Migraines arent just a bad headache theyre a complex mix of genetics, hormones, nerves, and everyday habits that can feel like an unpredictable storm inside your skull. In the next few minutes, lets unpack whats really happening behind those thumping pains, why they show up differently for men and women, and what you can do right now to start taking control.
Quick Overview Snapshot
At their core, migraines arise when the brains painprocessing pathways get woken up by a cascade of chemical and vascular changes. Think of it like a faulty fire alarm that goes off even when theres no fire a tiny trigger can set off a fullblown response.
Three big buckets drive this cascade:
- Genetic predisposition: If your parents or siblings migraine, chances are youve inherited a sensitivity.
- Neurovascular dysfunction: The brainstem and the trigeminal nerve start shouting, releasing chemicals like CGRP that dilate blood vessels.
- Triggermediated cascades: Hormones, foods, stress, sleep patterns, and even the weather can tip the balance.
Understanding which bucket (or combination) is most active for you is the first step toward lasting relief.
Gender Specific Causes
Ever notice that your partners migraines seem to follow a different rhythm than yours? Thats not a coincidence men and women often have distinct underlying triggers.
What causes migraines in females?
For many women, the hormonal rollercoaster of the menstrual cycle is the main driver. Estrogen drops around day13 of your period can set off what doctors call menstrual migraine. Oral contraceptives, pregnancy, and menopause can also shuffle hormone levels enough to spark attacks.
Beyond hormones, women are slightly more likely to experience migraine with aura, a visual or sensory warning that can precede the pain.
Hormonerelated trigger checklist
| Hormone Shift | Typical Pattern | Quick Management Tip |
|---|---|---|
| Estrogen drop (period) | Day13 of cycle | Track cycle, consider magnesium or lowdose estrogen therapy |
| Progesterone rise (midluteal) | Latecycle headache | Sleep hygiene + stressreduction techniques |
| Pregnancy hormone surge | Second trimester spikes | Consult OBGYN for safe acute relief options |
Realworld example: Anna, 28, noticed that every month her migraines hit the same day. By logging her cycle and adding a daily magnesium supplement, her attacks dropped from four to one per month. Small changes, big impact.
What causes migraines in males
Men dont have the same hormonal swings, so lifestyle factors tend to dominate. Alcohol, especially red wine, caffeine overuse, and tobacco can all prime the trigeminal nerve. Stress and irregular sleep are also heavy hitters.
Research from the shows that men with chronic migraines often report higher rates of sleep apnea and high blood pressure both of which can aggravate vascular instability.
Malefocused quick tips
- Limit alcohol to 2 drinks a day.
- Keep caffeine under 200mg (about one strong coffee).
- Aim for 79hours of consistent sleep.
- Incorporate a daily 10minute walk to lower stress.
Core Biological Roots
Lets dive a little deeper into the bodys internal wiring.
Mitochondrial dysfunction & oxidative stress
Think of mitochondria as tiny power plants in each cell. When theyre sluggish, brain cells cant meet their energy demands, making the nervous system hyperexcitable. Studies suggest that supplements like CoQ10, riboflavin (vitaminB2), and magnesium can boost mitochondrial efficiency and cut migraine frequency for many people.
Key research snapshot
A 2022 peerreviewed trial found that daily riboflavin (400mg) reduced migraine days by 30% over three months compared to placebo. The authors highlighted the low sideeffect profile, making it a solid firstline preventive option.
Neuroinflammation & the trigeminal nerve
The trigeminal nerve is the main pain messenger for head pain. When it gets activated, it releases calcitonin generelated peptide (CGRP), a molecule that swells blood vessels and fuels inflammation. Thats why the newest class of migraine drugsCGRP antagonistsare making waves.
How CGRP meds work
These drugs bind to the CGRP receptor, preventing the peptide from tying the knot, thus stopping the vascular dilation that drives throbbing pain. Theyre not a cureall, but for many with chronic migraine, they offer a lifeline.
