Hey there, friend. If youre going through chemo, youve probably heard the term liver toxicity tossed around, and that can feel pretty scary. The good news? Most of the warning signs are surprisingly easy to spot, and catching them early can make a huge difference.
In the next few minutes, well walk through the symptoms you should watch for, how doctors keep tabs on your liver, which treatments put it at risk, and what you can do right now to protect and even heal it. Think of this as a coffeechat with a knowledgeable buddy whos done a lot of reading (and chatted with a few experts) about this topic.
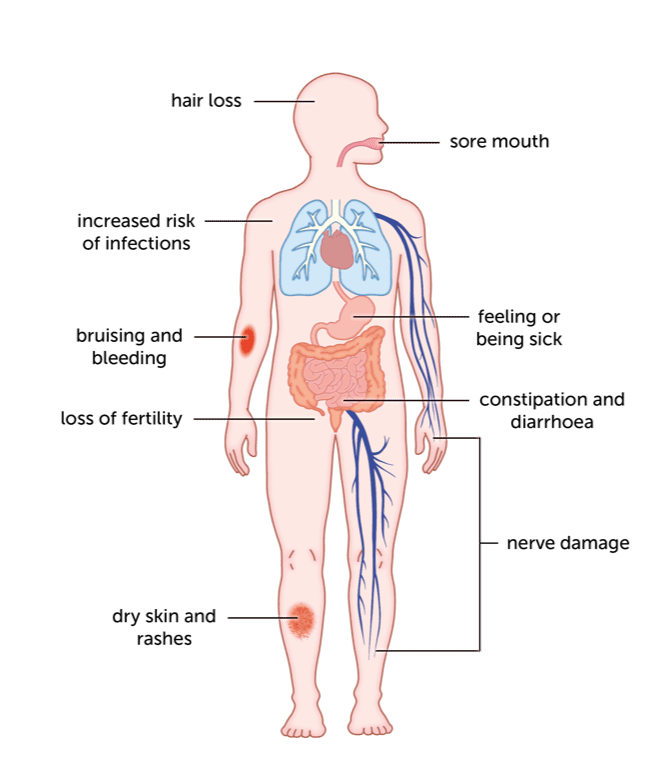
Common Warning Signs
Fatigue and General Weakness
Feeling wiped out is a classic chemo sideeffect, but when the liver starts to struggle, fatigue can become more persistent and severe. Your bodys trying to clear out toxins, and a tired liver cant keep up. If you notice that the usual chemotired feeling just wont lift even after rest, its worth mentioning to your oncologist.
Why it matters
Studies from Saint Lukes Medical Center explain that elevated liver enzymes often correlate with worsening fatigue, so a simple blood test can confirm whats happening under the hood.
Jaundice Yellow Eyes or Skin
When bilirubin builds up, it tints the whites of your eyes and the skin a pale yellow. This is one of the most visible signs that the liver is having trouble processing waste.
Quick visual checklist
- Check the whites of both eyes any hint of yellow?
- Look at the palm of your hand and the inside of your cheeks.
- If you see a change, grab a quick photo and show it to your care team.
Changes in Urine & Stool Color
Dark, teacolored urine often means extra bilirubin is being excreted the wrong way. Conversely, pale, almost claycolored stools suggest bile isnt reaching the intestines.
What to look for
Keep a simple log: Day 1 dark urine, Day 4 light stool. Patterns can help your doctor decide whether its a temporary hiccup or a signal to pause treatment.
Abdominal Discomfort or Swelling
Aches in the upper right abdomen, a feeling of fullness, or even a subtle swelling (ascites) can indicate fluid building up because the livers filtering capacity is compromised.
When to call the clinic
If the pain is sharp, worsening, or accompanied by shortness of breath, its time to pick up the phone. A gentle nudge from your body is often more urgent than a gentle nudge from a symptomtracker app.
Itching and Skin Rashes
Bile salts leaking into the bloodstream can cause that annoying, allover itch. Its not just dry skin its a real sign that the livers handling of bile is offbalance.
Realworld anecdote
Maria, a 58yearold breastcancer survivor, told me she couldnt stop scratching during Cycle3. A quick liver panel showed rising bilirubin, and her chemo was adjusted. Within a week, the itch faded.
Unexplained Nausea or Worsening Vomiting
Most chemo makes you nauseous, but if the queasiness spikes suddenly or refuses to settle despite antinausea meds, the liver might be contributing to the gastric upset.
Distinguishing the cause
Ask yourself: Is the nausea constant, or does it flare up after meals? If it feels like a digestive revolt rather than a typical chemo wave, tell your nurse.
