If you notice any warning signs or have risk factors, catching it early can mean the difference between a quick recovery and serious heart damage. Below well walk through what creates a clot, how to spot it, what doctors do to dissolve it, and how you can keep it from happening again.
Understanding Coronary Thrombosis
What is coronary thrombosis?
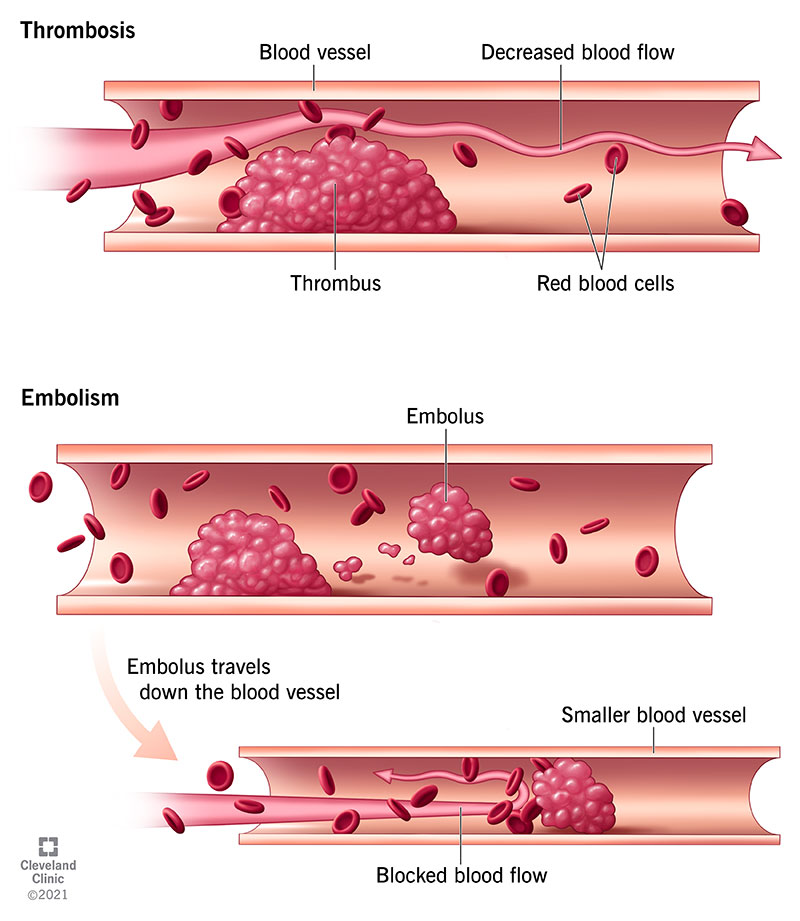
In plain language, a thrombosis is a clot, and when it settles in a coronary artery its called coronary thrombosis. The clot can form on top of a ruptured plaquea fatty deposit that has been building up in the artery wall for years. Once the clot blocks the artery, the heart muscle downstream begins to starve for oxygen. This is the physiological engine behind many heart attacks.
Coronary thrombosis is also known as
Medical literature may refer to the condition as a coronary artery thrombus, coronary clot, or simply an intracoronary thrombus. All these terms point to the same dangerous blockage.
Quick Fact Box
| Fact | Details |
|---|---|
| Typical Age | 4575 years, but can appear younger with strong risk factors |
| Gender Trend | Men are 23 more likely; womens risk rises after menopause |
| Key Trigger | Rupture of an atherosclerotic plaque |
| Outcome With Prompt Care | Survival >90% when treated within the first hour |
Causes and Risk Factors
What triggers a clot in the hearts arteries?
The primary culprit is a ruptured atherosclerotic plaque. When the fibrous cap of a plaque tears, the underlying lipid core meets circulating blood, prompting platelets to stick together and form a clot. Other contributors include:
- Inherited clotting disorders (e.g., Factor V Leiden)
- Chronic inflammation from conditions such as rheumatoid arthritis
- Prolonged immobilization or major surgery
Is coronary thrombosis hereditary?
Family history does play a role, especially if close relatives have earlyonset heart disease or known thrombophilias. Genetic factors can make your blood more sticky, raising the odds that a small plaque rupture will become a fullblown clot.
Other major risk factors
Beyond genetics, lifestyle and health conditions pack a punch. The biggest risk carriers are:
RiskFactor Comparison
| Risk Factor | How it Increases Clot Formation | Simple Mitigation |
|---|---|---|
| Smoking | Damages artery lining, accelerates plaque buildup | Quit using nicotine replacement or counseling |
| High LDL Cholesterol | Feeds plaque growth | Statins or diet low in saturated fats |
| Hypertension | Strains arterial walls, promotes rupture | Regular BP checks; ACE inhibitors if needed |
| Diabetes | Elevates inflammation and plaque instability | Maintain HbA1c <7% with meds and diet |
| Sedentary Lifestyle | Reduces circulation, encourages clotting | 150min moderate exercise weekly |
Symptoms and Warning Signs
Typical symptoms
When a coronary artery gets blocked, the heart sends out distress signals. Most people feel:
- Heavy or crushing chest pressure that may radiate to the left arm, jaw, or back
- Shortness of breath, even at rest
- Cold sweats, nausea, or a vague sense of dread
These sensations often mirror a classic heart attack, because technically a large clot is a heart attack.
