Pep airway clearance is a simple, lowcost technique that uses a small handheld device to add resistance while you exhale, helping loosen and move mucus out of the lungs. In the next few minutes youll learn how it works, which devices are best, when to avoid it, and stepbystep tips so you can start clearing your airways safely today.
How It Works
What is pep therapy used for?
At its core, pep (Positive Expiratory Pressure) therapy is all about keeping your airways open long enough for mucus to slide out. When you exhale against a slight resistance, the pressure created behind the blockage helps splint the airway walls, preventing them from collapsing. That extra pressure pushes air into the small sidebranches of the lungs where mucus loves to hide.
What happens inside the lungs during pep?
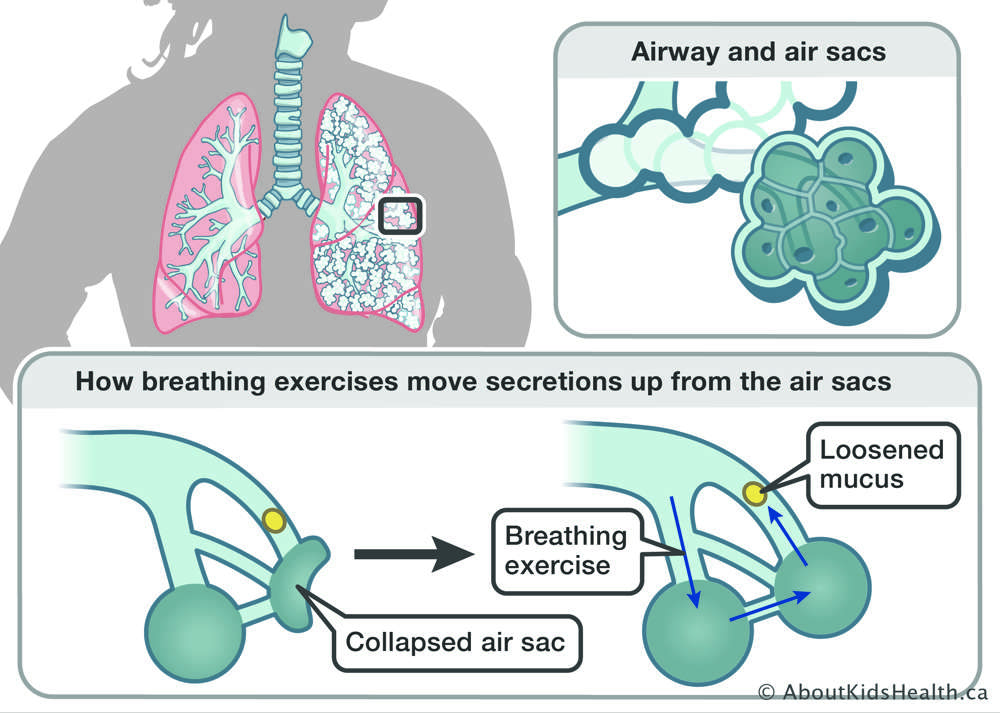
Think of your lungs like a network of tunnels. In a healthy system, air gushes in and out with ease. When mucus builds up, some tunnels narrow or close, trapping secretions. Pep creates a gentle backpressure that inflates those narrow tunnels, a phenomenon scientists call collateral ventilation. The result? Air reaches deeper parts of the lung, loosening the gunk so you can cough it up.
Why is positive expiratory pressure beneficial?
Unlike the usual huff or cough where you blast air out, pep adds a modest, steady resistance. This steadiness reduces the risk of airway collapse and gives the mucus a chance to detach without the harsh spikes that can irritate sensitive tissue. A recent found that patients using pep devices showed modest improvements in FEV and reported fewer exacerbations compared with plain breathing exercises.
Device Types
What are the main types of pep devices?
There are three popular families of pep equipment, each with its own vibe:
- Static PEP Classic masks or mouthpieces that provide a fixed resistance (e.g., Flutter or PEP mask).
- Oscillating PEP Devices that add a rapid vibration to the airflow (e.g., Aerobika, Acapella), which can further shake loose stubborn mucus.
- Bubble PEP The DIY version: a waterfilled bottle with a straw. You breathe out through the straw, creating bubbles that give you the needed pressure.
Which pep device is best for mucus clearance?
