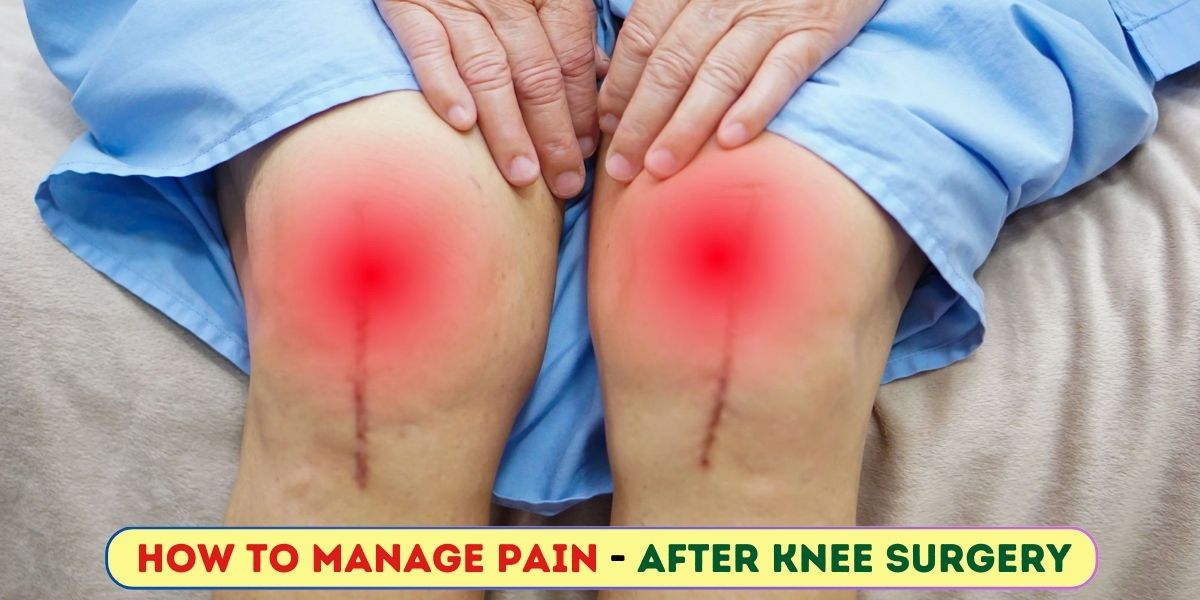
Hey there, youve just had a knee replacement and the ache feels like a stubborn guest that wont leave. Lets cut to the chase: some soreness in the first weeks is completely expected, but a sharp, relentless pain or new swelling after a couple of months is a red flag that deserves a quick call to your surgeon or physiotherapist. Below youll find everything you need to tell the difference, manage the discomfort, and keep your recovery on track.
Quick Answers Guide
Is any pain after knee replacement normal?
Short answer: yes, but only up to a point. During the first six to eight weeks its typical to feel an ache, some swelling, and occasional nighttime throbbing. Think of it like a bruise that needs time to fade. By the third month most patients report a noticeable drop in pain intensity.
When should I be alarmed?
Any of these signs should make you pick up the phone:
- Fever over 38C (100.4F)
- Rapidly increasing swelling or redness
- Sharp, stabbing pain that doesnt improve with rest or medication
- Sudden loss of range of motion
- Unexplained drainage from the incision
These symptoms can point to infection, nerve irritation, or a mechanical problem with the implant.
How long does normal pain usually last?
Heres a quick timeline you can keep on your fridge:
| Phase | Typical Pain Level (VAS 010) | What to Expect |
|---|---|---|
| 02Weeks | 68 | Sharp ache after therapy, moderate swelling |
| 26Weeks | 45 | Steady decrease, more comfortable walking |
| 612Weeks | 23 | Residual stiffness, occasional night pain |
| >12Weeks | 02 | Most patients painfree, occasional whatwasthat? moments |
If youre still hitting a 5 or higher after three months, its time for a professional checkup.
Common Pain Types
Sharp pain on the inside of the knee
This one often gets confused with normal postop soreness. A sharp, localized sting on the medial side can be caused by the implants edge, scar tissue, or irritation of the saphenous nerve. If the pain spikes suddenly during a stretch or after a longer walk, give your surgeon a headsup.
