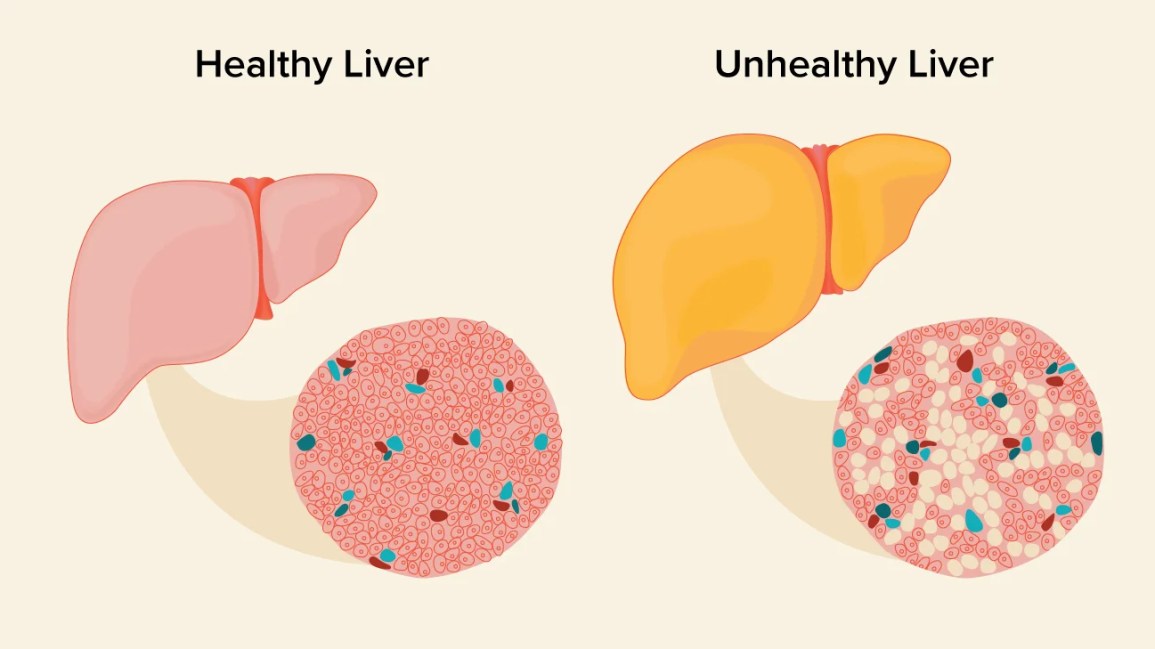
Is It Truly Hereditary?
What does hereditary actually mean?
In everyday conversation hereditary often gets tossed around like a buzzword, but medically it means a trait passed down through DNA. Its different from familial, which can include shared habits, and polygenic, where many genes each add a small piece to the puzzle. Understanding these nuances helps you see where the science ends and where your daily choices begin.
How strong is the genetic link?
Researchers have crunched the numbers and found that about 3040% of the risk for nonalcoholic fatty liver disease (NAFLD) is genetic. One sibling study reported a 59% similarity, while parentchild pairs showed up to a 78% overlap. Below is a quick snapshot:
| Relationship | Heritability Estimate |
|---|---|
| Siblings | 59% |
| ParentChild | 78% |
| General Population | 3040% |
Which genes are most often involved?
The heavy hitters are PNPLA3I148M, TM6SF2, GCKR, and MBOAT7. If you carry the PNPLA3 variant, your liver cells tend to stash more fat, making you more prone to NAFLD even if youre relatively fit. Think of these genes as tiny fatstorage managers that sometimes get a little overenthusiastic.
Can genetic testing confirm my risk?
There are consumer panels (like those offered by 23andMe) and clinical tests that look for the variants mentioned above. The upside is you get a headsup; the downside is that genes only tell part of the story. A positive result doesnt guarantee disease, and a negative result doesnt mean youre safe. If youre curious, talk to your doctor about whether a fatty liver inheritance panel fits into your overall health plan.
Does family history outweigh lifestyle?
Short answer: no. While a family history can tip the scales, the biggest lever you control is what you put on your plate and how you move your body. MedlinePlus notes that variations in several genes as well as lifestyle choices contribute to NAFLD. In other words, even if the cards are stacked against you, you can still play a winning hand.
Your Family Risk
Should I get screened if a relative has NAFLD?
The American Association for the Study of Liver Diseases (AASLD) recommends a liver ultrasound or FibroScan if you have a firstdegree relative (parent, sibling, or child) with NAFLD. Adding a simple blood panel for liver enzymes (ALT, AST) can catch early changes before you feel any symptoms.
