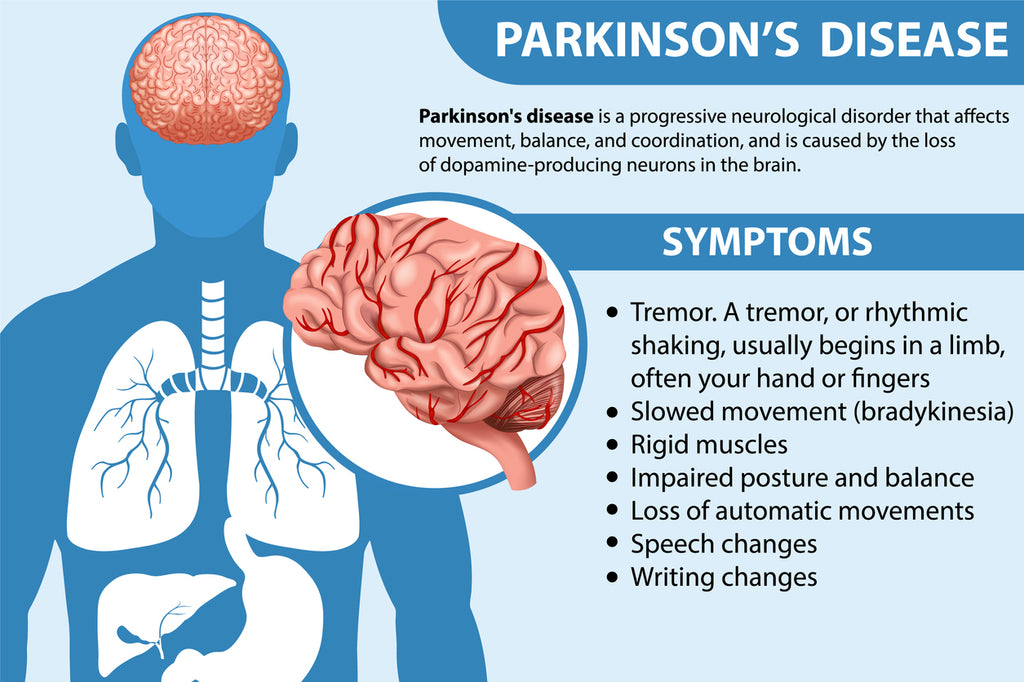
If you or a loved one lives with Parkinsons and suddenly feels foggy, shaky, or notices a strange smell in the bathroom, a urinarytract infection (UTI) could be the hidden culprit.
In the next few minutes well walk through how UTIs can worsen Parkinsons dementia, what subtle symptoms to watch for, and the best ways to treat and prevent themso you can keep the brain fog, falls, and extra doctor trips to a minimum.
Why UTIs Matter
What is a UTI?
A urinarytract infection is an invasion of bacteriaoften E.coliinto any part of the urinary system, from the urethra up to the kidneys. Most people feel a burning sensation when they pee, but thats just the tip of the iceberg.
How often do Parkinsons patients get UTIs?
Research from the Parkinsons Foundation shows that people with Parkinsons are up to three times more likely to develop a UTI than the general population. A 2023 review in found that nearly 40% of hospitalised Parkinsons patients experienced a urinary infection during their stay.
What makes Parkinsons patients vulnerable?
Three main factors create a perfect storm:
- Slowed bladder emptying due to autonomic dysfunction.
- Mobility limitations that make it harder to reach the bathroom in time.
- Cognitive decline that can lead to missed hygiene steps.
Link between UTIs and dementiatype symptoms
When bacteria release toxins, your bodys inflammatory response can cross the bloodbrain barrier, briefly ramping up neuroinflammation. That extra noise often shows up as sudden confusion, worsening memory loss, or even a temporary surge in tremor severity. In short, a UTI can act like a spotlight on the underlying Parkinsons dementia.