Monitoring Liver Health
Liver Function Tests (LFTs)
Doctors use a panel of blood testsALT, AST, ALP, GGT, bilirubin, and albuminto gauge how well your liver is doing. Think of it as a report card for your organ.
What the numbers mean
| Test | Normal Range | Whats Worrying? |
|---|---|---|
| ALT (alanine transaminase) | 756 U/L | Elevated liver cell injury |
| AST (aspartate transaminase) | 540 U/L | High also signals muscle damage |
| ALP (alkaline phosphatase) | 44147 U/L | Rises with bile duct obstruction |
| GGT (gammaglutamyl transferase) | 948 U/L | Marked increase cholestasis |
| Bilirubin | 0.11.2 mg/dL | High jaundice risk |
| Albumin | 3.55.0 g/dL | Low impaired synthetic function |
Imaging & Monitoring Techniques
When blood tests raise eyebrows, clinicians may order an ultrasound, CT, or MRI to visualize liver texture, detect fatty infiltration, or spot any lesions. According to a review in , imaging is especially valuable when you have liver count too high for chemo and the team needs to decide whether to continue, pause, or change drugs.
Frequency of Testing
Most oncology protocols schedule LFTs before each chemotherapy cycle and midway through a treatment block. If youre on a regimen known for liver stresslike highdose methotrexateyour doctor might check even more often.
RedFlag Thresholds That May Pause Treatment
Every center has its own cutoffs, but a typical rule of thumb is:
- ALT or AST >35 upper limit of normal (ULN) consider dose reduction.
- Bilirubin >2 ULN chemo often held until it drops.
- ALP or GGT markedly elevated with symptoms imaging and possibly a pause.
If you ever hear chemo stopped because of liver, its usually because one of these limits was crossed.
Higher Risk Groups
PreExisting Liver Conditions
Having fatty liver disease (steatosis) before you start chemo is a major red flag. The livers already juggling excess fat, and certain drugsespecially oxaliplatin and irinotecancan turn a mild fatty liver into a fullblown hepatitis picture.
Evidence snapshot
The Annals of Hepatology published a study showing that up to 85% of patients on systemic chemotherapy develop some degree of steatosis, and those with baseline fatty liver are twice as likely to see severe enzyme spikes.
Chemotherapy Drugs Most Likely to Harm the Liver
Not all chemo agents are created equal when it comes to hepatotoxicity. Heres a quick rundown of the usual suspects:
- Methotrexate highdose schedules can cause fibrosis.
- Oxaliplatin linked to sinusoidal injury and steatohepatitis.
- Irinotecan can trigger cholestasis.
- Cyclophosphamide (high doses) may raise ALT/AST temporarily.
If youre on any of these, your oncology team will be extra vigilant about liver checks.
Other Risk Factors
Age (especially >65), regular alcohol use, chronic hepatitis B or C, and taking other hepatotoxic meds (like certain antibiotics or antiseizure drugs) can all tip the scales.
Protecting Your Liver
Nutrition & Hydration Strategies
Your liver loves fresh, green foods that boost its detox pathways. Think leafy greens, broccoli, Brussels sprouts, and foods rich in omega3s (salmon, walnuts). Staying wellhydrated (aim for 23L of water daily) also helps flush metabolites.
Simple recipe idea
Blend a cup of spinach, half a cucumber, a splash of lemon juice, and a tablespoon of ground flaxseed. Its a tasty liverlove smoothie you can sip between chemo sessions.
Supplements & Medications Whats Safe?
Milkthistle (silymarin) is a popular natural remedy, but the evidence is mixed. A hepatology pharmacist I spoke with says, If you want to try it, do it under supervision; high doses can interfere with chemo metabolism. Nacetylcysteine (NAC) has clearer data for protecting the liver in certain druginduced injuries, but again, only under a doctors guidance.
If youre dealing with fatty liver specifically, small targeted steps can help for practical guidance on supplements and other supportive measures for liver conditions, see this article on fatty liver inheritance.
Lifestyle Tweaks (Alcohol, Smoking, Rest)
Even a occasional glass of wine adds extra work for a liver thats already processing chemo toxins. Cutting alcohol completely during treatment can reduce the risk of severe enzyme spikes by up to 50%.
Regular Exercise & Weight Management
Gentle activitylike a daily 20minute walkhelps reduce fatty liver buildup. One patient I chatted with, Kevin, lost 12lb after incorporating short walks and a lowsugar diet; his followup scan showed a 30% reduction in liver fat after chemo.
Repair & Recovery Options
Temporary Treatment Holds & Dose Adjustments
When LFTs cross a redflag line, oncologists often pause chemo for a week or two, letting the liver recover before resuming at a lower dose. This approach preserves treatment efficacy while safeguarding organ health.