Is coronary thrombosis a heart attack?
Yeswhen the clot stops blood flow long enough to damage heart muscle, doctors label it an acute myocardial infarction, or heart attack. The difference is mostly semantic; the underlying problem is the same blockage.
When symptoms are subtle
Some people report atypical signs like indigestion, fatigue, or mild back pain. Women, older adults, and diabetics especially may experience less dramatic chest pain, making early detection trickier.
How It\'s Diagnosed
What tests are used?
Doctors start with a quick electrocardiogram (ECG) to spot electrical changes that suggest a blockage. Blood tests for cardiac enzymes (troponin) confirm heartmuscle injury. If a clot is suspected, imaging steps in:
- Coronary angiography a dyeinjected Xray that visualizes the exact site of the clot.
- CT coronary angiogram a noninvasive scan useful for highrisk patients.
- Intravascular ultrasound (IVUS) provides a crosssection view of plaque and clot inside the artery.
Can it be caught before a heart attack?
Screening highrisk individuals with stress tests or coronary calcium scans can reveal vulnerable plaques before they rupture. A routine exercise stress test is often used to evaluate symptoms and exercise tolerance and can be part of that early detection strategy. However, no test guarantees that a clot wont form tomorrow. Thats why lifestyle control remains essential.
Treatment Options
Immediate emergency care
If a clot is actively blocking flow, time is muscle. Doctors aim to restore perfusion as fast as possible:
- Primary PCI (percutaneous coronary intervention) a balloon and stent open the artery within minutes.
- Thrombolytic therapy clotdissolving drugs (e.g., alteplase) given when PCI isnt immediately available.
- Antiplatelet & anticoagulant meds aspirin, clopidogrel, heparin, or newer agents keep the clot from growing.
Longterm medical management
After the emergency passes, a regimen of medicines keeps you clotfree:
Medication Table
| Drug | Class | Purpose | Typical Dose |
|---|---|---|---|
| Aspirin | Antiplatelet | Prevent new clot formation | 81mg daily |
| Clopidogrel | Antiplatelet | Dual antiplatelet therapy (DAPT) | 75mg daily |
| Atorvastatin | Statin | Lower LDL, stabilize plaque | 4080mg nightly |
| Metoprolol | Betablocker | Reduce heart workload | 25100mg BID |
| Lisinopril | ACE inhibitor | Control blood pressure, protect heart | 1040mg daily |
Surgical options
When blockages are too extensive for stenting, coronary artery bypass grafting (CABG) reroutes blood around the clogged segment using vessels from the leg or chest. Although more invasive, CABG offers excellent longterm survival for multivessel disease.
Expert insight
According to a senior interventional cardiologist at the Cleveland Clinic, Early reperfusionwhether via PCI or thrombolysisremains the most powerful predictor of survival after coronary thrombosis.
Prognosis and Survival Rate
What is the survival outlook?
When treated within the first hour, the 30day mortality drops below 10%. Fiveyear survival climbs above 80% for patients who stay on guidelinedirected medical therapy and adopt hearthealthy habits. Delays, extensive clot burden, or comorbidities (like kidney failure) worsen the outlook.
Coronary artery thrombosis sudden deathhow common?
Sudden cardiac death accounts for roughly 1520% of all coronary thrombosis cases, especially when the clot completely occludes a major artery without warning. A large cohort study published in the Journal of the American College of Cardiology found that immediate PCI reduced suddendeath risk by 50% compared with medical therapy alone.
Prevention Strategies
Modifiable riskfactor control
Quitting smoking, managing blood pressure, and keeping cholesterol in check are the three pillars of prevention. Even modest changeslike swapping a sugary soda for watercan shift your risk profile substantially.
