Feeling like every joint in your body is throwing a tantrum? Thats what we call widespread joint pain, and its a sign that something underneath needs attention. The good news is you dont have to live with it forever once you understand whats going on, you can pick the right strategies to calm those aches and get back to doing the things you love.
In this post Ill walk you through the most common reasons your joints might be hurting all over, point out the redflag symptoms that demand a doctors look, and share practical, everyday steps you can try right now. Think of it as a friendly chat over coffee, where we sort out the confusing bits together.
Understanding the Triggers
Inflammatory arthritis
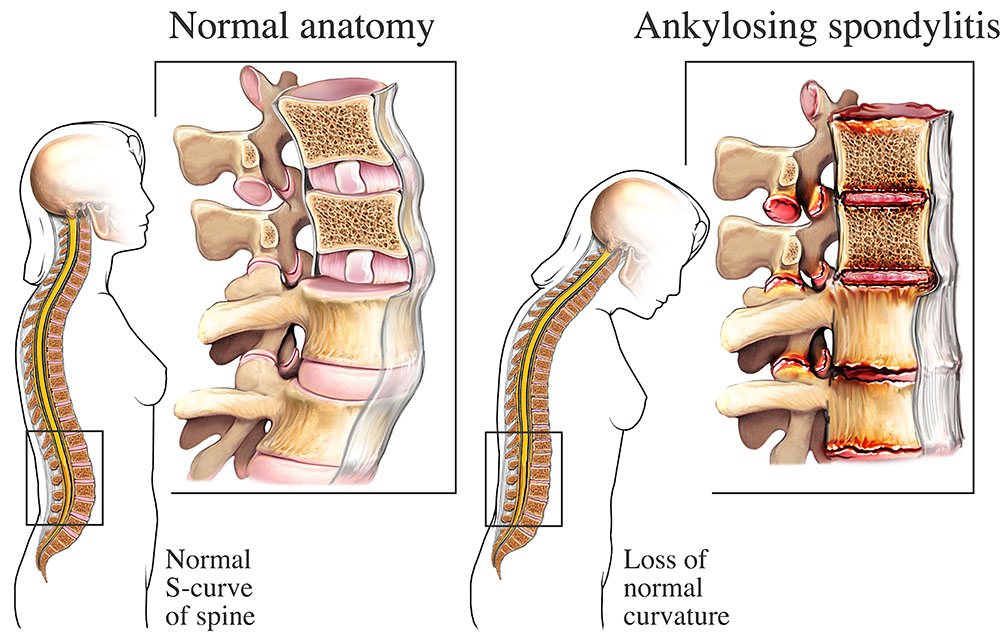
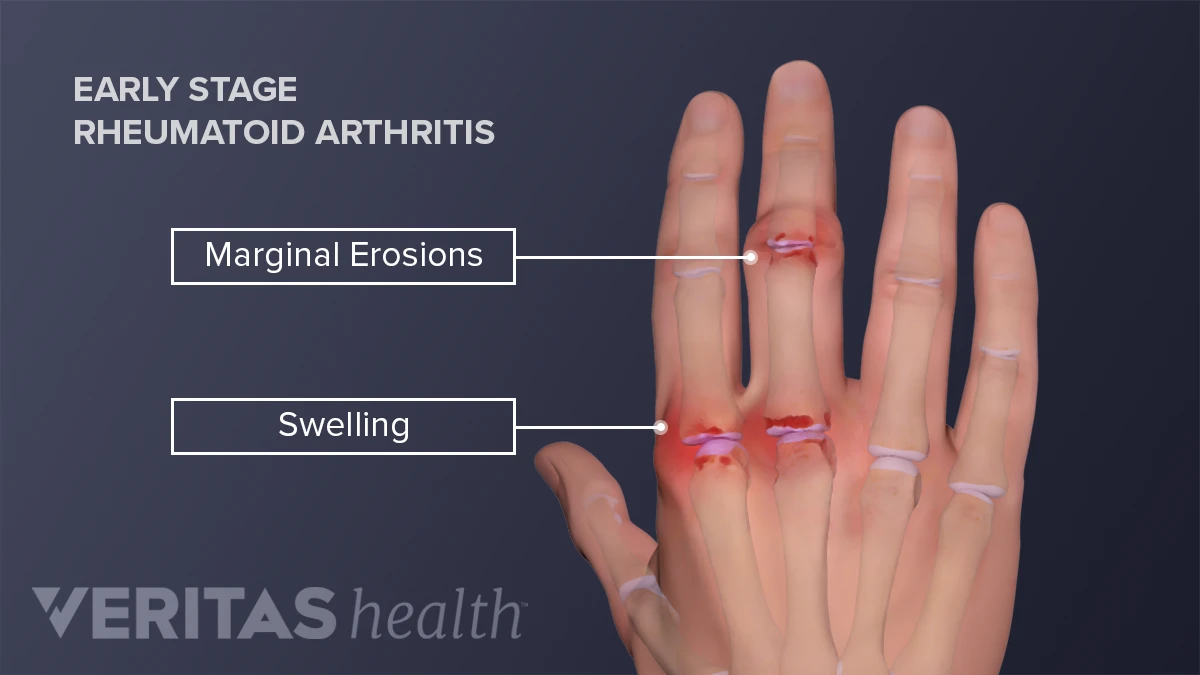
When the immune system mistakenly attacks the lining of your joints, it creates swelling, pain, and stiffness that can spread from hand to knee. Rheumatoid arthritis is the classic example, but there are other forms like psoriatic arthritis and juvenile idiopathic arthritis that act in a similar way. According to the , the hallmark is symmetric joint pain thats worse in the morning and improves with movement. You should also be aware of conditions such as ankylosing spondylitis criteria, which help clinicians decide when inflammatory back pain and related joint problems fit a specific diagnosis.
