Hey there! If you or someone you love lives with cystic fibrosis, you know that dealing with thick, sticky mucus can feel like trying to empty a clogged drain with a fork. The good news? There are proven airway clearance methods that make that fork a whole lot more effective. Below, Ill walk you through why airway clearance matters, the top techniques, how to pick the right device, and how to stitch everything into a doable daily routine. Grab a cup of tea, settle in, and lets make those lungs breathe a little easier together.
Why Clearance Matters
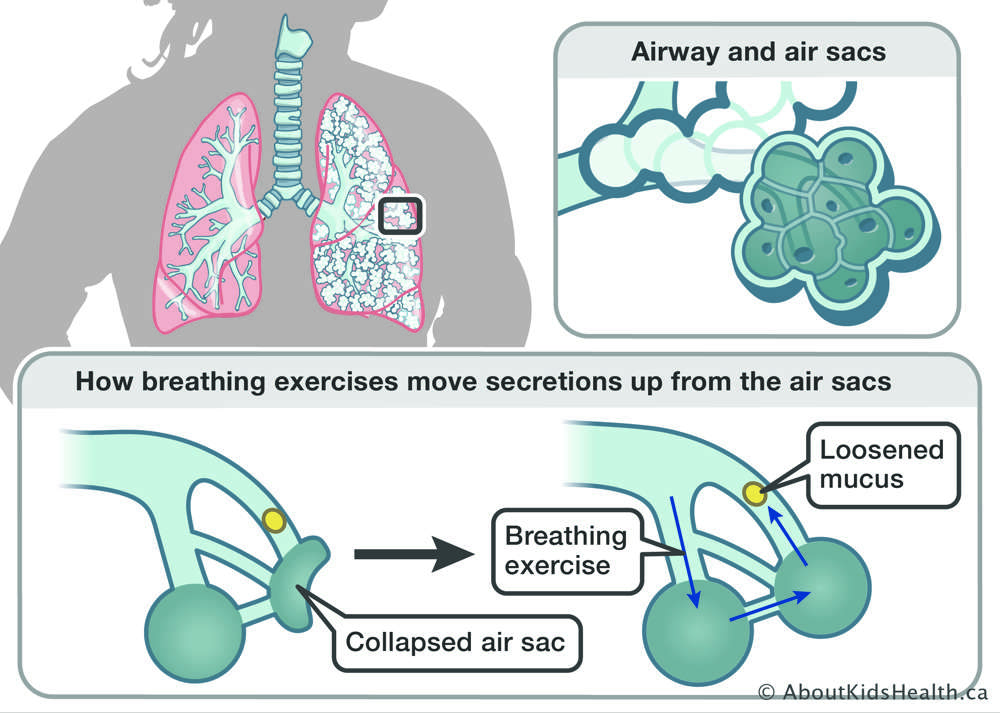
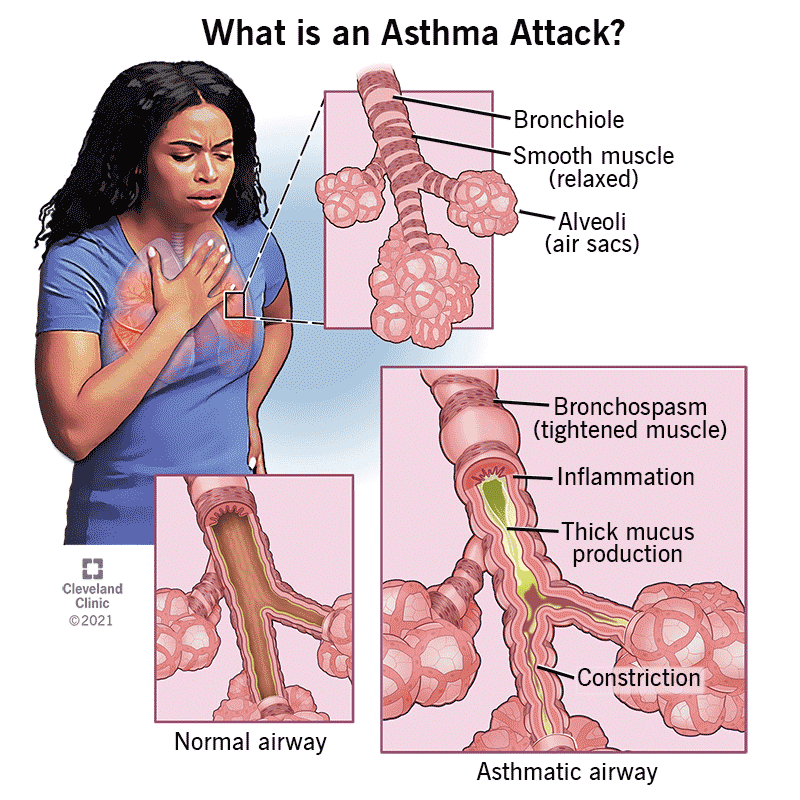
What problems does mucus cause in CF lungs?
