Lets cut to the chase: osteoporosis is a silent thief that steals bone strength, and the good news is that targeted physiotherapy can help you keep those bones sturdy. Below youll find everything you needstraightforward explanations, practical exercises, safety tips, and even a free downloadable planso you can take charge of your bone health today.
Quick Answer Overview
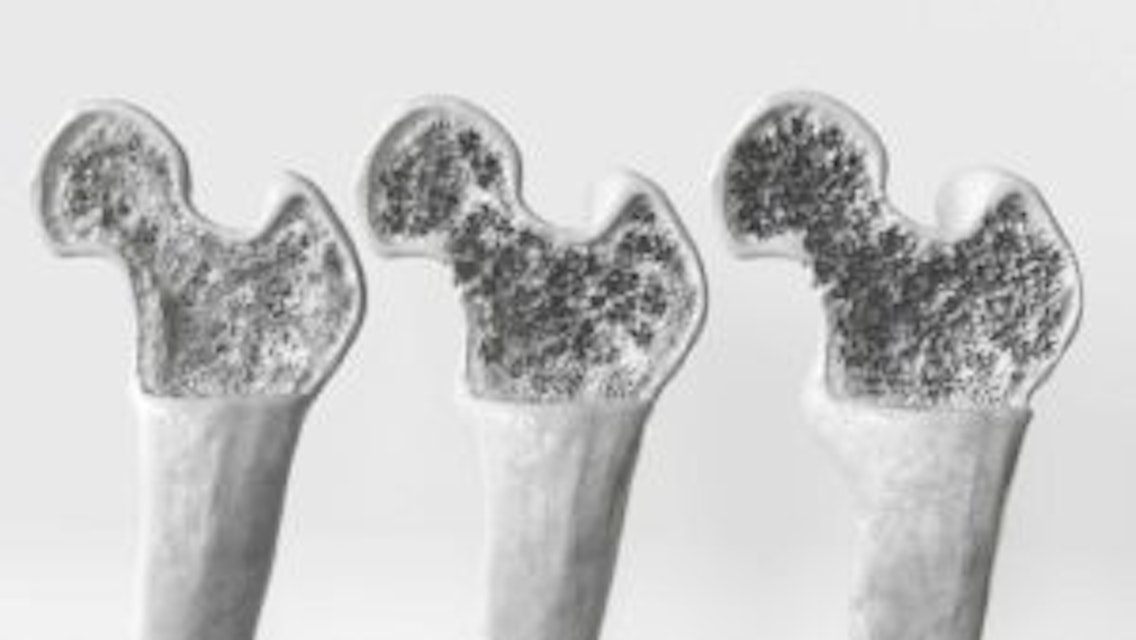
What is osteoporosis? Its a condition where bone mineral density drops below a safe threshold, making bones fragile and more likely to fracture from everyday activities. Why does physiotherapy matter? Because weightbearing and resistance exercises can stimulate bone formation, improve balance, and dramatically lower the risk of falls and fractures.
Understanding Osteoporosis Basics
What Causes Bone Loss?
Think of your bones as a living, remodeling structure. Hormonal shifts (especially dropping estrogen after menopause), insufficient calcium or vitaminD, chronic inflammation, and certain medications (like longterm steroids) all tip the balance toward bone breakdown.
How Is Bone Density Measured?
The gold standard is a DXA (dualenergy Xray absorptiometry) scan, which gives you a Tscore. A score of 2.5 or lower signals osteoporosis. For a quick risk check, many clinicians also use the FRAX tool, which predicts 10year fracture probability, its a reliable complement to DXA. If you need a clear plan to improve strength and bone health, a focused osteoporosis physical therapy program can be particularly helpful.
What Are the Quiet Warning Signs?
