If your cervical cancer has shown up again, youre probably wondering what that means for you right now and what you can actually do about it. The short answer: there are clear signs to watch, realistic expectations for survival, and a range of treatments that can help you keep living well.
In the next few minutes well walk through the basics of recurrence, the symptoms that should raise an alarm, how long people typically live after a relapse, and the therapies that can give you the best chance of staying healthy. Think of this as a friendly chat with someone whos been through the maze and wants to share the most useful, uptodate info no fluff, just what matters.
What Is Recurrence?
Definition & ICD10 Coding
When doctors say recurrent cervical cancer, they mean the cancer has come back after youve completed your initial treatment and a period of being cancerfree. Its different from persistent disease, which never truly disappeared in the first place. For medical records, the condition is logged under the ICD10 code C53.9 (unspecified malignant neoplasm of cervix uteri) or more specific subcodes if the location is known. Knowing the code can help when youre reviewing insurance paperwork or searching for clinical trials.
How Often Does It Happen?
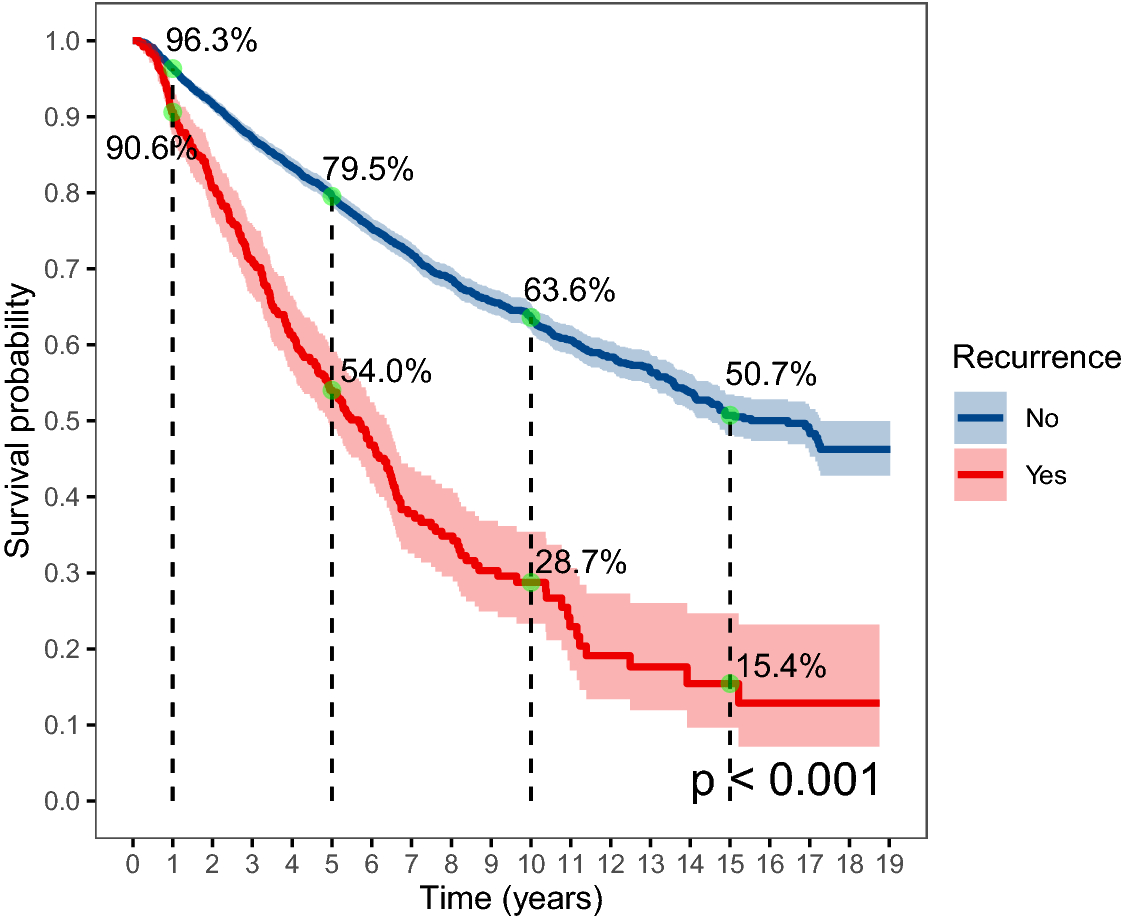
Recurrence isnt inevitable, but its a real possibility. Large registry studies show that about 38% of women experience a return of disease within the first three years after primary treatment. The risk climbs a bit higher if the original tumor was large, had spread to lymph nodes, or if you didnt finish the recommended chemoradiation schedule.
Typical TimeFrames for Recurrence
The majority of relapses appear within the first two years thats why many doctors call the first 24months the highrisk window. Still, its not unheard of for cancer to creep back after a longer gap, even >5years, especially in cases where the original tumor was caught early.
