systemsexactly the regions also implicated in ADHD. A 2023 reported that early trauma predicts higher ADHD symptom scores in adulthood, even after controlling for genetics.
How trauma rewires attention
When youre under threat, cortisol spikes and the brain goes into hypervigilance mode. Over time, that constant alertness can blunt dopamine receptors, making it harder to focus on anything that isnt perceived as a danger. Think of it as a car thats always stuck in first gearyou cant smoothly shift to cruise control.
Spotting Overlap
Which ADHD signs mimic trauma?
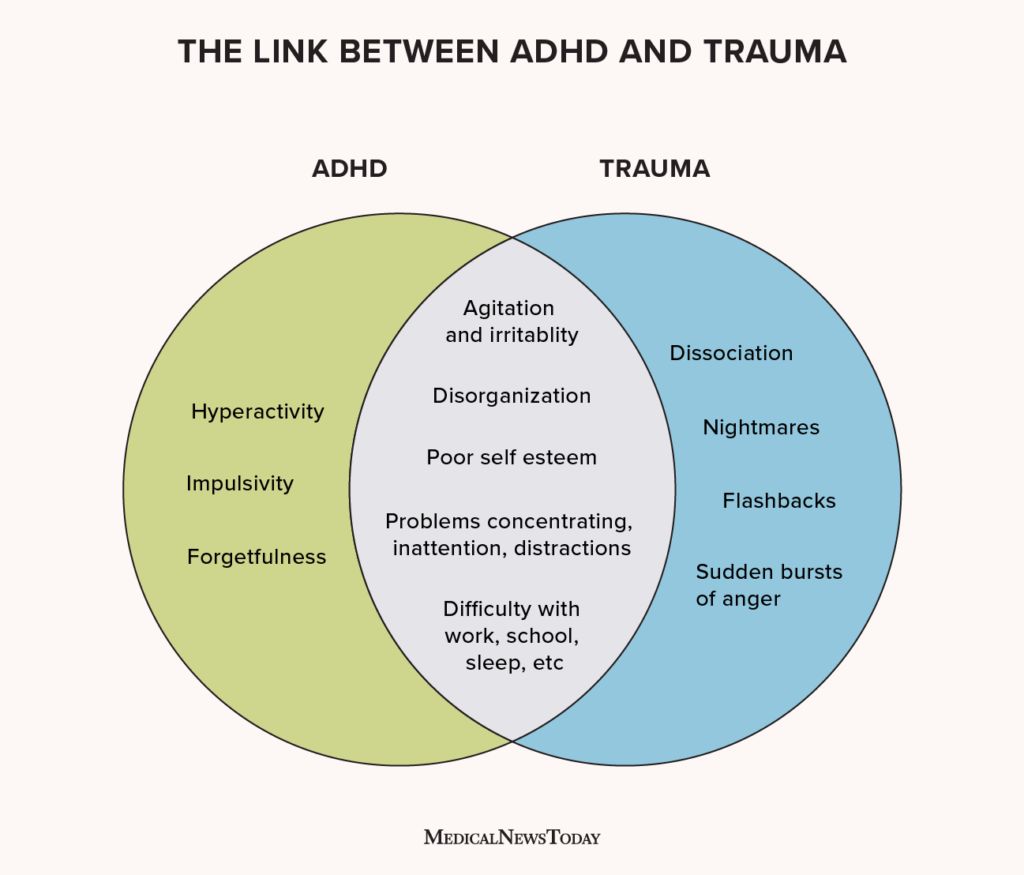
Both conditions can cause:
| Symptom | Typical ADHD Origin | Typical Trauma Origin |
|---|---|---|
| Inattention | Difficulty sustaining focus on tasks | Mind drifts to whatif survival scenarios |
| Impulsivity | Acting without thinking | Reacting to perceived threats |
| Emotional dysregulation | Quick mood swings | Heightened startle and anger responses |
| Sleep disturbances | Restless nights from racing thoughts | Nightmares or hyperarousal from trauma |
Can trauma cause ADHDlike symptoms in adults?
