Stick with me for the next few minutes and youll walk away with a handy symptom checklist, a quick selfscreening tool, and a roadmap of proven treatments. Think of this as a friendly guide not a textbook that you can dip into whenever you need a little reassurance or direction.
Understanding PTSD in Women
What exactly is PTSD for women?
Posttraumatic stress disorder (PTSD) is a mentalhealth condition that can develop after you experienceor witnessa terrifying event. The Diagnostic and Statistical Manual of Mental Disorders (DSM5) defines it by four core clusters: intrusive memories, avoidance, negative mood/cognition, and heightened arousal. For many women, these clusters intertwine with hormonal cycles, interpersonal dynamics, and social expectations, giving PTSD a slightly different flavor.
How common is PTSD among women?
According to the , about 1012% of women will experience PTSD at some point in their lives, compared with roughly 5% of men. That gap widens further when you consider specific traumas such as sexual assault or intimatepartner violence, which disproportionately affect women.
Key research findings (20232025)
Recent studies from the American Psychological Association and the VA show three main reasons for this disparity:
- Biological differences estrogen can amplify the brains fearmemory pathways.
- Trauma type women are more likely to experience chronic or interpersonal trauma, which tends to produce stronger PTSD reactions.
- Social stigma women often silence themselves out of fear of judgment, delaying diagnosis and treatment.
Common PTSD Symptoms
What are the 17 symptoms of PTSD?
Heres the full DSM5 checklist, broken down in plain language. If you tick several of these off, consider reaching out to a professional:
- Repeated, unwanted memories of the event
- Distressing dreams related to the trauma
- Flashbacks that feel like youre reliving it
- Intense psychological distress when reminded of it
- Physical reactions (sweat, rapid heartbeat) to reminders
- Avoiding places, people, or activities that trigger memories
- Feeling detached or numb
- Loss of interest in previously enjoyed activities
- Negative beliefs about yourself or the world
- Persistent guilt or shame
- Memory problems about the trauma
- Hypervigilance always on guard
- Easily startled
- Sleep disturbances (insomnia or nightmares)
- Irritability or angry outbursts
- Difficulty concentrating
- Selfdestructive behavior (substance use, reckless driving)
Physical symptoms of PTSD in women
Beyond the mentalhealth checklist, many women report bodily signs that are easy to overlook:
- Chronic headaches or migraines
- Stomachaches, irritable bowel syndrome, or other GI issues
- Unexplained fatigue or brain fog
- Muscle tension, especially in the neck and shoulders
- Sudden heart palpitations without a medical cause
Complex PTSD (CPTSD) in women how it differs
When trauma is prolonged or repeated (e.g., ongoing abuse), many women develop Complex PTSD. The added symptom clusters include:
- Emotional dysregulation mood swings that feel out of control
- Negative selfconcept persistent feelings of worthlessness
- Relationship difficulties extreme trust issues or clinginess
| Symptom | Standard PTSD | Complex PTSD (CPTSD) |
|---|---|---|
| Flashbacks | ||
| Persistent guilt | (more intense) | |
| Relationship difficulties | ||
| Emotional numbness |
Why Women Are More Susceptible
Trauma types that hit women hardest
Sexual assault, intimatepartner violence, childhood abuse, and even complications during childbirth rank as the top triggers for PTSD in women. These events often involve a betrayal of trust, which intensifies the emotional imprint.
Biological & genetic factors
Recent work from VCU Health (2025) points to a geneenvironment interaction: women with certain variants of the FKBP5 gene experience stronger cortisol spikes after trauma, making fear memories more entrenched.
Social & environmental contributors
Factors like economic instability, lack of social support, and cultural stigmas around mental health can widen the gap. On the flip side, strong community ties, access to therapy, and education act as protective buffers.
Diagnosis and Screening
How long do women usually wait before getting diagnosed?
Unfortunately, the average delay for women is about four years. Thats a long time to live with intrusive thoughts and physical pain without a name attached to it.
What assessments do clinicians use?
Professionals typically rely on:
- CAPS5 the ClinicianAdministered PTSD Scale, the gold standard interview.
- PCL5 a selfreport questionnaire you can fill out at home.
- Comprehensive trauma history and medical evaluation.
When to suspect postpartum PTSD?
