Looking for fast relief from that nagging back ache? A back pain treatment injectionmost often a lumbar epidural steroid injectiondelivers anti-inflammatory medication right where the nerves are irritated, giving you a chance to move without that constant burning. It works, but it isn't a magic wand; the benefits come with costs, potential side effects, and a few decisions you'll want to weigh before signing the consent form.
How They Work
What Is a Lumbar Epidural Steroid Injection?
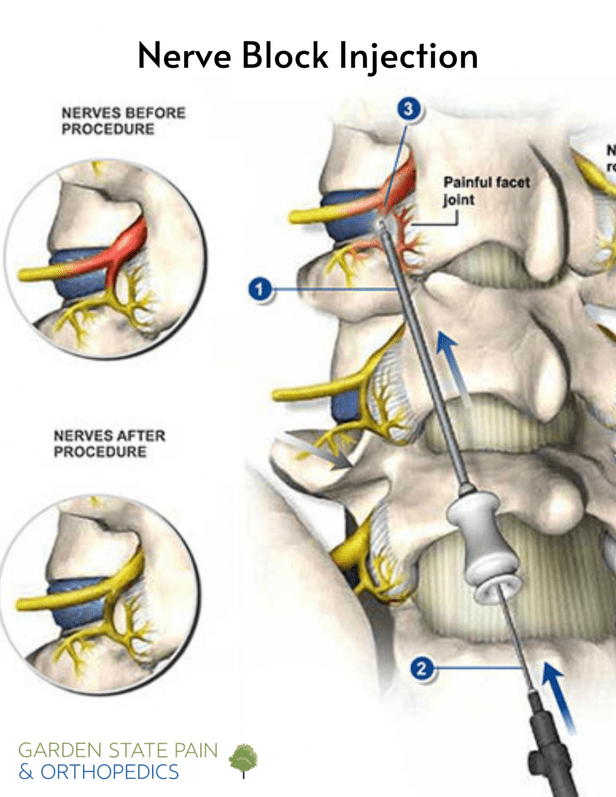
Think of your spine like a busy highway. When an accident (a herniated disc, arthritis, or swelling) blocks the lanes, traffic (pain signals) backs up and you feel the pain down the leg. An epidural steroid injection (ESI) drops a small amount of steroidoften dexamethasone or triamcinoloneright into the epidural space, the little cushion-filled tunnel around the spinal nerves. The medication calms the inflammation, clears the traffic jam, and the pain eases. According to , most patients notice relief within a few days.
Why Dexamethasone?
Dexamethasone is a nonparticulate steroid that's less likely to cause tiny clots in the bloodstream, making it a popular choice for cervical and lumbar injections. If you've read about dexamethasone injection for back pain, you're probably spotting it in the drug-name list on a prescription padbecause doctors often prefer it for its safety profile.
Injection Types
Back pain isn't a one-size-fits-all problem, and neither are the injections. Below is a quick rundown of the most common names of pain injections you'll encounter, plus a glimpse at cost and side-effect profiles.
| Injection Type | Primary Target | Typical Use | Cost (US$) | Common Side Effects |
|---|---|---|---|---|
| Epidural Steroid Injection (ESI) | Spinal nerve roots | Sciatica, herniated disc, spinal stenosis | 3001,200 per shot | Temporary soreness, headache, mild nausea |
| Facet Joint Injection | Facet joints | Arthritic facet pain | 250800 | Bruising, temporary numbness |
| Sacroiliac (SI) Joint Injection | SI joint | Lower back/pelvic pain | 200700 | Local swelling, rare infection |
| Trigger-Point Injection | Myofascial knots | Muscle-related pain | 100300 | Minor bleeding, brief discomfort |
| Selective Nerve Root Block | Specific nerve | Precise diagnosis of nerve pain | 350950 | Transient weakness, allergic reaction |
What Is the Best Injection for Sciatica?
If you've Googled what is the best injection for sciatica, you'll see two names pop up most often: the standard lumbar ESI and the selective nerve root block. Studies from the suggest that ESIs offer broader pain relief for most patients, while nerve root blocks are great for pinpointing the exact culprit when the diagnosis is uncertain.