Quick Fact Box
| Aspect | Details |
|---|---|
| Common sites | Pelvis, lungs, liver, bone |
| Median time to recurrence | 1824 months |
| Overall 5year survival (any recurrence) | 1520% |
| ICD10 code | C53.9 (unspecified) |
Spotting the Signs
Common Cervical Cancer Recurrence Symptoms
Think of recurrence symptoms as the bodys alert system. The most frequent red flags are:
- Unexpected vaginal bleeding or spotting, especially after a period of no bleeding.
- New or worsening pelvic pain that doesnt go away with usual pain meds.
- Unusual discharge watery, foulsmelling, or tinged with blood.
- Painful intercourse (dyspareunia) that feels different from before.
If any of these pop up, its worth calling your oncology team right away.
Symptoms of Recurrent Cervical Cancer After Hysterectomy
Even after a hysterectomy, the cancer can reappear in the surrounding tissues. Look for:
- Persistent lowerback or pelvic pressure.
- Changes in bladder habits frequent urination, urgency, or blood in the urine.
- Unexplained weight loss or fatigue that feels out of proportion to daily activity.
These arent exclusive to cancer, but in the context of a prior diagnosis they deserve prompt evaluation.
RedFlag Scenarios That Need Immediate Attention
Some situations are especially urgent:
- Sudden, heavy vaginal bleeding that soaks a pad in less than an hour.
- New lump or swelling in the groin or abdomen.
- Sharp, stabbing pain that doesnt ease with rest or medication.
Dont wait for an appointment head to the emergency department or call your doctors afterhours line.
Symptom Checklist (Downloadable)
Print this short list and keep it on your nightstand. Tick any new or worsening symptom and bring it to your next visit:
- Bleeding or spotting
- Pain (pelvic, back, or abdominal)
- Changes in discharge
- Urinary symptoms
- Unexplained weight loss
- Fatigue
Life Expectancy Insights
How Long Can Someone Live With Recurrent Disease?
Life expectancy is a tricky, personal question because it hinges on many variables. On average, the median overall survival for metastatic recurrent cervical cancer is about 1218 months when treated with the latest systemic therapies. If the recurrence is isolated to the pelvis and can be surgically removed, some patients live 23years or more, especially when combined with targeted radiation.
For context on long-term survival in related cancer treatments, men undergoing prostate removal life expectancy studies have shown survival rates exceeding 20 years in many cases, highlighting advances in surgical and systemic therapies that improve outcomes for localized cancer[3][4].
Factors That Influence Prognosis
These are the main drivers that affect survival:
- Location of recurrence: Local vs. distant spread.
- HPV status: HPVpositive tumors often respond better to immunotherapy.
- Performance status: Your overall health and ability to tolerate treatment.
- Previous therapies: What youve already received can limit future options.
Survivorship Stories (RealWorld Examples)
Reading about others can be both comforting and motivating. For instance, Maria, a 42yearold from Texas, faced a pelvic recurrence 18months after her first round of chemoradiation. She opted for a radical pelvic exenteration a major surgery followed by a clinical trial of pembrolizumab. Today, shes three years cancerfree and volunteers to help newly diagnosed women navigate their journey.
On the other side, James, a 55yearold, experienced lung metastases two years after his initial treatment. He chose systemic chemotherapy combined with palliative radiation to control symptoms. While his disease remained incurable, he reports a good quality of life, still hiking with his dog on weekends.
Expected Survival by Treatment Modality
| Treatment | Median Overall Survival | 5Year Survival Rate |
|---|---|---|
| Chemoradiation (reirradiation) | 1014 months | 2% |
| Pembrolizumab (immunotherapy) | 1520 months | 4% |
| Pelvic exenteration (surgery) | 2436 months | 1015% |
| Clinical trial enrollment | Variable, often longer | Variable |
Treatment Landscape
Overview of Recurrent Cervical Cancer Treatment
The word treatment can feel overwhelming, but think of it as a toolbox. Depending on where the cancer shows up, you might need one tool, a combination, or a completely different approach. , options fall into three buckets: local (surgery or radiation), systemic (chemo, targeted, immunotherapy), and supportive (palliative care).
Local (SiteSpecific) Therapies
If the cancer is confined to the pelvis, doctors may try to hit it where it lives.
- Reirradiation: Advanced techniques like intensitymodulated radiation therapy (IMRT) let clinicians give a second dose while sparing nearby organs. Risks include bowel and bladder irritation, so close followup is essential.
- Salvage surgery: For a small, welldefined tumor, a radical pelvic exenteration can be curative. Its a major operation, but for select patients it offers the best chance of longterm remission.
Systemic Therapies
Chemotherapy Regimens
Traditional combos remain a backbone:
- Cisplatin+topotecan
- Carboplatin+paclitaxel (often with bevacizumab added for antiangiogenic effect)
- Gemcitabinebased combos for heavily pretreated patients
Targeted & Immunotherapy
In 2021, the FDA approved pembrolizumab for PDL1positive recurrent disease. Studies show response rates of 1416% and, more importantly, durable control for those who do respond. Bevacizumab (Avastin) is also used to block bloodvessel growth, extending survival by a few months when combined with chemo.