Degenerative arthritis
Osteoarthritis is the wearandtear arthritis most people think of when they hear joint pain. It usually starts in weightbearing joints, but as cartilage thins out it can spread, leading to a feeling that all my joints hurt suddenly. The pain generally worsens with activity and eases with rest.
Systemic illnesses
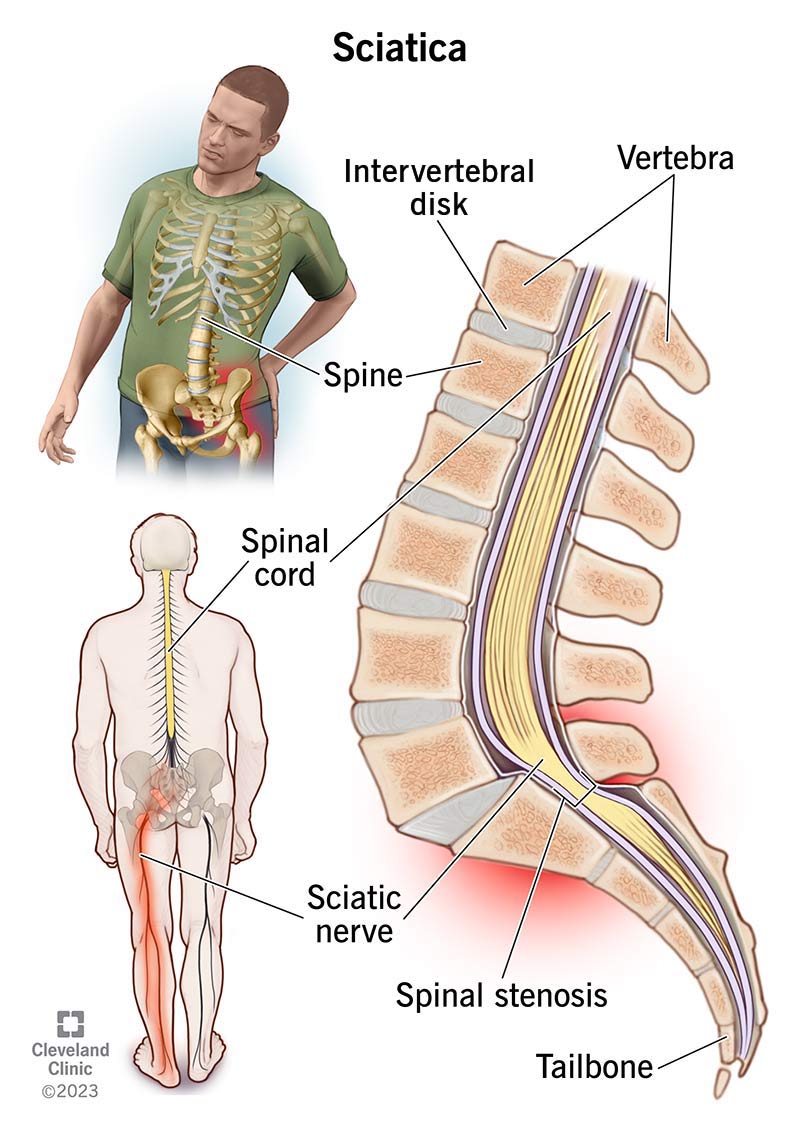
Diseases like lupus, ankylosing spondylitis, and even thyroid disorders can send pain signals to many joints at once. What makes this tricky is that the joints often feel achy without obvious swelling a scenario many describe as multiple joint pain without swelling.
