If youre dealing with gut turmoil that swings between constipation and diarrhea, youre probably facing IBSM the mixedtype of irritable bowel syndrome. It brings unpredictable bowel habits, cramping, and that lingering feeling of urgency.
Below youll discover why IBSM happens, how to spot its key signs, which foods should stay off your plate, and the most effective treatment routes backed by gastroenterology experts. Lets dive in, friendtofriend.
What Is IBS-M?
Definition & How It Differs From Other IBS Types
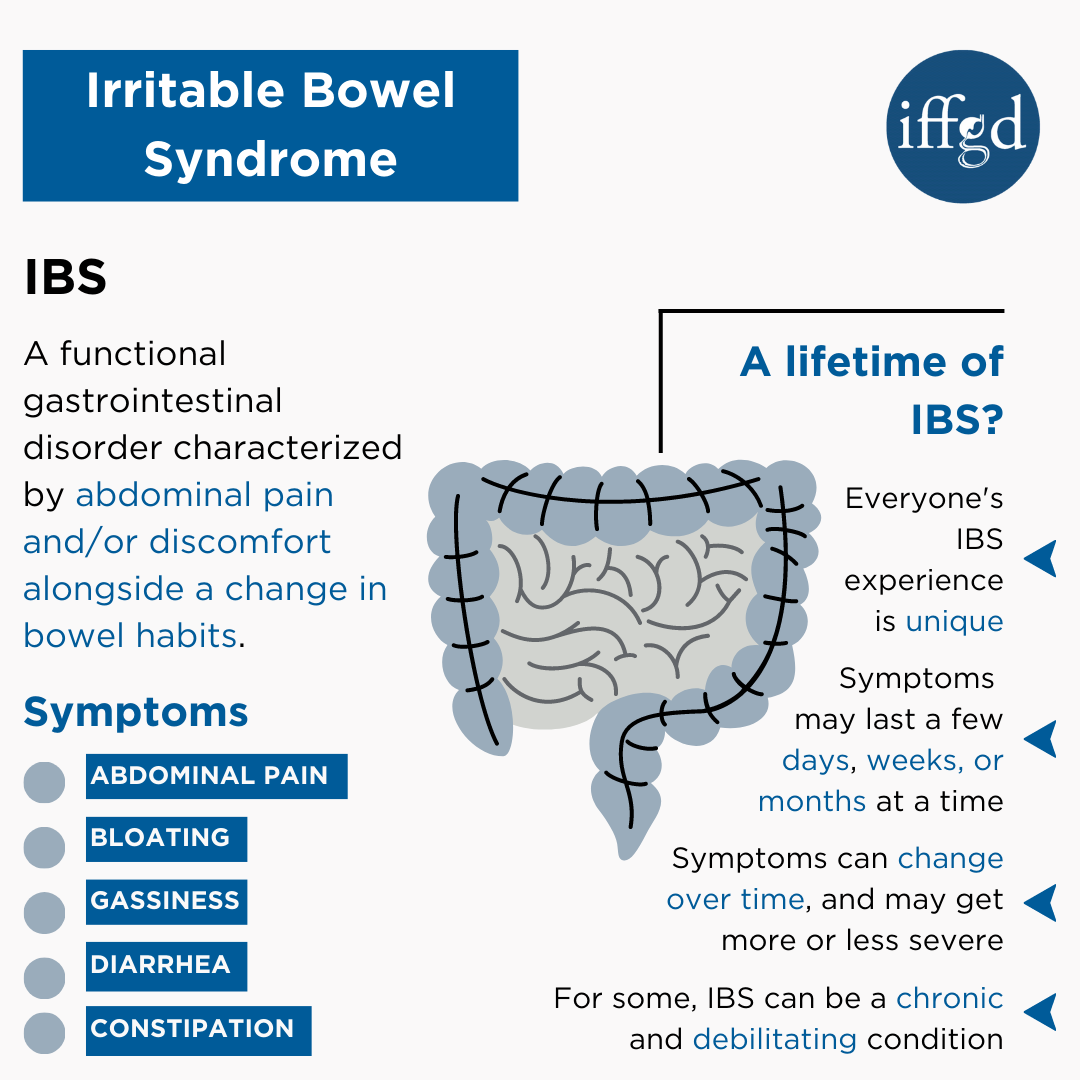
IBSM (mixed) is a chronic functional disorder where the colon alternates between diarrheadominant (IBSD) and constipationdominant (IBSC) episodes. Unlike the steadystate patterns of IBSD or IBSC, IBSM is a rollercoaster that can switch from loose stools one day to hard, painful poop the next.