In cystic fibrosis, the body produces mucus thats far thicker than normal. This gooey slab blocks the airways, traps bacteria, and fuels chronic infections. Over time, it can lead to bronchiectasispermanent airway widening that makes clearing even harder. A 2024 analysis from the Cystic Fibrosis Foundation (CFF) Registry showed that patients who consistently performed airway clearance had 30% fewer pulmonary exacerbations than those who didnt.
What are the proven benefits of regular ACTs?
Regular airway clearance techniques (ACTs) do more than just loosen mucus. Studies have demonstrated:
- Improved FEV (the measure of lung function) by up to 5% after three months of daily clearance .
- Reduced hospital stays by an average of 1.2 days per year.
- Better qualityoflife scores, especially for teenagers who feel less tied down by their treatment schedule.
What risks or misconceptions should I watch for?
Nothing is perfect, and airway clearance is no exception. Overaggressive percussion can irritate the airway lining, while skipping hydration may make mucus even thicker. And heres a common myth: One technique fits everyone. The truth is, each persons lungs, lifestyle, and preferences shape the best approach. Balancing benefits with potential downsides is keythink of it like tuning a guitar; you need the right tension for the right sound.
Core ACT Techniques
Which techniques are most recommended?
Heres the starter pack that most CF clinics suggest:
- Chest Percussion & Vibration: A rhythmic clapping or vibrating pad applied to the chest for 23minutes per session. Great for loosening the glue in the upper lobes.
- Active Cycle of Breathing Techniques (ACBT): A threestep dancebreathing control, thoracic expansion, then a forced expiration (or huff). Works like a gentle wind that pushes mucus toward the mouth.
- Positive Expiratory Pressure (PEP) Devices: Small handheld tools (like the 's recommended Aerobika) that create resistance as you breathe out, splitting the mucus apart.
How does the huffcough differ from a regular cough?
A regular cough is a quick, forceful expulsion that can cause airway collapse, especially in narrowed bronchi. The huffcough uses a slower, forced exhalation through an open mouththink of it as a controlled sigh that pushes mucus out without crushing the airway walls. Its less tiring and often more effective for thick secretions.
What role do airway clearance exercises play?
Exercise isnt just for heart health; moving your whole body can act like a natural vibration for the lungs. Simple treadmill walking, cycling, or even yoga twists increase the breathing rate and shear forces, helping mucus drift toward the larger airways. A 2024 PubMed study found that a 30minute aerobic session boosted clearance rates by 12% compared with rest.
Where can I find a printable airway clearance techniques PDF?
Most CF centers host a free PDF guide that lists stepbystep instructions, timing charts, and safety tips. The CFFs 2022 Airway Clearance Techniques fact sheet is a solid gotoyou can download it directly from their website and even print a handy checklist to stick on your fridge.
Choosing Devices
What are the main categories of devices?
Two families dominate the market:
| Category | Examples | How It Works | Best For |
|---|---|---|---|
| Oscillating PEP | Flutter, Aerobika, Acapella | Creates rapid pressure swings as you exhale, shaking mucus loose. | Home use, portable, good for kids and adults. |
| HighFrequency Chest Wall Oscillation (HFCWO) | Vest, SmartVest | Vibrating vest inflates/deflates at 515Hz, mimicking percussion. | Severe disease, nighttime use, those who cant do manual clapping. |
How do devices compare to manual techniques?
