Ever felt that sudden, odd fencing pose your arm takes after a hard knock to the head? You're not alone. A fencing response is an immediate reflex that pops up seconds after a concussion-type impact, while decorticate posturing shows up later and usually signals a far more serious brain injury. Knowing which one you're looking at can be the difference between a quick checkup and an emergency call.
In the next few minutes, we'll walk through what each posture means, why they happen, what you should do if you see them, and how they affect recovery. Grab a coffee, settle in, and let's dive in together.
Quick Check Guide
What Is the Fencing Response?
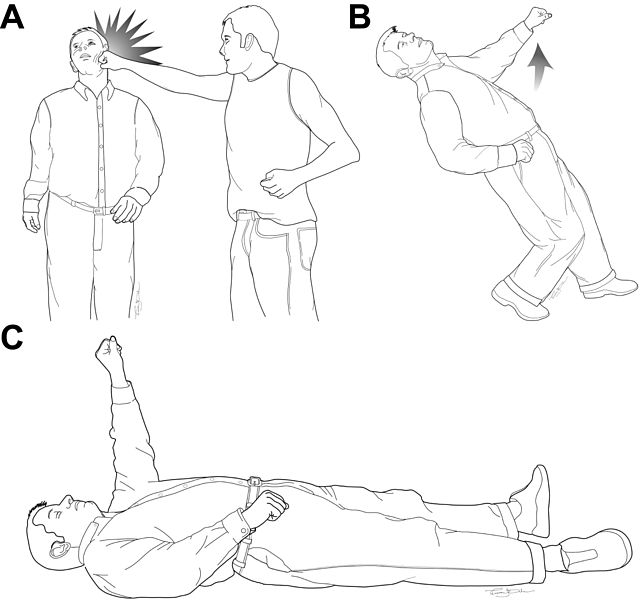
The fencing response is a brief, involuntary arm extension and pronation that appears within seconds of a head impact. It's named for the way the arm resembles a fencer's lunge. This reflex comes from the brainstem's reticular formation and usually fades within minutes to a few hours.
Real-World Example
Imagine a high school football player taking a tackle. The next thing he knows, his right arm is outstretched, palm down, while his head spins. He's startled, but the coach quickly notes the posture, stops the play, and calls for medical evaluation. That fast reaction can prevent a missed concussion.
What Is Decorticate Posturing?
Decorticate posturing is a more ominous sign: both arms flex at the elbows, shoulders curl inward, and the legs extend. It typically emerges hours to days after a severe head injury, indicating damage to the corticospinal tract above the red nucleus.
Clinical Snapshot
Dr. Patel, a neurosurgeon, explains that decorticate posturing often means the brain's higher centers are under significant pressure. When you see this, he says, it's a red flag that we need immediate neuroimaging and intensive care.
Key Clinical Differences
Timing & Underlying Physiology
Fencing response happens instantly, driven by a brainstem reflex that spikes motor activity. Decorticate appears later, reflecting structural damage deeper in the brain. Knowing the timing helps you gauge injury severity.
Comparison Table
| Feature | Fencing Response | Decorticate Posturing |
|---|---|---|
| Onset | Seconds after impact | Hours to days later |
| Typical injury severity | Mild to moderate concussion | Severe brain injury |
| Prognosis | Usually resolves quickly | Associated with poorer outcome |
| Seizure risk | Low | Higher if persistent |
| Immediate action | Monitor, seek evaluation | Emergency care, neuroimaging |
What Each Posture Tells You About Brain Damage
A fencing response often points to a functional, temporary disturbancethink of it as the brain's alarm system. Decorticate, on the other hand, suggests structural injury that may involve swelling, bleeding, or herniation. While the fencing response rarely means permanent damage, decorticate can be a sign of lasting consequences.
If you or someone you know has had a brain injury and exhibits unusual postures, it's essential to assess for related neurological conditions that might require ongoing management. For instance, patients with conditions like atypical Rett syndrome often face complex neurological symptoms that need specialized care and support.
Top Common Questions
Can a Fencing Response Lead to Death?
It's extremely rare. The response itself is a reflex, not a sign of catastrophic swelling. However, it does flag a concussion that warrants medical attention.
Is the Fencing Response Bad?
Not inherently. It's a signal that the brain has been jolted. Think of it like a car's check-engine lightit's not the problem, but it tells you to look under the hood.
Does It Mean Brain Damage?