The Dark Side of Epidural Steroid Injection
Every medical option has a shadow side, and ESIs are no exception. While most people experience only mild, short-lived side effects, there are rare but serious complications that deserve a mention:
- Infection: Introducing a needle into the spine, even under sterile conditions, carries a small infection risk.
- Dural puncture: Accidental tear of the covering around the spinal cord can cause a post-dural puncture headache, which can linger for weeks.
- Systemic steroid effects: Blood-sugar spikes, especially in diabetics, and temporary suppression of the adrenal glands.
According to a review in , these complications occur in less than 1% of cases, but they're why a candid conversation with your physician is essential.
Benefits vs Risks
Proven Benefits
When the injection hits the right spot, the payoff can feel like a fresh breeze after a sweltering summer day. Research shows that about 6070% of patients report at least a 50% reduction in pain within a week of the first ESI. The relief often translates into better mobility, less reliance on oral pain meds, andcruciallya shorter window of disability.
Potential Risks & Side Effects
Balance is the name of the game. Here's a quick cheatsheet of the types of injections for back pain side effects you'll most likely read about:
- Short-term: headache, facial flushing, temporary weakness, bruising at the injection site.
- Long-term (rare): cartilage degeneration, steroid-induced osteoporosis, nerve damage.
For anyone with uncontrolled diabetes, a steroid injection can push blood-sugar levels sky-high. If you're on blood thinners, your doctor may ask you to pause them for a few days to lower bleeding risk.
Decision-Making Checklist
| Question | Why It Matters | How to Answer It |
|---|---|---|
| Do you have uncontrolled diabetes? | Steroids raise glucose | Discuss alternatives or tighter glucose monitoring with your doctor |
| Are you on blood thinners? | Higher bleed risk | Plan a temporary pause under medical supervision |
| How long have you had pain? | Acute vs. chronic influences efficacy | Chronic cases may need a series of injections |
| Have you had recent spine surgery? | Infection risk climbs | Delay injection or opt for a different approach |
Procedure Journey
Pre-Procedure Prep
Before the day of the injection, your doctor will review your medication listespecially anything that thins your blood, like aspirin or warfarin. You'll also get a quick imaging scan (fluoroscopy or CT) to map out the exact needle pathway. Some clinics ask you to fast for a few hours, just to keep the stomach empty in case they need a mild sedative.
Day-Of Steps
Here's what typically happens, broken down into bite-size moments:
- Check-in & consent: You'll sign a form confirming you understand the benefits and risks.
- Positioning: Most people lie on their side with knees drawn up (the fetal position) to open the spaces between the vertebrae.
- Sterile prep & local anesthetic: The skin is cleaned, and a tiny dose of lidocaine numbs the entry point.
- Needle placement: Using real-time X-ray guidance, the doctor threads a thin needle into the epidural space.
- Medication delivery: The steroidanesthetic mix is injected, and you'll stay still for a few minutes while the doctor watches for any immediate reaction.
- Observation: Most clinics keep you for 3045 minutes post-procedure to ensure you're stable.
Post-Procedure Care
After you're back home, treat the area gently. Rest for the first 2448 hours, avoid heavy lifting, and use a cold pack for the first day if you notice swelling. Hydration helps flush out the anesthetic. If you develop a fever, worsening pain, or a sudden loss of sensation, call your provider right awaythose could be signs of infection or nerve irritation.
Money Matters
Cost Ranges
Even before you step into a clinic, the types of injections for back pain cost can vary widely. Here's a snapshot of typical U.S. price brackets (out-of-pocket, before insurance):
- ESI: $300$1,200 per shot
- Facet joint injection: $250$800
- SI joint injection: $200$700
- Trigger-point injection: $100$300
Prices shift based on geography, the facility's overhead, and whether imaging guidance (fluoroscopy vs. CT) is used. Some hospitals bundle the cost of the imaging and medication, while outpatient centers might charge them separately.
