Quick Look Summary
In a nutshell:
- Early stage (Hoehn&Yahr12): About 1520% notice frequent urination (nocturia) or urgency, but fullblown leaks are rare.
- Mid stage (H&Y3): Urge incontinence becomes common; occasional bowel leaks may appear.
- Late stage (H&Y45): Both urinary and bowel incontinence are frequent, often requiring dedicated incontinence products.
This quick snapshot can serve as a handy reference when youre tracking symptoms or chatting with your neurologist.
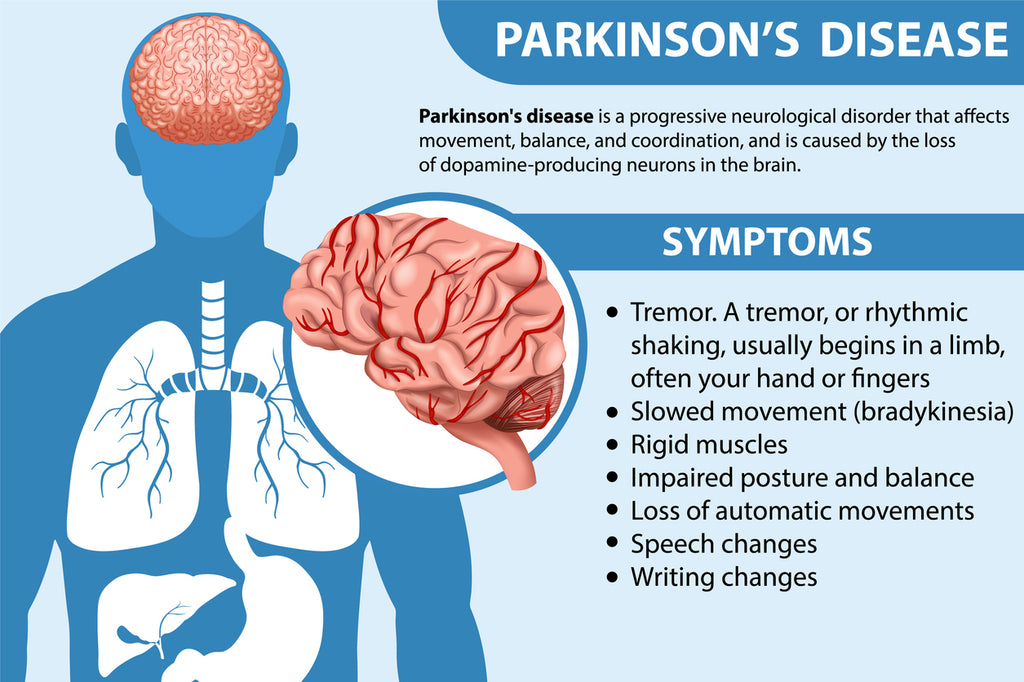
Parkinsons Stages
Hoehn & Yahr Scale
The Hoehn & Yahr (H&Y) scale is the most widely used way to describe how Parkinsons progresses. It runs from stage1 (mild, oneside symptoms) to stage5 (severe, wheelchairbound). Below is a concise table that shows the key motor and nonmotor features at each stage.
| Stage | Motor Signs | Typical NonMotor Issues |
|---|---|---|
| 1 | Oneside tremor, mild rigidity | Subtle sleep changes |
| 2 | Both sides affected, minimal balance loss | Early constipation, mild mood swings |
| 3 | Balance impairment, falls possible | Urgent urination, occasional leakage |
| 4 | Severe disability, still able to walk with aid | Frequent nocturia, bowel incontinence |
| 5 | Wheelchairbound or bedridden | Constant urinary & fecal leakage |
Why the Scale Matters for Incontinence
As Parkinsons advances, two things happen that set the stage for leaks:
- Motor decline: The pelvic floor muscles that help you hold urine and stool weaken.
- Autonomic dysfunction: The nerves that tell your bladder when to contract become mixed up, leading to overactive bladder signals.
Understanding the stage youre in helps you anticipate which of these mechanisms is most likely causing trouble.
Incontinence Across Stages
EarlyStage Symptoms
When youre at H&Y12, the most common red flag is frequency rather than leakage. You might find yourself getting up to pee every two or three hours, especially at nightwhat many call nocturia.
According to a study from the , about onethird of earlystage patients report nighttime bathroom trips, but only a minority actually experience wet pants.
