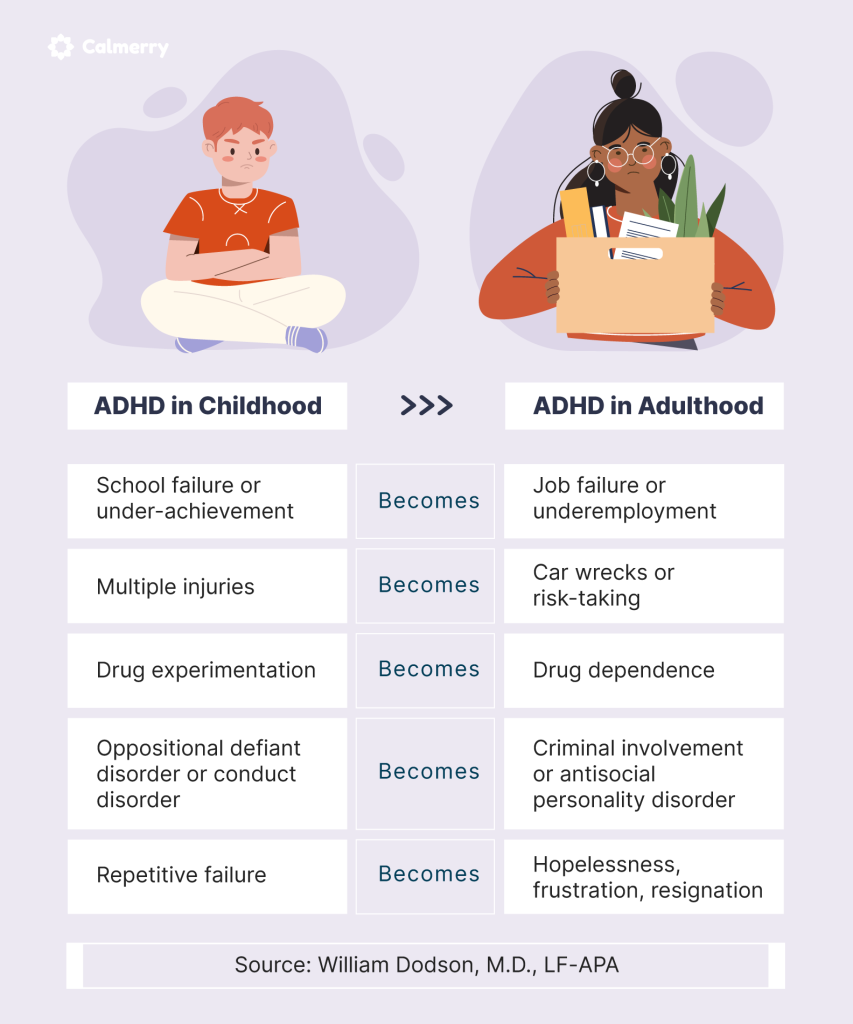
Short answer: Yes. Research shows that traumatic experiencesespecially earlylife traumacan deepen existing ADHD symptoms and even spark ADHDlike difficulties in adults who didn't previously meet criteria.
Short answer: The relationship works both ways. Having ADHD can increase the chance of encountering trauma, and trauma can intensify distractibility, impulsivity, and emotional turbulence. Below we'll unpack why, who's most at risk, how to tell the two apart, and what to do about it.
Why Trauma Connects
What the Science Says
Multiple peerreviewed studies have found a clear link between stressful or traumatic events and heightened ADHD symptoms. For example, a recent metaanalysis reports that individuals who experienced childhood adversity are much more likely to meet ADHD criteria as adults. Experts from Medical News Today point out that trauma can rewire the brain's stress circuits, making it harder for someone with ADHD to regulate attention and impulse control. In other words, the brain's response to threat can mimic and magnify the core challenges of ADHD.
BrainLevel Overlap
Trauma triggers a cascade of neurochemical changesespecially in the prefrontal cortex, amygdala, and dopamine pathways. The prefrontal cortex is the command center for planning and focus; the amygdala flags emotional danger; dopamine helps us stay motivated. When trauma disrupts these systems, it can deepen the executivefunction deficits we already see in ADHD.
Think of it as a radio station: ADHD gives you static on the focus frequency, and trauma cranks up the volume on the stress channel, making everything louder and harder to tune out.
