What Is Functional Dysphagia
Simple definition
Functional dysphagia is the sensation that food or liquids are sticking, moving slowly, or getting hung up in the esophagus, but medical tests (endoscopy, barium swallow, manometry) dont show any physical blockage or muscle disorder. In short, its a symptom without a structural cause.
How it differs from mechanical dysphagia
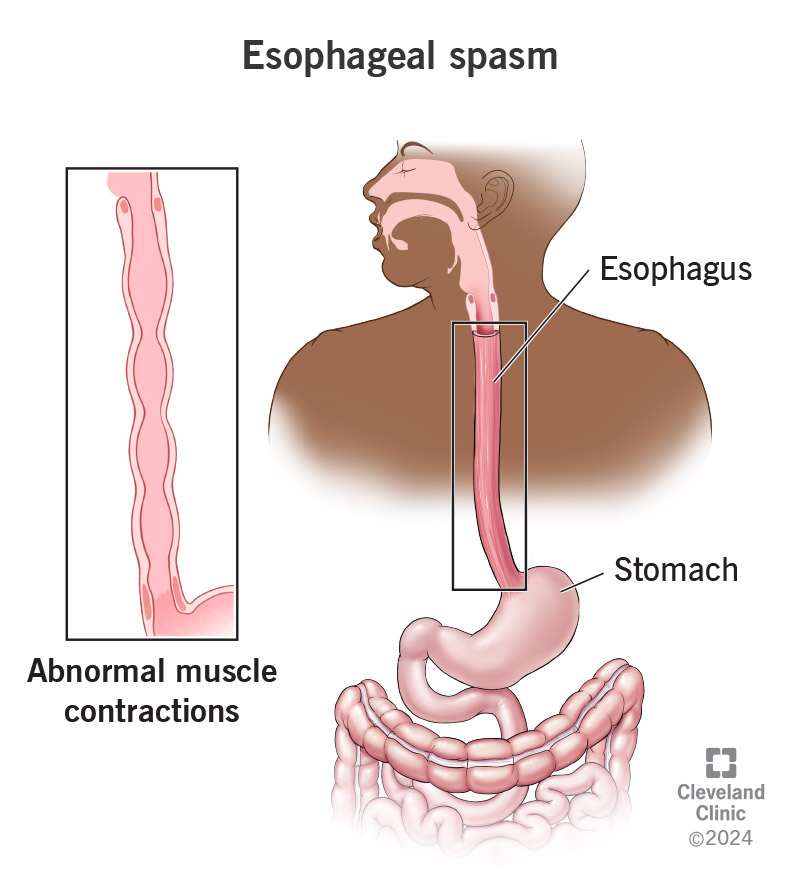
Think of the esophagus like a highway. A mechanical problem is like a construction zone that physically blocks traffic. Functional dysphagia, on the other hand, is like rushhour traffic where the road is clear but the flow feels jammed because the drivers (your nerves) are overly cautious.
| Aspect | Functional Dysphagia | Mechanical Dysphagia |
|---|---|---|
| Cause | Visceral hypersensitivity, anxiety, functional braingut dysregulation | Stricture, tumor, Schatzki ring, achalasia |
| Diagnostic findings | Normal endoscopy, normal manometry, no obstruction on imaging | Visible narrowing or abnormal motility on studies |
| Treatment focus | Behavioral therapy, stress management, swallow exercises | Endoscopic dilation, surgery, medication for acid reflux |
ICD10 coding
In the medical records world, functional dysphagia is usually coded under R13.10 (Dysphagia, unspecified). Some clinicians may also reference K22.2 (Globus sensation) when the feeling is primarily of a lump in the throat. Knowing the code can help you understand insurance paperwork and what your doctor is really looking at.
Symptoms & Warning Signs
Core symptoms youll notice
- Feeling of food stuck or delayed transit, especially with solids.
- Intermittent sensation of a lump in the throat (often called globus).
- Mild chest discomfort that isnt sharp or burning.
- Occasional coughing or throat clearing after meals.
Redflag signs that need urgent attention
While functional dysphagia is usually benign, certain signs suggest a more serious underlying issue. If you experience any of the following, see a doctor right away:
- Unexplained weight loss.
- Persistent vomiting or regurgitation.
- Severe pain while swallowing.
- Difficulty breathing or a choking sensation.
What can trigger the symptoms?
Stressful days, large meals, carbonated drinks, or lying down shortly after eating can make the sensation flare up. Many people also report that caffeine, alcohol, and spicy foods amplify the feeling of something being stuck.
Why It Happens
Visceral hypersensitivity
Research points to an overresponsive nervous system in the esophaguswhat doctors call visceral hypersensitivity. The nerves send pain signals even when the food is moving normally. A 2023 review in highlighted this as the leading hypothesis for functional dysphagia.
Functional dysphagia and anxiety
Theres a twoway street between anxiety and swallowing problems. Anxiety can heighten the braingut reflex, making the esophagus feel tighter; conversely, the unsettling sensation of food stuck can increase anxiety. Think of it as a nervous loop that keeps feeding itself.
Lifestyle and dietary factors
Smoking, heavy caffeine intake, and certain medications (like antihistamines or calciumchannel blockers) can irritate the esophageal lining, making it more prone to hypersensitivity. Even everyday habits like eating too fast can trigger the symptom.
Medications that mimic dysphagia
| Medication | Potential Effect |
|---|---|
| Antihistamines | Dry mouth thicker bolus feeling of stuck food |
| Calciumchannel blockers | Relaxed lower esophageal sphincter reflux irritation |
| NSAIDs | Esophageal irritation heightened sensitivity |
How Its Diagnosed
Diagnosis of exclusion
Because functional dysphagia has no visible cause, doctors first rule out structural problems. That usually means an upper endoscopy, a barium swallow, and sometimes esophageal manometry. When all those tests come back normal, the diagnosis shifts toward a functional disorder.