Who Gets IBS-M? (Prevalence & Risk Groups)
About 1015% of adults worldwide report IBS symptoms, and roughly onethird of those fall into the mixed category. Women are about twice as likely as men to be diagnosed, often in their 20s to 40s. Family history, high stress levels, and prior gastrointestinal infections raise the odds.
Quick Quiz: Do You Have IBSM?
Answer yes to at least two of these statements:
- My bowel movements swing from watery to hard within a week.
- I experience abdominal cramping that eases after I go.
- Stress or certain foods make my symptoms flare up.
- I notice frequent gas, bloating, or mucus in my stool.
If you nodded along, you might be dealing with IBSM. A proper diagnosis will confirm it.
Main Causes & Triggers
Physiological Roots
The gutbrain axisa twoway street linking our brain and digestive tractcan get out of sync. When signals misfire, the colons muscles contract erratically (visceral hypersensitivity) and motility becomes uneven, leading to the mixed stool pattern.
Common Lifestyle & Dietary Triggers
Stress, inadequate sleep, and sedentary habits often amplify symptoms. On the food side, highFODMAP items (those that ferment quickly in the gut), caffeine, and alcohol are frequent culprits.
Top 10 IBSM Triggers vs. How They Affect You
| Trigger | Typical Effect | Simple Swap |
|---|---|---|
| Wheat (gluten) | Bloating & constipation | Glutenfree oats or rice flour |
| Onions & garlic | Gas & diarrhea spikes | Use chives or asafoetida powder |
| Coffee | Increased urgency | Switch to decaf or herbal tea |
| Artificial sweeteners | Loose stools | Natural sweeteners like maple syrup |
| Highfat fried foods | Slowed gut motility | Bake or grill instead of fry |
| Dairy (lactose) | Cramping & gas | Lactosefree milk or almond milk |
| Beans & lentils | Excessive gas | Soak and rinse, or use canned lowFODMAP versions |
| Carbonated drinks | Bloating & belching | Still water or infused plain water |
| Stressful workdays | Allover flareup | Brief mindfulness breaks (5min) |
| Irregular meals | Unpredictable bowel rhythm | Eat at consistent times, 34 small meals |
Key Symptoms Overview
Core Symptom Checklist
- Alternating diarrhea and constipation.
- Abdominal cramping that eases after a bowel movement.
- Urgent need to go, sometimes with little warning.
- Bloating, excess gas, and occasional mucus in stool.
When Symptoms Overlap With Other Conditions
IBSM can mimic inflammatory bowel disease (IBD), celiac disease, or even colon cancer. Redflag signs like unexplained weight loss, blood in stool, or nighttime diarrhea warrant immediate medical evaluation.
Infographic Idea (for future visual)
Imagine a dayinthelife timeline showing a morning flareup, a midday calm after a lowFODMAP lunch, an evening stresstrigger, and a soothing bedtime routine. Such a visual helps readers see the pattern.
How Its Diagnosed
Rome IV Criteria
Doctors rely on the RomeIV questionnaire, which asks about symptom frequency, pain location, and relationship to bowel movements. Meeting the criteria plus ruling out other diseases leads to an IBSM diagnosis.
Tests Physicians May Order
Standard labs (CBC, thyroid panel) and stool studies rule out infection. If alarm symptoms appear, a colonoscopy may be recommendednot because IBSM needs it, but to exclude more serious pathology.