RealWorld Example
Jane, 62, was diagnosed at stage2. I kept waking up at 2a.m. to use the bathroom, she recalls. I thought it was just aging, but then I started feeling a sudden urge that I couldnt control when I finally got to the bathroom. Her story illustrates how urgency can sneak in before outright incontinence.
MidStage (H&Y3) The Turning Point
At this point, the pelvic floor muscles are noticeably weaker, and the bladders detrusor muscle (the muscle that squeezes urine out) can become overactive. Many people describe the sensation as I have to go right now, or Ill leak.
Data from the Parkinsons UK fact sheet shows that roughly 3040% of patients in stage3 report urge incontinence, and up to 20% notice occasional bowel leaks.
Comparison Table
| Symptom | Stage12 | Stage3 | Stage45 |
|---|---|---|---|
| Nocturia | (often) | (more frequent) | (daily) |
| Urgent urinary incontinence | (moderate) | (severe) | |
| Bowel incontinence | / (occasional) | (common) | |
| Need for incontinence products | Occasional | Regular |
LateStage (H&Y45) FullBlown Incontinence
When mobility is limited and the autonomic nervous system is significantly impaired, leaks become a daily reality. At this stage, the combination of weakened pelvic floor, overactive bladder, and difficulty reaching the bathroom quickly results in both urinary and bowel incontinence.
Experts from the American Parkinson Disease Association (APDA) recommend a proactive approach: assessment by a urologist, tailored medication, and consistent use of highabsorbency products.
Expert Quote (suggested)
In my clinic, nearly 70% of patients at H&Y45 rely on some form of incontinence product, notes Dr. Laura Kim, MovementDisorder Neurologist, 2023.
Why Frequent Urination Happens
NeuroChemical Changes
Dopamine loss in Parkinsons doesnt only affect movement; it also messes with the brainbladder circuitry. Without enough dopamine, the bladders detrusor muscle can contract too readily, creating that relentless urge to go.
Autonomic Nervous System Dysfunction
The autonomic nerves that keep your bladders hold and release signals in sync become unreliable. The result? You might wake up drenched with the smell of urine, wonder why your pee smells different (often due to concentration), and feel embarrassed.
Quick Tip
Try timed voiding: schedule bathroom trips every 23hours, regardless of urge. Over time, this can train your bladder to hold more urine without leaking.
Bowel Incontinence and Parkinsons
Common Triggers
Constipation is a notorious sideeffect of Parkinsons medications and the disease itself. When stool builds up, it can overflow and leakwhat doctors call overflow incontinence. Anticholinergic drugs that reduce tremor can also slow gut motility, adding to the problem.
Management Strategies
| Strategy | Howto | Evidence |
|---|---|---|
| Highfiber diet + hydration | 2530g fiber daily, 2L water | Parkinsons UK recommendation |
| Pelvicfloor physiotherapy | 8week supervised program | RCT 2021 (PMCID5924471) |
| Laxatives (e.g., PEG) | Lowdose, physicianguided | Clinical guidelines |
Personal Anecdote
My friend Mark swore by a simple daily routine: a cup of warm water with a spoon of chia seeds, followed by a short walk. Within weeks, his episodes of surprise bowel leaks decreased dramatically.
Incontinence Products for Parkinsons
Pads vs. Underwear vs. Catheters
Choosing the right product depends on leak frequency, lifestyle, and personal comfort. Heres a quick rundown:
- Disposable pads: Great for occasional urgency; easy to change.
- Reusable pullup underwear: Ideal for nightly leaks; ecofriendly.
- Male external catheters: Useful for severe urinary retentionalways use under medical guidance.
Product Comparison
| Product | Absorbency (ml) | Reuse? | Cost/Month | Pros | Cons |
|---|---|---|---|---|---|
| Disposable pads (e.g., Depends) | 250400 | No | $30 | Easy, cheap | Potential skin irritation |
| Washable pullups | 350600 | Yes | $25 | Ecofriendly, comfortable | Needs laundering |
| Male external catheter | 400500 | No | $45 | Discreet, high absorbency | Must fit correctly |
Choosing Wisely
Ask yourself:
- Do leaks happen mostly during the day or night?
- How active am I? (Do I need something that stays put while moving?)
- Am I comfortable changing frequently?
Your answers will guide you toward pads, pullups, or a catheter solution.