How does heredity affect life expectancy?
Studies on show that the overall outlook is heavily tied to whether the disease progresses to fibrosis or cirrhosis. Early detection and lifestyle changes can bring life expectancy back to the baseline for most people, even those with a strong genetic predisposition.
Is fatty liver reversible if it runs in the family?
Absolutely. A 710% weight loss (think shedding 1520pounds for someone at 180lb) can cut liver fat by roughly onethird. Combine that with a Mediterraneanstyle diet, regular exercise, and limiting sugary drinks, and many people see their liver clear up on followup imaging.
Are there treatments that target the genetic root?
Scientists are testing drugs that specifically silence the PNPLA3 defectcalled antisense oligonucleotides. These are still in clinical trials, so right now the best genetic treatment is a proactive lifestyle that neutralizes the genes effect.
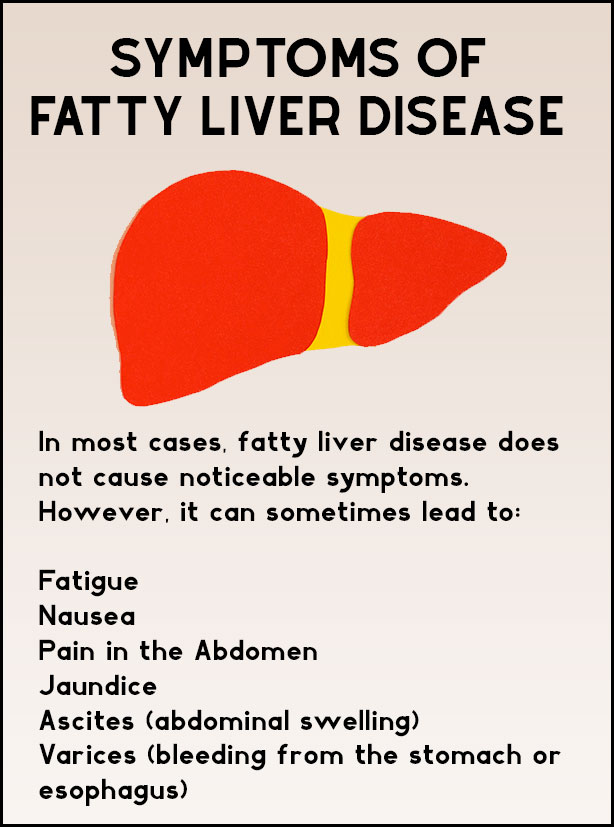
How do symptoms differ in women?
Women, especially after menopause, can experience a slightly higher risk of progressing to fibrosis. Hormonal shifts may make the liver more vulnerable, and symptoms such as fatigue, mild abdominal discomfort, or unexplained weight gain can sometimes be brushed off as just getting older. Being aware of these signsoften listed under fatty liver symptoms in femaleshelps you act sooner.
Is fatty liver dangerous or curable?
It can be dangerous if it progresses to nonalcoholic steatohepatitis (NASH), fibrosis, or cirrhosis. However, the term curable is more nuanced. The underlying fat accumulation is highly reversible, but chronic damage (scar tissue) may be permanent. Thats why early intervention matters.
Lifestyle Beats Genes
Diet tweaks that beat the genes
Think of your liver as a kitchen: the better the ingredients, the cleaner the dishes. Embrace a Mediterranean patternlots of olive oil, leafy greens, fish, nuts, and whole grains. Cut back on fructose (found in soda, candy, and even some fruit juices) and saturated fats (think fries and fatty cuts of meat). A sample day could look like this:
- Breakfast: Greek yogurt with berries, a drizzle of honey, and a sprinkle of walnuts.
- Lunch: Quinoa salad with cherry tomatoes, cucumber, feta, and a lemonoliveoil dressing.
- Dinner: Grilled salmon, roasted broccoli, and a side of lentils.
Exercise routines proven to lower liver fat
Movement is medicine. Aim for at least 150minutes of moderateintensity aerobic activity per weekthink brisk walking, cycling, or dancing. Add resistance training twice a week (bodyweight squats, pushups, or light dumbbells) to boost muscle mass, which in turn helps the liver burn fat.