The ChickenorEgg Question
Does ADHD lead to more trauma, or does trauma create ADHD? The answer is both. Kids with ADHD often act impulsively, which can place them in risky situationsbullying, accidents, or even abusive environments. Conversely, chronic exposure to trauma can impair attention networks, producing ADHDlike symptoms even in those without a prior diagnosis.
So it's a twoway street, and that's why a thorough assessment is essential before deciding on treatment.
Who Is Affected
Adults vs. Children
Adults who lived through childhood trauma often report lingering concentration problems, mood swings, and impulsivity that mimic adult ADHD. Studies show that the ADHDplustrauma group tends to have more severe functional impairment than those with ADHD alone.
For children, the picture is similar but more pronounced. The Centers for Disease Control and Prevention's ACE (Adverse Childhood Experiences) study found that higher ACE scores predict a greater likelihood of meeting ADHD criteria before age 12.
Gender Considerations ADHD and Trauma in Women
Women with ADHD are statistically more likely to experience interpersonal trauma, such as emotional or sexual abuse. This isn't just a numbers game; the trauma often intensifies the internalising symptoms (like anxiety and depression) that many women with ADHD already battle.
That overlap can make it tricky to differentiate whether anxiety stems from ADHD, trauma, or both. A traumainformed lens is therefore crucial when evaluating women's mentalhealth presentations. For clinicians looking to better understand trauma's role in attentional symptoms, see this concise overview on ADHD and trauma.