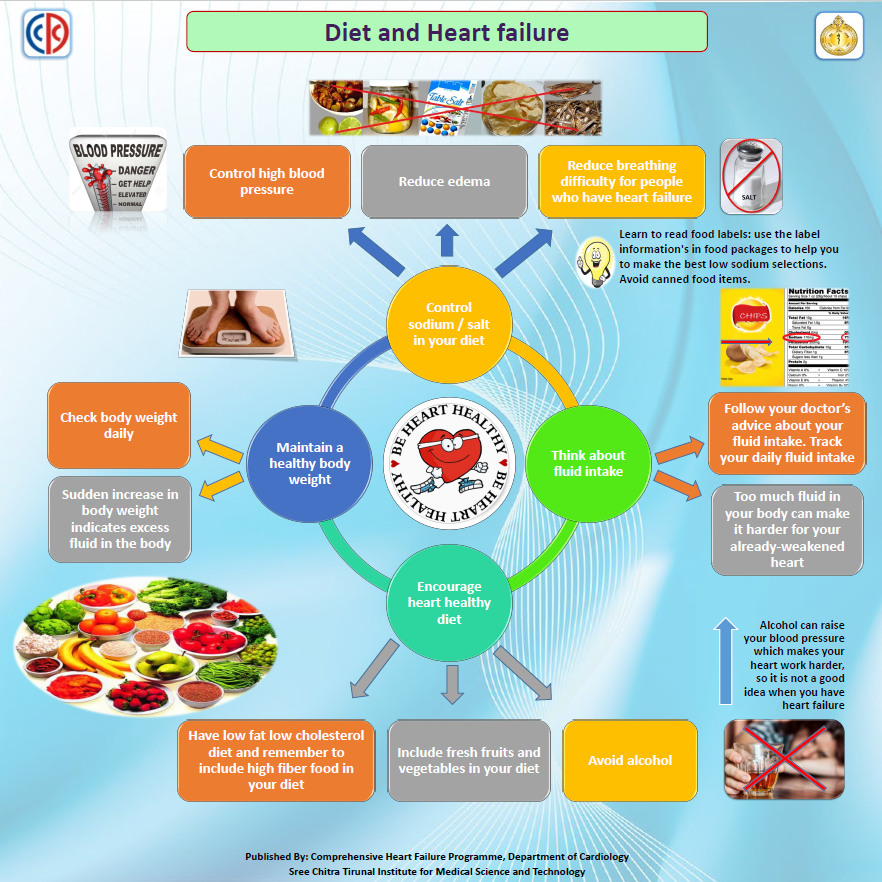
Hearthealthy diet
Think Mediterranean: plenty of leafy greens, olive oil, fatty fish, nuts, and whole grains. These foods lower LDL cholesterol and provide antiinflammatory omega3 fatty acids.
Physical activity & weight management
Aiming for at least 150minutes of moderate aerobic exercise each week (brisk walking, cycling, swimming) improves circulation and makes platelets less prone to clump together.
When to see a doctor
Call emergency services if you experience crushing chest pain, unexplained shortness of breath, or sudden weakness. For nonemergent concerns, schedule a checkup if you have any of these red flags:
- Family history of early heart disease
- Uncontrolled hypertension or diabetes
- Persistent chest discomfort during activity
RealWorld Experience
Patient testimonial (anonymous)
I was in my late 40s and felt a tightness in my chest after a weekend hike. I thought it was just indigestion, but the pressure didnt fade. My wife called 911, and within an hour the ER team opened the artery with a stent. The doctor explained that a tiny plaque had ruptured, and a clot formed right there. Because they acted fast, Im now on a simple regimen of aspirin and a statin, and Ive cut back on red meat. I feel lucky, but I also know I could have been one of those silent cases that never got treatment.
Clinicians perspective
Dr. Elena Martnez, a cardiology fellow, says, Patients often underestimate how quickly a clot can evolve. She stresses the importance of routine blood work, especially checking highsensitivity Creactive protein (hsCRP) as a marker of inflammation that can herald plaque instability.
Key takeaways
- Coronary thrombosis = clot in a heart artery; it often manifests as a heart attack.
- Risk comes from both genetics and lifestylesmoking, high LDL, hypertension, diabetes, inactivity.
- Early symptoms include chest pressure, shortness of breath, and sweating; they can be subtle.
- Fast treatment (PCI or thrombolysis) dramatically improves survival.
- Longterm meds, a hearthealthy diet, exercise, and regular checkups keep you safe.
Remember, knowledge is power. If any of the signs feel familiar, dont waittalk to a healthcare professional today. Youve got the tools, the facts, and a supportive community behind you. Stay curious, stay proactive, and keep your heart happy.
FAQs
What exactly is coronary thrombosis?
It is a blood clot that forms inside a coronary artery, often on a ruptured atherosclerotic plaque, blocking oxygen‑rich blood to the heart muscle.
How can I tell if I am experiencing a coronary thrombosis?
Typical warning signs include crushing chest pressure, pain radiating to the arm or jaw, shortness of breath, cold sweats, nausea, or an unexplained sense of dread.
What immediate treatments are used to dissolve the clot?
Emergency care may involve primary PCI (balloon and stent), thrombolytic drugs to dissolve the clot, and antiplatelet/anticoagulant medications to stop further clot growth.
Can lifestyle changes really lower my risk of another clot?
Yes. Quitting smoking, controlling blood pressure and cholesterol, managing diabetes, regular aerobic exercise, and a Mediterranean‑style diet substantially reduce recurrence risk.
When should I see a doctor if I have risk factors but no symptoms?
Schedule a check‑up if you have a family history of early heart disease, uncontrolled hypertension or diabetes, persistent chest discomfort during activity, or any other major risk factors.