Why should you care? Early detection means you can start diseasemodifying therapies before irreversible erosion sets in, preserving not just your joints but also your quality of life. Lets walk through what to look for, how doctors pin down the disease, and what you can do right now to protect yourself.
Early Warning Signs
What symptoms usually show up first?
RA loves to start quietly, targeting the small joints first. Common early clues include:
- Joint tenderness or dull ache in the fingers, toes, or wrists
- Morning stiffness that lasts longer than 30 minutes
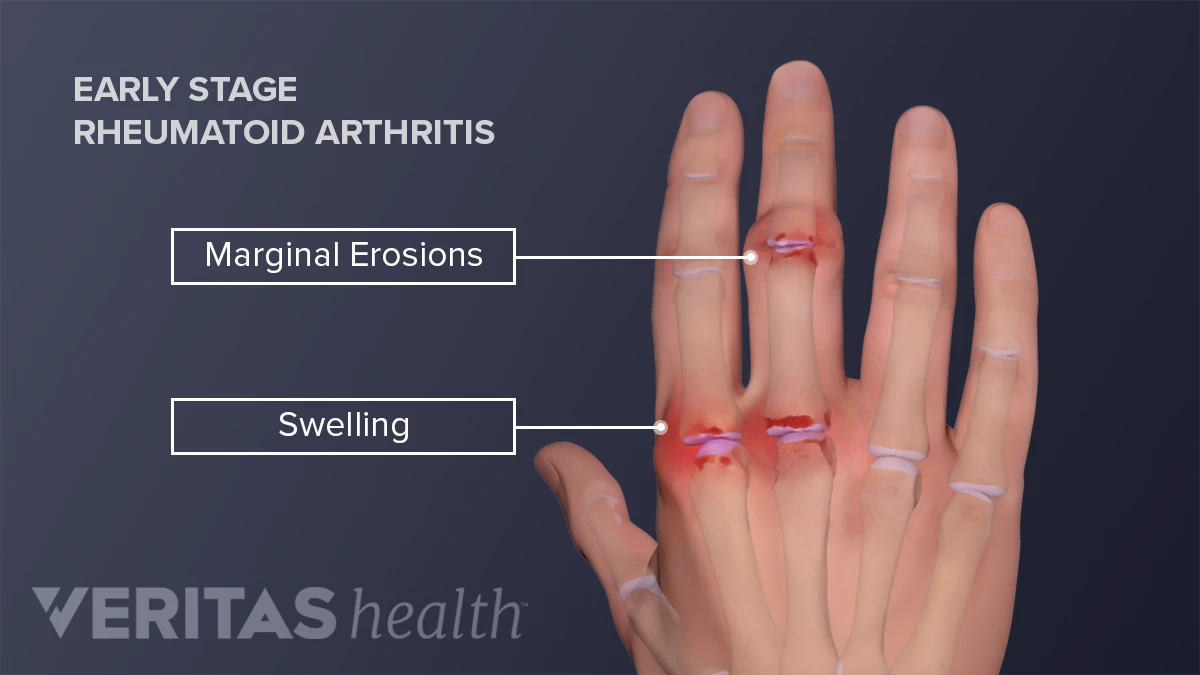
- Swelling that makes the affected joint look puffy
- Lowgrade fever, fatigue, and occasional weight loss
These symptoms often appear symmetricallymeaning the same joints on both sides of the body are affected. If youve been blaming a new keyboard for that cramp in your hand, it might be worth a second look.
What are the 4 stages of rheumatoid arthritis?
Understanding the diseases progression helps you grasp why early diagnosis matters. The four classic stages are:
- Stage1 Early/Incipient: Mild pain, no visible damage on Xray.
- Stage2 Moderate: Swelling becomes more obvious; early erosions appear on imaging.
- Stage3 Severe: Significant joint damage, functional limitations, and deformities start to show.
- Stage4 Endstage: Joint destruction is extensive; surgery may be required.
Catch it in Stage1, and you can often halt the march to Stage4.
Is rheumatoid arthritis hereditary?
Genetics play a role, but theyre not the whole story. Certain genesespecially the HLADR4 alleleraise your risk, and having a close relative with RA roughly doubles your odds. However, lifestyle factors like smoking, diet, and infections can trigger the disease even in people with no family history. So, while a family tree can hint at risk, its not a guarantee.
Core Diagnostic Steps
How is rheumatoid arthritis diagnosed?
Doctors follow a systematic pathway:
- Clinical exam: The physician checks for swollen joints, warmth, and reduced range of motion.
- Blood work: Specific tests look for antibodies and inflammation markers.
