At first, I thought it was nothing just a little sore gum that popped up after a stressful week. But when the redness wouldnt go away and my skin flared up at the same time, I realized there might be a deeper link between my mouth and my psoriasis. The short answer? Yes, psoriasis can affect your dental health, and knowing how to manage that connection can save you a lot of trouble (and a few dentist appointments).
Heres the lowdown on whats really going on, the oral issues you might notice, and the everyday steps you can take so your smile stays as healthy as your skin. Think of this as a friendly chat over coffee, with a sprinkle of science to keep things legit.
Science Behind Psoriasis
What do the latest studies say?
Research over the past few years has painted a pretty clear picture: people with psoriasis are23times more likely to develop gum disease compared to those without the condition. A 2020 cohort study found a markedly higher prevalence of periodontitis among psoriasis patients, while a 2021 investigation into psoriatic arthritis (PsA) showed a threefold increase in advanced dental disease risk. Even a 2023 nationwide retrospective analysis published in PeerJ described a twoway street gum disease can worsen skin plaques, and severe skin inflammation can accelerate periodontal breakdown.
How does inflammation connect skin & mouth?
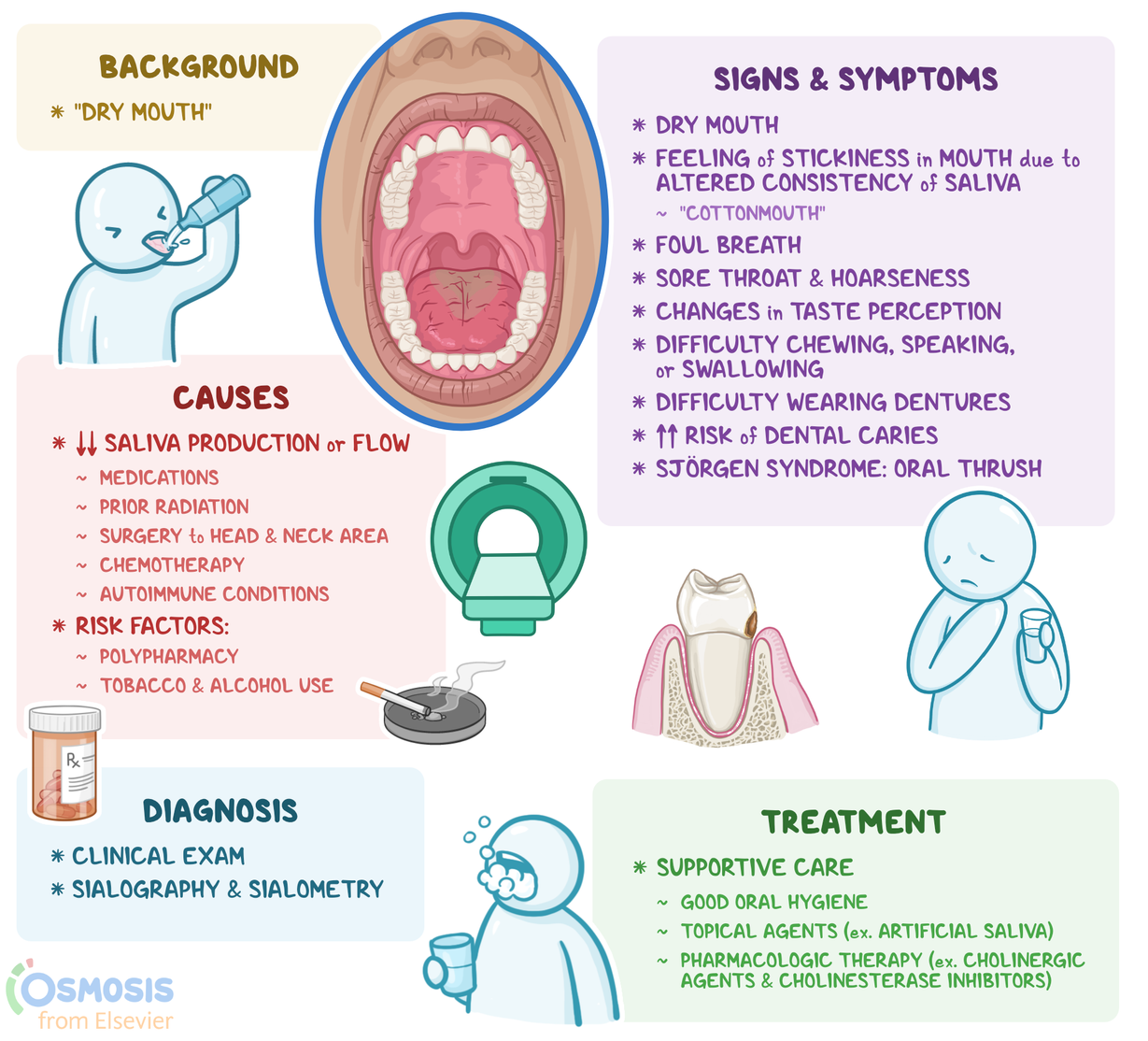
Both psoriasis and periodontal disease share a stubborn inflammatory cocktail: cytokines like TNF, IL17, and IL23 go rogue and keep the immune system on high alert. When these messengers flood the bloodstream, they dont stay confined to the skin they head straight for the delicate tissues supporting your teeth. The result? The gum tissue becomes more prone to infection, bone loss, and, ultimately, tooth instability. Some psoriasis medications can reduce saliva flow, worsening this dry environmentif you want to know more about morning dry mouth, it's worth checking how it can relate to your dental health.