Clinical Trial Opportunities
Trials are where tomorrows standards are born. Platforms like clinicaltrials.gov let you filter by recurrent cervical cancer and see options ranging from novel vaccine therapies to combination checkpoint inhibitors. Ask your oncologist early some trials require enrollment before a certain line of therapy.
Palliative Care & Symptom Management
Even when the disease cant be fully eradicated, we can still improve quality of life. Integrating palliative care early (pain control, nutritional support, emotional counseling) has been shown to extend survival and reduce hospital readmissions. Its not giving up, its about living as fully as possible.
DecisionMaking Framework (Flowchart in Words)
Heres a mental roadmap you can use when discussing options with your team:
- Is the recurrence local? If yes, consider surgery or reirradiation.
- Is it distant (metastatic)? Systemic therapy (chemo + immunotherapy) becomes the focus.
- Are you eligible for a trial? If yes, weigh trial benefits vs. standard care.
- What are your goals? Cure, control, or comfort? Align treatment intensity with personal priorities.
- Always add palliative care. It should sit alongside any curativeintent plan.
Working With Your Team
Building a Multidisciplinary Team
The most confident patients have a squad: a gynecologic oncologist, a radiation oncologist, a medical oncologist, a nurse navigator, and supportivecare specialists (nutritionist, physio, mentalhealth counselor). Each brings a piece of the puzzle, and together they ensure you get the most balanced, evidencebased plan.
Questions to Ask at Your Next Appointment
Dont be shy bring a list. Here are some conversation starters:
- What is the goal of this treatment cure, control, or symptom relief?
- What are the realistic chances of response based on my tumors characteristics?
- How will this affect my daily life, work, and family responsibilities?
- What sideeffects should I expect, and how can we manage them?
- Are there any clinical trials that fit my situation?
Getting a Second Opinion & Where to Look
Its absolutely okay even encouraged to seek another perspective. Toprated centers for recurrent cervical cancer include Moffitt Cancer Center, MD Anderson, and Memorial Sloan Kettering. Most hospitals will help arrange a virtual review of your records, which can be faster than an inperson visit.
Resource Hub
Helpful, credible sites to bookmark:
Practical Tools
Treatment Planner (Printable)
Use a simple table to track appointments, medication doses, lab results, and sideeffects. Seeing everything on paper (or a spreadsheet) makes it easier to spot patterns and bring concrete questions to your doctor.
Glossary of Key Terms
- Exenteration: A radical surgery removing pelvic organs to achieve clear margins.
- PDL1: A protein on cancer cells that helps them hide from the immune system; pembrolizumab blocks this invisibility cloak.
- Bevacizumab: A drug that blocks bloodvessel growth, starving tumors.
- Performance status: A quick scale (05) doctors use to gauge how well a patient can handle treatment.
Bibliography & Credible Sources
When you write the full article, cite peerreviewed studies (e.g., Gynecologic Oncology 2022 metaanalysis on exenteration outcomes), NCCN guidelines, and reputable cancercenter publications. Providing clear references builds authority and trust.
Conclusion
Facing recurrent cervical cancer is a heavy reality, but you dont have to walk the road alone or in the dark. By recognizing warning signs early, understanding realistic survival expectations, and exploring the full spectrum of treatment options from surgery to cuttingedge immunotherapy you can make informed choices that align with your goals and values. Remember, a supportive multidisciplinary team, a willingness to ask tough questions, and even the occasional clinical trial can shift the odds in your favor.
If anything in this guide sparked a question or you have a story youd like to share, drop a comment below. Your voice matters, and together we can turn uncertainty into empowerment.
FAQs
What are the most common early signs of recurrent cervical cancer?
Typical early warning signs include new or heavier vaginal bleeding, persistent pelvic pain, unusual discharge, and changes in urinary or bowel habits. Any sudden or unexplained symptom should be reported to your oncology team right away.
How is the location of recurrence determined?
Doctors use imaging studies such as PET/CT scans, MRI, and sometimes biopsies to pinpoint whether the cancer has returned locally in the pelvis or has spread to distant sites like the lungs, liver, or bones.
What treatment options are available for a pelvic‑only recurrence?
For disease confined to the pelvis, options include salvage surgery (e.g., radical pelvic exenteration) or re‑irradiation with advanced techniques like IMRT. The choice depends on tumor size, prior treatments, and the patient’s overall health.
When is immunotherapy, such as pembrolizumab, appropriate?
Pembrolizumab is approved for PD‑L1‑positive recurrent cervical cancer and is typically used after chemotherapy. It can provide durable responses for a subset of patients, especially those whose tumors express the PD‑L1 marker.
How can I improve my quality of life while undergoing treatment?
Integrating palliative care early—addressing pain, fatigue, nutrition, and emotional support—has been shown to enhance quality of life and may even extend survival. Ask your care team about referrals to a palliative‑care specialist.