Hey there! If youve ever stared at a screen, typed pain treatment options, and felt a wave of overwhelm, youre not alone. Whether youre battling a nagging back ache, wrestling with chronic joint pain, or dealing with severe flareups, finding the right relief can feel like searching for a needle in a haystack. The good news? There are plenty of paths to feel bettersome involve a tiny pill, others a gentle stretch, and a few even a bit of tech magic. Below, Ill walk you through the most common options, the pros and cons of each, and a simple plan to start testing what works for you.
Medication Based Options
OvertheCounter Relief
First stop on most peoples list is the pharmacy aisle. Nonsteroidal antiinflammatory drugs (NSAIDs) like ibuprofen or naproxen, and acetaminophen (Tylenol) are the goto buddies for mildtomoderate aches. Theyre fast, cheap, and you dont need a prescription.
Benefits: Quick pain knockdown, reduces inflammation (especially NSAIDs).
Risks: Stomach irritation, higher bleed risk, and possible kidney strain if you overdo them. A simple tip? Take them with food and avoid daily use longer than ten days unless a doctor says its safe.
Prescription Pain Medications
When OTCs arent enough, doctors may suggest prescription meds. These fall into a few families:
- Opioids (e.g., morphine, oxycodone): Powerful for severe pain but come with dependence, tolerance, and respiratorydepression risks. The stress the lowest effective dose, shortest duration rule.
- COX2 inhibitors (e.g., celecoxib): Target inflammation with less stomach upset than traditional NSAIDs, but watch for cardiovascular warnings.
- Antidepressants (SNRIs like duloxetine, TCAs like amitriptyline): Helpful for neuropathic pain and often doubleduty for mood.
- Antiseizure drugs (gabapentin, pregabalin): Work wonders for nerverelated pain (think shingles or diabetic neuropathy).
Every class has its sweet spot, and the best pain medication for chronic pain is the one that matches your pain type, health background, and lifestyle.
Injectable & Targeted Therapies
Sometimes a single injection can give a few weeks of relief. Common types include:
- Triggerpoint injections (local anesthetic + steroid) for tight muscle knots.
- Epidural steroid injections for radicular (nerve root) pain.
- Nerve blocks using anesthetic agents to turn off painful signals.
These are usually paired with physical therapy to keep the gains moving forward.
Procedural and Device Options
Transcutaneous Electrical Nerve Stimulation (TENS)
A TENS unit is a small, batterypowered gadget that sends mild electrical pulses through the skin. The idea? Gate control theory the pulses jam the pain signals before they reach the brain. A 2024 systematic review (see ) found modest pain reduction for lowback and knee osteoarthritis. Its drugfree, portable, and you can try it at home.
Neuromodulation & Surgical Implants
If pain has turned chronic despite meds and PT, neurodevices might help. Options include:
- Spinal cord stimulators a tiny wire placed near the spine, sending gentle tingles to mask pain.
- Peripheral nerve stimulators target a specific nerve (e.g., the sciatic nerve).
- Intrathecal pumps deliver tiny doses of medication directly into the spinal fluid, lowering systemic sideeffects.
These are big decisions, usually reserved after interdisciplinary review. The notes they can cut opioid use by up to 50% in selected patients.
Minimally Invasive Procedures
Procedures like radiofrequency ablation, cryoablation, or prolotherapy aim to alter paingenerating tissue without major surgery. Theyre often outpatient, with quick recovery times.
Therapy Driven Options
Physical & Occupational Therapy
Think of therapy as the maintenance crew for your body. A skilled therapist will:
- Teach you proper movement patterns to reduce strain.
- Use manual techniques to loosen tight muscles.
- Prescribe homeexercise programs that build strength and flexibility.
Studies from show that combining PT with medication often yields the best functional outcomes.