Key data points you can cite
| Study | Finding |
|---|---|
| 2018 Cohort (USA) | Psoriasis odds of periodontitis by 2.4 |
| 2020 Metaanalysis | Systemic inflammation links to higher plaque scores |
| 2021 PsA Dental Study | Advanced dental disease 3 more common in PsA |
| 2023 PeerJ Review | Bidirectional relationship confirmed |
Common Oral Issues
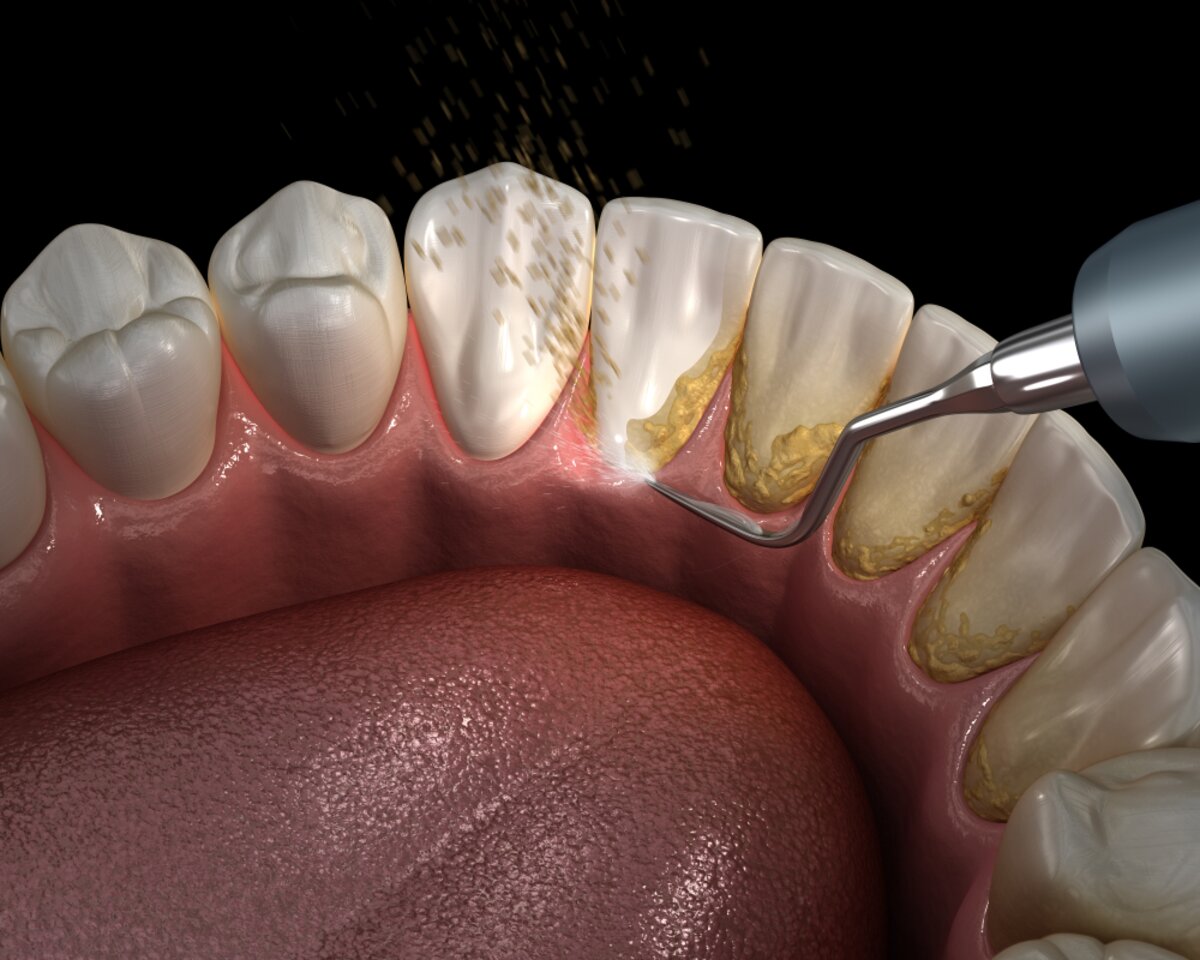
Gum disease (periodontitis & gingivitis)
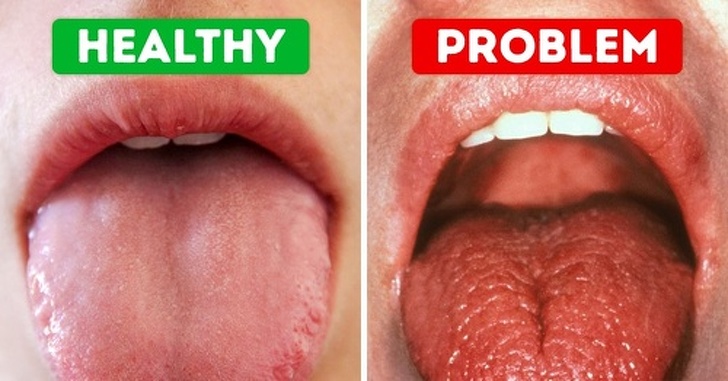
Gum disease is the most common oral manifestation for folks with psoriasis. Early signsred, swollen gums that bleed when you brushcan be easy to miss, especially when youre already dealing with itchy skin patches. If left unchecked, the inflammation can advance to periodontitis, where the supporting bone starts to erode, potentially leading to tooth loss. Understanding your dry mouth causes can also be crucial, as dry mouth exacerbates gum disease risk.
Oral psoriasis lesions
While it sounds rare, psoriasis can show up inside the mouth. You might notice welldefined whitetored plaques on the palate, tongue, or inner cheeks. Theyre often painless, which means you could be living with them for months without realizing theyre related to your skin condition. If you ever spot something that looks like pictures of oral psoriasis, its worth getting a professional opinion.
Tooth decay & dry mouth
Many systemic treatments for psoriasislike methotrexate or certain biologicscan reduce saliva flow, creating a drymouth environment thats a perfect breeding ground for cavities. Even the occasional craving for sugary comfort foods during a flare can tip the balance toward decay. For guidance on effective dry mouth treatment, consulting your healthcare provider is recommended.
