Hey there! If a doctor has mentioned an alpha-1 antitrypsin test and youre wondering what the fuss is about, youve come to the right place. In a nutshell, this test measures the level of a protein that protects your lungs and liver. Knowing whether you have enough of it (or too much) can help steer treatment, lifestyle tweaks, or further testing.
Why should you care? Because a low or abnormal result can explain persistent coughs, earlyonset COPD, or weird liverenzyme spikes. And spotting it early gives you a chance to act before serious damage sets in. Lets break it all down togetherno medical jargon, just friendly facts.
Why Get Tested
Ever felt like youre the only one coughing on a clear day, or noticed liver labs that just wont normalize? Those are classic red flags that might tip a doctor toward ordering an alpha1 antitrypsin blood test. Heres when the test usually pops up:
- Unexplained chronic obstructive pulmonary disease (COPD) or emphysema, especially in people who never smoked.
- Persistent liver problems with no clear causethink abnormal ALT/AST that keep hovering high.
- Family history of AAT deficiency or related lung disease.
- Before starting certain medications (like hormone therapy) that can affect liver enzymes.
Guidelines from specialty societies suggest screening anyone with earlyonset COPD (before age 45) or unexplained liver disease. So, if any of that sounds familiar, youre definitely in the right spot.
How Test Is Done
Good news: the test is quick and painless. Most labs draw a regular venous blood sample, but some also accept a cheek swab if needles make you squirm. Either way, the specimen goes to a certified lab where they quantify the amount of alpha1 antitrypsin (AAT) protein.
Preparation tips:
- No fasting neededjust bring a photo ID and your insurance card.
- If youre on steroids or hormonal meds, let the lab know; they may note it on the report.
- Ask your doctor whether they want a genetic panel in addition to the protein level; the two together give a complete picture.
Turnaround time is usually 57 business days, though some urgent services can deliver results within 48 hours. Once you have the numbers, your physician will interpret them alongside your clinical story.
Reading Your Results
Now the moment of truthwhat do the numbers actually mean? Labs report AAT concentrations in either milligrams per deciliter (mg/dL) or grams per liter (g/L). The normal range can vary slightly between labs, but a typical alpha1 antitrypsin reference range g/l looks like this:
| Lab | Normal Range (g/L) | Low (Deficiency) Threshold |
|---|---|---|
| Mayo Clinic | 0.92.0 | <0.7 |
| Labcorp | 1.02.2 | <0.8 |
| ARUP | 0.952.15 | <0.75 |
If your result lands in the low zone, it suggests AAT deficiency, which can be categorized as mild, moderate, or severe based on how far below the threshold you are. Severe deficiency (<0.5g/L) is the one most strongly linked to early lung disease.
But what if the number is high? Elevated AAT can happen during acute infections (your liver is cranking out more protein to fight off bacteria), pregnancy, or when youre on estrogen therapy. Its also seen in certain cancers. In other words, a high result isnt a red flag by itselfcontext matters.
Another common question is how AAT levels intersect with liver enzymes. Studies show that patients with AAT deficiency often exhibit alpha1 antitrypsin elevated liver enzymes early on, before any visible liver disease appears. Thats why doctors may order the test when ALT/AST are inexplicably high.
Cost & Access
Money talklets be real. The alpha1 antitrypsin test price can range from $70 to $150 if youre paying outofpocket. Most major insurers cover it when its medically indicated (e.g., for COPD evaluation), but youll want to confirm any priorauthorization steps your plan requires.
Where can you get it?
- Primary care office (your doctor can order it and send the sample to a local lab).
- Specialty labs like Labcorp or Quest Diagnosticsoften faster turnaround.
- Online services that ship a fingerprick kit to your door (handy if you live far from a clinic).
Tip: Ask your provider to doublecheck whether the test is medical necessity. That phrasing usually smooths out insurance hiccups.
Benefits & Risks
Every test carries a balance of upside and downside. Heres a quick rundown so you can weigh them yourself.
Benefits
- Early detection: Spotting AAT deficiency before severe lung or liver damage develops.
- Targeted therapy: Some patients qualify for augmentation therapy (infusions of purified AAT) that can slow lung decline.
- Family screening: If youre deficient, relatives can be tested early, allowing preventive measures.
Risks/Limitations
- Falsenegatives: During a flareup or heavy inflammation, the protein level can temporarily rise, masking deficiency.
- Emotional impact: Receiving an abnormal result can be anxietyprovoking; its normal to need time to process.
- Interpretation complexity: A borderline result often requires genetic testing for a definitive answer.
When you sit down with your doctor, bring a list of questions like: What does my specific level mean for my lung health? and Should I consider genetic counseling? That way you stay in the drivers seat.
Next Steps After Receiving Your Results
Got your lab report in hand? Heres what to do next, depending on what the numbers say.
If Your Level Is Normal
Great news! A normal result usually means your AAT isnt the culprit behind your symptoms. Still, keep an eye on any lingering cough or liver irregularitiesother causes might be at play, and your doctor may order additional tests.