If youre hunting the best pep device, look at three factors: resistance range, ease of cleaning, and whether you want vibration. Oscillating devices often win the prize for thick mucus because the added wobble helps break up clumps. However, a static mask can be perfectly adequate for milder secretions and might be more budgetfriendly.
| Device | Resistance (cm HO) | Vibration | Cost | Ideal For |
|---|---|---|---|---|
| Flutter | 515 | No | $$ | Pediatric, occasional use |
| Aerobika | 1020 | Yes | $$$ | Chronic bronchitis, COPD |
| Bubble PEP (DIY) | 512 | No | $ | Home experiment, lowbudget |
Bubble pep for adults does it work?
Surprisingly, yes! The concept is the same: exhaling through a waterfilled bottle builds pressure as bubbles form. Some adults find the bubble sound oddly soothing, turning a medical routine into a minirelaxation ritual. Just be sure the bottle is sturdy, the water is clean, and the straw fits snugly.
How to use a pep device correctly?
Heres a quick, friendtofriend walkthrough:
- Sit upright, shoulders relaxed.
- Take a normal breath in through your nose.
- Seal the mouthpiece (or place the straw in your mouth) and exhale slowly and steadily against the resistance. Aim for 1015 breaths per set.
- Take a short pause, then repeat for 23 sets.
- Finish with a gentle cough to clear the loosened mucus.
Keep the resistance at a level where you can maintain a smooth exhale without straining. If it feels like youre pushing too hard, dial the resistance down.
Pep device maintenance & hygiene
Cleaning is a must. Rinse the mouthpiece with warm water after each session, then soak it once a week in a mild disinfectant (e.g., diluted hydrogen peroxide). Let it airdry before storing. Avoid harsh chemicals that could degrade the plastic.
Clinical Benefits
What are the proven benefits of pep airway clearance?
Research consistently shows that regular pep use can:
- Increase sputum volume, making it easier to expectorate.
- Improve lung function metrics such as FEV and FVC.
- Reduce the frequency of respiratory infections and hospital readmissions.
- Enhance qualityoflife scores, especially in cystic fibrosis and bronchiectasis patients.
Can pep improve quality of life?
Patients often report feeling "less breathless" and more in control of their daily activities. A survey by the Cystic Fibrosis Foundation noted that participants who incorporated pep into their routine felt more confident traveling and exercising. For those navigating cystic fibrosis relationships, incorporating airway clearance into daily routines can reduce treatment burden and improve shared activities.
Does pep reduce hospital readmissions?
One longitudinal study of COPD patients showed a 15% drop in readmission rates among those who performed pep therapy twice daily compared with a control group receiving standard care.
When is pep therapy NOT recommended?
Safety first! Pep therapy contraindications include:
- Uncontrolled hemoptysis (significant coughing up of blood).
- Recent thoracic surgery or rib fractures.
- Severe pneumothorax (collapsed lung).
- Active respiratory infections where coughing could spread pathogens.
If any of these apply, pause the therapy and talk to your healthcare provider. Balancing benefits with risks is the hallmark of trustworthy care.
How does pep compare with other airway clearance techniques?
Heres a snapshot of the main options:
| Technique | Pros | Cons |
|---|---|---|
| Pep (static/oscillating) | Easy, portable, inexpensive, good for daily use | May need coaching for optimal technique |
| Highfrequency chest wall oscillation (vest) | Handsfree, great for severe mucus | Expensive, bulky |
| Autogenic drainage | No equipment needed, highly customizable | Learning curve, requires therapist guidance |
Daily Routine
Creating a personalized pep schedule
Most experts recommend 23 sessions per day, ideally after inhaled medication when the airways are more relaxed. Each session typically lasts 1015 minutes. Feel free to experiment: some people swear by a morning wakeup set, a midday midbreak set, and an evening winddown set.
Integrating pep with inhaled meds
Take your bronchodilator or mucolytic first, wait a couple of minutes for it to take effect, then dive into your pep routine. The dilated airways let the pressure work more efficiently, and the loosened mucus is easier to cough out.
Tips for children & seniors
For kids, choose a colorful mask or a smaller mouthpiece and turn the session into a game (Can you blow as many bubbles as you can?). For seniors, a lightweight static mask is often simpler, and a caregiver can assist with the seal to ensure comfort.