Mostly functional disruption, not permanent structural damage. Most people recover fully with proper rest and evaluation.
What About Head Injuries?
The fencing response often appears after a direct blow, sudden acceleration, or even a whiplash-type motion. Spotting this reflex can improve concussion diagnosis on the field.
Is It a Reliable Concussion Marker?
Yes. Researchers have found that the presence of a fencing response correlates strongly with concussive forces and can help clinicians decide when to sideline athletes.
What Should I Do If I See It?
Stop activity immediately, call emergency services if the person loses consciousness or shows other severe signs, keep the head still, and monitor breathing.
Why Do the Fingers Curl?
The reflex engages extensor muscles, often leaving the hand supinated with a slight flexion of the fingersan involuntary grip that looks like a fencer's hand ready to thrust.
Can It Trigger a Seizure?
The response itself isn't a seizure, but severe head trauma can coexist with posttraumatic seizures. Keep an eye out for convulsions and seek urgent care if they occur.
First Aid Steps
Immediate Checklist
- Stop the activity or sport.
- Assess consciousnessask simple questions.
- Call 911 if there's loss of consciousness, vomiting, or worsening posture.
- Keep the person still; avoid moving the neck.
- Monitor breathing and pulse until help arrives.
Sample Script for Bystanders
Hey, we need to keep you still. I'm calling emergency services now. Stay with me, focus on your breathing, and try not to move your head.
Medical Evaluation: What Docs Look For
Doctors will usually order a CT or MRI to check for bleeding, assess the Glasgow Coma Scale, and perform a full neurological exam. Observation in a hospital may be recommended even if imaging is clear, especially with a fencing response.
When Imaging Is Needed
If decorticate posturing appears, imaging is virtually mandatory. For a fencing response, imaging is considered if symptoms persist, there's a loss of consciousness, or the patient has a history of prior brain injury.
Long-Term Outlook
Recovery After a Fencing Response
Most athletes return to play within a week to ten days, following a graduated return-to-activity protocol. Rest, hydration, and gradual cognitive loading are key.
Rehab Tips
- Start with light aerobic activity (walking, stationary bike).
- Progress to balance drills and sports-specific drills only when symptom-free.
- Consider a neurocognitive test before full return.
Prognosis After Decorticate Posturing
Survival rates vary widely based on cause and speed of treatment. Intensive care, controlling intracranial pressure, and early surgery can improve outcomes, but many patients face long-term disabilities.
Support for Families
Family members should stay informed, ask for clear timelines, and seek counseling if needed. Coordinating with a multidisciplinary teamneurologists, physical therapists, and social workershelps manage the road ahead.
Bottom Line Takeaway
In a nutshell, the fencing response is an immediate, reflex-driven sign of a mild to moderate concussion, while decorticate posturing is a delayed indicator of severe brain injury. Spotting the difference quickly can guide you to the right level of carewhether it's a prompt evaluation or an emergency response.
Next time you're on the field, at the gym, or even at home, keep an eye out for those telltale arm positions. If you or someone you know experiences either posture, don't waitact fast, get professional help, and follow recovery steps. Your brain will thank you.
What's your experience with these postures? Have you ever seen a fencing response in action? Share your story in the comments below, and feel free to ask any questions you might have. We're here to help each other stay safe and informed.
FAQs
How can I tell if someone is showing a fencing response?
Look for a sudden, involuntary extension of one arm with the palm facing down, often accompanied by a brief head turn. It appears within seconds of a head impact and fades quickly.
What does decorticate posturing indicate about brain injury?
Decorticate posturing signals damage to the corticospinal tract above the red nucleus, usually reflecting a severe brain injury that requires immediate neuro‑imaging and intensive care.
Should I call emergency services if I see a fencing response?
If the person is conscious, has no other severe symptoms, and the posture resolves quickly, monitor and seek medical evaluation. Call emergency services if there is loss of consciousness, vomiting, worsening posture, or any sign of a serious head injury.
Can a fencing response turn into a more serious condition?
The response itself is a reflex, not a progressive condition. However, it indicates a concussion‑type impact, so proper evaluation and rest are essential to prevent complications.
What are the treatment steps after observing decorticate posturing?
Immediate emergency care is required: stabilize the airway, call 911, keep the neck immobile, and transport the patient for CT/MRI imaging. Hospital management focuses on controlling intracranial pressure and addressing the underlying cause.