- Imaging: Xray, ultrasound, or MRI helps spot early joint changes.
- Referral: If suspicion remains, youll see a rheumatologist for a definitive diagnosis.
Rheumatoid arthritis blood test
Blood tests arent a magic wand, but theyre incredibly useful when combined with clinical findings. The most common panels include:
- Rheumatoid Factor (RF): Positive in ~7080% of established RA cases, but can be absent early on.
- AntiCCP antibodies: Highly specific for RA and often detectable before joint damage appears. A positive antiCCP result can predict a more aggressive disease course.
- ESR and CRP: General markers of inflammation that help gauge disease activity.
According to a study published in the , antiCCP has a specificity of over 95% for early RA, making it a cornerstone of early diagnosis.
Imaging tools for early detection
When symptoms are vague, imaging can provide the missing piece of the puzzle.
| Modality | What it Shows | Cost & Availability | Sensitivity (Early RA) |
|---|---|---|---|
| Xray | Joint space narrowing, overt erosions | Low cost, widely available | Low changes often appear later |
| Ultrasound | Synovial thickening, powerDoppler blood flow (active inflammation) | Moderate cost, operatordependent | High can detect inflammation before Xray changes |
| MRI | Bone edema, early erosions, softtissue detail | High cost, limited availability | Very high gold standard when Xray is normal but suspicion remains |
In practice, most doctors start with an Xray and add ultrasound if the picture isnt clear. MRI is reserved for complex cases where early erosion is suspected but not yet visible.
How quickly does rheumatoid arthritis spread?
Without treatment, RA can progress from mild joint pain to visible erosions within 312months. The speed variessome people experience a slow crawl, while others see rapid joint destruction in just a few weeks. This variability underscores why early detection and treatment are nonnegotiable.
Reading Test Results
What does a positive antiCCP result mean?
A positive antiCCP indicates a higher likelihood of developing erosive disease and usually prompts an aggressive treatment approach. Its not a death sentence, but it tells your rheumatologist that the disease may be more stubborn, so starting diseasemodifying antirheumatic drugs (DMARDs) early is crucial.
When should you see a rheumatologist?
If youve had persistent joint symptoms for more than six weeks, especially with a positive RF or antiCCP, its time to get a specialists opinion. Rheumatologists have the expertise to finetune treatment plans and monitor disease activity over time.
Can rheumatoid arthritis be cured permanently?
Unfortunately, theres no permanent cure for RA yet. However, many patients achieve longterm remissionmeaning the disease is quiet, and they feel symptomfreethrough early and consistent use of DMARDs, biologics, and lifestyle adjustments. Research into targeted therapies is promising, but cure remains a future goal.
Lifestyle Support Tips
What is the best pain relief for rheumatoid arthritis?
Managing pain while you wait for DMARDs to take effect is a balancing act:
- NSAIDs (e.g., ibuprofen, naproxen): Great for shortterm relief but watch for stomach or kidney side effects.
- Lowdose steroids: Can quickly diminish inflammation, but longterm use may lead to bone loss.
- Topical agents: Capsaicin or diclofenac gels work well for localized pain without systemic risks.
- Acetaminophen: Safe for mild pain, though it doesnt reduce inflammation.
Rheumatoid arthritis diet
Food isnt a magic bullet, but certain dietary patterns can help calm the immune system:
- Omega3 fatty acids: Found in fatty fish, flaxseed, and walnuts, they have antiinflammatory properties.
- Fruits and vegetables: Rich in antioxidants that combat oxidative stress.
- Whole grains: Provide fiber and help maintain stable blood sugar.
- Avoid: Processed sugars, excess red meat, and trans fats, which may aggravate inflammation.
According to the , an antiinflammatory diet can modestly reduce pain and improve joint function when paired with medical therapy.
Exercise & joint protection for early RA
Movement may feel counterintuitive when your joints hurt, but staying active is vital. Heres a quick friendtofriend checklist you can start today:
- Gentle rangeofmotion stretches for hands (e.g., finger bends, wrist circles).
- Lowimpact cardiothink walking, swimming, or stationary cyclingfor 2030minutes, three times a week.
- Strength training with light resistance bands to keep muscles supportive.
- Use ergonomically designed tools (keyboard, mugs with wide handles) to reduce joint strain.
- Apply heat before activity and cold after if swelling flares up.
