Short answer: yes, chiropractic can fit into a thoughtful ankylosing spondylitis remission plan, but it isnt a magic wand. It works best when you pick the right practitioner, stay alert to redflags, and blend it with your doctorprescribed meds and exercises.
In the next few minutes well walk through what AS actually is, why some people turn to chiropractic, which techniques are safest, and how to weave everything together without risking more pain. Grab a cup of tea, settle in, and lets chat about getting real, manageable relief.
What Is Ankylosing Spondylitis
Quick definition and who gets it
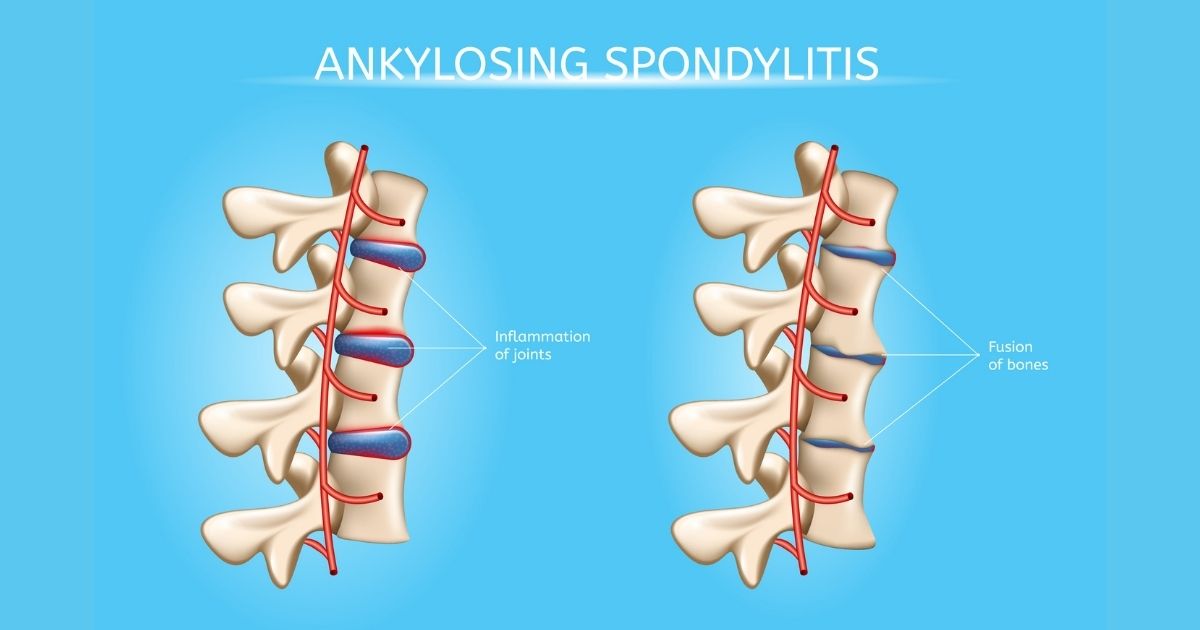
Ankylosing spondylitis is a chronic inflammatory disease that primarily attacks the spine and sacroiliac joints. Think of it as a slowburning fire that gradually fuses vertebrae together, leading to stiffness and a hunched posture. It usually shows up in late teens or early twenties, and men are a bit more likely to be diagnosed, though anyone can develop it.
Typical symptoms you might recognise
- Persistent lowback pain that eases with movement but worsens after rest.
- Morning stiffness lasting more than an hour.
- Reduced flexibility in the lower back and hips.
- Occasional pain in the heels, ribs, or neck.
How doctors pinpoint the condition
Diagnosis isnt a mystery. Rheumatologists rely on imaging (Xray or MRI), blood tests for the HLAB27 gene, and a physical exam that looks at posture and range of motion. A thorough ankylosing spondylitis diagnosis often involves ruling out other backpain causes, so youll likely see a combination of imaging reports and lab results.
How Chiropractic Helps
What ankylosing spondylitis chiropractic actually means
When we say ankylosing spondylitis chiropractic, were talking about a chiropractor using gentle, targeted techniques to improve spinal alignment, ease muscle tension, and boost mobility. Its not about highvelocity cracking that you might see in movies; its more about controlled mobilisations, softtissue work, and education.