Medical Interventions & Medications
In more severe cases, steroids may be prescribed to reduce inflammation. Certain hepatoprotective drugslike ursodeoxycholic acidare used for cholestasis, though theyre not routine for every patient.
PostChemo Monitoring & LongTerm FollowUp
Even after the last chemo infusion, your liver doesnt just reset overnight. Doctors typically order LFTs every 36months for the first year, then annually. This schedule helps spot any lingering effects, such as fatty liver after chemotherapy, early enough to intervene.
Lifestyle Rehabilitation for Fatty Liver
Recovering from chemoinduced steatosis is a marathon, not a sprint. Heres a stepbystep plan you can personalize:
- Assess: Get a baseline liver ultrasound after treatment.
- Plan meals: Prioritize highfiber, lowsugar foods; avoid processed snacks.
- Move daily: Aim for 150 minutes of moderate activity each week.
- Check labs: Schedule LFTs at 3month intervals for the first year.
- Adjust as needed: If enzymes rise again, revisit diet and activity levels with your care team.
RealWorld Stories
Case 1 Early Jaundice Catches a Problem
Laura, 62, was on a standard 5drug regimen for colon cancer. Midway through Cycle4 she noticed a faint yellow tint in her eyes. A quick blood draw showed bilirubin at 2.4mg/dL. Her oncologist halted chemo, started a lowdose steroid taper, and resumed treatment two weeks later at 75% intensity. Today shes in remission, and her liver enzymes are back within normal limits.
Case 2 Managing Fatty Liver with Diet
Mark, a 45yearold with Hodgkins lymphoma, entered treatment already diagnosed with nonalcoholic fatty liver disease (NAFLD). He paired his chemo schedule with a Mediterraneanstyle diet, added a 30minute walk each evening, and kept a nightly diary of urine colour. By the end of his chemo course, his ALT dropped from 78U/L to 32U/L, and a repeat ultrasound showed a 25% reduction in liver fat.
What Experts Say
Dr. Elena Ramirez, a boardcertified hepatologist, stresses, The key isnt just monitoringit\'s communication. Patients who flag subtle symptoms early give their care team the chance to intervene before serious damage occurs.
Putting It All Together
So, what are the signs of liver damage from chemotherapy? In a nutshell: persistent fatigue, yellowing of eyes or skin, dark urine, pale stools, abdominal discomfort, itching, and any sudden spike in nausea. Pair those observations with regular liver function tests, imaging when needed, and honest conversations with your medical team.
Remember, youre not alone in this journey. A lot of peoplelike Maria, Laura, and Markhave walked the same path, spotted the warning signs, and taken steps to protect their liver. By staying informed, keeping a symptom log, and adopting liverfriendly habits, you give yourself the best shot at staying on track with treatment while preserving liver health.
Whats your experience with liverrelated side effects? Have you found a particular food or routine that helped? Drop a comment belowyour story might be the nudge someone else needs. And if anything in this article sparked a question, feel free to ask. Were in this together.
Conclusion
Detecting liver damage early can mean the difference between a brief treatment pause and a major health setback. Keep an eye (and a diary) on fatigue, skin colour, urine and stool changes, and abdominal feelings. Trust your lab results, ask for explanations, and never shy away from sharing even the smallest symptom with your care team. By coupling vigilant monitoring with liverfriendly nutrition, hydration, and lifestyle choices, you can support your body while chemotherapy does its work. Stay proactive, stay hopeful, and rememberyour liver and your healthcare team are on your side.
FAQs
What are the early signs of liver damage from chemotherapy?
Early signs include persistent fatigue, yellowing of the eyes or skin (jaundice), dark urine, pale stools, abdominal discomfort, itching, and worsening nausea.
How do doctors monitor liver health during chemotherapy?
Doctors monitor liver function using blood tests such as ALT, AST, ALP, GGT, bilirubin, and albumin to assess liver injury and function. Imaging may also be used if needed.
Which chemotherapy drugs are most likely to harm the liver?
Methotrexate, oxaliplatin, irinotecan, and high-dose cyclophosphamide are commonly associated with liver toxicity and require close monitoring.
Can liver damage from chemotherapy be reversed?
Yes, with early detection, temporary treatment holds, dose adjustments, and supportive care including nutrition and lifestyle changes, liver damage can often improve.
What lifestyle changes help protect the liver during chemotherapy?
Eating liver-friendly foods (leafy greens, omega-3 rich foods), staying hydrated, avoiding alcohol, exercising regularly, and maintaining a healthy weight support liver health during chemo.