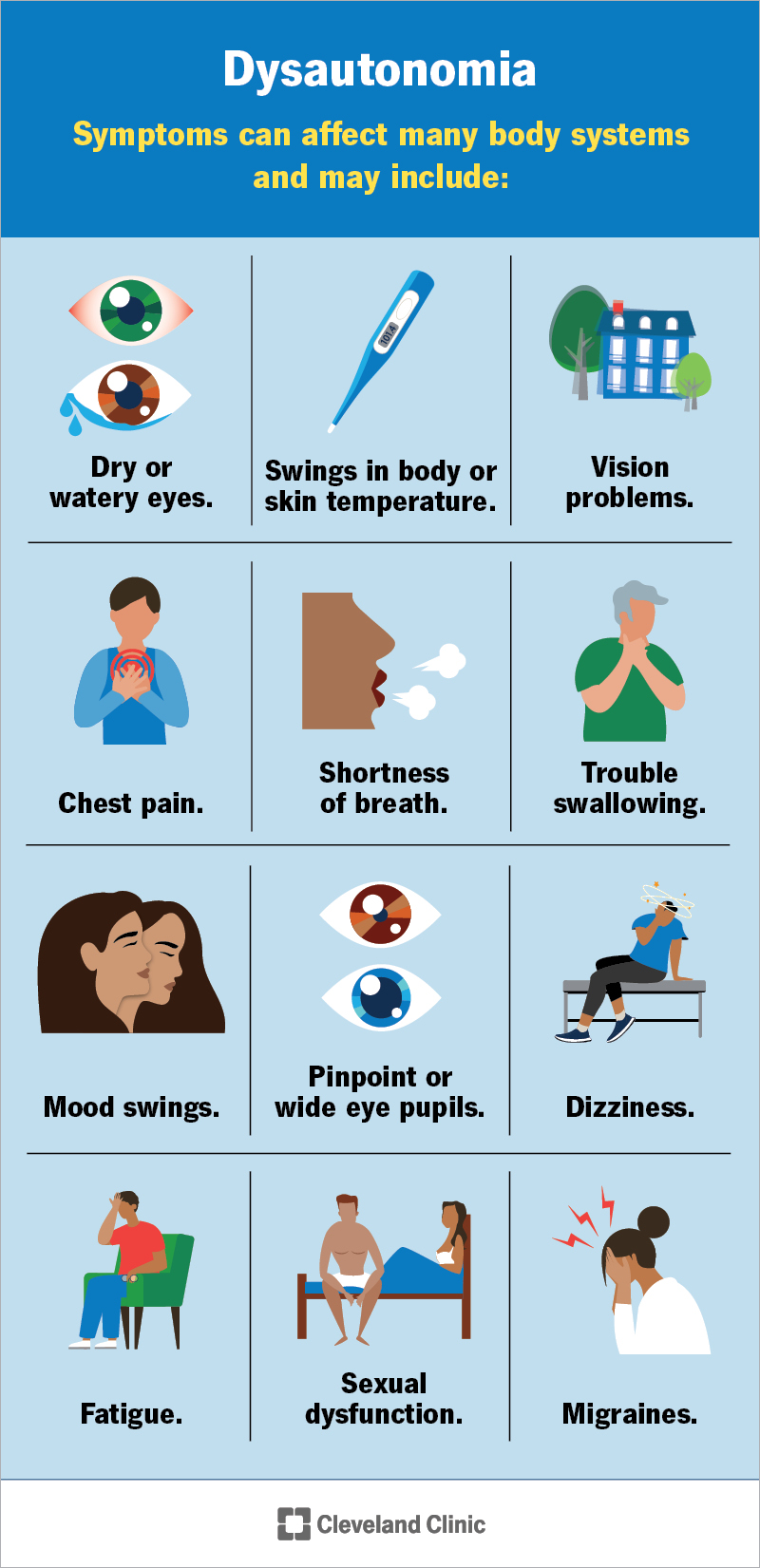
Medical conditions that amplify migraines
Sometimes, migraines are the bodys alarm bell for something else:
- Depression & anxiety: Mood disorders share neurotransmitter pathways with migraine pathways.
- Thyroid disorders: Hypo or hyperthyroidism can destabilize hormone balance.
- Polycystic ovary syndrome (PCOS): Hormonal chaos can trigger frequent attacks.
- Sleep apnea: Low oxygen at night spikes vascular reactivity.
If you have any of these, a conversation with a neurologist or your primary doctor can clarify whether treating the underlying condition eases your migraine load.
Everyday Lifestyle Triggers
Even if your genetics are set, everyday habits can either fan the flames or douse them.
Common dietary culprits
Items like aged cheese, MSG, artificial sweeteners, and nitrates (found in processed meats) can trigger attacks in sensitive people. Its not that theyre bad for everyonejust that they can act as a key for a migraine lock you already carry.
7day foodlog template
Print a simple table, jot down everything you eat and drink, and mark any headache that follows. Patterns often appear after a week or two.
Stress and the cortisol cascade
Stress isnt just a feeling; it releases cortisol, which can heighten the brains pain pathways. Chronic stress may keep the trigeminal nerve on high alert.
Stressrelief toolkit
- 5minute breathing exercise (inhale 4sec, hold 4sec, exhale 4sec).
- Evening walk without screens.
- Journaling one thing youre grateful for each day.