Below is a quick snapshot:
- Cost: Manual percussion is free; oscillating PEP devices range $30$150; HFCWO vests can exceed $4,000.
- Time: Manual methods need 1015minutes; most devices achieve similar results in 57minutes.
- Efficacy: Studies show oscillating PEP improves mucus clearance by ~20% over manual techniques alone.
- User Satisfaction: A 2023 survey reported 78% of adults preferred a handheld device because it felt less messy.
Which device suits children vs. adults?
Kids often enjoy the handheld flutter devices because theyre lightweight and gamelike. For adults, especially those with limited hand strength, a vest can be a lifesaverjust hop onto the couch, strap it on, and let the machine do the work while you bingewatch your favorite show.
Are there options for other conditions?
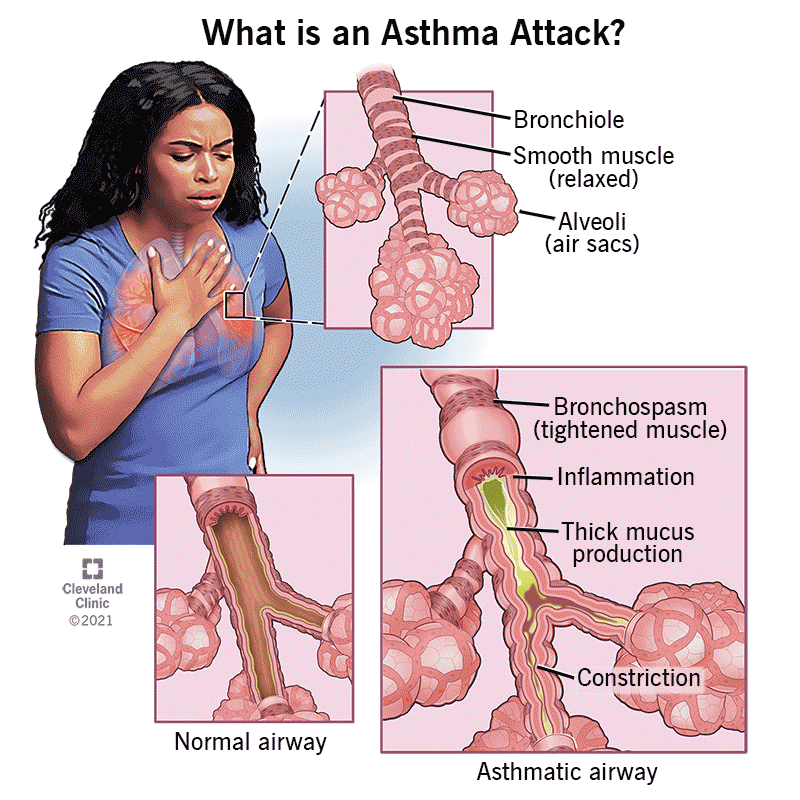
Yes! The same ACTs help people with bronchiectasis, COPD, and even pneumonia. While the underlying disease differs, the goalclearing mucusremains the same. For COPD, lowpressure PEP is usually recommended; for pneumonia, clinicians often pair ACTs with antibiotics and chest physiotherapy.
Daily Routine Guide
How often should ACTs be performed?
Most experts suggest 23 sessions per day, especially on days when you notice more sputum. If youre on a busy schedule, aim for a short morning session (right after inhaled meds) and an evening winddown. Consistency beats intensitythink drinking water daily rather than guzzling a bottle once a week.
Whats the ideal order of techniques?
Heres a flowchart that many patients find helpful:
- Warmup Breathing (2min): gentle diaphragmatic breaths to loosen the airway muscles.
- PEP Device (35min): creates the pressure swing that starts breaking up the mucus.
- Percussion/Vibration (2min): manual or vestbased, to shake the loosened secretions toward the larger airways.
- HuffCough (23min): clear the mucus thats now ready to exit.
- Hydration (throughout): sip water or a saline solution to keep the mucus thin.
