So, youve probably heard the term Hashimoto brain disease tossed around and wondered what on earth it means. In short, its a rare, autoimmunerelated encephalopathy that can cause seizures, memory fog, and mood swings but the good news is that most people respond well to treatment and can lead normal lives. Below, Ill walk you through everything you need to know, from the basics to how doctors diagnose it, the treatment options, and what the outlook looks like.
Understanding the Condition
What exactly is Hashimotos Encephalopathy?
Also called steroidresponsive encephalopathy or SREAT, Hashimotos encephalopathy (sometimes shortened to Hashimoto encephalopathy) is an inflammatory brain condition linked to the same autoimmune antibodies that cause Hashimotos thyroiditis. The brain gets caught in the crossfire, leading to a mix of neurological and psychiatric symptoms. Its not just a thyroid problem the brain involvement makes it a distinct entity, which is why its often compared with Hashimotos thyroiditis in the medical literature.
Who gets it?
Although anyone can develop it, the condition primarily affects women (about 90% of cases) and typically shows up between the ages of 30 and 60. People with other autoimmune diseases like rheumatoid arthritis or lupus might be at a slightly higher risk, too. Occasionally, symptoms might overlap or be initially mistaken for rare neurological syndromes such as atypical Rett syndrome, which is another disorder presenting with varied neurological symptoms.
Why does it happen? (Current theories)
Researchers arent 100% sure yet, but the leading theory is that antibodies aimed at the thyroid (especially antiTPO) also mistakenly target brain tissue. Inflammation, cytokine release, and possibly a viral trigger can all fan the flames. A recent study suggests that these antibodies may cross a leaky bloodbrain barrier, igniting the brains immune response.
Spotting the Signs
Core neurological symptoms
- Seizures often hard to control with standard antiepileptic drugs.
- Confusion or brain fog that comes and goes.
- Memory lapses and trouble concentrating.
Psychiatric manifestations
- Sudden mood swings, anxiety, or depression.
- Episodes that look like psychosis or reversible dementia.
Other possible clues
- Persistent headaches, ataxia (loss of coordination), or visual disturbances.
- Hearing loss or tinnitus.
Quick SymptomRating Table
| Symptom | Present? | Frequency |
|---|---|---|
| Seizures | Occasional / Daily | |
| Brain fog | Several times a day | |
| Memory loss | ||
| Mood swings | Often |
Feeling a little dizzy reading this? I once talked to a friend who thought her stressinduced forgetfulness was just part of a busy life. It wasnt until she started having brief seizures that the diagnosis finally clicked. Youre not alonerecognizing the pattern early can save a lot of worry.
Diagnosis Process
Key tests & what they reveal
| Test | What it shows | Typical result in HE |
|---|---|---|
| Blood work thyroid antibodies (TPO, Tg) | Autoimmune activity level | Often elevated |
| EEG | Brain electrical activity | Diffuse slowing, sometimes epileptiform spikes |
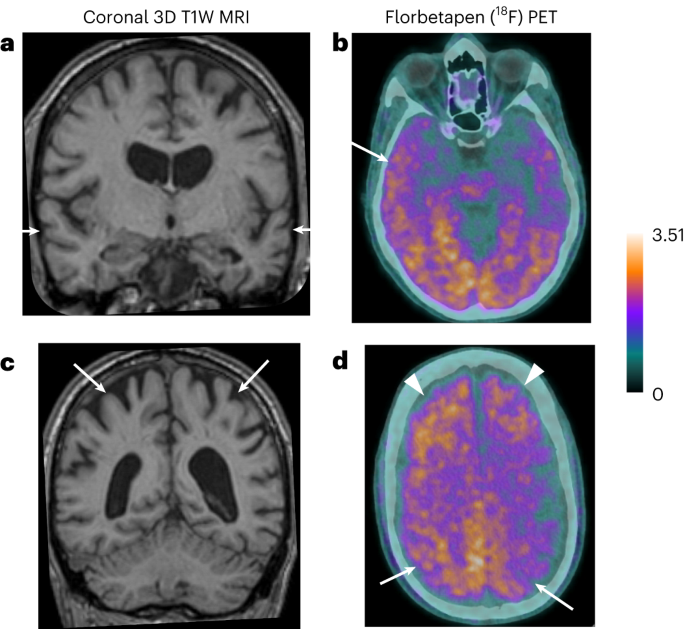
| MRI | Structural brain changes | May be normal; occasionally frontal lobe atrophy (hashimoto's encephalopathy mri findings) |
| CSF analysis | Inflammation markers | Elevated protein, normal glucose |
| Neuropsych testing | Cognitive baseline | Helps track improvement after treatment |
There isnt a single definitive test. Diagnosis is a blend of clinical observation, lab results, and ruling out other causes (like infections, metabolic disturbances, or other autoimmune encephalopathies). In other words, doctors use a hashimoto's encephalopathy test panel of sorts, but the final call rests on the overall picture. If the presentation involves unusual neurological or movement symptoms, clinicians might also consider alternative causes, such as fencing response meaning in the context of seizures or transient neurological events.