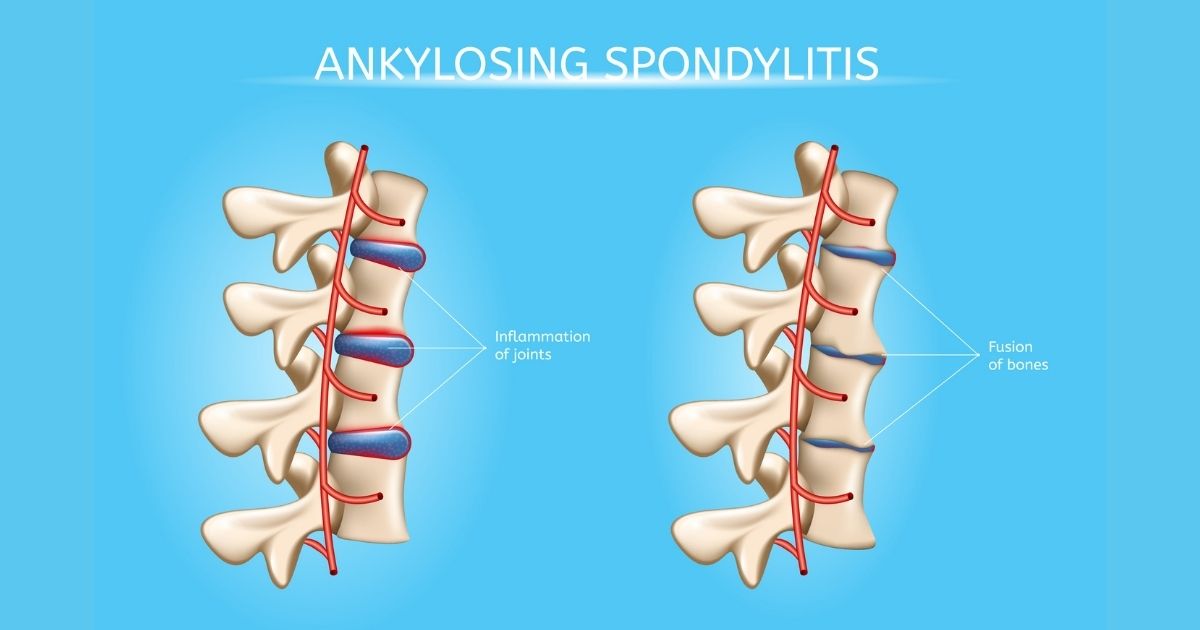
Because some inflammatory conditions share symptoms with RA, it can help to read about closely related disorders and remission definitions; for example, patients seeking guidance on controlling spinal inflammation might find resources on ankylosing spondylitis remission useful for comparison when discussing remission goals with their rheumatologist.
Putting It All Together
Diagnosing rheumatoid arthritis early isnt about a single test; its a detective story where symptoms, blood work, imaging, and your personal risk factors each contribute a clue. When you combine these pieces quickly, you give yourselfand your doctorthe best chance to start treatment before the disease can cause permanent damage.
Remember, you dont have to navigate this alone. If you notice the warning signs, book an appointment, ask for the rheumatoid arthritis blood test panel, and dont shy away from discussing imaging options like ultrasound. While theres no permanent cure today, modern therapies can put the disease into remission, letting you enjoy everyday moments without the shadow of joint pain.
Take the first step now: write down any joint symptoms youve had in the past month, gather your family health history, and schedule that short visit with your GP. Early action today could mean a future where your hands keep typing, cooking, and hugging without hesitation.
Whats your experience with early joint pain? Have you found a particular diet or exercise routine that helped? Share your thoughts belowwere all learning together.
FAQs
What are the first symptoms to watch for in rheumatoid arthritis?
Early symptoms usually include joint tenderness, swelling, and morning stiffness lasting more than 30 minutes, mainly in small joints like fingers, wrists, and toes. Fatigue, low-grade fever, and symmetric joint involvement are also common early signs.
Which blood tests help diagnose rheumatoid arthritis early?
Key blood tests include Rheumatoid Factor (RF), Anti-Cyclic Citrullinated Peptide (anti-CCP) antibodies, and inflammatory markers such as ESR and CRP. Anti-CCP is highly specific and can detect RA before joint damage occurs.
How does imaging aid in early rheumatoid arthritis diagnosis?
X-rays detect later-stage joint damage, while ultrasound and MRI are more sensitive in early RA. Ultrasound can detect synovial inflammation, and MRI can reveal bone edema and early erosions not visible on X-rays.
When should I see a rheumatologist for my joint symptoms?
If joint symptoms persist for more than six weeks, especially with positive RF or anti-CCP blood tests, seeing a rheumatologist is crucial for specialized diagnosis and tailored treatment.
Can rheumatoid arthritis be cured if diagnosed early?
There is no permanent cure currently, but early diagnosis allows for prompt treatment with disease-modifying drugs that can induce long-term remission and prevent joint damage.