Did you know that endometriosis isnt just a young womans problem? Even after the hot flashes and the hormonal rollercoaster of menopause, some women keep feeling the same stubborn pelvic pain, bowel disturbances, or bladder irritation that they thought belonged to their twenties. This isnt just part of getting older its a specific condition called postmenopausal endometriosis. In the next few minutes well unpack what it looks like, why it happens, how doctors figure it out, and what you can actually do about it. Grab a cup of tea, settle in, and lets have a friendly chat about it.
What Is It?
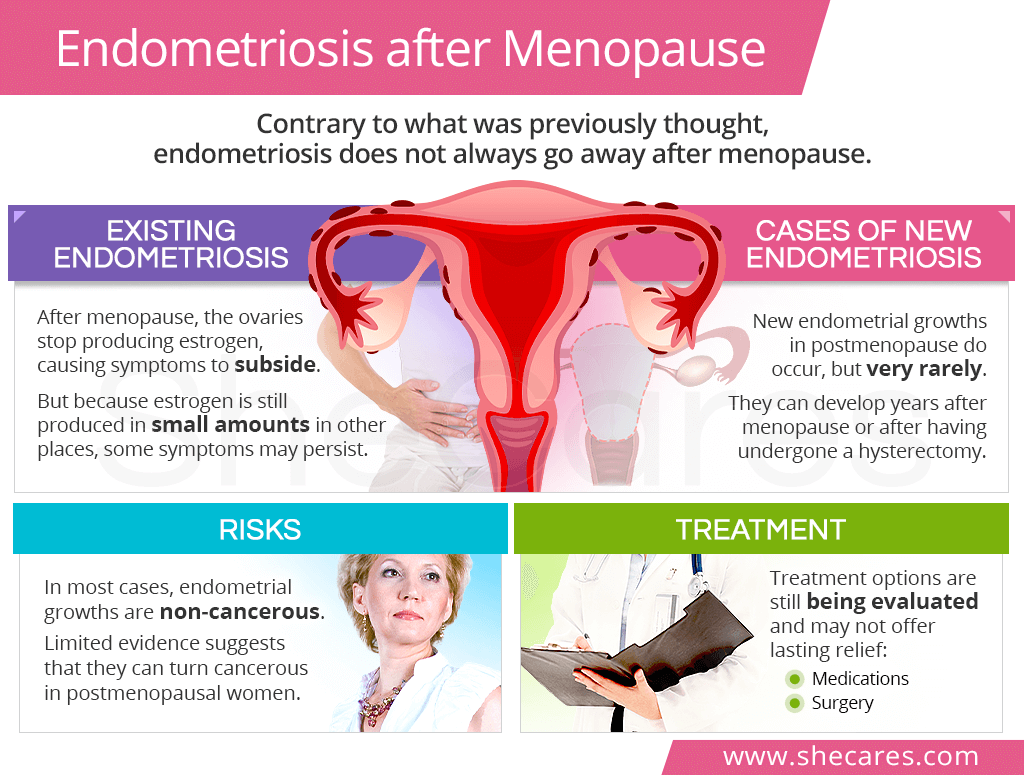
In simple terms, postmenopausal endometriosis is the presence of endometriallike tissue after a woman has stopped having periods. The tissue can still bleed, swell, and cause inflammation, even when the ovaries have largely shut down. Studies suggest it affects roughly 25% of postmenopausal women, and the odds rise if youre taking hormonereplacement therapy (HRT) or have a history of endometriosis before menopause.
Why Does It Stick Around?
Even when ovarian estrogen drops, tiny pockets of estrogen can be made in fat tissue, the adrenal glands, or directly within the endometriotic lesions themselves. Add an exogenous source like a lowdose estrogenprogestin pill and you give those stubborn cells a little fuel to keep the party going. This estrogen threshold concept is highlighted in a recent review in Aging & Disease (2023), which notes that peripheral conversion of androgens to estrogen can be enough to maintain disease activity.
Expert Insight
We often see women who stopped periods years ago, yet their pain never quit. The key is looking beyond the ovaries and checking for local estrogen production, explains Dr. Laura Mitchell, a gynecologicendocrinology specialist at the Womens Health Institute.