Rome IV criteria for esophageal functional disorders
The Rome IV consensus (published by the International Foundation for Functional Gastrointestinal Disorders) lists specific criteria: recurrent dysphagia, normal endoscopic findings, and symptoms not explained by other medical conditions. You can find the full checklist .
Selfscreening tools
Several questionnaires help gauge severity. The EAT10 (Eating Assessment Tool) asks ten simple questions about swallowing difficulty. A quick internet search for functional dysphagia quizlet also pulls up usergenerated flashcards that can give you a rough idea of what clinicians look for.
When to see a specialist
If youve tried basic lifestyle tweaks and your symptoms persist, a referral to a gastroenterologist or a speechlanguage pathologist (SLP) is warranted. SLPs specialize in swallow therapy and can run specialized tests like highresolution impedance manometry.
Functional vs Mechanical
Key clinical differences
Functional dysphagia is primarily a sensory issue without an anatomical blockage, while mechanical dysphagia stems from a physical obstruction or motility disorder. The response to treatment is also distinctbehavioral and stressreduction strategies work best for functional cases, whereas mechanical cases often require procedural intervention.
Quick comparison
| Feature | Functional Dysphagia | Mechanical Dysphagia |
|---|---|---|
| Onset | Gradual, often after stress spikes | Sudden or progressive with food impaction |
| Test results | Normal endoscopy/manometry | Abnormal imaging or motility study |
| Primary treatment | CBT, swallow exercises, diet adjustments | Dilation, surgery, acidsuppression meds |
| Typical triggers | Anxiety, large meals, carbonated drinks | Stricture, tumor, Schatzki ring |
Realworld story
Emily, a 38yearold teacher, went to three different doctors over two years. Each endoscopy was clean, but she kept hearing no blockage. After a referral to an SLP, she learned that her highstress job and frequent caffeine intake were amplifying her esophageal sensitivity. With a mix of CBT and swallow exercises, her stuck feeling dropped from daily to once a month. Emilys journey shows why distinguishing functional from mechanical is crucial.
Treatment & SelfHelp
Psychological interventions
Because anxiety often fuels functional dysphagia, cognitivebehavioral therapy (CBT) and mindfulness practice can break the anxietyswallow loop. A 2024 clinical trial published in found that patients who completed an eightweek CBT program reported a 45% reduction in dysphagia scores.
Speechlanguage therapy and swallow exercises
SLPs teach techniques like the effortful swallow (harder swallow to boost muscle activation) and the Mendelsohn maneuver (holding the throat open longer). Consistent practiceabout 10 minutes, three times a daycan improve esophageal coordination and reduce the stuck sensation.
Medication options
When anxiety is a major driver, lowdose tricyclic antidepressants (e.g., amitriptyline) or selective serotonin reuptake inhibitors (SSRIs) can dampen nerve hypersensitivity. Gabapentin is another offlabel option, but always discuss risks with your doctor.
Lifestyle tweaks that really help
- Eat smaller bites and chew thoroughly.
- Stay upright for at least 30 minutes after meals.
- Limit carbonated drinks, caffeine, and very spicy foods.
- Practice a simple breathing exercise before meals: inhale deeply, hold for three seconds, exhale slowly while visualizing the food moving smoothly.
When surgery or endoscopy is considered
Only after a thorough workup that rules out mechanical causes would a physician think about dilation or other procedures. In functional dysphagia alone, those invasive steps rarely bring lasting relief and can create unnecessary risk.
Final Thoughts & Action
Functional dysphagia can feel like an invisible obstacletheres no clear blockage to point at, yet the discomfort is very real. The good news? Most people find relief by addressing the braingut connection, adopting gentle swallow exercises, and managing anxiety. If you recognize the symptoms described above, start with a simple selfscreen (the EAT10) and talk to your primary care provider about a referral to a gastroenterologist or speechlanguage pathologist.
Take one step today: write down the times you notice the stuck feeling, note what you ate, and how stressed you felt. Share that log with your doctorthis concrete information helps them zero in on the functional aspect rather than chasing every possible mechanical cause.
Have you tried any of the tips above? Do you have a story about how anxiety or stress impacted your swallowing? Drop a comment below, or join the conversation on the functional dysphagia . Together we can make this confusing condition a little less mysterious and a lot more manageable.
FAQs
What exactly is functional dysphagia?
Functional dysphagia is the feeling that food or liquid is stuck in the throat even though all medical tests (endoscopy, barium swallow, manometry) show no structural blockage or muscle disorder.
How can I tell if my dysphagia is functional or mechanical?
Functional dysphagia usually has normal test results and triggers like stress, large meals, or carbonated drinks. Mechanical dysphagia shows up as a narrowing, ring, tumor, or abnormal motility on imaging or endoscopy.
Which lifestyle changes help reduce functional dysphagia symptoms?
Eat smaller bites, chew thoroughly, stay upright 30 minutes after meals, limit caffeine, alcohol, spicy foods, and practice calming breathing exercises before eating.
Can therapy really improve the “stuck” feeling?
Yes. Cognitive‑behavioral therapy (CBT) and mindfulness reduce anxiety‑driven hypersensitivity, while speech‑language therapy teaches swallow exercises (effortful swallow, Mendelsohn maneuver) that improve esophageal coordination.
When should I see a specialist for my swallowing problems?
If symptoms persist despite basic changes, or if you notice red‑flag signs such as unexplained weight loss, severe pain, vomiting, or breathing difficulty, get a referral to a gastroenterologist or a speech‑language pathologist.