Understanding the Threshold
What Tscore range defines osteopenia?
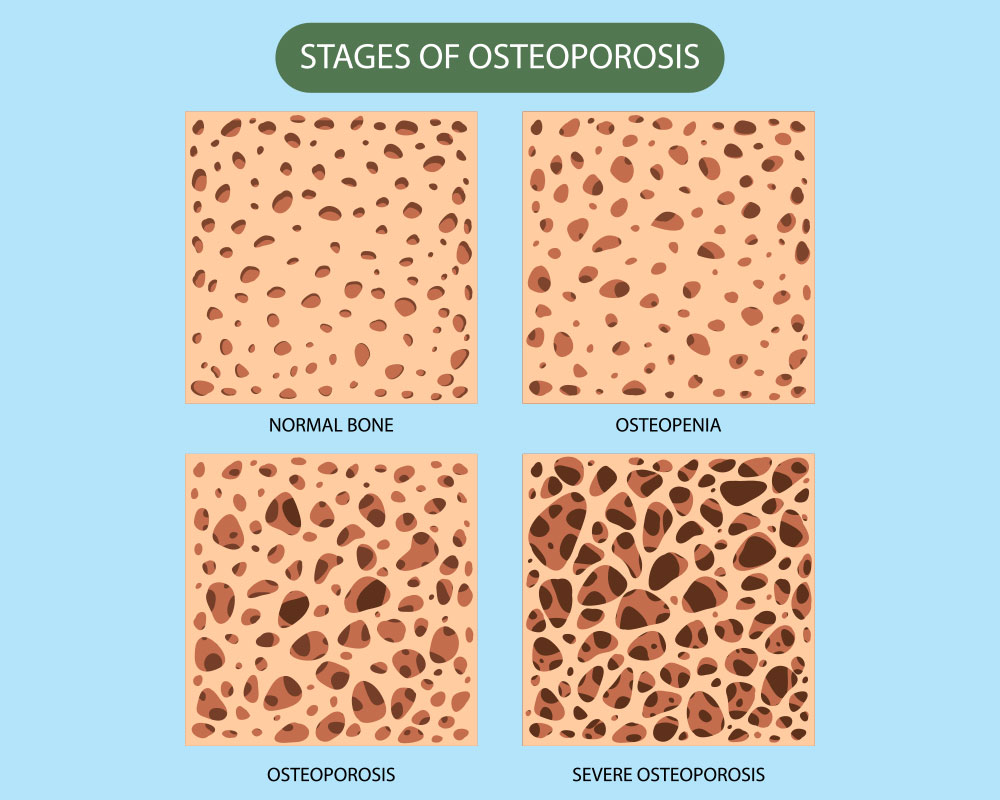
The World Health Organization (WHO) sets the benchmark: a Tscore between 1.0 and 2.5 on a DEXA scan signals osteopenia. That score compares your bone density to the average healthy 30yearold of the same sex. Anything above 1.0 is considered normal, and a score lower than 2.5 slides you into osteoporosis territory.
How is the threshold measured?
Doctors use a DEXA (dualenergy Xray absorptiometry) machine, which takes a quick, painless picture of your lumbar spine and hip. The scan calculates the amount of mineral in those bones and spits out the Tscore. Think of it like a bone selfie that tells you how dense you are compared to your peers.
Osteopenia vs. osteoporosis key differences
| Aspect | Osteopenia | Osteoporosis |
|---|---|---|
| Tscore | 1.0 to 2.5 | Below 2.5 |
| Fracture risk | Elevated, but moderate | High, especially hip & spine |
| Typical treatment trigger | Lifestyle changes; meds if high risk | Medication usually recommended |
Both conditions involve bone loss, but osteoporosis carries a steeper risk of fractures. Knowing where you fall on the osteopenia threshold helps you decide when its time to act.
Reading Your Results
Bonedensity chart by age
Age matters. Below is a quick snapshot of typical Tscore ranges you might see on a bonedensity chart, based on data from the and other reputable sources.
| Age | Men (Tscore) | Women (Tscore) |
|---|---|---|
| 2029 | 0 to +1 | 0 to +1 |
| 3039 | +0.5 to +1 | +0.5 to +1 |
| 4049 | +0 to +0.5 | +0 to +0.5 |
| 5059 | 0.5 to 0 | 0.5 to 0 |
| 6069 | 1.0 to 0.5 | 1.0 to 0.5 |
| 7079 | 1.5 to 1.0 | 1.5 to 1.0 |
Notice how the normal range slides a bit lower as we age. Thats why a Tscore of 1.3 might feel alarming for a 45yearold but is more typical for someone in their 70s.
What does a borderline score mean?
If your scan lands you at the edgesay, 1.0 or 2.4youre in a gray zone. This is where the becomes handy, estimating your 10year fracture risk based on age, sex, BMI, and lifestyle factors. A borderline score combined with a high FRAX probability may tip the scale toward medication, even if you technically have osteopenia.
When to consider pharmacologic intervention?
Guidelines from the International Osteoporosis Foundation suggest starting meds when any of the following apply:
- FRAX 10year major osteoporotic fracture risk 20%.
- History of a lowimpact fracture (e.g., wrist, hip).
- Rapid bone loss (5% per year) on repeat DEXA.
If you tick one of those boxes, a conversation with your doctor about medication is worth having.
Health Implications
Osteopenia symptoms (or lack thereof)
Most people with osteopenia feel perfectly finehence the phrase silent condition. Rarely, you might notice vague aches in the back or joints, but those symptoms are often unrelated. The biggest concern is the hidden fracture risk, especially in the spine, hip, and wrist.