Common Symptoms
Symptoms can be a mixed bag, and thats why theyre easy to overlook. Below is a quicklook table that matches the most frequent complaints with what you might actually be experiencing.
| Symptom | Typical Presentation | When to Seek Care |
|---|---|---|
| Pelvic or abdominal pain | Persistent, dulltosharp; may worsen after intercourse | Immediate especially if new or worsening |
| Bowel changes | Constipation, diarrhea, occasional occult blood; bowel endometriosis after menopause | Prompt rule out colorectal issues |
| Bladder irritation | Urgency, dysuria, recurring UTIs; bladder endometriosis after menopause | Prompt especially with blood in urine |
| Unexpected vaginal spotting | Any bleeding after menopause | Immediate could signal malignancy |
| Fatigue or lowback ache | Often dismissed as just aging | When persistent and unexplained |
How to Tell It Apart From Normal Menopause
Menopause can bring its own set of aches, but a few red flags set postmenopausal endometriosis apart:
- Timing: Pain that spikes after sex or during bowel movements.
- Location: Deep, localized tenderness near the uterus, bladder, or sigmoid colon.
- Pattern: Cyclicallike pain that seems to come and go rather than a constant achy feeling.
RealWorld Story
Take Anna, a 62yearold former teacher who started HRT after her periods stopped. Six months in, she began complaining of stomach cramps that felt like gas, plus occasional blood on the toilet paper. After a colonoscopy showed nothing, a pelvic MRI finally revealed a small lesion on the left side of her uterus. Laparoscopic removal gave her back her normal life.
Diagnosis Tools
Diagnosing postmenopausal endometriosis is a bit like detective work. It starts with a thorough history and physical exam, followed by imaging, and often ends with a minimally invasive procedure.
Imaging First
Transvaginal ultrasound is usually the first stop its quick, cheap, and can spot ovarian cysts or deep infiltrating lesions. If the ultrasound is inconclusive, an MRI of the pelvis provides a clearer picture of fibrotic tissue, especially useful for bowel endometriosis after menopause. For any suspicion of malignancy, a CT or PETCT may be added.
What Radiology Shows in LowEstrogen States
According to a 2024 article in Radiology, lesions in postmenopausal women often appear more fibrotic and less cystic than in younger patients, which can make them tricky to spot without a highresolution MRI.
Laparoscopy The Gold Standard
If imaging suggests endometriosis, a diagnostic laparoscopy allows the surgeon to directly visualize and, if needed, excise the tissue. Biopsy confirms the diagnosis and rules out rare malignant transformation.
Doctors Checklist (Downloadable)
When you sit down with your gynecologist, bring this simple list:
- All pain locations and triggers (sex, bowel movements, bladder filling)
- Any recent changes after starting or stopping HRT
- Results of any recent imaging (ultrasound, MRI)
- Questions about the need for biopsy vs. watchful waiting
Treatment Options
Good news: there are several evidencebased ways to tame postmenopausal endometriosis, ranging from medicallydriven hormone tweaks to precise surgery.
Medical Pathways
Lowdose estrogenprogestin therapy can actually help by stabilising the hormonal environment, but its a balancing act too much estrogen may fuel the disease. Aromatase inhibitors (like letrozole) block peripheral estrogen production and are useful for women who cant stop HRT. GnRH agonists or antagonists push the body into a hypoestrogenic state, often combined with addback therapy to protect bone density.
Pros & Cons Table
| Option | How It Works | Best For | Key Risks |
|---|---|---|---|
| Lowdose HRT | Provides steady estrogen & progestin | Mild pain, osteoporosis risk | Potential lesion growth |
| Aromatase inhibitors | Blocks peripheral estrogen synthesis | Women on HRT who cant stop | Joint pain, bone loss |
| GnRH agonist/antagonist | Creates hypoestrogenic state | Severe pain, deep infiltrating disease | Hot flashes, mood swings (addback needed) |
| NSAIDs & neuropathic agents | Pain control | All stages | GI irritation, dependence |
Surgical Solutions
If medication isnt enough, a laparoscopic or robotic excision can remove the offending tissue, relieve adhesions, and restore normal organ function. Surgery carries typical risks infection, bleeding, or need for repeat procedures but for deep bowel or bladder disease, its often the most definitive option.