Complex PTSD & ADHD in Adults
Complex PTSD (CPTSD) arises from prolonged, repeated traumathink ongoing abuse or chronic neglect. Its symptom set includes affect dysregulation, dissociation, and persistent negative selfperception, all of which can masquerade as ADHD symptoms.
When CPTSD coexists with ADHD, the two conditions feed each other: hypervigilance can exacerbate distractibility, while impulsivity can trigger flashbacks. Proper differential diagnosis often requires both a trauma questionnaire and an ADHD rating scale.
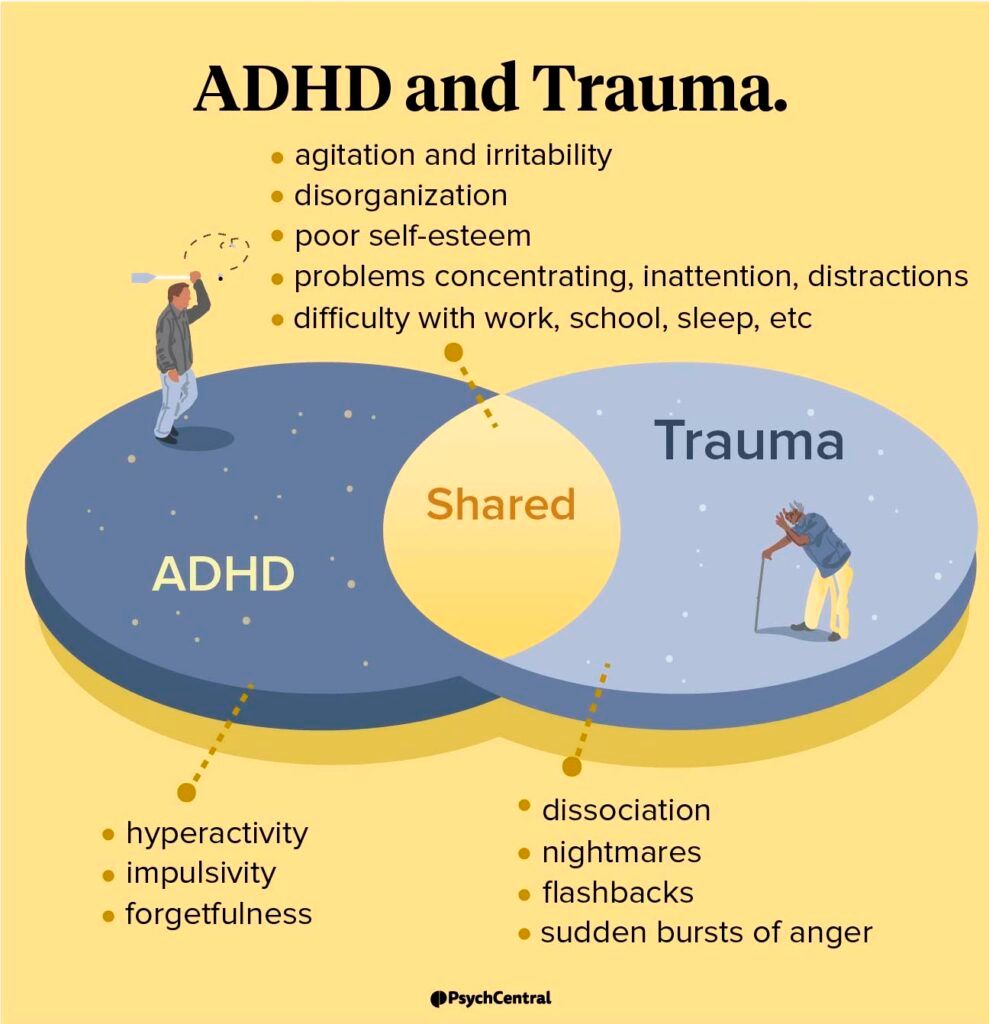
Spotting the Overlap
SymptombySymptom Comparison
| Symptom | Typical ADHD | TraumaRelated (PTSD/CPTSD) | Overlap & How to Differentiate |
|---|---|---|---|
| Distractibility | Persistent difficulty sustaining attention | Hypervigilance to perceived threats | Look for triggerlinked spikes (e.g., after a loud noise) |
| Impulsivity | Acting without thinking, risktaking | Reactive aggression, selfprotective fightorflight | Context matters: safetydriven vs. rewarddriven |
| Mood Swings | Emotional dysregulation, quick to frustration | Affective instability, flashbacks | Traumalinked mood changes often follow reminders |
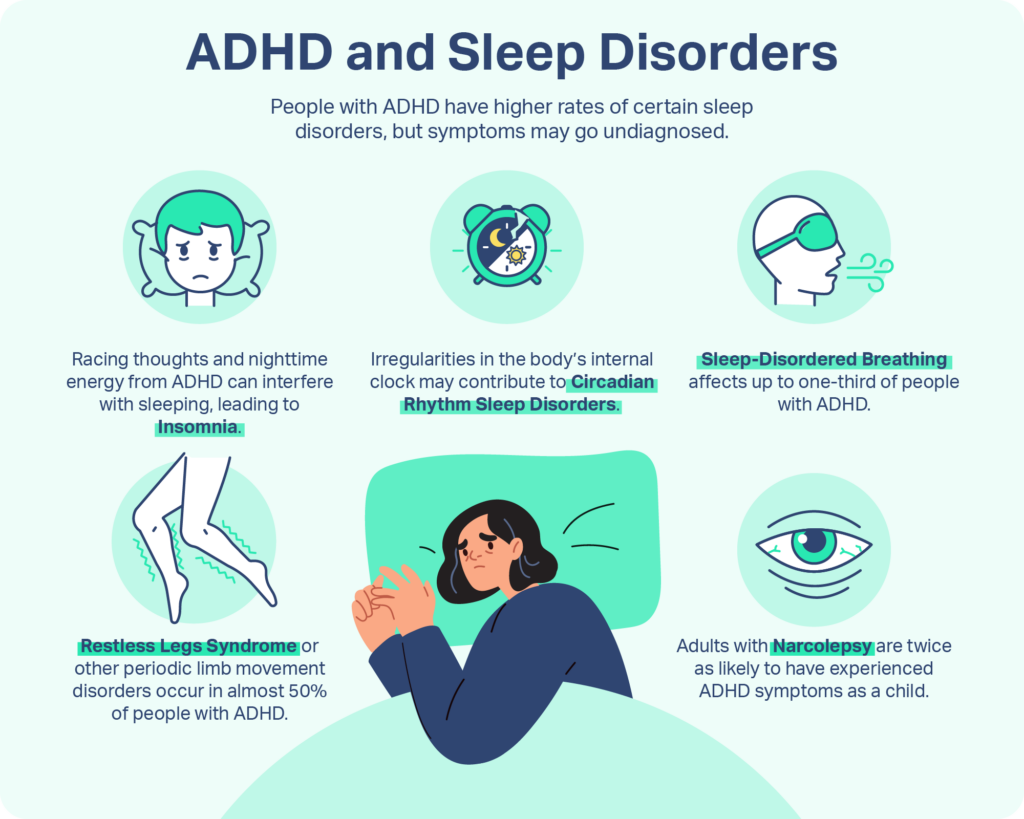
| Sleep Problems | Restlessness, difficulty winding down | Nightmares, insomnia from hyperarousal | Assess dream content vs. physical restlessness |
Common Misdiagnoses
Because the symptom clouds overlap, clinicians sometimes label traumadriven inattention as just ADHD, or viceversa. This can lead to inappropriate medication choicesstimulants may heighten anxiety if trauma isn't addressed first.