Complications with dental implants & extractions
Thinking about a dental implant? Good news: its not offlimits, but youll need a thorough preoperative assessment. Studies show that implant failure rates are slightly higher in patients with active psoriasis, especially when the disease isnt wellcontrolled. Tooth extraction can also be slower to heal, so discussing your psoriasis status with the oral surgeon is essential.
Checklist for patients
- Tell your dentist you have psoriasis (and any meds youre on).
- Ask about prophylactic antibiotics before major surgery.
- Schedule cleanings every 34months if you have moderatetosevere disease.
- Request a periodontal evaluation before any implant.
Managing Dental Health
Daily oralcare routine that works
Think of your mouth as a tiny ecosystem that needs the right balance of cleaning, protection, and nourishment.
- Toothpaste: Choose a fluoride formula thats free of sodium lauryl sulfate (SLS) SLS can irritate sensitive oral tissue, and many people with psoriasis report less discomfort with SLSfree options. Look for soothing agents like aloe or chamomile for that extra calming effect.
- Brushing: Use a softbristle brush and gentle circular motions. Two minutes, twice a day, is the sweet spot.
- Floss & interdental cleaners: These get rid of plaque that a brush cant reach, reducing inflammatory load.
- Antimicrobial mouthwash: An alcoholfree rinse with chlorhexidine or essential oils can lower bacterial counts without drying out the mouth.