DecisionMaking Flowchart (Simplified)
1Start with symptoms 2Get ultrasound 3If unclear, MRI 4Medical trial (36months) 5If pain persists or lesions deep, consider laparoscopy.
Risks & Complications
While many women manage their symptoms well, its essential to know the possible complications. Being aware empowers you to act quickly if something changes.
Serious Concerns
- Fibrosis & adhesions can cause chronic pelvic pain even after the lesions are gone.
- Endometriosisassociated ovarian cancer (EAOC) rare, but risk rises with prolonged estrogen exposure.
- Bowel obstruction or fistula especially with deep infiltrating disease involving the colon or rectum.
- Urinary problems recurrent infections, retention, or even hydronephrosis when the bladder is involved.
When to Call an Emergency
Sudden severe abdominal pain, vomiting, or visible blood in stool or urine should be treated as an emergency. These could signal a bowel perforation or a rapidly growing lesion.
Trusted Sources
For a concise governmentbacked overview, see the . It aligns with the data we discuss here and offers patientfocused resources.
Living Well
Besides medical or surgical interventions, everyday habits can make a world of difference. Think of it as a holistic toolbox you can fill with anything that eases your discomfort.
Practical Tips
- Symptom diary write down pain scores, triggers, and menstruallike patterns. Over time youll see patterns that help your doctor tailor treatment.
- Antiinflammatory diet plenty of leafy greens, omega3 rich fish, and limited red meat can reduce systemic inflammation.
- Gentle movement lowimpact cardio, yoga, and pelvicfloor physiotherapy keep muscles flexible and improve blood flow.
- Mindbody care meditation, deepbreathing, or counseling can ease the emotional load that chronic pain often brings.
Support Communities
Connecting with others who get it can be a lifeline. Online forums hosted by the Endometriosis Association and local meetups provide a space to share stories, ask questions, and celebrate small victories.
Conclusion
Postmenopausal endometriosis may feel like an unexpected guest after years of menopause is over. Yet with the right knowledge, a clear line of communication with your healthcare team, and a few lifestyle tweaks, you can regain control of your body and your peace of mind. If any of the symptoms above sound familiar, dont brush them offschedule an appointment, bring your symptom diary, and explore the treatment options that feel right for you. Were all in this together, and sharing experiences makes the journey a little less lonely. Feel free to comment below with your story or any questionsyoure not alone, and were here to help.
FAQs
What are the most common symptoms of postmenopausal endometriosis?
Typical signs include persistent pelvic or abdominal pain, bowel changes (constipation, diarrhea, or occult blood), bladder irritation (urgency, dysuria, recurrent UTIs), unexpected vaginal spotting, and chronic low‑back ache.
How is postmenopausal endometriosis diagnosed?
Diagnosis starts with a detailed history and physical exam, followed by transvaginal ultrasound. If needed, a pelvic MRI provides clearer images, and definitive confirmation is often achieved via diagnostic laparoscopy with biopsy.
Can hormone‑replacement therapy (HRT) worsen postmenopausal endometriosis?
Yes. Exogenous estrogen from HRT can act as a fuel for residual endometrial tissue, especially in women with a prior history of endometriosis. Low‑dose combined estrogen‑progestin regimens may help some, but the balance must be carefully managed.
What medical treatments are available for this condition?
Options include low‑dose estrogen‑progestin therapy, aromatase inhibitors (e.g., letrozole), GnRH agonists/antagonists (often with add‑back therapy), and symptom‑targeted NSAIDs or neuropathic pain agents.
When is surgery recommended for postmenopausal endometriosis?
Surgery is considered when pain persists despite optimal medical therapy, when lesions are deep (involving bowel or bladder), or when there is suspicion of malignant transformation. Laparoscopic or robotic excision can remove the tissue and relieve adhesions.