Fibromyalgia and chronic fatigue
Fibromyalgia is a wholebody pain syndrome that loves to pair with extreme fatigue. If youve ever wondered what causes extreme fatigue and joint pain, this could be the answer. Unlike inflammatory arthritis, theres no swelling or lab marker; instead, tenderness points and a cloudy feeling dominate the picture.
Infections and toxins
Sometimes a virus or bacteria hijacks your joints. Parvovirus, Lyme disease, and even COVID19 have been linked to sudden, widespread joint discomfort. notes that joint pain from infection often comes with fever, rash, or a recent tick bite.
Quick comparison of common causes
| Cause | Typical Symptoms | RedFlag Clues | Common Age |
|---|---|---|---|
| Rheumatoid arthritis | Symmetric pain, morning stiffness >30min | Rapid joint erosion | 3060y |
| Osteoarthritis | Pain worsens with use, mild swelling | Sudden severe pain after trauma | >50y |
| Fibromyalgia | Widespread ache, fatigue, sleep trouble | Tender points, no inflammation | 2050y |
| Infection (e.g., Lyme) | Joint pain + fever, rash | High fever, joint effusion | Any age |
Red Flag Symptoms
Extreme fatigue and joint pain
If youre battling both muscle and joint pain with fatigue, it could be a systemic issue like lupus or a hidden infection. Pay attention to night sweats, unexplained weight loss, or a persistent rash those are green lights for a prompt medical visit.
Swelling, deformity, or loss of motion
Any visible swelling, a joint that wont straighten, or a new deformity (think knobby fingers) deserves immediate evaluation. Even if the pain isnt terrible, structural damage can creep in silently.
Young adults and joint pain
Dont assume youre too young for serious joint issues. Earlyonset rheumatoid arthritis, juvenile idiopathic arthritis, and even metabolic problems like hyperuricemia can appear in people in their 20s and 30s. If youre in this age group and wonder joint pain causes in young adults, its worth a chat with a rheumatologist.
Minicase stories
- Case 1: Alex, 24, a marathon runner, woke up with all my joints hurt suddenly after a mild fever. Blood tests revealed a viral arthropathy symptoms faded with rest and hydration.
- Case 2: Maya, 38, a office manager, reported multiple joint pain without swelling. Imaging and labs confirmed early rheumatoid arthritis; early DMARD therapy prevented further damage.
Diagnostic Roadmap
History & physical exam
First, your doctor will listen to your story when the pain started, how it moves, and any accompanying symptoms. A handson exam can reveal subtle tenderness, swelling, or limited range of motion that you might not have noticed.
Lab workup
Common blood tests include:
- Complete blood count (CBC) checks for infection or anemia.
- ESR/CRP measures inflammation.
- Rheumatoid factor and antiCCP markers for rheumatoid arthritis.
- ANA screening for lupus.
- Uric acid and thyroid panel rule out gout or thyroid disease.
Imaging studies
Xrays show bone erosion or joint space narrowing. Ultrasound can spot early synovitis that Xrays miss, while MRI is the gold standard for detecting subtle joint damage in the first months of disease.
What tests should you ask for?
If you feel overwhelmed, bring a simple checklist: CBC, ESR/CRP, rheumatoid factor, antiCCP, ANA, uric acid, thyroid panel, Xray of the most painful joint, and an ultrasound if available. Your doctor will tailor it, but having a list shows youre engaged.
Treatment Options
Firstline symptom relief
Overthecounter NSAIDs like ibuprofen or naproxen can calm inflammation and pain. Pair them with ice packs for 1520 minutes after activity, and heat for stiff mornings. Gentle movementthink short walks or swimmingkeeps joints lubricated without overloading them.
Diseasemodifying therapies
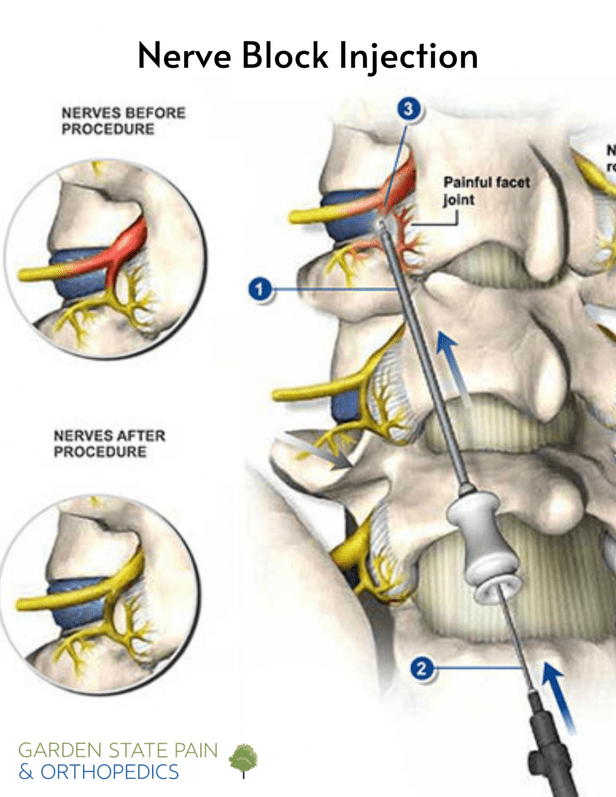
If labs point to an inflammatory arthritis, diseasemodifying antirheumatic drugs (DMARDs) become the backbone of treatment. Methotrexate is often the first choice; biologic agents (TNF inhibitors, IL6 blockers) step in if symptoms persist. These drugs aim to halt joint damage, not just mask pain.