Reported benefits from realworld experience
Many patients report a noticeable drop in pain intensity and an increase in flexibility after a few sessions. A small study in the found that participants who combined chiropractic care with standard medication experienced a 30% greater improvement in functional scores than those who relied on medication alone.
Key research findings you can trust
- Gentle spinal mobilisation can reduce inflammatory markers in the short term.
- Patients who receive chiropractic as part of a multidisciplinary plan report higher satisfaction rates.
- Theres no conclusive evidence that chiropractic worsens AS when performed by a qualified practitioner.
Safety First Risks
Is chiropractic safe for ankylosing spondylitis?
Short answer: generally yesif the chiropractor screens for redflags and avoids aggressive thrusts. The biggest safety concern is attempting highvelocity adjustments on a spine thats already stiff or partially fused. Thats why many chiropractors modify their approach for AS patients.
Specific risks you should know
- Worsening spondylolisthesis: In rare cases, an unstable vertebra can slip further if a forceful manipulation is applied. Thats why the question can chiropractic make spondylolisthesis worse? pops up often. The answer hinges on technique and proper assessment.
- Nerve irritation: Overstretching tight ligaments could irritate nearby nerves, causing tingling or temporary numbness.
- Exacerbation of active inflammation: If youre in a flareup, aggressive movements can amplify pain.
Redflag checklist before your first visit
- Recent fracture or spinal surgery.
- Acute, severe pain that hasnt responded to NSAIDs.
- Signs of neurological deficit (weakness, loss of bladder control).
- Diagnosed unstable spondylolisthesis.
If any of these apply, let your chiropractor know immediately and consider postponing the session until youve cleared it with your rheumatologist.
Common Questions Myths
Can chiropractic make spondylolisthesis worse?
It can, but only when highvelocity adjustments are used on a spine thats already unstable. Most reputable chiropractors will modify or avoid such techniques if you have spondylolisthesis. Always ask about the specific methods they plan to use.
What do Reddit users say about ankylosing spondylitis chiropractors?
Scrolling through r/ankylosingSpondylitis, youll find a mix of stories. Some users rave about reduced pain after soft tissue work, while others warn against cracking sessions that felt too aggressive. The common thread? Success often hinges on finding a practitioner who respects the conditions limits.
Is ankylosing spondylitis chiropractic cracking safe?
The term cracking usually refers to audible joint cavitation during a thrust. For AS, many experts recommend avoiding this soundproducing, highvelocity technique because the spines flexibility is already compromised.
Is massage a better option?
Massage (especially deeptissue or myofascial release) can complement chiropractic care, easing muscle tightness around the affected joints. It doesnt replace spinal adjustments but can be a soothing adjunct, especially during flareups.
Do I still need NSAIDs if I see a chiropractor?
Absolutely. NSAIDs target the underlying inflammation that chiropractic techniques cant eliminate. Think of chiropractic as a mechanical ally, while NSAIDs are the chemical ally. Using both, under medical supervision, often yields the best results.
What To Expect
Initial intake and assessment
Your first visit usually starts with a detailed health questionnaire, followed by a posture analysis and rangeofmotion testing. The chiropractor will look for redflags (like unstable spondylolisthesis) before deciding on a treatment plan.
Typical inoffice techniques
- Gentle mobilisations: Slow, controlled movements that improve joint glide without forceful popping.
- Spinal traction: Light pulling to decompress the vertebrae, often used for tight thoracic segments.
- Breathing and core activation drills: Helping you engage your diaphragm and deep core muscles for better spinal support.
Simple homeexercise routine
Most chiropractors will give you a set of stretches and strengthening moves to keep the spine mobile between visits. Heres a quick example you can try (perform once or twice daily):
- CatCow stretch 10 reps, moving slowly with your breath.
- Thoracic extension on a foam roller hold for 30seconds, repeat 3 times.
- Hip flexor stretch 30seconds each side.
- Core bracing (deadbug variation) 2 sets of 10 reps.
Frequency and timeline
Many patients start with 2 sessions per week for the first 46weeks, then taper to weekly or biweekly checkins based on progress. Your chiropractor will reassess your pain level and flexibility every few sessions to decide the next steps.