When to suspect and when to refer
If you notice rapidonset seizures, sudden memory loss, or unexplained mood changes, its time to see a neurologist. A coordinated approach neurology + endocrinology usually yields the quickest, most accurate diagnosis.
Treatment Options
Firstline: Steroid therapy
Highdose oral prednisone (often 6080mg per day) is the goto treatment. Most patients start feeling better within a week, and around 80% see significant improvement within a month. The key is a careful taper to avoid rebound inflammation.
Steroidsparing agents
If steroids cause side effects or dont fully control symptoms, doctors may add:
- Azathioprine or mycophenolate
- Intravenous immunoglobulin (IVIG)
- Plasma exchange in severe cases
Managing symptoms
Antiepileptic drugs (AEDs) help control seizures while steroids take care of the underlying inflammation. Cognitive rehab, therapy, and a good sleep routine can also smooth out the brain fog.
Lifestyle & supportive care checklist
- Prioritize 79 hours of sleep nightly.
- Practice stressrelief techniques (gentle yoga, meditation).
- Maintain a balanced diet rich in omega3s and vitamin D.
- Stay hydrateddehydration can worsen cognitive symptoms.
My cousin, whos been on steroids for six months, swears by a morning brainboost smoothie (spinach, berries, and a splash of almond milk). Its not a cure, but those tiny daily wins keep morale up.
Prognosis & Life Expectancy
Is Hashimotos encephalopathy fatal?
Rarely. When the condition is identified early and treated with steroids, mortality is exceptionally low. Most deaths that do occur stem from untreated severe seizures or complications from prolonged highdose steroidsnot the encephalopathy itself.
Longterm outlook
People generally enjoy a normal life expectancy. However, about 30% experience relapses, meaning they might need a lower maintenance dose of steroids or another immunosuppressant down the road. Cognitive recovery is often good, though a small subset may retain mild deficits (like occasional wordfinding trouble).
Comparing HE vs. Hashimotos thyroiditis outcomes
| Aspect | Hashimoto Encephalopathy | Hashimoto Thyroiditis |
|---|---|---|
| Primary organ affected | Brain (central nervous system) | Thyroid gland |
| Typical symptoms | Seizures, confusion, mood swings | Fatigue, weight gain, cold intolerance |
| Firstline treatment | Highdose steroids | Levothyroxine hormone replacement |
| Prognosis | Usually good with early therapy | Generally excellent; lifelong medication |
RealWorld Stories
Patient case summaries
Case 1: A 42yearold woman experienced sudden memory gaps and blurry vision. After a full workup (elevated TPO antibodies, abnormal EEG), she started prednisone and fully recovered in six weeks. She now volunteers with a raredisease support group.
Case 2: A 58yearold man had refractory seizures that didnt respond to typical AEDs. Adding mycophenolate to his steroid regimen steadied his condition, and hes been seizurefree for over a year.
Trusted resources
For anyone looking to dive deeper, reputable organizations like the and the provide uptodate guidelines and patient stories. If you are interested in symptom overlap or differential diagnosis for similar conditions, you might explore more resources on Rett syndrome criteria or related neurological disorders.
Conclusion
Hashimoto brain disease may sound intimidating, but with the right knowledge and a proactive medical team, most people live full, vibrant lives. Recognizing the hallmark symptomsseizures, confusion, and mood changesgets you to the right doctors fast, and the steroidresponsive nature of the illness offers a solid chance of recovery. If you or a loved one notice these signs, dont waitreach out to a neurologist or endocrinologist today. Early action truly makes the difference.
Feel free to share your own experiences in the comments, download our printable symptomchecklist, or join an online community for support. Together we can turn uncertainty into confidence.
FAQs
What exactly is Hashimoto brain disease?
Hashimoto brain disease, also called Hashimoto’s encephalopathy or SREAT, is a rare autoimmune‑related inflammation of the brain linked to thyroid antibodies.
What are the most common symptoms?
Typical signs include seizures, episodic “brain fog,” memory problems, mood swings, anxiety, and sometimes headaches, ataxia, or visual disturbances.
How is the condition diagnosed?
Doctors combine clinical assessment with blood tests for thyroid antibodies (anti‑TPO/Tg), EEG, MRI, CSF analysis, and neuropsychological testing while ruling out other causes.
What treatments are available?
The first‑line therapy is high‑dose corticosteroids (prednisone). If needed, steroid‑sparing agents like azathioprine, mycophenolate, IVIG, or plasma exchange are added, plus seizure control meds and supportive lifestyle changes.
Can Hashimoto brain disease be fatal?
Fatality is rare. Most mortality is linked to untreated severe seizures or complications from long‑term high‑dose steroids, not the encephalopathy itself.