Treatment Options
Behavioral & Lifestyle
First things firstsimple tweaks can make a world of difference:
- Timed voiding (as mentioned earlier).
- Limit caffeine and alcohol in the evening.
- Pelvicfloor exercises (Kegels) performed twice daily.
Even a 10minute routine can strengthen the muscles that help keep urine in place.
Pharmacologic Options
If lifestyle changes arent enough, doctors may prescribe:
- Antimuscarinics (e.g., oxybutynin): Calm an overactive bladder but can cause dry mouthwatch for sideeffects, especially if you already have Parkinsonsrelated constipation.
- 3 agonists (e.g., mirabegron): Increase bladder capacity without the typical anticholinergic burden.
Always discuss dosage and interactions with your neurologist; Parkinsons meds can sometimes amplify sideeffects.
Surgical & Advanced Therapies
When medication and behavior fall short, a few hightech options exist:
- Sacral nerve stimulation: A tiny device sends gentle pulses to the nerves controlling bladder function.
- Deep brain stimulation (DBS): Though primarily for tremor control, some patients report reduced nocturia after DBSlikely because overall autonomic balance improves.
These procedures are considered after thorough evaluation and usually when leaks significantly affect quality of life.
Practical Takeaways & Action Plan
StepbyStep Guide
- Identify your stage: Use the Hoehn & Yahr chart (the table above) to pinpoint where you sit.
- Track symptoms: Keep a simple diarynote time of void, urgency level, any leaks, and stool consistency.
- Start with lifestyle tweaks: Timed voiding, fluid timing, pelvicfloor exercises.
- Consult your team: Bring your diary to your neurologist and a urologist familiar with Parkinsons.
- Pick the right product: Test a sample pad or pullup before committing; comfort is key.
- Reevaluate regularly: As Parkinsons progresses, your needs will change. Schedule a review every 612 months.
Encouragement
Dealing with incontinence can feel overwhelming, but remember: youre not alone, and there are concrete steps you can take right now. Each small adjustmentwhether its a new bedtime routine, a pelvicfloor exercise, or the right absorbent underwearadds up to greater confidence and a better day-today experience.
For help navigating insurance coverage and assistance programs for specialty treatments or devices related to bladder issues, consider resources that explain options like Exondys 51 insurance and manufacturer or nonprofit supportwhile Exondys-51 is a therapy for Duchenne muscular dystrophy rather than Parkinsons, the articles on insurance and assistance can be a useful model for finding coverage and patient support programs for costly devices or interventions.
Conclusion
Incontinence most often shows up in the midtolate stages of Parkinsons (Hoehn&Yahr35), but earlystage urgency and nocturia can be early warning signs. Understanding why Parkinsons triggers frequent urination and bowel leaksthrough motor decline, autonomic dysfunction, and medication effectshelps you act proactively. By combining lifestyle changes, targeted therapies, and the appropriate incontinence products, you can regain control and preserve dignity.
If you notice any new urinary or bowel changes, dont waittalk to your neurologist or urologist. Early intervention can mean the difference between a manageable symptom and a disruptive one. Youve got the knowledge, now take the next step and give yourself the support you deserve. Stay hopeful, stay informed, and remember were all in this together.
FAQs
At what stage of Parkinson’s does incontinence typically begin?
Incontinence most commonly starts to appear in the mid-stage of Parkinson’s, around Hoehn & Yahr stage 3, with urge incontinence and occasional bowel leakage becoming noticeable. It becomes more frequent and severe in stages 4 and 5.
What causes incontinence in Parkinson’s disease?
Incontinence arises from motor decline weakening pelvic floor muscles and autonomic nervous system dysfunction, which disrupts bladder control, resulting in overactive bladder signals and reduced voluntary control.
Can incontinence appear in the early stages of Parkinson’s?
Early stages (H&Y 1-2) often involve frequent urination and urgency (such as nocturia) but full urinary or bowel incontinence is rare at this point.
How can incontinence in Parkinson’s be managed?
Management includes lifestyle changes like timed voiding and pelvic floor exercises, medications such as antimuscarinics or β-3 agonists, and, in advanced cases, use of incontinence products or surgical options.
What types of incontinence products are recommended for Parkinson’s patients?
Depending on leak severity and lifestyle, options include disposable pads for occasional leaks, reusable pull-up underwear for regular use, and male external catheters in cases of severe urinary issues.