Absolutely. Adults who endured childhood neglect or abuse often report attention fog, restlessness, and impulsivity that look just like adultonset ADHD. A 2024 article highlighted that up to 30% of adults with a trauma history meet ADHD criteria.
ADHD and trauma in women
Women tend to internalize symptomsso you might see anxiety, perfectionism, or chronic fatigue instead of classic hyperactivity. Studies show women are more likely to receive a late ADHD diagnosis after trauma is addressed, because providers often overlook quiet presentations.
Distinguishing Them
Redflag differences
Look for these clues:
| Feature | ADHD | Trauma |
|---|---|---|
| Onset age | Typically before 12 | Can appear after a specific event |
| Trigger pattern | Consistent across settings | Flareups linked to reminders |
| Medication response | Stimulants improve focus | Stimulants may increase anxiety |
How reliable is an ADHD or trauma quiz?
Selfscreeners like the ASRS (Adult ADHD SelfReport Scale) or the ACE questionnaire are great starting points, but theyre not diagnostic. Think of them as roadmaps that tell you you might need a professional copilot.
When to see a professional
Schedule an evaluation if you notice:
- Symptoms persisting for 6+ months.
- History of childhood adversity (abuse, neglect, prolonged stress).
- Daily functioning is impaired at work, school, or relationships.
- Any mentalhealth red flags (panic, selfharm, substance use).
Impact Over Lifespan
Kids
Early identification matters because the brain is still plastic. Untreated ADHDtrauma overlap can lead to academic setbacks, lower selfesteem, and strained family dynamics. A 2025 report notes that targeted, traumainformed interventions can improve school performance by up to 20%.
Teens
Adolescents often grapple with identity and peer pressure while dealing with hidden trauma triggers. You might see acting out in school, social withdrawal, or risky behaviors. One case study described a 16yearold who, after a combined CBTADHD and EMEMDR program, reported a 40% drop in impulsivity.
Adults
For grownups, the overlap can masquerade as chronic burnout, relationship chaos, or just being an overthinker. Data from the National Institute of Mental Health indicate adults with ADHD are 7 more likely to have PTSD, underlining the need for a dualdiagnosis approach.
Complex PTSD and ADHD in adults
Complex PTSD (CPTSD) adds layers of emotional numbness and relational difficulties. When it coexists with ADHD, treatment plans must address both attentional regulation and deepseated trauma memories. A flowchart often used by clinicians starts with a traumainformed interview, followed by neuropsych testing, then a coordinated medicationtherapy plan.
Assessment & Screening
Goldstandard ADHD tools
Conners3, ASRSv1.1, and the Clinical Interview for DSM5 are the goto instruments for ADHD. They capture frequency, severity, and functional impact.
Trauma screening tools
The ACEQ (Adverse Childhood Experiences Questionnaire) and the PCL5 (PostTraumatic Stress Disorder Checklist) are widely validated. For CPTSD, the ITQ (International Trauma Questionnaire) adds nuance.
Dualscreen approach
Combine the ASRS with the ACEQ in one session. This dual screen catches cases where a patient might score high on ADHD items but also reveal early trauma, prompting a more thorough followup.
Treatment Strategies
Medication considerations
Stimulants (methylphenidate, amphetamines) work well for pure ADHD, but if traumarelated anxiety is high, they can feel jittery. Nonstimulants like atomoxetine or guanfacine often have a smoother sideeffect profile for mixed presentations.
Therapy options
Evidencebased combos work best:
- CBT for ADHD: Improves executive function, timemanagement, and organization.
- TraumaFocused CBT or EMDR: Processes painful memories, reduces hypervigilance.
- Integrated DBTADHD programs: Teach emotion regulation while addressing impulsivity.
Lifestyle hacks
Simple habits can tip the balance:
- Set a consistent sleep routineaim for 79 hours.
- Move your body dailyshort walks reset cortisol.
- Mindful breathing (478 technique) before stressful tasks.
- Use visual planners or digital timers to break tasks into bitesize blocks.
School & work accommodations
For kids, an IEP or 504 plan can provide extra time, preferential seating, or a quiet zone. Adults can request reasonable accommodations under the ADA, such as flexible deadlines or a designated focus room.