- Sudden loss of height (often a few centimeters)
- A stooped posture, sometimes called a dowagers hump
- Frequent lowimpact fractureslike a wrist break from a simple fall
Normal vs. Osteoporotic BMD Values
| Location | Normal BMD (g/cm) | Osteoporotic BMD (g/cm) |
|---|---|---|
| Hip (Femoral Neck) | >1.0 | 0.8 |
| Lumbar Spine | >1.2 | 0.9 |
| Forearm | >0.9 | 0.6 |
Managing Osteoporosis with Physio
Core Goals of Physiotherapy
Any good physiotherapy program for osteoporosis aims to:
- Preserve or modestly increase bone mineral density
- Boost balance and gait stability
- Relieve pain and keep daily activities independent
EvidenceBased Exercise Programs
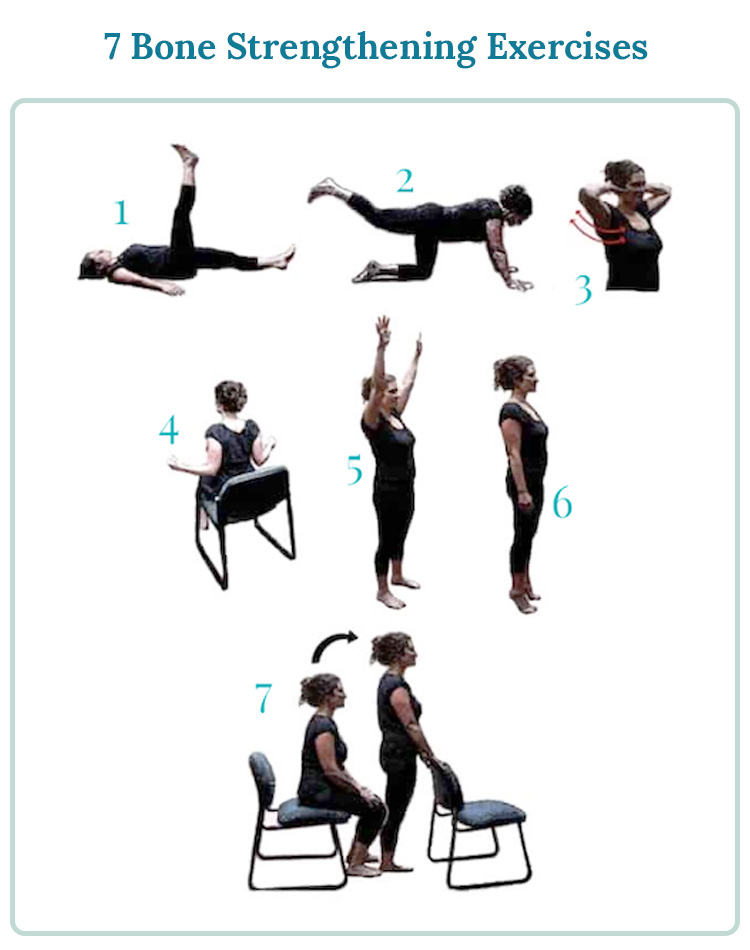
Research on osteogenic exercises shows that lowimpact, weightbearing activities are the sweet spot for stimulating bone growth without overloading fragile skeletons. Here are the three pillars most recommends:
- Weightbearing osteogenic moves: marching in place, stepups, and gentle stair climbing. Aim for 1015minutes, three times a week.
- Resistance training: using bands or light dumbbells (510kg). Perform 23 sets of 812 repetitions for major muscle groups, twice weekly.
- Balance & proprioception drills: singleleg stands, heeltotoe walks, or a wobble board for 5minutes, four times a week.
Sample Weekly Exercise Sheet (PDFStyle)
Imagine a printable osteoporosis physiotherapy management pdf you can keep on your fridge. It would look something like this:
- Monday 10min marching + 10min balance
- Tuesday Upperbody resistance (bands)
- Wednesday Rest or gentle walking
- Thursday Stepups + lowerbody resistance
- Friday Balance circuit + core work
- Saturday Light yoga or taichi
- Sunday Rest
ContraIndications & Safety Tips
Not every movement is safe when bones are fragile. Keep these red flags in mind:
- Highimpact jumping or deep twisting
- Lifting more than 10kg without supervision
- Exercising during an acute fracture or severe pain flare
- Uncontrolled hypertension or severe osteoporosis (T3.5)
QuickReference Safety Checklist
- Check with your physiotherapist before starting new exercises
- Warmup for at least 5minutes (marching, gentle arm circles)
- Use a chair or rail for support during balance work
- Stop immediately if you feel sharp pain or dizziness
Tailoring Programs for Different Groups
One size never fits all. Heres how you can adapt the plan:
- Postmenopausal women: Focus on hipstrengthening moves and calciumrich nutrition.