Insurance Tips
Most major insurers cover ESIs when they're deemed medically necessary. The key is the CPT codeusually 62322 for a lumbar epidural steroid injection. If your claim gets denied, ask for an appeal and provide your doctor's note that explains the diagnosis (sciatica, spinal stenosis) and why conservative therapy (physical therapy, NSAIDs) didn't work.
Real-World Example
Jane, a 52-year-old accountant, tried NSAIDs and weeks of physical therapy with little relief. Her insurer initially said no to the first ESI, labeling it experimental. After her pain specialist submitted a detailed letter citing the AAOS guidelines, the insurer approved a series of three injections. Jane paid $850 out-of-pocket for the first shot, but the subsequent two were covered, saving her roughly $1,500.
Choosing the Right Provider
When it comes to anything that involves a needle near your spine, the person holding that needle matters. Look for a board-certified physiatrist, pain-management specialist, or orthopedic spine surgeon with at least five years of experience performing ESIs. Many clinics proudly display the number of procedures they've done annuallyaim for providers who log >200 injections per year, as that volume often translates into steadier hands and fewer complications.
During your consultation, ask these quick questions:
- What's your success rate for patients with similar back pain?
- How do you track side effects after the injection?
- What's the follow-up plan if I don't feel relief?
And don't forget to check for third-party reviews, Joint Commission accreditation, and any patient testimonials that speak to transparency and aftercare support.
Conclusion
Back-pain treatment injections, especially lumbar epidural steroid injections, can be a game-changer when done for the right reasons and with the right guidance. They offer swift, targeted pain relief that often lets you return to the activities you love, but they also carry realistic costs, potential side effects, and limits on how often they can be safely repeated. By understanding how each injection type works, weighing benefits against risks, and partnering with an experienced, trustworthy provider, you can make an informed choice that aligns with your health goals.