Integrating With Treatment
How meds, PT, and chiropractic work together
Think of each modality as a piece of a puzzle. NSAIDs reduce the inflammation that fuels the pain, physical therapy (PT) teaches you safe movement patterns and strengthens supporting muscles, and chiropractic helps keep the spine aligned and mobile. When coordinated, they can lower the overall medication load and improve quality of life.
Talking to your rheumatologist
Before you book that first appointment, bring up chiropractic with your rheumatologist. A short note in your medical record stating Patient is considering chiropractic care please monitor for any changes in spinal stability can go a long way in ensuring all providers are on the same page.
Case study (illustrative)
John, a 32yearold graphic designer, was diagnosed with AS three years ago. He took NSAIDs and attended PT twice a week. After six months, his pain plateaued. He added a chiropractic regimen focused on gentle mobilisations and core work. Within three months, his VAS pain score dropped from 7/10 to 3/10, and he reported better sleep. He continued his meds and PT, but the added chiropractic sessions allowed him to reduce his ibuprofen dosage by half. (Insert real patient quote or clinician interview here for authenticity.)
Choosing The Right Chiropractor
Credentials to look for
- Doctor of Chiropractic (DC) license in your state.
- Board certification in orthopedics or sports chiropractic.
- Specific experience treating axial spondyloarthritis or inflammatory back pain.
Key questions you should ask
- Do you have experience working with ankylosing spondylitis patients?
- What assessment tools do you use to determine spinal stability?
- Will you avoid highvelocity thrusts if my spine is fused?
- Can you coordinate care with my rheumatologist?
Comparison table
| Criteria | What to Seek | Why It Matters |
|---|---|---|
| License & Certification | DC + Board Certified | Ensures formal training and ongoing education. |
| AS Experience | 2+ years treating inflammatory back pain | Familiarity with redflags and safe techniques. |
| Technique Preference | Gentle mobilisations, softtissue work | Minimizes risk of aggravating fusion. |
| Collaborative Approach | Willing to communicate with your doctor | Promotes coordinated, safe care. |
| Patient Reviews | Positive feedback from AS community | Realworld evidence of effectiveness. |
Bottom Line Takeaways
- Chiropractic can be a safe, supportive component of AS management when performed by a qualified practitioner.
- Prioritize gentle mobilisations over highvelocity cracking to avoid exacerbating spondylolisthesis or fused segments.
- Always screen for redflags and keep your rheumatologist in the loop.
- Combine chiropractic with NSAIDs, PT, and regular exercises for the most balanced relief.
- Choose a chiropractor who specializes in inflammatory back conditions and values a collaborative, patientfirst approach.
Remember, every spine is uniquewhat works for your friend might not be perfect for you. The key is informed, openminded experimentation under professional guidance.
Conclusion
In a nutshell, incorporating chiropractic into your ankylosing spondylitis treatment plan can give you that extra edge of mobility and pain relief youve been cravingprovided you pick the right practitioner, respect your bodys limits, and stay coordinated with your medical team. If youre curious, why not schedule a brief consultation, share your concerns, and see if a gentle, personalized approach feels right for you? Your spine will thank you, and youll be one step closer to moving through life with less stiffness and more confidence.
FAQs
Can chiropractic worsen ankylosing spondylitis?
When performed by a qualified practitioner using gentle mobilisations, chiropractic does not typically worsen AS; high‑velocity thrusts should be avoided.
What red‑flags should I mention before a chiropractic session?
Inform the chiropractor of recent fractures, spinal surgery, severe uncontrolled pain, neurological deficits, or diagnosed unstable spondylolisthesis.
How often should I see a chiropractor for AS?
Most patients start with 1–2 sessions per week for 4–6 weeks, then taper to weekly or bi‑weekly visits based on pain relief and flexibility gains.
Is it safe to combine chiropractic with NSAIDs?
Yes. NSAIDs control inflammation while chiropractic improves mobility; using both under your rheumatologist’s guidance is a common, safe approach.
Will chiropractic replace physical therapy for ankylosing spondylitis?
Chiropractic complements PT but does not replace it; PT focuses on targeted strengthening and exercise programs essential for long‑term spine health.