- Adults over 70: Prioritize slow, steady balance drills and use resistance bands instead of weights.
- Men on longterm steroids: Add extra core stability work to counter muscle loss.
RealWorld Success Story
Take Sarah, 68, who slipped on a kitchen tile and fractured her wrist. After a 12week physiotherapy program that followed the osteoporosis physiotherapy management ppt protocol, her BMD at the hip improved by 2% and she reported no new falls. Stories like Sarahs illustrate how small, consistent steps can make a big difference.
Complementary Lifestyle Strategies
Nutrition That Supports Bone Health
Exercise alone isnt enough. Pair it with a diet rich in:
- Calcium (1,200mg/day) think dairy, fortified plant milks, leafy greens.
- VitaminD (800IU/day) sunlight, fatty fish, or a supplement if youre low.
- Protein (1.01.2g/kg body weight) lean meats, beans, tofu.
- Magnesium and VitaminK2 nuts, seeds, and fermented foods.
FallPrevention at Home
Even the best exercises cant protect you if you trip over a loose rug. Quick fixes:
- Remove clutter from walkways
- Install nonslip mats in the bathroom
- Secure handrails beside stairs and in the shower
- Use nightlights to improve visibility at night
When to Call a Professional
If you notice any of the following, its time to schedule a physiotherapy assessment:
- New or worsening back pain
- Loss of height or posture changes
- A recent fragility fracture
- Difficulty rising from a chair without using hands
Physiotherapy vs. Medication: A Quick Comparison
| Aspect | Physiotherapy | Medication (e.g., bisphosphonates) |
|---|---|---|
| Primary Benefit | Improves strength, balance, and modest BMD gain | Directly slows bone resorption |
| Side Effects | Minimal; risk only if exercises are performed incorrectly | Gastrointestinal upset, rare osteonecrosis of jaw |
| Cost | Variable (session fees, often covered by insurance) | Prescription cost, may need regular monitoring |
| LongTerm Adherence | Requires commitment to routine activity | Requires daily pill intake |
Helpful Resources Download
Want something you can refer to whenever you need a quick reminder? Grab the following:
- Osteoporosis Physiotherapy Management PDF: A printable weekly planner with exercise details.
- Osteoporosis Physiotherapy Management PPT: A slide deck you can watch on a phone or tablet.
- Full Osteoporosis Pathophysiology Overview: Links to indepth articles on at Physiopedia.
Final Takeaway Summary
Osteoporosis doesnt have to be a life sentence of fear and limitation. By understanding the conditions root causes, getting the right bonedensity tests, and embracing a balanced physiotherapy programcomplete with safe weightbearing moves, resistance work, and balance drillsyou can protect your skeleton while still enjoying the activities you love. Pair these exercises with solid nutrition, smart home safety tweaks, and regular professional checkins, and youll be giving your bones a fighting chance.
Ready to start? Download the free osteoporosis physiotherapy management pdf, try the simple stepup routine tomorrow, and let us know how you feel after the first week. Your bone health journey is a conversationnot a lectureso feel free to share your questions or success stories in the comments. Were all in this together.
FAQs
What is osteoporosis and how does physiotherapy help?
Osteoporosis is a condition where bone mineral density decreases, making bones fragile and prone to fractures. Physiotherapy uses weight-bearing and resistance exercises to stimulate bone growth, improve balance, and lower fall and fracture risk.
What kinds of exercises are recommended for osteoporosis?
Recommended exercises include weight-bearing osteogenic moves (marching, stair climbing), resistance training with bands or light weights, and balance drills such as single-leg stands or heel-to-toe walks.
Are there safety precautions for exercising with osteoporosis?
Yes, avoid high-impact jumping, deep twisting, lifting heavy weights (>10 kg) without supervision, and exercising during acute fractures or severe pain. Always warm up and use support during balance exercises.
Can physiotherapy improve bone mineral density (BMD)?
Physiotherapy may modestly preserve or increase BMD through targeted exercise routines, while also enhancing balance and muscle strength to reduce fracture risk.
When should I see a physiotherapist for osteoporosis?
Schedule a physiotherapy assessment if you have new or worsening back pain, noticeable loss of height, a recent fragility fracture, or difficulty rising from a chair without assistance.