Heres the good news: you dont need a Ph.D. in neuroradiology to understand the essentials. In the next few minutes well walk through the most important MRI sequences, show you how to spot the redflag spots, decode the language that radiologists use, and let you know exactly when a call to your doctor is urgent. Think of this as a friendly cheatsheet you can keep beside your coffee mug.
MRI Basics Explained
What is a brain MRI and why is it used in stroke workup?
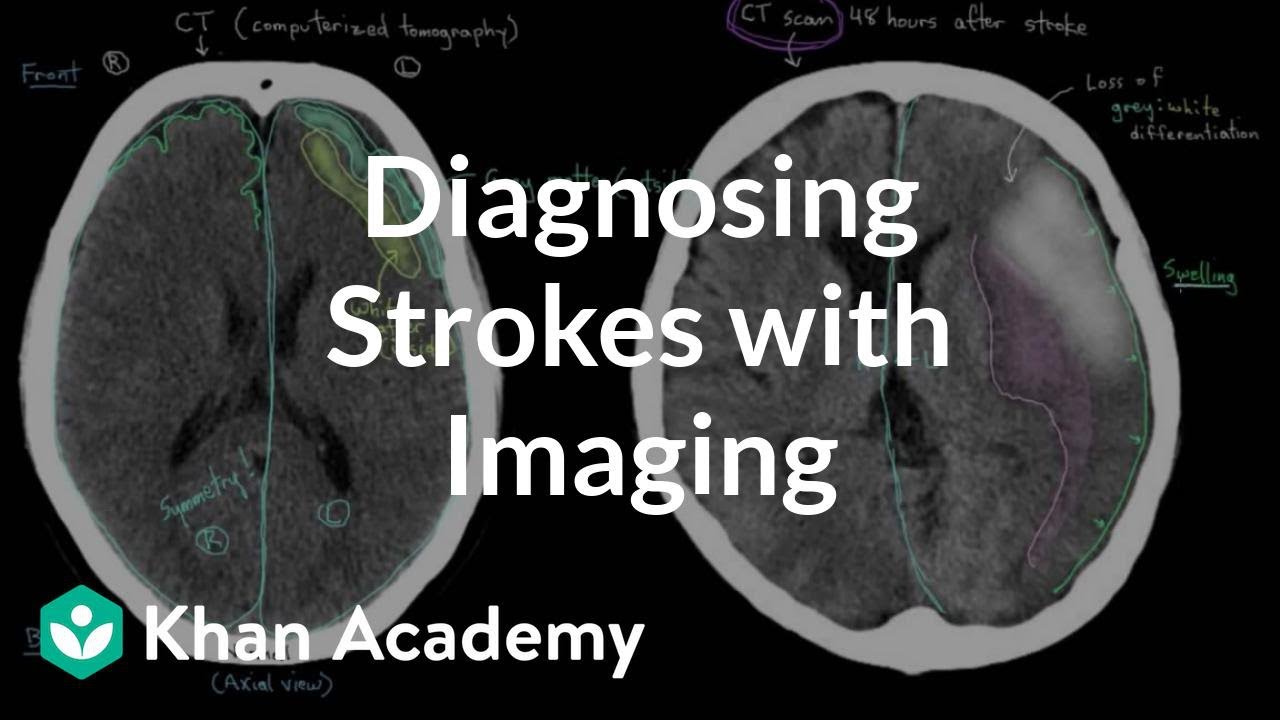
An MRI (Magnetic Resonance Imaging) uses powerful magnets and radio waves to create detailed pictures of the brain. For stroke, the trick is that certain sequences light up areas where blood isnt flowing properly. Unlike a CT scan, MRI can detect damage within minutes of symptom onset, giving doctors a chance to intervene early.
Which MRI sequences matter most for detecting stroke?