Pain 8months after knee replacement
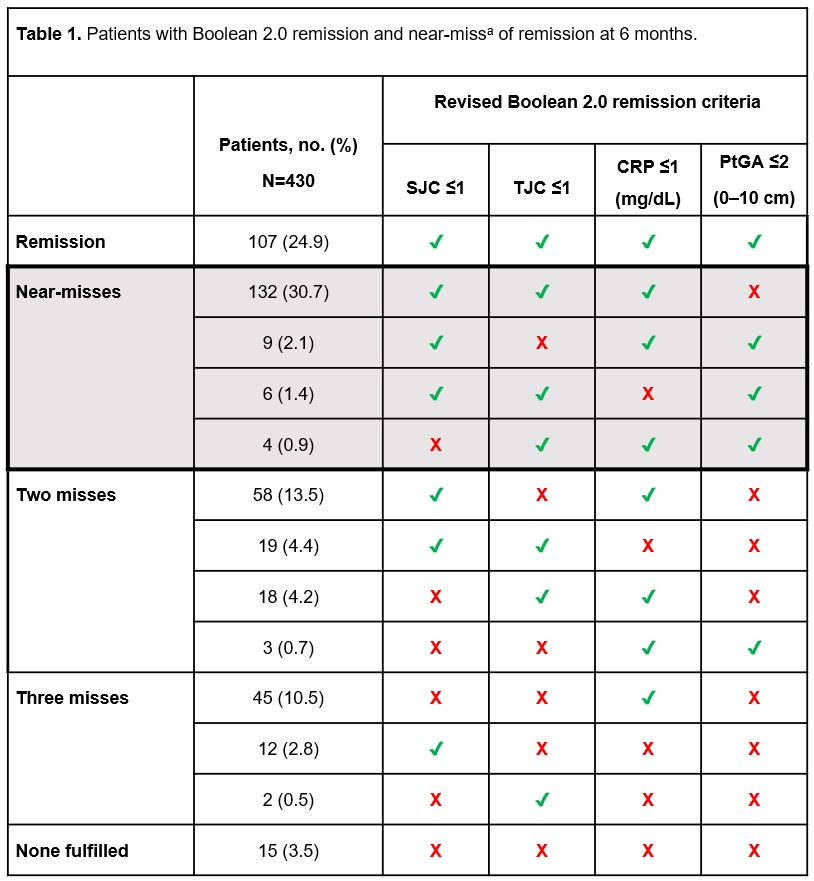
Eight months in, you should be mostly back to normal activities. Persistent pain at this stage may be chronic postsurgical pain (a condition documented in dozens of ankylosing spondylitis remission studies). Common culprits include hidden infection, component loosening, or nerverelated issues.
Total knee replacement pain at night
Nighttime aches can stem from fluid buildup, lingering inflammation, or even the way you position your leg while sleeping. Raising the foot with a small pillow and applying a gentle ice pack for 15 minutes before bed often calms the nighttime flareups.
Upper thigh pain after knee replacement
The quadriceps muscle attaches just above the knee. If youre overusing it too early, or if your hipknee kinetic chain is out of sync, youll feel a sore, sometimes burning sensation up the front of the thigh. Strengthening the quad gently (straightleg raises, seated marches) helps restore balance.
Pain behind the knee
Posterior knee discomfort can be a popliteal tendon irritation, a small Bakers cyst, or even referred pain from the lower back. If the pain is constant and accompanied by a feeling of tightness, an ultrasound or MRI may be recommended.
Why Pain Persists
Inflammation & swelling
After surgery, your body launches a fullblown inflammatory responsethink of it as the construction crew putting up scaffolding. Ice, elevation, and compression are the best tools to keep the scaffolding from becoming permanent.
Scar tissue / arthrofibrosis
When scar tissue builds up excessively, the knee can feel stiff and painful. In severe cases doctors may perform a manipulation under anesthesia to break the adhesions. Osteoporosis exercises notes that early, regular rangeofmotion exercises dramatically cut this risk.
Nerve irritation or neuroma
The saphenous and peroneal nerves run close to the surgical field. If theyre irritated, you might feel burning, tingling, or shocklike sensations. Medications such as gabapentin, topical lidocaine patches, or a TENS unit can bring relief. Osteoporosis physical therapy also recommends gentle nerve gliding exercises under a therapists guidance.
Component malalignment or loosening
Even a tiny shift in the implant can create uneven pressure and pain. Xray or CT scans will reveal if the hardware has moved. If loosening is confirmed, a revision surgery may be necessary.
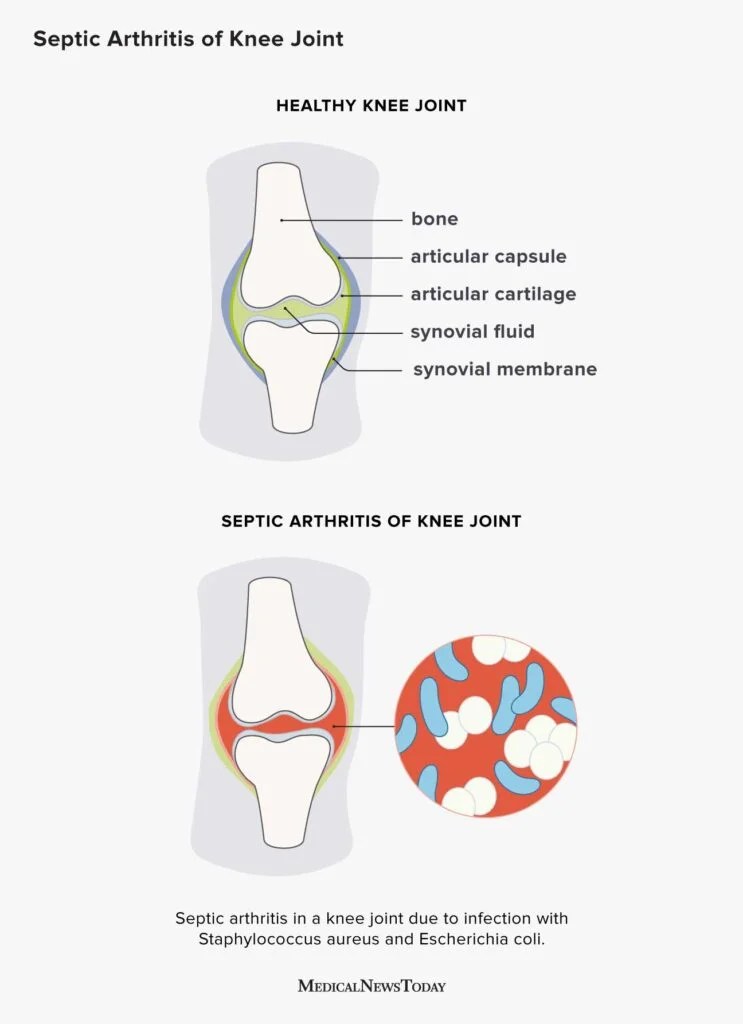
Infection
Even a lowgrade infection can hide behind vague aches. Look out for fever, redness, or unusual drainage. The CDC advises prompt treatment with antibiotics and possible surgical cleaning.