Spotting UTI Signs
Classic UTI clues
Firstline symptoms still apply: burning during urination, urgency, frequency, and cloudy or foulsmelling urine. The CDC notes that these signs are the most reliable early warnings for most adults.
UTI symptoms with Parkinsons
People with Parkinsons often experience a different pattern. Instead of intense pain, they might notice:
- Sudden mental fog or agitation.
- Newonset tremor spikes or stiffness.
- Unexpected falls or loss of balance.
- A noticeable parkinsons urine smell a stronger, sometimes ammonialike odor. For tips on managing related symptoms and support options, see Exondys 51 assistance which highlights patient support approaches that can be useful when managing complex medication and infection interactions.
Comparison Table
| Typical UTI | UTI in Parkinsons |
|---|---|
| Burning sensation | Often mild or absent |
| Frequent urge to urinate | May coexist with urgencyincontinence |
| Cloudy or bloody urine | Often accompanied by strong odor (parkinsons urine smell) and darker color |
| Fever and chills | Sometimes absent; confusion may be the first sign |
How long does confusion from a UTI take to go away?
Most patients see a noticeable improvement within 27days after starting appropriate antibiotics. However, older adults or those with advanced dementia may need up to two weeks for full mental clarity to return.
When should you call a doctor?
Red flags include a temperature above38C, sudden loss of consciousness, inability to walk, or severe agitation that doesnt settle. If any of these appear, seek medical help right away.
UTI Impact on Dementia
Why infections worsen cognitive decline
Inflammatory cytokines released during a UTI can temporarily increase amyloidbeta production, the same protein that piles up in Parkinsons dementia. This extra load can make memory lapses feel more intense and last longer than usual.
Effect on motor function
Even a mild infection can amplify rigidity and bradykinesia. You might notice your hands shaking a bit more, or your steps becoming shufflier than normal. These changes raise the risk of fallingsomething caregivers watch closely.
Can infection make Parkinsons worse?
Absolutely. While a UTI wont cause Parkinsons disease, it can accelerate its progression by stressing both the brain and the body. Thats why early detection and treatment are critical.
Longterm consequences if untreated
Repeated infections can lead to chronic inflammation, which researchers believe may hasten the shift from mild cognitive impairment to fullblown Parkinsons dementia. Moreover, chronic urinary retentiona common result of untreated infectionscan damage the bladder wall over time.
Getting Proper Diagnosis
Urine dipstick vs. culture
A dipstick test gives a quick glimpse (leukocyte esterase, nitrites) but can miss lowgrade infections. A urine culture is the gold standard, especially when symptoms are atypicalas they often are with Parkinsons.
When to ask for a bladder ultrasound?
If you suspect urinary retention (postvoid residual volume >200ml), an ultrasound can visualise how much urine remains after you empty your bladder. This is crucial for tailoring treatment.
Assessing Parkinsons urinary retention
Retention isnt rare; studies estimate that up to 30% of Parkinsons patients develop it. Treatment options range from intermittent catheterisation to medication like mirabegron, which relaxes the bladder without the anticholinergic side effects that can cloud cognition.
Screening for dementia during a UTI
Tools such as the MiniMental State Exam (MMSE) or Montreal Cognitive Assessment (MoCA) should be administered before and after the infection. A noticeable drop can signal that the UTI is directly affecting brain function.
Redflag labs
Elevated Creactive protein (CRP) and erythrocyte sedimentation rate (ESR) often accompany infections. Including these in the workup helps confirm that inflammation, not just a urinary symptom, is driving the cognitive shift.
Treating & Managing
Antibiotic therapy what works?
Firstline agents include trimethoprimsulfamethoxazole or nitrofurantoin, typically for 714days. Always discuss local resistance patterns with your clinician; overuse of broadspectrum antibiotics can lead to future complications.
Managing Parkinsons meds during a UTI
Sometimes a UTI can affect how your body absorbs levodopa. Doctors may adjust timing, increase the dose temporarily, or add a dopamine agonist to keep motor symptoms stable while the infection clears.