Think of each sequence as a different lens on the same scene. The three youll hear about most often are:
| Sequence | What it shows | Typical stroke sign |
|---|---|---|
| DWI (DiffusionWeighted Imaging) | Movement of water molecules | Bright spot = acute infarct (minuteshours) |
| ADC (Apparent Diffusion Coefficient) | Quantifies diffusion | Dark area confirms true restriction |
| FLAIR (FluidAttenuated Inversion Recovery) | Suppresses CSF, highlights edema | Hyperintensity appears after ~6h (subacute) |
| T2weighted | General tissue contrast | Shows swelling and chronic lesions |
| T1weighted | Anatomy, hemorrhage | Acute blood appears dark, subacute bright |
Radiologists often start with DWI/ADC to catch the freshoffthepress stroke, then use FLAIR and T2 to see how the damage is evolving.
Normal vs Abnormal
What does a normal brain MRI look like?
A normal scan is basically a wellorganized city map: the ventricles are dark on T1 and bright on T2, the white matter looks uniform, and theres no unexpected bright spot on DWI. If you can imagine a quiet lake at dawn, thats the baseline youre looking for.
How can you recognize common abnormalities?
When a stroke pops up, the MRI screams in color:
- Acute ischemia: DWI bright, ADC dark the classic brightdark combo.
- Hemorrhage: Early blood is dark on T2 but becomes bright on T1 as it ages.
- Chronic lesions: Older scars show as bright on T2 and slightly bright on T1, without diffusion restriction.
Seeing these patterns is a lot like learning to read traffic signs. Once you know the symbols, the road becomes much clearer.
Key Stroke Indicators
How does DWI/ADC confirm an acute stroke?
Within minutes of an arterial blockage, water molecules get trapped, causing a surge of signal on DWI while ADC drops. This restricted diffusion is the most reliable early marker. If you see that bright spot on DWI and a matching dark spot on ADC, youve likely found an acute infarct.
What does FLAIR hyperintensity tell us about timing?
FLAIR is a bit slower to react. It usually lights up around six hours after the event, marking the beginning of tissue swelling. So, a DWIpositive but FLAIRnegative scan often means the stroke is very recent (the golden hour for treatment).
When does a dark T2 signal suggest chronic damage?
Old infarcts lose their bright DWI signal and settle into a more muted T2 appearance. Over weeks to months they become slightly bright on T1 because of gliosis (scar tissue). If youre only seeing that gentle glow without any diffusion restriction, the injury is likely past the acute phase.
Minichecklist for the patient
Keep this quick reference handy when you open your PDF:
- Acute (024h): DWI, ADC brightdark combo.
- Early subacute (2472h): FLAIR, DWI may start to fade.
- Chronic (>1week): T2, T1 (gliosis), no diffusion restriction.
These three lines will help you answer the most common question: Is this happening right now, or is it old news?
Reading the Report
Where to find the Impression vs. Findings sections?
Radiology reports are usually split into two parts. Findings is the detailed walkthrough of each slice think of it as the map legend. Impression is the summary, the headline you want to focus on. Its the radiologists short answer to Whats going on?
How to decode phrases like acute infarct in the right MCA distribution?
Break it down piece by piece:
- Acute infarct: Fresh tissue death (usually <24h).
- Right MCA distribution: The blockage is in the right middle cerebral artery, which supplies the outer portion of the brains frontal, temporal, and parietal lobes.
If you ever see no diffusion restriction, thats actually good news it means theres no fresh ischemia right now, even if you might have older changes.
Sample report snippet (adapted from a brainMRIreportsample.pdf)
Findings:- DWI shows a focal area of high signal in the right insular cortex.- Corresponding low ADC values confirm diffusion restriction.Impression:- Acute ischemic infarct in the right middle cerebral artery territory.
Notice how the Impression repeats the key terms from the Findings but in a concise, actionoriented way. Thats the line youd tell your doctor about.
Useful resource: how to read MRI brain PDF
If you love a printable cheatsheet, a quick Google search for how to read MRI brain PDF will turn up several free guides. One of the most userfriendly is a downloadable PDF from a reputable university radiology department. Keep it bookmarked for future scans.