Common Questions
Can trauma cause ADHD in adults?
It doesnt create the disorder from scratch, but chronic stress can mimic or amplify ADHD symptoms. Think of trauma as turning up the volume on underlying attentional challenges.
Whats the difference between ADHD and trauma symptoms in adults?
ADHD symptoms are usually pervasive across all life areas and improve with stimulant medication. Trauma symptoms, however, often flare with reminders of the original event and may involve flashbacks, hyperarousal, or avoidance.
How do I know if my childs behavior is ADHD or trauma?
Ask yourself: Did the behavior start before a known adverse event? Does it improve in safe, predictable environments? If youre unsure, a combined assessment (see Dualscreen approach) is the safest route.
Is there a reliable ADHD or trauma quiz?
Selftests are useful for awareness but not diagnosis. The best practice is to share your quiz results with a licensed clinician who can interpret them in context.
What does ADHD and trauma overlap look like in real life?
Imagine Sara, a 28yearold graphic designer. Shes brilliant when deadlines loom, but outside work she feels spaced out, forgets appointments, and gets sudden panic attacks when a coworker raises their voice. A dual assessment revealed adult ADHD plus unresolved childhood emotional neglect.
Where can I find community support?
Subreddits like r/ADHD and r/traumarecovery host moderated discussions where members share coping tips. Remember to verify advice with professionalsonline forums are great for empathy, not a substitute for treatment.
How does neglect factor into ADHD and trauma?
Neglect is a chronic, lowgrade stressor that can stunt the development of executive functionsthe brains CEO. Research links prolonged neglect to poorer working memory and increased impulsivity, hallmarks of ADHD.
Resources & Next Steps
Quickstart toolkit
Download a free PDF that includes:
- Symptom tracker worksheet.
- List of traumainformed therapists (by state).
- Medicationquestion guide for your next doctor visit.
Trusted organizations
For reliable information and crisis help, visit:
- CHADD (Children and Adults with ADHD)
- APAs Trauma Center
- National Suicide Prevention Lifeline (988)
Talking to your doctor
Try this script: Ive been experiencing difficulty focusing and also have a history of childhood trauma. Could we explore whether these issues are related and discuss a combined treatment plan?
Conclusion
ADHD and trauma often travel together, weaving a complex story of brain chemistry, lived experience, and emotional response. By recognizing the overlap, seeking a traumainformed assessment, and embracing a balanced treatment planmedication, therapy, and lifestyle tweaksyou can untangle the knot and reclaim clarity. Download the free toolkit, join a supportive community, and schedule that honest conversation with a qualified professional. You deserve a life where focus and peace coexist, not compete. Whats your next step toward that balance?
FAQs
Can trauma cause ADHD‑like symptoms in adults?
While trauma doesn’t create ADHD from scratch, chronic stress can mimic or amplify attentional difficulties, impulsivity, and restlessness, making the symptoms look very similar to adult‑onset ADHD.
How can I tell if my challenges are due to ADHD or trauma?
Key clues include the age of onset (ADHD usually before age 12), consistency across settings (ADHD) versus symptom spikes linked to reminders of a traumatic event (trauma), and how you respond to stimulant medication (improved focus for ADHD, possible anxiety increase for trauma).
What assessments are recommended to identify both conditions?
Use a dual‑screen approach: combine a validated ADHD tool such as the ASRS‑v1.1 or Conners‑3 with a trauma questionnaire like the ACE‑Q or PCL‑5. Follow up with a comprehensive clinical interview and, if needed, neuro‑psychological testing.
Which medications work best when ADHD and trauma coexist?
Stimulants are first‑line for pure ADHD, but if trauma‑related anxiety is high, non‑stimulants (atomoxetine, guanfacine) or a low‑dose stimulant plus an anxiolytic may provide a smoother effect. Always discuss your trauma history with the prescriber.
What lifestyle strategies help manage both ADHD and trauma?
Prioritise regular sleep, daily physical activity, and mindfulness breathing (4‑7‑8). Use visual planners or timers to break tasks into short blocks, and create a calm workspace to reduce hyper‑vigilance.