Sleep patterns & circadian rhythm
Both too little and too much sleep can provoke migraines. Aim for a regular bedtime, dim the lights an hour before, and keep the bedroom cool.
3step bedtime routine
- Turn off screens at least 60minutes prior.
- Spend 5minutes stretching or gentle yoga.
- Use a whitenoise or naturesound app to lull the brain.
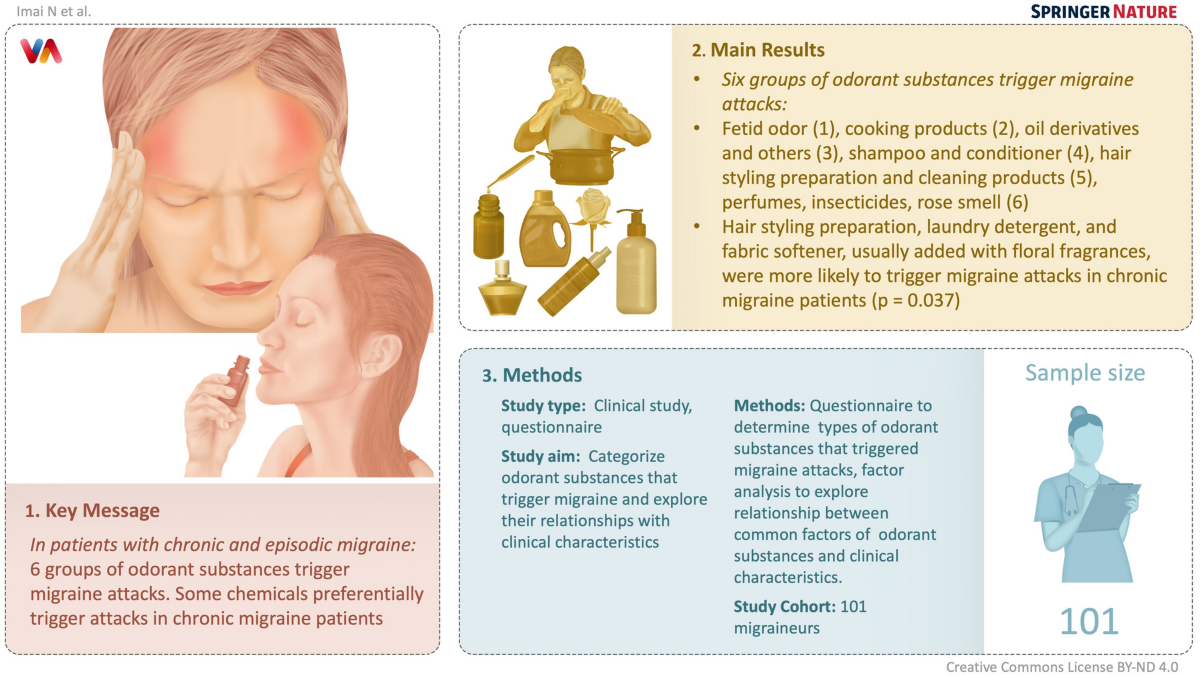
Environmental sensitivities
Bright fluorescent lights, strong perfumes, and sudden weather changes can act as sensory overload. Bluelight glasses and air purifiers arent just for office workersthey can reduce the probability of an attack during a hectic day.
Danger Assessment Overview
Most migraines are not lifethreatening, but certain types merit extra caution.
When a migraine signals danger
- Migraine with aura: Increases the risk of ischemic stroke, especially in smokers or those on estrogen therapy.
- Sudden, thunderclap headache: Could indicate a brain bleed; seek emergency care.
- Medicationoveruse headache: Using pain relievers more than 10days a month can paradoxically cause more headaches.
Redflag symptoms
If you notice any of these, call emergency services:
- New weakness or numbness on one side.
- Sudden vision loss.
- Confusion or difficulty speaking.
- Severe headache after a head injury.
Longterm consequences of ignoring causes
Untreated underlying factors can transform episodic migraines (<10days/month) into chronic migraine (15days/month). Chronic migraine is linked with higher rates of depression, anxiety, and reduced work productivity.
Stat snapshot
According to the , about onethird of chronic migraine sufferers also meet criteria for major depressive disorder, creating a vicious cycle.
Personalized Action Plan
Now that weve explored the science, lets turn insight into action. Below is a stepbystep RootCause Discovery worksheet you can fill out at home.
Stepbystep worksheet
- Familyhistory audit: Do any firstdegree relatives have migraines? Mark yes or no.
- Hormone & menstrual diary (if applicable): Note cycle days, any aura, and headache intensity.
- Lifestyle log (7days): Record foods, caffeine/alcohol, sleep hours, and stress levels.