If you notice after birth that you have intrusive memories of delivery, avoid caring for your newborn, or feel intense anxiety when you hear a baby cry, these may be signs of signs of PTSD in women after birth. Postpartum PTSD affects roughly 16% of new mothers, yet its often mistaken for baby blues.
Selfscreening checklist (downloadable PDF)
Below is a quick 10item screen you can print out. If you check five or more, consider making an appointment with a mentalhealth professional.
Effective Treatment Options
Evidencebased therapies
Two therapies dominate the research landscape for women:
- TraumaFocused Cognitive Behavioral Therapy (TFCBT) helps reframe trauma memories and develop coping skills.
- Eye Movement Desensitization and Reprocessing (EMDR) uses bilateral stimulation to unstick traumatic memories.
Both have shown significant symptom reduction in women, with effect sizes comparable to medication.
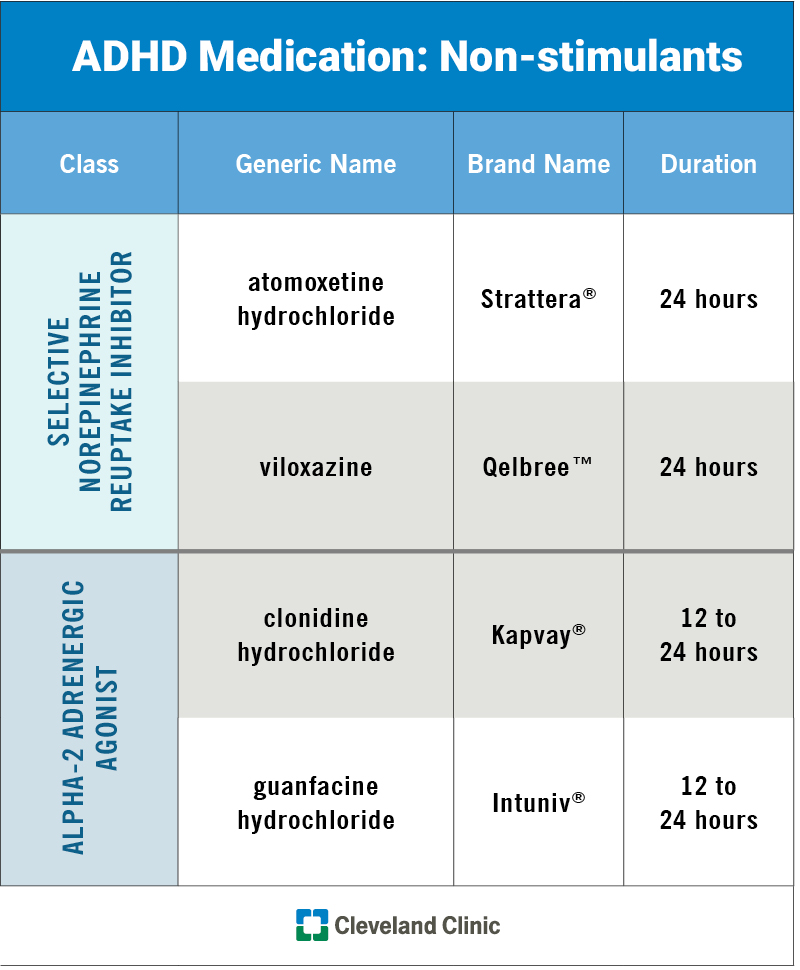
Medication considerations for women
Selective serotonin reuptake inhibitors (SSRIs) such as sertraline and paroxetine are FDAapproved for PTSD. Women should discuss hormonal influences with their prescriber, as estrogen can affect drug metabolism. If youre breastfeeding, sertraline is often recommended as a lowrisk option.
Specialized programs for Complex and Postpartum PTSD
Integrated care centerslike the Womens PTSD Clinic at the VAoffer combined therapy, medication, and motherinfant psychotherapy for postpartum cases. These programs acknowledge that healing isnt just in the head; its also in the body and relationships.
Stepbystep treatment plan template
Use this template as a starting point:
- Initial assessment (CAPS5 or PCL5)
- Choose a primary therapy (TFCBT or EMDR)
- Discuss medication options, if needed
- Set shortterm goals (e.g., reduce flashbacks from daily to weekly)
- Review progress every 46 weeks and adjust accordingly
Daily Coping Strategies
Grounding techniques for flashbacks
The 54321 method is a lifesaver:
- Identify 5 things you can see
- 4 things you can touch
- 3 things you can hear
- 2 things you can smell
- 1 thing you can taste
Doing this anchors you back in the present, breaking the flashback loop.