What is life expectancy with osteopenia?
Good news: osteopenia itself doesnt shave years off your life. Studies published in show that, when managed properly, people with osteopenia have a comparable life expectancy to those with normal bone density. The key is to stay proactivemonitor bone health, keep active, and address risk factors early.
Risks vs. benefits of early treatment
Starting medication too soon can bring sideeffects like gastrointestinal irritation (for oral bisphosphonates) or rare atypical femur fractures. Conversely, delaying treatment when risk is already high can lead to a break that drastically impacts mobility and independence. The sweet spot is a balanced, personalized plansomething your doctor can help you craft after weighing the numbers and your preferences.
Lifestyle and Nutrition
Exercise recommendations for osteopenia
Movement is medicine. Aim for:
- Weightbearing activities: brisk walking, jogging, dancing34 times a week.
- Resistance training: light dumbbells or resistance bands, focusing on major muscle groups, 23 sessions weekly.
- Balance work: yoga or tai chi to reduce fall risk.
Start slow, listen to your body, and build up gradually. Remember, consistency beats intensity for bone health.
What foods to avoid with osteopenia?
While theres no bonekilling diet, certain habits can blunt your progress:
- Excessive sodium (<2,300mg/day) it leaches calcium.
- High caffeine (>3 cups of coffee) can increase calcium loss.
- Heavy alcohol (2 drinks/day) impairs bone formation.
- Very high protein without adequate calcium can acidify the body.
Swap those for calciumrich goodies: lowfat dairy, fortified plant milks, leafy greens, and almonds. Pair calcium with vitaminD (sunlight or fortified foods) for optimal absorption.
Realworld case example
Meet Maya, a 58yearold marketing director. Her DEXA came back at 1.6, putting her firmly in the osteopenia range. Instead of reaching for medication right away, Maya teamed up with a physio, added 30minutes of brisk walking five days a week, and swapped soda for almond milk. Six months later, a repeat scan showed an improvement of 0.3pointsher Tscore rose to 1.3. She didnt cure osteopenia, but she shifted her risk profile substantially. Stories like Mayas illustrate how lifestyle can move the needle, especially when the fracture risk is modest.
Medical Treatment Options
Firstline agents
If your doctor recommends medication, the most common firstline drugs are bisphosphonates (e.g., alendronate, risedronate). They work by slowing bone breakdown and are usually taken once a week or once a month. Sideeffects can include stomach upset, so taking the pill with water and staying upright for 30minutes helps.
Emerging therapies & clinicaltrial data
For those who cant tolerate bisphosphonates or have a higher fracture risk, newer options exist:
- Denosumab: a biannual injection that blocks a protein (RANKL) involved in bone loss.
- Teriparatide: a daily injectable that actually builds bone, used for a limited 2year course.
- Romosozumab: a newer antibody that both builds and preserves bone, showing promising results in recent trials.
These therapies are typically prescribed by specialists and may be covered by insurance for highrisk patients. Always discuss benefits, costs, and monitoring requirements.
Decisionmaking framework
Heres a quick checklist you can use when talking to your doctor:
- What is my current Tscore and FRAX risk?
- Do I have any prior fractures or rapid bone loss?
- Am I comfortable with lifestyle changes alone, or do I need medication?
- What are the sideeffects and costs of the proposed drug?
- When should we recheck my bone density?
Answering these questions together builds a shareddecision plan that respects your values and health goals.
Takeaway Summary
Lets recap the three big takeaways:
- Know your numbers. Your Tscore tells you exactly where you stand on the osteopenia threshold and guides next steps.
- Combine lifestyle with expert guidance. Weightbearing exercise, balanced nutrition, and, when needed, medication work handinhand to protect your bones.
- Stay proactive. Schedule regular DEXA scans, use tools like FRAX, and keep an open dialogue with your healthcare team.
Bone health is a marathon, not a sprint. If youve just learned about your osteopenia status, take a breath, make a small plan for movement or a food swap, and set a reminder to chat with your doctor in a few weeks. Youve got this!
One helpful resource on exercise-based approaches to strengthen bones is osteoporosis exercises, which offers practical routines you can discuss with your physiotherapist.
What steps are you thinking of taking first? Share your thoughts in the comments, or drop a question if anything feels unclear. Im here to help you on this journey.
FAQs
What is the osteopenia threshold?
The osteopenia threshold is defined as a bone density T-score between -1.0 and -2.5 on a DEXA scan, indicating your bones are weaker than normal but not yet osteoporotic[2][3][5].
How is the osteopenia threshold measured?
Doctors use a DEXA (dual-energy X-ray absorptiometry) scan to measure your bone mineral density, comparing it to a reference group of young healthy adults to produce your T-score[3][5].
What’s the difference between osteopenia and osteoporosis?
Osteopenia means bone density is lower than normal but not severe (T-score -1 to -2.5). Osteoporosis is more advanced (T-score below -2.5), with much higher fracture risk[2][3][5].
Do people with osteopenia always need medication?
No—many people with osteopenia only need lifestyle changes. Medication may be considered if you have a high fracture risk according to tools like FRAX, a history of fractures, or rapid bone loss[1].
Can you improve your T-score if it’s in the osteopenia range?
Yes, weight-bearing exercise, balanced nutrition, and sometimes calcium/vitamin D supplements can help maintain or slightly improve bone density, especially if started early[6].