What to Bring to Your Appointment
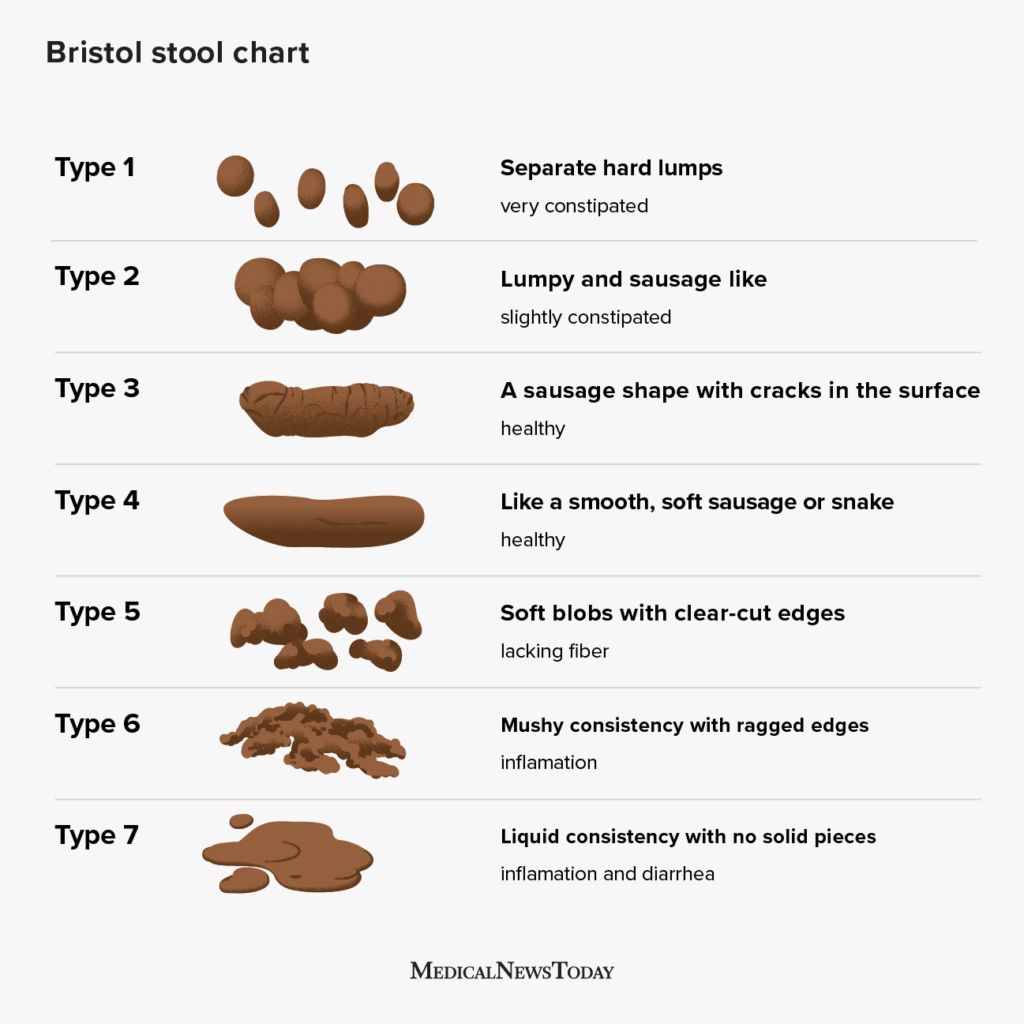
- A 2week symptom diary (including meals, stress events, and stool type).
- List of current medications and supplements.
- Questions about diet, lifestyle, and mental health support.
Effective Treatment Options
Dietary Approaches
The lowFODMAP diet is the gold standard. It involves three phases: elimination (46 weeks), systematic rechallenge, and personalization. During elimination, you avoid highFODMAP foods like apples, wheat, and certain dairy.