- Medical review checklist: List current meds, known conditions (e.g., thyroid, hypertension), and any recent changes.
After a twoweek trial, compare the patterns you see. Which factor appears most frequently before an attack? Thats your prime target.
When to seek professional help
Consider scheduling an appointment if:
- You experience migraine on 4days/month.
- Overthecounter remedies provide little relief.
- You notice any redflag symptoms listed above.
- Stress, sleep, or diet changes havent shifted the pattern after a month.
A headache specialist can order imaging, discuss preventive medications, or explore newer options like CGRP inhibitors or neuromodulation devices.
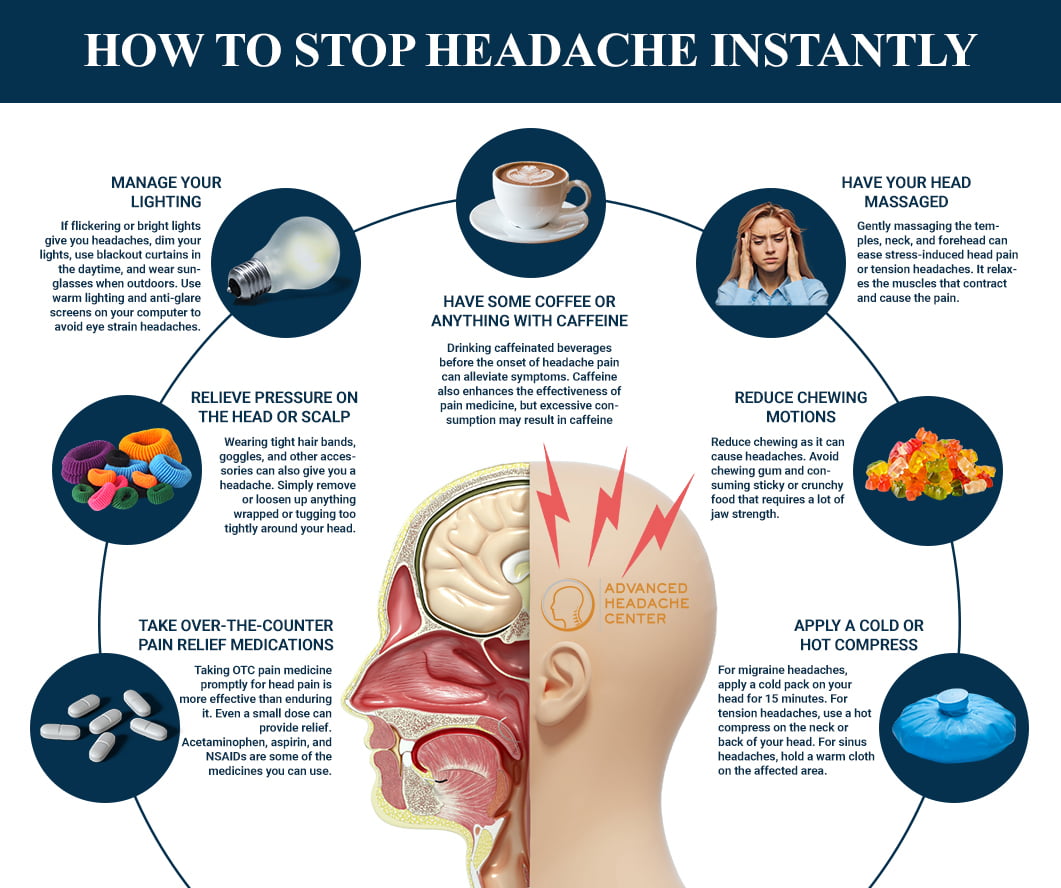
5 tips for instant migraine relief
- Cold compress: Apply a cold pack to the forehead for 15minutes.
- Dark, quiet room: Light and sound amplify pain signals.
- Hydration: Sip water slowly; dehydration is a common trigger.
- Magnesium supplement: 200400mg can calm neuronal excitability.
- Gentle neck stretch: Tilt your head sidetoside, holding each stretch for 10seconds.
These arent cures, but they often give enough respite to get through a flare without reaching for stronger meds.
Conclusion
Understanding the underlying causes of migraines is a gamechanger. By recognizing the trio of genetics, neurovascular quirks, and daytoday triggers, you move from reacting to headaches to proactively steering them away. Whether youre a woman navigating hormonal ups and downs or a man wrestling with caffeine and stress, theres a concrete, personalized plan you can start today.
Take the worksheet, try the instantrelief tips, and keep an eye on those redflag signals. If the headaches persist, dont hesitate to reach out to a specialist you deserve a life where migraines dont call the shots.