Managing noninflammatory pain
For fibromyalgia or hypermobility, lowdose antidepressants (like duloxetine) and cognitivebehavioral therapy can reduce pain perception. Structured exercise programsstarting with 510minutes of lowimpact activity and gradually building uphelp rebuild strength without triggering flareups.
Lifestyle toolbox
- Antiinflammatory diet: Load up on omega3 rich fish, berries, leafy greens, and cut back on processed sugars.
- Sleep hygiene: Aim for 79hours, keep a dark room, and avoid screens before bed.
- Stress reduction: Mindfulness meditation or gentle yoga can lower cortisol, which in turn eases joint inflammation.
- Complementary therapies: Acupuncture, massage, or taichi can be soothing, but always check with your physician first.
Living with Joint Pain
Daily habits that protect joints
Small tweaks make a big difference. Adjust your workstation so your wrists stay neutral, wear supportive shoes, and use a padded floor mat if you stand a lot. Break up long periods of sitting with a 2minute stretch every hour.
Support networks
Youre not alone. Organizations like the Arthritis Foundation and Fibromyalgia Support Groups offer webinars, local meetups, and reliable literature. Connecting with people who get it can lift your spirits and give you fresh coping ideas.
Monitoring progress
Keep a simple pain journal: note the time of day, activity level, pain intensity (010 scale), and any new symptoms. Apps that calculate HAQ (Health Assessment Questionnaire) or WOMAC scores can turn your notes into a clear picture you can share with your doctor.
Quickanswer box
Q: Can I exercise if every joint hurts?
A: Yes lowimpact activities like swimming, cycling, or waterbased aerobics keep joints moving without pounding them. Start with 510minutes, listen to your body, and increase gradually.
Balancing Benefits & Risks
Medication sideeffects vs. disease progression
Longterm NSAID use can irritate the stomach lining and affect kidney function. Biologics, while powerful, may raise infection risk. The trick is to weigh these downsides against the danger of uncontrolled inflammation, which can permanently damage cartilage.
Personalized care plans
Age, comorbidities, lifestyle, and even your personality shape the best treatment mix. A 30yearold athlete might lean toward physical therapy and a short course of NSAIDs, while a 65yearold with heart disease may need a lowerdose DMARD plus strict monitoring.
Key takeaways
- Identify redflag symptoms early dont ignore fever, severe swelling, or sudden loss of motion.
- Work with a healthcare provider to get the right labs and imaging.
- Combine medication with lifestyle changes for the best longterm outcome.
- Stay connected to supportive communities and track your progress.
Widespread joint pain is a signal, not a sentence. By understanding the possible causes, staying alert to warning signs, and embracing a balanced treatment plan, you can move from ouch to I feel in control. If anything in this article sparked a question or you have a story to share, feel free to reach out were in this together.
FAQs
What are the most common causes of widespread joint pain?
The most common causes include inflammatory arthritis (such as rheumatoid or psoriatic arthritis), osteoarthritis, autoimmune diseases (like lupus), fibromyalgia, and infections such as the flu or COVID-19[1][3].
When should I see a doctor for joint pain?
You should see a doctor if you have severe swelling, joint deformity, loss of motion, or if pain persists without a clear cause or is accompanied by fever, rash, or unexplained weight loss[1].
Can fibromyalgia cause widespread joint pain?
Yes, fibromyalgia often causes widespread pain throughout the body, fatigue, and sleep disturbances, but unlike arthritis, it does not cause joint swelling or damage[1][3].
What tests are used to diagnose the cause of widespread joint pain?
Common tests include blood work (CBC, ESR/CRP, rheumatoid factor, ANA, uric acid, thyroid panel) and imaging studies (X-rays, ultrasound, MRI) to check for inflammation, infection, or joint damage[2][3].
What are some effective ways to manage widespread joint pain at home?
Over-the-counter NSAIDs, hot/cold therapy, gentle exercise, an anti-inflammatory diet, good sleep hygiene, and stress reduction techniques can all help manage symptoms, but persistent pain should be evaluated by a healthcare provider[1][2][4].