CognitiveBehavioral Therapy (CBT) & Mindfulness
It might sound odd, but the way you think about pain can amplify it. CBT helps reframe catastrophic thoughts (Ill never be able to walk again) into realistic goals. Mindfulness meditation teaches you to observe pain without judgment, which can lower its emotional intensity.
One randomized trial found that patients receiving CBT reduced opioid doses by ~30% compared with standard care ().
Biofeedback & Guided Imagery
These techniques give you realtime data (like heart rate) and teach you to control physiological stress, which often reduces perceived pain. Affordable apps now offer guided sessions you can try before bedtime.
Complementary Lifestyle Options
Acupuncture & Massage
Both aim to stimulate the bodys own painrelief chemicals. A metaanalysis in concluded that acupuncture provides moderate relief for chronic lowback pain, especially when combined with conventional care.
Heat, Cold, Exercise, Yoga, & Tai Chi
Simple tools that pack a punch:
- Heat: Relaxes muscles, improves blood flow.
- Cold: Reduces swelling and numbs sharp pain.
- Exercise: Releases endorphins natures own opioids.
- Yoga/Tai Chi: Blend gentle movement with breath work, perfect for chronic tension.
Nutrition & Weight Management
Inflammation loves sugar, refined carbs, and trans fats. Adding omega3 rich foods (salmon, walnuts) and spices like turmeric can dial down systemic inflammation. Maintaining a healthy weight also eases joint load, especially for knees and hips.
Choosing the Right Option
Now that weve surveyed the landscape, how do you pick a path? Heres a friendly checklist you can run through:
- Identify pain type: Is it nociceptive (from tissue damage), neuropathic (nerverelated), or a mix?
- Review medical history: Liver or kidney issues, allergies, previous opioid exposure.
- Set realistic goals: Less pain, more function, better sleep? Write them down.
- Start low, go slow: Begin with OTC or a lowimpact therapy, then step up if needed.
- Track progress: Keep a simple diary note pain level (010), activities, meds taken.
- Checkin with a professional: A pain specialist or primary care doctor can help you calibrate the plan.
Tip: Download a that you can print and fill out each week. Its a handy way to visualize trends and discuss them with your clinician.
Risks and Benefits
| Option | Primary Benefit | Main Risk / SideEffect | Mitigation Strategy |
|---|---|---|---|
| NSAIDs | Fast antiinflammatory relief | GI bleed, kidney strain | Take with food, limit duration |
| Opioids | Powerful analgesia for severe pain | Dependence, respiratory depression | Lowest effective dose, regular review |
| TENS | Drugfree, portable pain masking | Skin irritation, modest efficacy for deep pain | Rotate electrode sites, combine with PT |
| CBT | Improves coping, may lower opioid need | Requires time & therapist access | Telehealth sessions, selfguided apps |
| Acupuncture | Targets trigger points, low systemic risk | Variable practitioner skill | Choose licensed acupuncturist, verify credentials |
Remember, no single option is a magic bullet. The magic happens when you balance what works for you with a realistic view of the downsides.
Sample 4Week Plan
Heres a starter roadmap you can tweak. It blends medication, movement, and mindcalming techniquesall doable without a pharmacyorder for every step.
- Week1: Take an NSAID (if safe) after meals for breakthrough pain. Add a 20minute brisk walk most days and finish each morning with 5minutes of mindful breathing.
- Week2: Schedule two physicaltherapy sessions. Use a warmpack on sore spots after activity. Keep a pain diary.
- Week3: If pain stays above 4/10, call your doctor about a lowdose gabapentin trial or a TENS unit test. Continue walks and breathing.
- Week4: Review diary with your clinician. If youre still stuck, discuss a short course of corticosteroid injection or explore acupuncture.
This iterative approach respects your bodys feedbacknothing is set in stone, and you can always adjust.