If Your Level Is Low (Deficiency)
- Specialist referral: A pulmonologist can assess lung function (spirometry) and discuss augmentation therapy if needed.
- Liver followup: A hepatologist will monitor liver enzymes and possibly schedule imaging to check for early fibrosis.
- Genetic counseling: Since AAT deficiency is inherited, your close relatives should consider testing.
- Lifestyle tweaks: Avoid smoking, limit alcohol, stay vaccinated (flu, pneumococcal) and maintain a healthy weight.
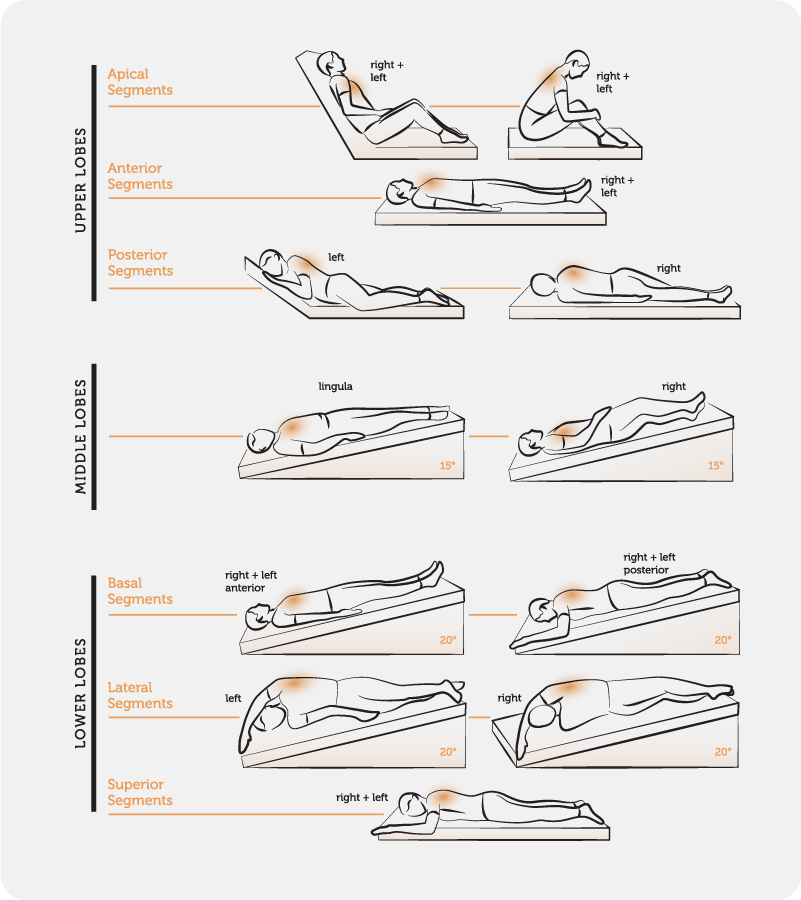
For people with underlying respiratory conditions, incorporating supportive therapieslike airway clearance and chest physiotherapycan help manage mucus buildup and reduce infections. If you or a family member are exploring options for airway clearance, resources on cystic fibrosis airway clearance explain common techniques and when to discuss them with your care team.
If Your Level Is Elevated
High AAT isnt usually dangerous, but it can signal an acute infection or hormonal influence. Your doctor may repeat the test after the infection clears or review any current medications (like estrogen patches).
Regardless of the result, keep a written copy of the report and note the reference range printed on itlabs can differ, and that reference is your best friend when discussing findings with another provider.
Conclusion
The alpha1 antitrypsin test is a straightforward, powerful tool that can explain puzzling lung or liver issues, guide treatment, and even alert family members to hidden risks. Understanding the normal range, the meaning of low or high readings, and the cost and accessibility of the test empowers you to have a productive conversation with your healthcare team. If youve been advised to get tested, dont hesitateask questions, note the results, and take the next steps that feel right for you. Your health journey is personal, and were rooting for you every step of the way.
FAQs
What does the alpha-1 antitrypsin test measure?
The test measures the concentration of the alpha‑1 antitrypsin (AAT) protein in your blood, which protects the lungs and liver from damage.
When should I ask for an alpha-1 antitrypsin test?
It’s recommended if you have early‑onset COPD/emphysema, unexplained liver enzyme elevations, a family history of AAT deficiency, or before starting certain hormone therapies.
What do low results indicate?
A low AAT level suggests a deficiency that can increase the risk of lung disease (like COPD) and liver problems; severity depends on how far the value falls below the normal range.
Can a high alpha-1 antitrypsin level be a problem?
High levels are usually temporary and occur during infections, pregnancy, or while on estrogen therapy. They are not typically harmful but should be interpreted in clinical context.
What are the next steps after an abnormal result?
Depending on the result, you may be referred to a pulmonologist or hepatologist, offered genetic counseling, and advised on lifestyle changes such as avoiding smoking and limiting alcohol.