Handling urinary retention
Options include:
- Intermittent catheterisation (clean technique once every few hours).
- Alphablockers such as tamsulosin, which relax the bladder neck.
- Mirabegron (a bladderspecific 3 agonist) often highlighted as a safe .
Nonpharmacologic support
Simple habits can make a huge difference:
- Encourage a fluid scheduleabout 1.52L spread throughout the day.
- Timed voiding every 23hours, even if you dont feel the urge.
- Pelvicfloor exercises (Kegels) to strengthen bladder control.
- Probiotic supplementation (e.g., Lactobacillusrhamnosus) to maintain healthy urinary flora.
Preventive strategies
Staying ahead of UTIs is the best medicine. Here are a few evidencebased steps:
- Maintain proper perineal hygienewipe fronttoback and change underwear daily.
- Avoid prolonged catheter use; if a catheter is necessary, follow strict sterile protocols.
- Regular bladder scans for those with known retention to catch early buildup.
- Seasonal checkups with a urologist, especially after any hospitalisation.
When to consider a specialist
If infections recur more than twice a year, or if urinary retention persists despite firstline measures, its time to see a continence nurse, a urologist, or a movementdisorder neurologist. A multidisciplinary team can tailor a longterm plan that respects both motor and cognitive health.
Quick FAQ Answers
Can Parkinsons disease cause urinary problems?
Yes. The disease affects the nerves that control bladder emptying, leading to urgency, frequency, and retention.
How does a UTI affect Parkinsons disease?
A UTI can amplify tremor, increase rigidity, and trigger sudden confusion or delirium in someone with Parkinsons.
What are UTI symptoms with Parkinsons?
Look for mental fog, worsening tremor, stronger urine odor, and any sudden change in gait or balanceeven if burning isnt present.
How long does confusion from a UTI last?
Typically 27days after successful antibiotic treatment, though some patients need up to two weeks.
Can infection make Parkinsons worse?
Infections accelerate neuroinflammation, which can temporarily worsen both cognitive and motor symptoms.
What is the best treatment for Parkinsons urinary retention?
Intermittent catheterisation combined with bladdertraining and, when appropriate, mirabegron or an alphablocker.
Helpful Resources
For deeper dives and community support, consider these trusted sources:
- Parkinsons Foundation offers guides on bladder health and caregiving tips.
- U.S. Centers for Disease Control and Prevention (CDC) provides uptodate UTI prevention recommendations.
- National Institute on Aging detailed articles on infectionrelated delirium.
Downloadable tools like a UTI Symptom Tracker or a MedicationInteraction Cheat Sheet can be handy for daily monitoring (look for them on reputable healthcare websites).
Conclusion
UTIs are a common but often hidden aggravator of Parkinsons dementia and motor decline. Spotting the subtle signsconfusion, stronger urine odor, sudden fallsand acting fast with proper testing and treatment can keep symptoms from spiralling and protect quality of life. Talk to your neurologist or urologist the moment any new urinary or cognitive change appears, stay on top of hydration and bladdertraining, and use the tools above to track progress. Have you or someone you love dealt with a UTItriggered flareup? Share your experience in the commentswere stronger together.
FAQs
Can Parkinson's dementia increase UTI risk?
Yes, Parkinson's dementia increases UTI risk due to cognitive decline, reduced self-care, and higher likelihood of catheter use.
How does a UTI affect Parkinson's dementia?
A UTI can worsen confusion, memory loss, and motor symptoms in Parkinson's dementia, sometimes triggering delirium.
What are UTI symptoms in Parkinson's dementia?
Symptoms include sudden confusion, agitation, stronger urine odor, falls, and sometimes mild or absent burning.
Can UTIs make Parkinson's dementia worse?
Yes, UTIs can temporarily worsen Parkinson's dementia symptoms and may accelerate cognitive decline if untreated.