Lifestyle habits that reduce symptom severity
Simple, consistent habits make a huge difference:
- Exercise 30 minutes of moderate activity (walking, yoga) boosts endorphins and improves sleep.
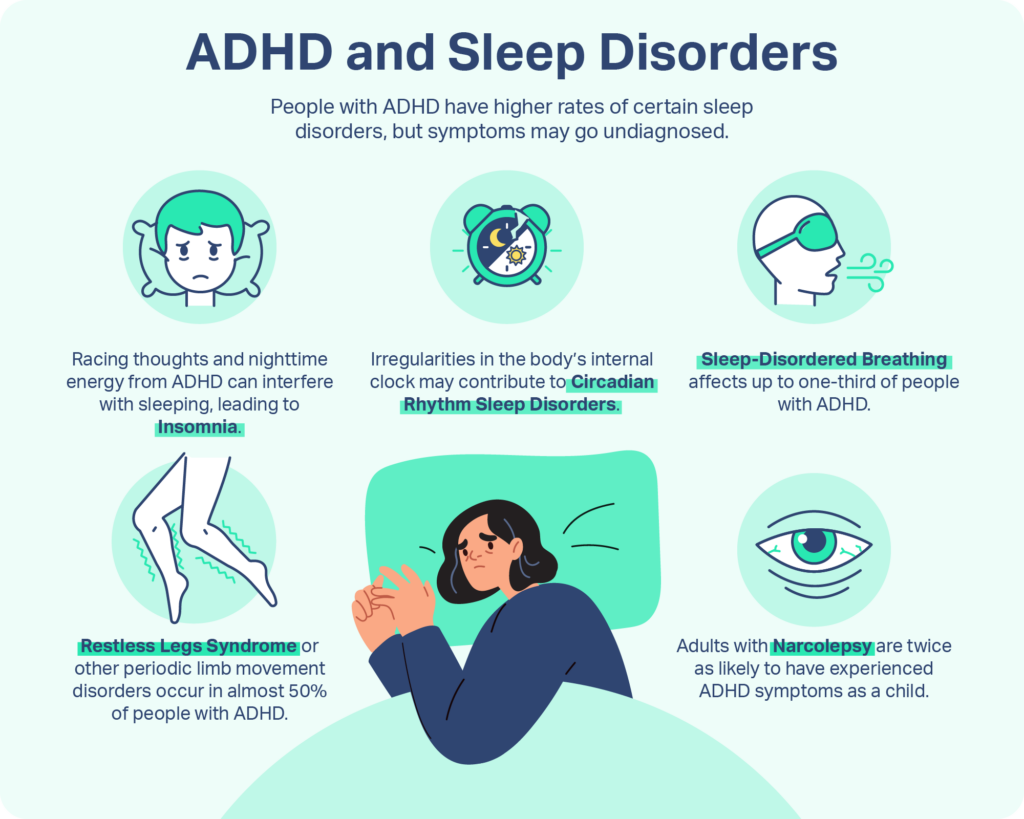
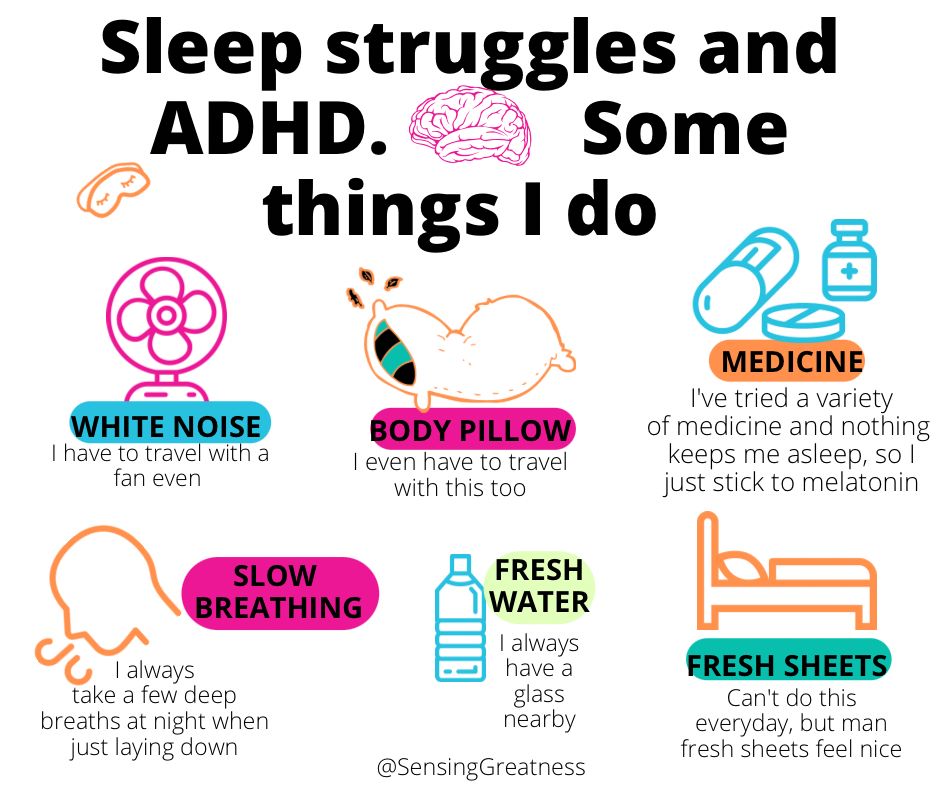
- Sleep hygiene Keep a regular bedtime, limit caffeine after 2p.m., and create a calming presleep routine. For readers who struggle with sleep related to attention or trauma, practical sleep tips ADHD can be adapted to support trauma recovery by stabilizing routines and reducing nighttime hyperarousal.
- Nutrition Foods rich in omega3s (salmon, walnuts) support brain health.
- Mindfulness A 10minute daily meditation can lower hypervigilance.
Building a supportive network
Isolation fuels PTSD. Reach out to trusted friends, join a womenfocused support group, or consider online communities like the VA PTSD forums. Sharing your storyeven just a sentencehelps normalize your experience and reduces shame.
Resources and Support
Here are a few reliable places to get help right now:
- Suicide & Crisis Lifeline 988 (U.S.) 24/7 free support.
- VA Womens Health Services specialized PTSD care for veterans.
- Womens PTSD Clinic (UCLA) offers both inperson and telehealth options.
- National Center for PTSD a treasure trove of selfhelp tools and therapist directories.
All of these resources are vetted by reputable health agencies, so you can feel confident your time is well spent.
Conclusion
PTSD in women is a real, often hidden, challenge that blends emotional, physical, and relational pain. Yet, as youve just read, theres a clear path forwardrecognize the 17symptom checklist, seek a timely diagnosis, and explore evidencebased therapies that respect the unique ways trauma shows up for women. Remember, you dont have to navigate this alone; community, professional care, and daily coping tools can transform the storm into a manageable breeze.