Sample 10minute routine
Timestamped for a quick morning:
- 02min: Diaphragmatic breathing (inhale through the nose, exhale slowly).
- 25min: Use your Aerobika PEP device5cmHO resistance, steady exhalations.
- 57min: Light chest percussion (use a soft rubber cup or a handheld vibrator).
- 79min: Perform three huffcough cycles, focusing on the upper lobes.
- 910min: Drink a glass of water and take a few deep breaths to finish.
How to track progress?
Keep a simple log:
- Date/Time
- Technique(s) used
- Sputum volume (ml) a rough estimate works
- Effort rating (15)
- Any changes in FEV (if you have a home spirometer)
This ACT Tracker can be printed from the CFF PDF and slid into a pocket notebook. Seeing trends over weeks helps you and your care team adjust the plan.
What if I miss a session?
Dont panic. Skipping one session isnt catastrophic, but try to doubleup on the next day only if you feel comfortable. Overdoing it (like a marathon session) can lead to fatigue and, paradoxically, more mucus retention.
Managing Challenges & Safety
Feeling dizzy or lightheaded?
First, pause. Sip water, sit upright, and resume only after you feel steady. Dizziness can stem from low oxygen levels or dehydrationboth easily fixed with a quick break.
How to avoid injury from percussion?
Use a soft, handheld cup and keep the pressure moderatethink gentle tapping rather than drumming. Aim for 23minutes per side; longer sessions dont equal better results and can irritate the skin.
Equipment malfunction?
If a PEP valve feels clogged, disassemble it (most devices have a simple twistoff design), rinse with warm water, and let it airdry. Replace the valve every 612 months according to manufacturer guidelines.
Does clearance increase infection risk?
Actually, proper airway clearance reduces the bacterial load, lowering infection risk. A 2024 review in Respiratory Care highlighted that patients adhering to ACTs had 25% fewer positive cultures for Pseudomonas aeruginosa.
When should I call my doctor?
Watch for red flags: persistent fever, suddenly purulent sputum, sharp chest pain, or a drop in oxygen saturation below 92% (if you use a pulse oximeter). In those cases, reach out to your CF team right away.
Resources & Further Reading
Here are a few trusted places to deepen your knowledge:
- Johns Hopkins CF AirwayClearance Program (detailed videos and guides)
- Downloadable PDFs:
- 2022 CFF Airway Clearance Techniques fact sheet
- UK Cystic Fibrosis Trust physiotherapy guide (2020)
- Video demonstrations on the CFF YouTube channel perfect for visual learners.
Conclusion
Consistent, personalized airway clearance is the cornerstone of keeping lungs healthy in cystic fibrosis. Whether you favor a handheld PEP device, a highfrequency vest, or just a good oldfashioned clap on the back, the goal is the same: move that stubborn mucus out before it becomes a problem. Remember to balance the benefits with safety, stay hydrated, and track your progressyour future self will thank you.
Got a technique that works wonders for you? Or a question thats been bugging you? Drop a comment, share your story, or reach out to your CF care team. Were all in this together, and every little tip helps the whole community breathe a little easier.
FAQs
How often should I perform airway clearance for cystic fibrosis?
Most clinicians recommend 2‑3 sessions per day, ideally after inhaled medications in the morning and before bedtime.
What’s the difference between a huff‑cough and a regular cough?
A huff‑cough uses a forced, open‑mouth exhalation that pushes mucus out without collapsing the smaller airways, making it gentler and more effective for thick secretions.
Which device is best for a teenager with cystic fibrosis?
Hand‑held oscillating PEP devices like the Flutter® or Aerobika® are usually preferred because they’re portable, easy to use, and can be gamified for motivation.
Can I combine exercise with my airway clearance routine?
Yes—light aerobic activity such as walking or cycling increases shear forces in the lungs and can boost mucus clearance by about 10‑12% when done after a PEP session.
What should I do if I feel dizzy during a clearance session?
Stop the session, sit upright, hydrate, and take a few slow breaths. If dizziness persists or is accompanied by shortness of breath, contact your CF care team.