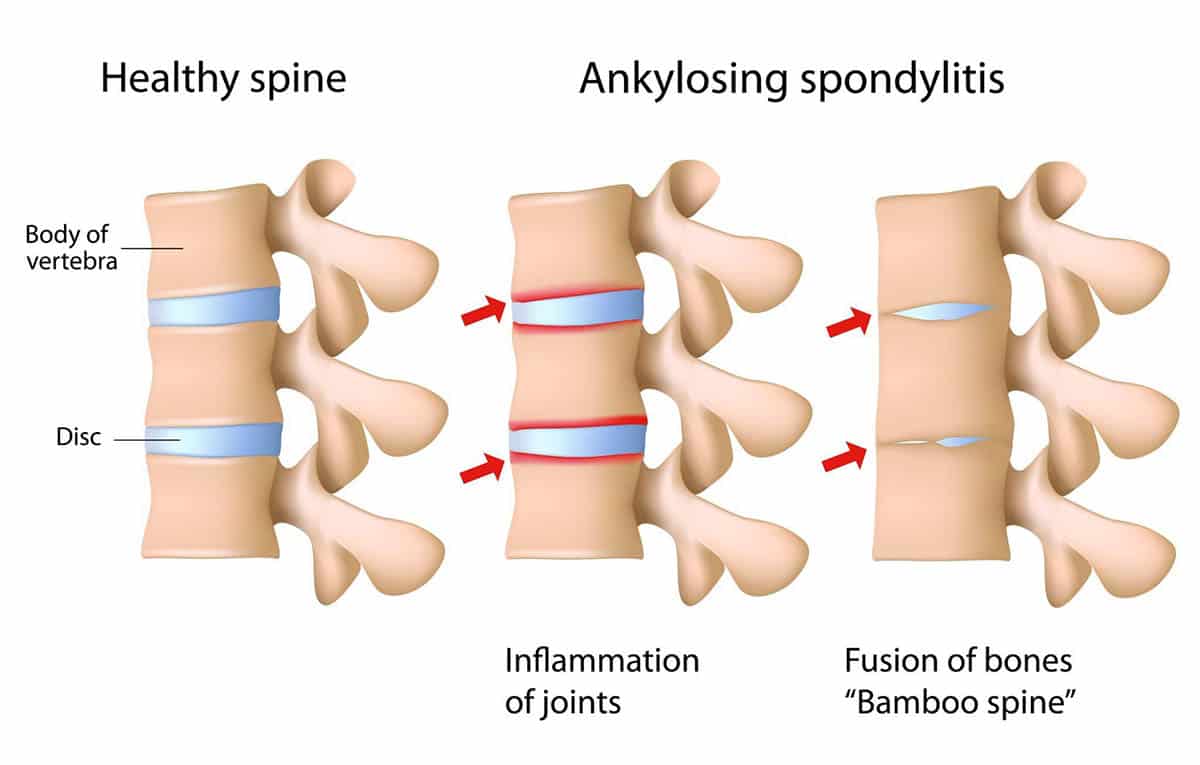
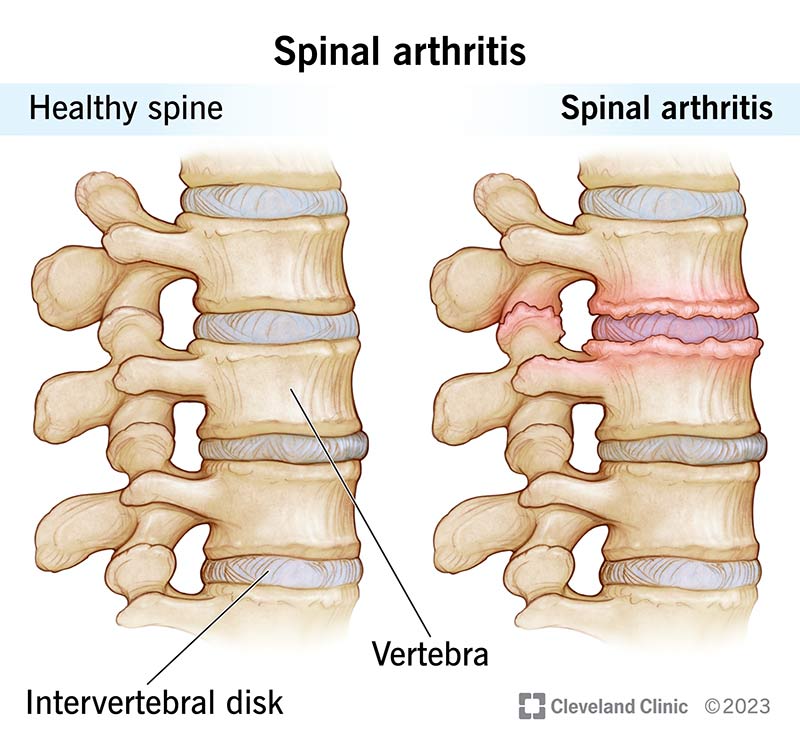
If you're curious about whether an injection might be right for you, schedule a chat with a board-certified pain specialist. Bring this guide along, ask all the questions that matter, and take the next step toward a pain-free tomorrow. For patients with overlapping spinal inflammation or related conditions, consider reading more about spine inflammation to better understand contributing factors and noninvasive management options.
FAQs
What is a back pain treatment injection and how does it work?
A back pain treatment injection, most commonly a lumbar epidural steroid injection, delivers anti‑inflammatory medication directly into the epidural space around the spinal nerves, reducing swelling and interrupting pain signals.
Who is a good candidate for an epidural steroid injection?
Patients with sciatica, herniated discs, spinal stenosis, or facet joint arthritis who have not found adequate relief from physical therapy, oral meds, or rest are typical candidates.
How many injections can I safely receive in a year?
Most specialists limit ESIs to 3–4 shots per year to minimize steroid‑related side effects, though the exact number depends on individual response and medical history.
What are the common side effects and how can they be managed?
Typical short‑term effects include mild soreness, headache, and temporary flushing. Applying ice, staying hydrated, and following post‑procedure rest instructions usually help. Serious complications are rare.
How long does the pain relief from a back pain treatment injection typically last?
Relief can begin within a few days and often lasts from several weeks up to a few months; some patients experience longer‑lasting benefits when combined with physical therapy and lifestyle changes.