If anything in this guide resonated with you, or if you have questions about a specific symptom, feel free to drop a comment below. Sharing your experience not only helps you process what youre feeling, it also lights the way for someone else who might be scrolling in the dark. Lets keep the conversation goingbecause healing is better together.
FAQs
What are the most common PTSD symptoms in women?
Women with PTSD often experience intrusive memories, flashbacks, avoidance of reminders, heightened arousal, and physical signs such as chronic headaches, stomachaches, and fatigue.
How does complex PTSD differ from standard PTSD for women?
Complex PTSD includes the usual PTSD symptoms plus emotional dysregulation, a persistent negative self‑concept, and severe relationship difficulties, usually after prolonged or repeated trauma.
Why is PTSD more prevalent in women than in men?
Key factors include biological influences (e.g., estrogen’s effect on fear‑memory pathways), higher rates of interpersonal trauma like sexual assault, and social stigmas that delay help‑seeking.
What treatment options are most effective for women with PTSD?
Evidence‑based therapies such as Trauma‑Focused Cognitive Behavioral Therapy (TF‑CBT) and Eye Movement Desensitization and Reprocessing (EMDR) work well, often combined with SSRIs when medication is needed.
How can a new mother recognize postpartum PTSD?
Signs include intrusive memories of the birth, avoidance of baby‑related activities, intense anxiety when hearing a baby cry, and feeling detached from the newborn. If several of these appear, professional screening is recommended.