When to Worry
Which MRI findings need urgent followup?
Anything that says restricted diffusion (bright DWI, dark ADC) is a red flag. Thats an acute infarct, and you should call your neurologist or go to the emergency department right away. Time is brain.
How to interpret incidental whitematter changes?
These are common, especially in older adults or people with hypertension. They appear as fluffy bright spots on T2/FLAIR but usually have no diffusion restriction. While theyre not emergencies, they do signal that you should keep an eye on vascular risk factors think blood pressure, cholesterol, and lifestyle. If vascular risk management is a concern after an imaging finding, resources about headache assessment steps can sometimes be helpful in structuring symptom review and followup with your clinician.
When should you call your doctor versus waiting for a followup?
Use this simple decision tree (adapted from the stroke protocol):
- Diffusion restriction present? Call your neurologist now it could change treatment.
- Only FLAIR hyperintensity, no DWI change? Schedule a followup within 4872hours. Often the stroke is evolving but still not an emergency.
- Chronic lacunar infarcts, no new symptoms? Discuss longterm riskfactor management at your next routine visit.
In short: if the words acute or restricted diffusion appear, pick up the phone. If you only see old scar or whitematter change, a regular appointment will do.
Balancing Benefits and Risks
Understanding your MRI empowers you, but remember that interpretation is a partnership. Radiologists bring years of training; you bring the lived experience of symptoms and concerns. Together, you can decide on the right next steps, whether thats clotbusting therapy, rehab, or simply tighter bloodpressure control.
One of the best ways to stay informed is to ask your doctor to walk you through the images. A quick Can we look at the DWI together? can turn a scary PDF into a useful conversation.
Conclusion
Reading a brain MRI after a possible stroke doesnt have to feel like deciphering an alien language. Focus on three pillars: the sequence (DWI, ADC, FLAIR), the signal pattern (brightdark combos versus muted changes), and the radiologists impression. Spotting an acute infarct early can mean lifesaving treatment, while chronic findings guide longterm health decisions.
Use the quick checklists, sample report snippets, and decisiontree above as your personal guidebook. And whenever uncertainty creeps in, remember that a qualified neuroradiologist is just a call away you dont have to navigate this alone. Stay curious, stay proactive, and let your brains story be told in a way that helps you take the best next steps.
FAQs
What MRI sequences are most important for detecting a stroke?
The key MRI sequences to focus on are DWI (Diffusion Weighted Imaging), ADC (Apparent Diffusion Coefficient), and FLAIR (Fluid Attenuated Inversion Recovery). DWI shows acute infarcts as bright spots, ADC confirms diffusion restriction as dark spots, and FLAIR shows edema and tissue swelling appearing hours after stroke onset.
How does an acute stroke appear on MRI?
An acute ischemic stroke appears as a bright spot on DWI with a corresponding dark area on ADC, showing restricted diffusion. FLAIR may be negative very early on but becomes hyperintense after about 6 hours, indicating tissue swelling.
What is the difference between acute and chronic stroke on MRI?
Acute stroke shows diffusion restriction (bright DWI, dark ADC), while chronic stroke loses these diffusion changes and appears as hyperintense on T2-weighted images with slight brightness on T1 due to gliosis (scarring). Chronic lesions do not show diffusion restriction.
What should I look for in a radiology report on brain MRI for stroke?
Focus on the "Impression" section for a concise summary, which will highlight terms like "acute infarct" and specify the vascular location such as "right MCA distribution." The "Findings" detail the imaging observations such as high DWI signals or low ADC values confirming infarcts.
When should I seek urgent medical attention based on MRI stroke findings?
If the MRI shows restricted diffusion (bright on DWI and dark on ADC), this indicates an acute infarct and requires immediate contact with a neurologist or emergency care. Findings limited to FLAIR hyperintensity without diffusion restriction usually require follow-up rather than emergency care.