Conclusion
Finding relief isnt about hunting down one best pain medication; its about piecing together a toolbox that fits your unique story. By understanding medication options, procedural tools, handson therapies, and lifestyle tweaks, youre empowered to make choices that lower pain while keeping safety frontandcenter. Grab the free , start a simple diary, and talk to a trusted healthcare provider about the combo that feels right for you. You deserve comfort, and a thoughtful, balanced plan can get you there.
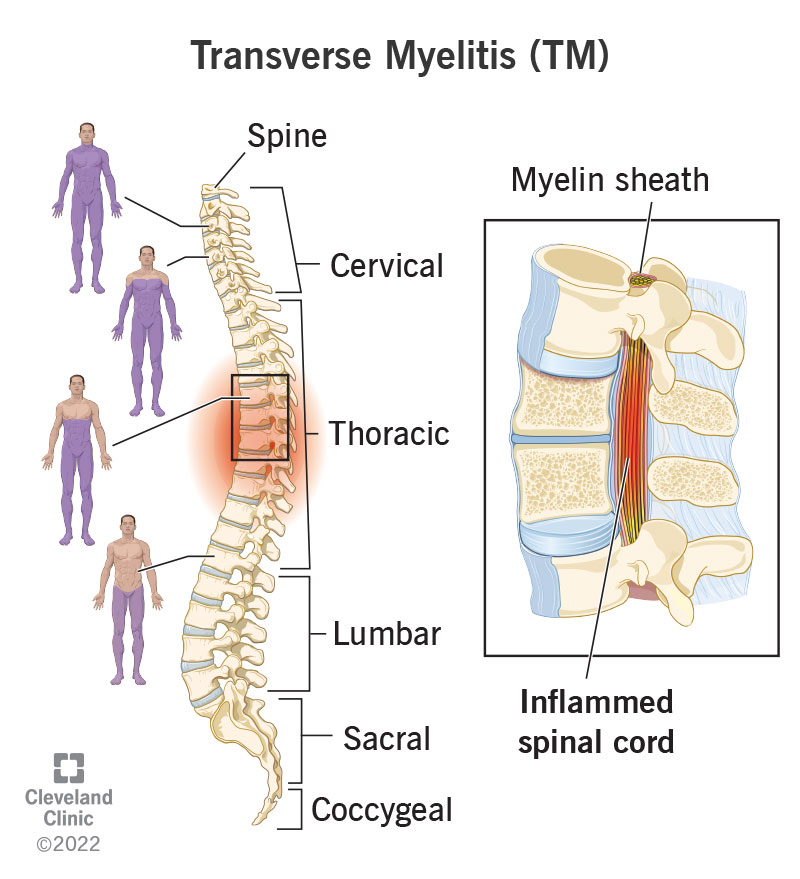
For readers dealing with chronic spinal inflammation or conditions like ankylosing spondylitis, consider reading more on spine inflammation to better understand how inflammation-focused strategies can be integrated into the pain plan above.
FAQs
What are the first steps to take when dealing with mild pain?
Start with over‑the‑counter options like NSAIDs or acetaminophen, apply heat or cold as appropriate, and keep moving gently. If pain persists beyond a few days, consider a short visit to a health professional.
When should I consider seeing a doctor for pain?
Seek medical advice if pain is severe, worsens over time, is accompanied by swelling, fever, numbness, or if you need medication for more than ten days without improvement.
Are over‑the‑counter medications safe for long‑term use?
OTC NSAIDs and acetaminophen are safe for short periods, but prolonged use can affect the stomach, kidneys, or liver. Always follow label directions and discuss extended use with a clinician.
How do non‑drug therapies like TENS or acupuncture help with pain?
These methods stimulate nerves or release the body’s own pain‑relieving chemicals, which can lower the perception of pain without the side‑effects of medication. Results vary, so try them alongside other strategies.
Can lifestyle changes actually reduce chronic pain?
Yes—regular low‑impact exercise, weight management, balanced nutrition, proper sleep, and stress‑reduction techniques such as mindfulness have been shown to lessen inflammation and improve pain tolerance.