Common mistakes & how to avoid them
- Overexertion: Pushing too hard can cause dizziness. Keep the exhale smooth.
- Leaky seal: Air escaping around the mouthpiece reduces pressure. Adjust the fit.
- Too high resistance: If you cant finish a set, dial it down.
Tracking progress & when to seek help
Grab a small notebook or a phone note and jot down:
- Date and time of each session.
- Number of breaths per set.
- How much sputum you expectorated.
- Any new symptoms (fever, increased shortness of breath).
If you notice a sudden spike in coughing, a fever, or a feeling of tightness that doesnt improve, its time to call your respiratory therapist or doctor.
RealWorld Experiences
Patient story: living with cystic fibrosis
Emily, a 22yearold college student, describes pep as her secret weapon. She says, I used to dread class mornings because my lungs felt clogged. After I started using an Aerobika twice a day, I could actually finish my lectures without a coughing fit. Its like giving my lungs a gentle wakeup call. For anyone Pep airway clearance is a simple, lowcost technique that uses a small handheld device to add resistance while you exhale, helping loosen and move mucus out of the lungs. In the next few minutes youll learn how it works, which devices are best, when to avoid it, and stepbystep tips so you can start clearing your airways safely today. At its core, pep (Positive Expiratory Pressure) therapy is all about keeping your airways open long enough for mucus to slide out. When you exhale against a slight resistance, the pressure created behind the blockage helps splint the airway walls, preventing them from collapsing. That extra pressure pushes air into the small sidebranches of the lungs where mucus loves to hide. Think of your lungs like a network of tunnels. In a healthy system, air gushes in and out with ease. When mucus builds up, some tunnels narrow or close, trapping secretions. Pep creates a gentle backpressure that inflates those narrow tunnels, a phenomenon scientists call collateral ventilation. The result? Air reaches deeper parts of the lung, loosening the gunk so you can cough it up. Unlike the usual huff or cough where you blast air out, pep adds a modest, steady resistance. This steadiness reduces the risk of airway collapse and gives the mucus a chance to detach without the harsh spikes that can irritate sensitive tissue. A recent found that patients using pep devices showed modest improvements in FEV and reported fewer exacerbations compared with plain breathing exercises. There are three popular families of pep equipment, each with its own vibe: If youre hunting the best pep device, look at three factors: resistance range, ease of cleaning, and whether you want vibration. Oscillating devices often win the prize for thick mucus because the added wobble helps break up clumps. However, a static mask can be perfectly adequate for milder secretions and might be more budgetfriendly. Surprisingly, yes! The concept is the same: exhaling through a waterfilled bottle builds pressure as bubbles form. Some adults find the bubble sound oddly soothing, turning a medical routine into a minirelaxation ritual. Just be sure the bottle is sturdy, the water is clean, and the straw fits snugly. Heres a quick, friendtofriend walkthrough: Keep the resistance at a level where you can maintain a smooth exhale without straining. If it feels like youre pushing too hard, dial the resistance down. Cleaning is a must. Rinse the mouthpiece with warm water after each session, then soak it once a week in a mild disinfectant (e.g., diluted hydrogen peroxide). Let it airdry before storing. Avoid harsh chemicals that could degrade the plastic. Research consistently shows that regular pep use can: Patients often report feeling "less breathless" and more in control of their daily activities. A survey by the Cystic Fibrosis Foundation noted that participants who incorporated pep into their routine felt more confident traveling and exercising. For those managing cystic fibrosis, integrating airway clearance into relationship routines or daily schedules can make adherence easier and support overall wellbeing; learn more about navigating cystic fibrosis relationships when planning treatments and daily care. One longitudinal study of COPD patients showed a 15% drop in readmission rates among those who performed pep therapy twice daily compared with a control group receiving standard care. Safety first! Pep therapy contraindications include: If any of these apply, pause the therapy and talk to your healthcare provider. Balancing benefits with risks is the hallmark of trustworthy care. Heres a snapshot of the main options: Most experts recommend 23 sessions per day, ideally after inhaled medication when the airways are more relaxed. Each session typically lasts 1015 minutes. Feel free to experiment: some people swear by a morning wakeup set, a midday midbreak set, and an