Weightloss goals & realistic timelines
Dropping 710% of your body weight isnt as scary as it sounds. If youre 200lb, thats 1420lb. Set a manageable goal of 12lb per weekhealthier and more sustainable. A quick progress calculator you can use is:
Target loss = Current weight 0.070.10Weeks needed Target loss 1.5
Supplement & medication guide
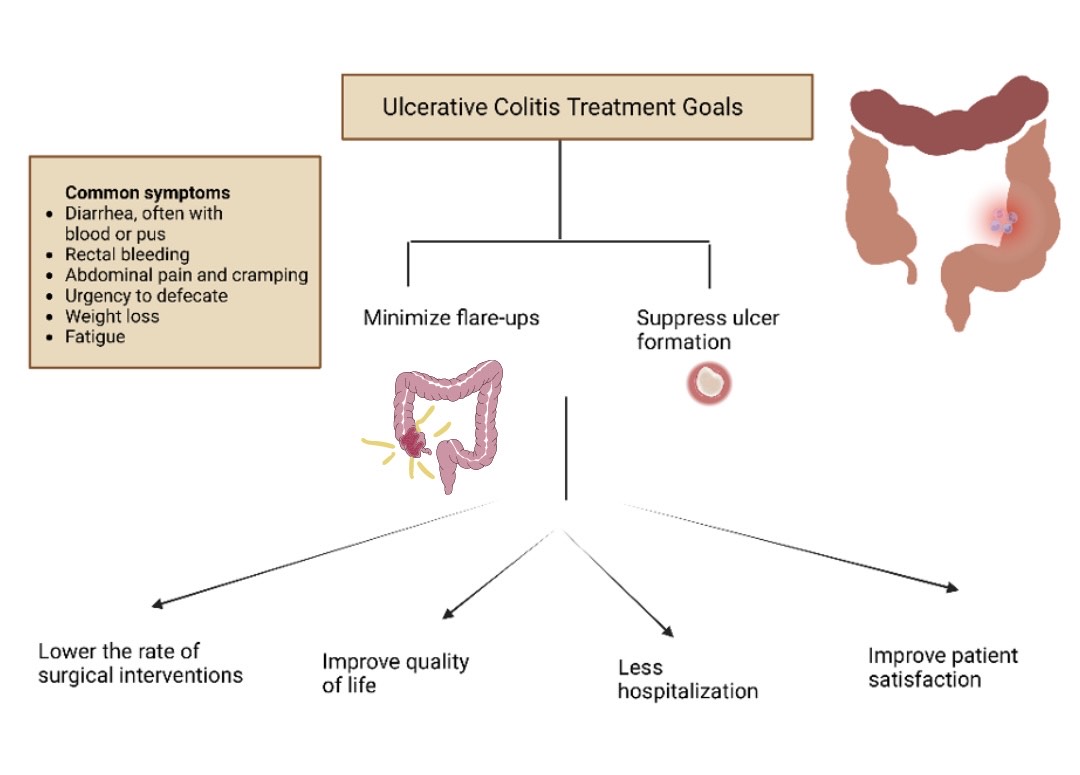
Some evidence points to coffee (yes, your morning brew) as a liver protector. VitaminE may help nondiabetics, while pioglitazone and newer GLP1 agonists (like semaglutide) are being studied for NASH. Always run these by a hepatologist before starting. For people also managing digestive issues, consider safe complementary optionssee guidance on ulcerative colitis supplements if you have overlapping inflammatory bowel disease, since choices can affect liver and gut together.
Monitoring progress
Schedule a repeat liver ultrasound or FibroScan every 612months, especially if you have a family history. Keep an eye on liver enzymes in your routine blood work; a steady decline often mirrors improvements in the liver.
Frequently Asked Questions
Is fatty liver hereditary?
Yes family studies show a 3040% genetic contribution, but lifestyle determines whether it actually develops.
Can I get genetic testing for fatty liver?
Certain labs offer panels for PNPLA3, TM6SF2, and other risk genes, but the results indicate risk, not certainty.
Is fatty liver reversible?
In most cases, losing 710% body weight and improving diet can fully reverse liver fat, even when genetics play a role.
Does having a family history mean a shorter life expectancy?
Not necessarily; early detection and treatment can bring life expectancy back to normal.
Are there any drugs that fix the genetic cause?
Emerging therapies targeting PNPLA3 are in trials, but no approved genespecific drugs exist yet.
Further Reading Links
To dive deeper, check out reputable medical sources such as MedlinePlus and the Mayo Clinic for uptodate research on NAFLD and its genetic aspects. Adding these trusted references into your knowledge base can help you feel more confident when discussing options with your healthcare provider.
Conclusion
Genetics does raise the odds of developing a fatty liver, but its far from a life sentence. By knowing your family history, getting screened early, and adopting a liverfriendly lifestyle, you can often reverse the condition and protect your longterm health. If a parent or sibling has NAFLD, consider chatting with your doctor about a simple genetic panel and a personalized prevention plan. Small, consistent changeslike swapping soda for water, strolling after dinner, or adding a coffee breakcan make a huge difference. Take the first step today, and give your liver the fresh start it deserves.