Professional dental care tips
Dont wait until you feel a twinge to see the dentist. With psoriasis, regular professional cleanings are a gamechanger. Aim for a visit every three months, and be upfront about your condition. Your dentist might want to monitor pocket depths more closely or adjust cleaning techniques to avoid traumatizing inflamed gums. Also, consider dry mouth prevention strategies as part of your routine care to protect against further complications from reduced saliva flow.
Lifestyle factors that help both conditions
Whats fascinating is how much the same habits that calm your skin also benefit your gums.
- Antiinflammatory diet: Omega3 rich foods (salmon, walnuts), plenty of leafy greens, and limited refined sugars can keep both the skin and gum pathways quieter.
- Stress management: Stress spikes cortisol, which can flare psoriasis and weaken gum immunity. Simple mindfulness, short walks, or a favorite hobby can make a big difference.
- Sleep hygiene: Aim for 79hours. Quality sleep helps the body repair both skin and periodontal tissue.
Sample 7day oralhealth planner
| Day | Morning | Evening |
|---|---|---|
| Mon | Brush + fluoride toothpaste | Floss + chlorhexidine rinse |
| Tue | Brush + SLSfree toothpaste | Interdental brush + water rinse |
| Wed | Brush + herbal mouthwash | Floss + fluoride rinse |
| Thu | Brush + fluoride toothpaste | Floss + chlorhexidine rinse |
| Fri | Brush + SLSfree toothpaste | Interdental brush + water rinse |
| Sat | Brush + herbal mouthwash | Floss + fluoride rinse |
| Sun | Brush + fluoride toothpaste | Relax no extra steps needed! |
When to involve a specialist
If you notice persistent bleeding, noticeable bone loss on Xrays, or oral plaques that wont go away, its time to see a periodontist. In more complex caseslike planning a dental implant while on biologic therapycoordinating care between your dermatologist and oral surgeon can dramatically improve outcomes.
Casestudy snippet
Maria, 42, lived with psoriatic arthritis for eight years. When she needed a singletooth implant, her dentist consulted her rheumatologist. By timing the procedure just after a biologic infusion and prescribing a short course of antibiotics, Marias implant integrated beautifully, and her gum health stayed stable for over two years.
Resources & Trusted Sources
Key scientific papers
For the curious mind, the following peerreviewed articles offer deeper insight:
- 2018 cohort on psoriasis & periodontitis (PubMed)
- 2020 systematic review linking systemic inflammation to oral health (Journal of Dermatology)
- 2021 study on psoriatic arthritis and advanced dental disease (Dental Research Journal)
- 2023 PeerJ article on bidirectional relationship (open access)
Patientfocused tools
The American Dental Association (ADA) provides an easytofollow oralhygiene guide, while the National Psoriasis Foundation (NPF) offers a downloadable DentalHealth Checklist for Psoriasis Patients. Both are free and highly practical.
Where to find images of oral psoriasis
If you want visual reference, licensed casereport images are available through reputable medical journals and the NPFs image library. Always ensure the source grants permission before reuse.
Conclusion
Living with psoriasis doesnt have to mean compromising on your smile. By understanding the shared inflammatory pathways, watching for early gum warnings, and pairing a gentle yet thorough oralcare routine with regular professional checkups, you can keep both your skin and teeth in good shape. Remember: communication is keylet your dentist know about your skin condition and any medications youre taking. If youve tried any of these tips or have questions, drop a comment below. Your experience could help someone else navigating the same crossroads. Lets keep the conversation (and our gums) healthy together.
FAQs
Can psoriasis cause gum disease?
Yes. Studies show people with psoriasis are 2‑3 times more likely to develop gingivitis or periodontitis due to shared inflammatory pathways.
What oral signs should I watch for if I have psoriasis?
Look for red, swollen gums that bleed easily, white‑to‑red plaques on the palate or tongue, dry mouth, and any persistent tooth sensitivity.
Do psoriasis medications affect my teeth?
Some systemic drugs (e.g., methotrexate, certain biologics) can reduce saliva flow, increasing the risk of cavities and slowing healing after dental work.
How often should I see the dentist?
Schedule professional cleanings every 3‑4 months and request a full periodontal evaluation, especially if your psoriasis is moderate‑to‑severe.
Are dental implants safe for people with psoriasis?
Implants are possible, but they require a well‑controlled disease state and a pre‑operative assessment; coordination between your dermatologist and oral surgeon improves success.