evening winddown set. Take your bronchodilator or mucolytic first, wait a couple of minutes for it to take effect, then dive into your pep routine. The dilated airways let the pressure work more efficiently, and the loosened mucus is easier to cough out. For kids, choose a colorful mask or a smaller mouthpiece and turn the session into a game (Can you blow as many bubbles as you can?). For seniors, a lightweight static mask is often simpler, and a caregiver can assist with the seal to ensure comfort. Grab a small notebook or a phone note and jot down: If you notice a sudden spike in coughing, a fever, or a feeling of tightness that doesnt improve, its time to call your respiratory therapist or doctor. Emily, a 22yearold college student, describes pep as her secret weapon. She says, I used to dread class mornings because my lungs felt clogged. After I started using an Aerobika twice a day, I could actually finish my lectures without a coughing fit. Its like giving my lungs a gentle wakeup call. Mark, 68, was told he needed a hospital stay after a flareup. Instead, his pulmonologist prescribed a daily pep routine with a static mask plus his usual inhalers. Within a week, his sputum production dropped, oxygen saturation rose from 89% to 94%, and he avoided admission altogether. Laura, a certified respiratory therapist, emphasizes the importance of proper coaching. The first few sessions can feel awkward, but once patients master the seal and breathing rhythm, pep becomes almost second nature. Its a lowtech tool with highimpact results. Pep airway clearance is a lowcost, evidencebacked way to move mucus, keep airways open, and improve breathing quality. The benefits are clear, but proper technique and awareness of contraindications are vital. By choosing the right device, fitting it into a realistic daily routine, and staying attentive to how your body responds, you can make a noticeable difference in your respiratory health. Ready to give it a try? Download our printable Pep Routine Checklist below, watch the short tutorial video, or schedule a quick chat with a certified respiratory therapist to personalize your plan. Your lungs will thank you. PEP airway clearance is a technique that uses a small handheld device to add resistance to your exhaled breath, helping to loosen and move mucus out of the lungs, especially for people with chronic respiratory conditions like COPD or cystic fibrosis[3][4]. A PEP device creates positive pressure during exhalation, which helps keep airways open and allows air to reach behind mucus blockages, making it easier to cough out secretions[3][4]. Oscillating PEP devices add vibrations to further help break up thick mucus[1][5]. PEP therapy is especially helpful for people with conditions that cause mucus buildup, such as cystic fibrosis, COPD, bronchiectasis, and sometimes asthma[1][3]. Regular use may improve lung function and quality of life[1][2]. PEP therapy should be avoided if you have uncontrolled coughing up of blood, recent chest surgery, pneumothorax, or certain severe cardiovascular conditions. Always consult your healthcare provider before starting[5]. Most experts recommend using a PEP device 2–3 times per day, with each session lasting 10–15 minutes, ideally after using inhaled medications to maximize effectiveness[1][3].How It Works
What is pep therapy used for?
What happens inside the lungs during pep?
Why is positive expiratory pressure beneficial?
Device Types
What are the main types of pep devices?
Which pep device is best for mucus clearance?
Device Resistance (cm HO) Vibration Cost Ideal For Flutter 515 No $$ Pediatric, occasional use Aerobika 1020 Yes $$$ Chronic bronchitis, COPD Bubble PEP (DIY) 512 No $ Home experiment, lowbudget Bubble pep for adults does it work?
How to use a pep device correctly?
Pep device maintenance & hygiene
Clinical Benefits
What are the proven benefits of pep airway clearance?
Can pep improve quality of life?
Does pep reduce hospital readmissions?
When is pep therapy NOT recommended?
How does pep compare with other airway clearance techniques?
Technique Pros Cons Pep (static/oscillating) Easy, portable, inexpensive, good for daily use May need coaching for optimal technique Highfrequency chest wall oscillation (vest) Handsfree, great for severe mucus Expensive, bulky Autogenic drainage No equipment needed, highly customizable Learning curve, requires therapist guidance Daily Routine
Creating a personalized pep schedule
Integrating pep with inhaled meds
Tips for children & seniors
Common mistakes & how to avoid them
Tracking progress & when to seek help
RealWorld Experiences
Patient story: living with cystic fibrosis
Case study: COPD exacerbation managed at home
Physiotherapists perspective
Conclusion
FAQs
What is PEP airway clearance?
How does a PEP device work?
Who can benefit from PEP therapy?
Are there any risks or times to avoid PEP?
How often should I use a PEP device?