Conversely, overlooking ADHD can leave a client stuck in a cycle of selfblame, thinking "I'm just unmotivated" when the underlying neurobiology is more complex.
RealWorld Impact
Personal Story (Optional)
Imagine Maya, a 28yearold graphic designer who's lived with ADHD all her life. After a car accident that left her with a mild concussion, she noticed her brain fog skyrocketshe missed deadlines, felt on edge, and started snapping at coworkers.
When she finally opened up to a therapist, the professional recognized that the trauma from the accident was amplifying her ADHD symptoms. With a combination of EMDR therapy and a modest adjustment to her medication, Maya reports a noticeable calmness returning to her workday.
Reddit & Forum Insights
In a popular mentalhealth subreddit, users often write, "Every time I'm stressed, my ADHD feels like it's on overdrive." These livedexperience snapshots echo what clinicians observe: stress and trauma act as accelerators for ADHDrelated challenges.
Clinical Case Vignettes (Expert Input)
Dr. Lina Patel, a licensed psychologist, shared a brief vignette (with consent) of a 42yearold veteran diagnosed with both CPTSD and ADHD. After coordinated caretraumafocused TFCBT plus a lowdose stimulantthe veteran reported a 30% reduction in intrusive memories and a marked improvement in daily task completion.
Managing the Double Challenge
EvidenceBased Treatments
TraumaFocused Therapy: EyeMovement Desensitization and Reprocessing (EMDR), TraumaFocused Cognitive Behavioral Therapy (TFCBT), and Accelerated Resolution Therapy have all demonstrated efficacy in reducing traumarelated arousal, which indirectly eases ADHD symptoms.
ADHD Interventions: Medication (stimulants or nonstimulants), CBT for executive function, and lifestyle tweaks (exercise, nutrition, sleep hygiene) remain cornerstones. For practical sleep strategies tailored to attention difficulties, consider resources on sleep tips ADHD.
Integrated Care Approach
- Comprehensive Assessment: Use both an ACE questionnaire and an ADHD rating scale (e.g., ASRS) to map the full picture.
- Collaborative Treatment Planning: Ideally, a psychiatrist and a trauma therapist comanage the case, sharing notes and progress.
- Medication Management: Start low, monitor for heightened anxiety or flashbacks, and adjust as needed.
- SkillBuilding: Grounding techniques, mindfulness, and structured routines provide the safety net that trauma therapy builds.
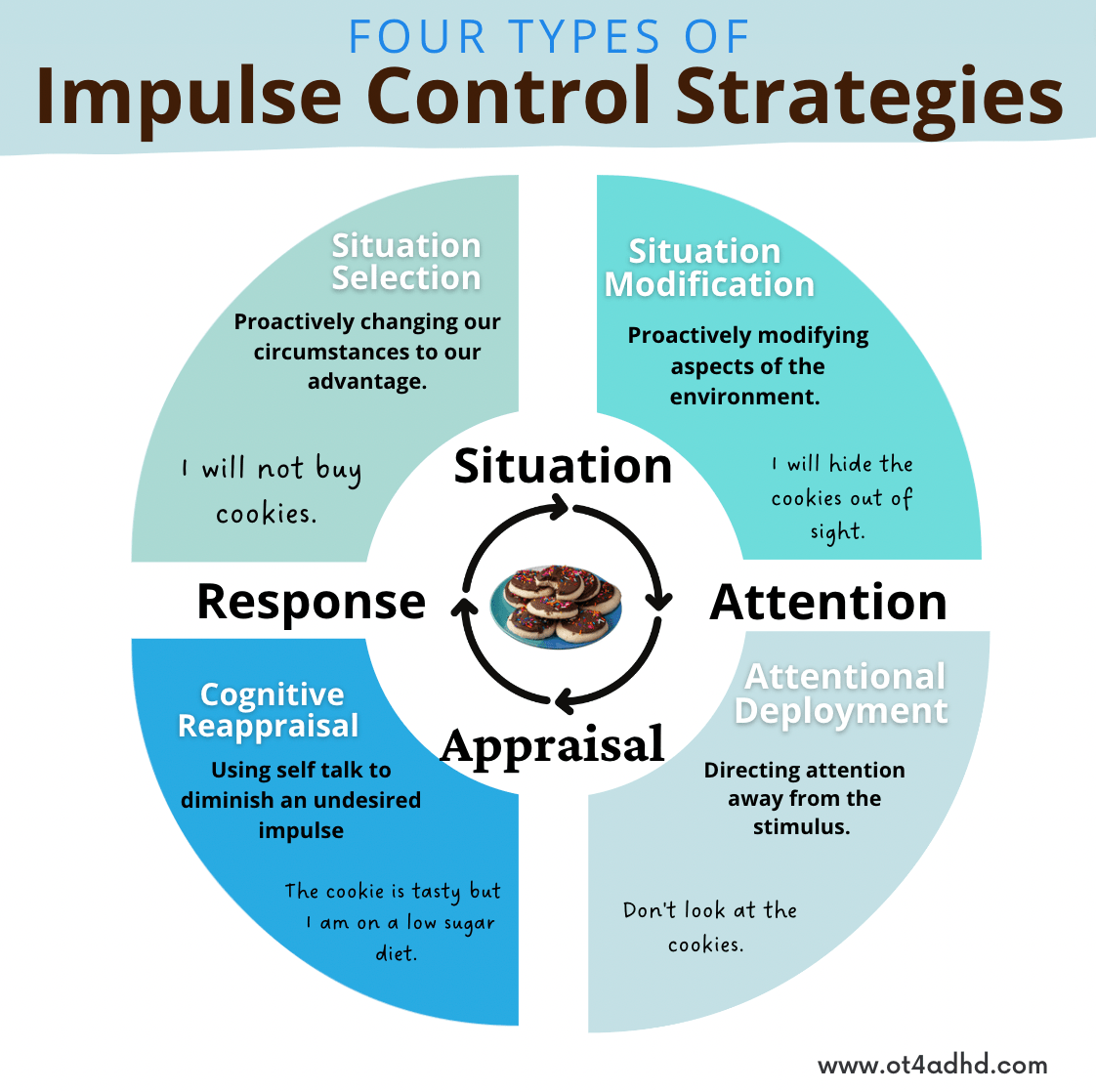
SelfHelp Strategies (Everyday)