Probiotics & Supplements
Specific strainsespecially Bifidobacterium infantis and Lactobacillus plantarumhave shown promise in easing bloating and normalizing stool patterns. Always discuss dosing with a clinician. For people who also have overlapping liver concerns in their family, checking liverfriendly supplement choices can be useful see guidance on family fatty liver when considering longterm supplement plans.
Medications & When to Use Them
- Antispasmodics (e.g., hyoscine) for cramp relief.
- Laxatives (e.g., polyethylene glycol) during constipationdominant phases.
- Antidiarrheals (e.g., loperamide) for diarrhea spikes.
- Lowdose tricyclic antidepressants to modulate pain signals.
Psychological & Lifestyle Therapies
Stress is a notorious trigger. Cognitivebehavioral therapy (CBT), mindfulness meditation, and regular aerobic exercise (30minutes, 45 times weekly) can dramatically lower flareups.
DecisionTree Flowchart (for future visual)
Start with Are symptoms severe? Try lowFODMAP. If no improvement Add antispasmodic. If still unresolved Consult gastroenterologist for medication review. This guide helps patients navigate choices.
RealWorld Case Study
Sarah, a 34yearold graphic designer, spent years juggling unpredictable bowel habits. After a structured lowFODMAP trial coupled with weekly CBT sessions, her flareup frequency dropped by 60%. Her story, featured by the Canadian Digestive Health Foundation, illustrates how combining diet and mindbody work can bring lasting relief.
Foods to Avoid
IBSM Foods to Avoid
Heres a quick cheatsheet of what to keep off your grocery list:
- HighFODMAP fruits: apples, pears, mangoes.
- Wheatbased breads, pasta, and cereals.
- Legumes: beans, lentils, chickpeas.
- Dairy containing lactose (regular milk, soft cheese).
- Cruciferous veg: broccoli, cauliflower, Brussels sprouts.
- Artificial sweeteners: sorbitol, mannitol.
- Caffeinated drinks and alcoholic beverages.
IBSMFriendly Foods
Enjoy these lowFODMAP choices without fearing a gut revolt:
- LowFODMAP veggies: carrots, zucchini, spinach.
- Proteins: chicken, turkey, firm tofu, eggs.
- Glutenfree grains: rice, quinoa, oats (certified lowFODMAP).
- Lactosefree dairy or fortified plant milks.
- Fruits in moderation: strawberries, blueberries, oranges.
Sample 7Day Meal Plan (downloadable PDF)
Each day features breakfast, lunch, dinner, and a snack, all built around lowFODMAP staples. Providing a printable version helps readers jump straight into action.
Bottom Line Summary
IBSM may feel like an unwelcome guest that never leaves, but a balanced approachunderstanding the gutbrain connection, pinpointing personal triggers, and combining dietary tweaks with medical and psychological supportoffers genuine relief. Beware of fad quick fixes that lack scientific backing; instead, lean on evidencebased strategies cited by reputable sources such as and the American College of Gastroenterology.
Remember, youre not alone on this journey. With the right tools, you can reclaim a calmer, more predictable digestive rhythm.
Ready to start? Grab the symptom diary, give the lowFODMAP diet a trial, and schedule a chat with a gastroenterology specialist to tailor a plan just for you. If you have questions or want to share whats worked for you, feel free to reach outyour experience could help someone else find their path to relief.
FAQs
What is IBS-M?
IBS-M is a type of irritable bowel syndrome where symptoms alternate between constipation and diarrhea, often with abdominal pain and bloating.
What causes IBS-M?
IBS-M is linked to gut-brain axis disruption, stress, certain foods, and changes in gut bacteria, though the exact cause is not fully understood.
How is IBS-M diagnosed?
IBS-M is diagnosed based on symptom patterns, medical history, and ruling out other conditions using criteria like Rome IV and symptom diaries.
What foods should be avoided with IBS-M?
People with IBS-M should avoid high-FODMAP foods, dairy, caffeine, artificial sweeteners, and fried foods to help reduce symptoms.
Can IBS-M be cured?
There is no cure for IBS-M, but symptoms can be managed with diet, lifestyle changes, and sometimes medication.