Even without professional help, simple habits can make a world of difference. Try a consistent sleep schedule, daily movement (even a brisk walk counts), and a braindump notebook before bed to offload racing thoughts.
Grounding exerciseslike the 54321 sensory checklistcan calm the nervous system during moments when trauma triggers spike your ADHD noise.
When to Seek Professional Help
Watch for red flags: escalating impulsivity that leads to risky behavior, thoughts of selfharm, substance misuse, or severe flashbacks that disrupt work or relationships. If any of these appear, reaching out to a qualified mentalhealth professional is the safest next step.
Bottom Line Balancing Risks & Benefits
The relationship between trauma and ADHD is undeniably bidirectionaltrauma can worsen ADHD, and ADHD can increase exposure to trauma. Understanding this interplay empowers you to pursue a nuanced, individualized approach rather than a onesizefitsall solution.
By combining traumainformed therapy, ADHDtargeted interventions, and everyday selfcare, you can reclaim focus, stability, and a sense of agency over your life.
Conclusion
In summary, yestrauma can make ADHD worse, but the good news is that an integrated, traumaaware treatment plan can bring meaningful relief. If you recognize any of the patterns discussed here, consider reaching out to a qualified professional for a thorough evaluation. You deserve support that addresses both the mind's firedrill response to trauma and the attention challenges of ADHD.
We'd love to hear from you: Have you noticed your ADHD symptoms shifting after a stressful event? Share your story in the comments, or ask any questions you havelet's keep the conversation going and support each other on the path to healing.
FAQs
Can trauma make ADHD symptoms worse?
Trauma can make ADHD symptoms worse by increasing distractibility, impulsivity, and emotional dysregulation.
Does childhood trauma cause ADHD?
Childhood trauma doesn’t always cause ADHD, but it can increase the risk and severity of ADHD symptoms.
How does trauma affect ADHD in adults?
Trauma can worsen ADHD in adults by amplifying inattention, mood swings, and difficulty with focus and impulse control.
Can trauma mimic ADHD symptoms?
Trauma can mimic ADHD symptoms, such as distractibility and impulsivity, making diagnosis more complex.
What treatments help when trauma makes ADHD worse?
Trauma-focused therapy, ADHD medication, and integrated care can help manage symptoms when trauma makes ADHD worse.







![[PDF] Neurobiology of ADHD – Quick, Reliable Summary](https://mnapi.io.vn/uploads/images/medicalhealthzone.com/2025/11/04/neurobiology-of-adhd-pdf.jpg)