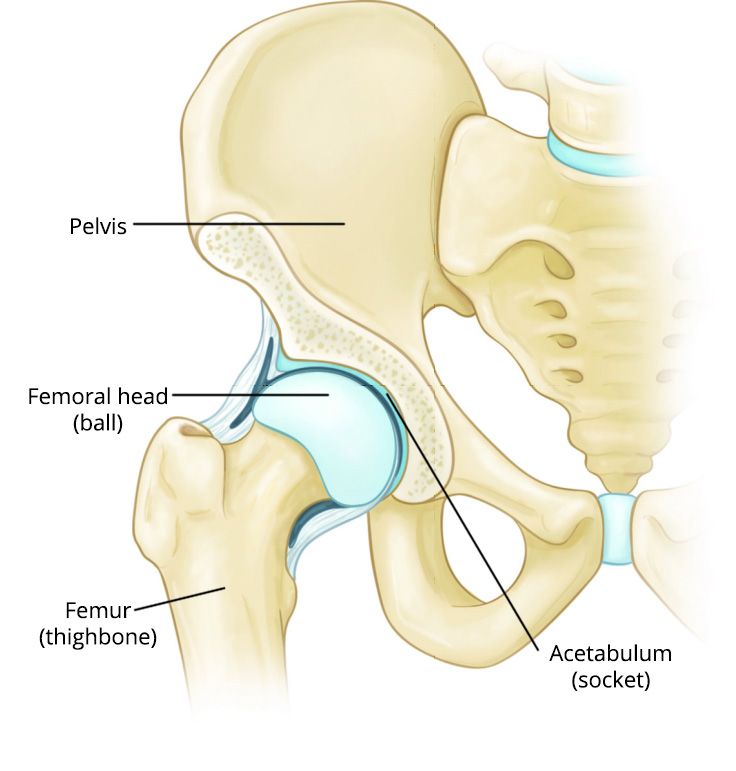
Referred pain from hip or spine
The lower back and hip share nerves with the knee. Sometimes an irritated lumbar disc or hip arthritis masquerades as knee pain. Simple screening questionslike does bending forward hurt more?can help pinpoint the true source.
Pain Recovery Timeline
02Weeks Immediate postop
Expect a pain level of 68 on the VAS scale. Pain meds (acetaminophen plus a short opioid bridge) are common. Ice for 20 minutes, three times a day, keeps swelling at bay.
26Weeks Early recovery
Swelling starts to subside; youll notice a steady decline in pain. Physical therapy focuses on gentle range of motion and weightbearing as tolerated.
612Weeks Medium term
Most patients report a quiet kneestill a little sore after long walks, but no constant throbbing. Light cardio (stationary bike, swimming) is encouraged.
>12Weeks Late recovery
By now you should be comfortable with daily activities. Any pain persisting above a 2 on the VAS scale warrants a followup.
>6Months Persistent pain
If pain sticks around beyond six months, its considered chronic. At this stage, a comprehensive evaluation (labs, imaging, nerve studies) is essential.
Top 5 Mistakes
1. Ignoring prescribed PT
Skipping physiotherapy is like refusing to water a sprouting plantyoull stunt the healing process.
2. Overdoing highimpact activities too soon
Running before your quadriceps are ready can overload the new joint. Stick to a graduated activity ladder: walking cycling light jogging.
3. Skipping painmanagement meds
Missing doses allows inflammation to flare, prolonging recovery. Set reminders on your phone to keep the schedule consistent.
4. Not reporting redflags
Its just a little swelling can sometimes mask an infection. Use the template email below to quickly inform your surgeon:
Subject: PostOp Concern Possible Red FlagHi Dr. [Name],Im experiencing increasing swelling and sharp pain on the inside of my knee, especially after my morning walks. Theres no fever, but the discomfort has been worsening over the past 48hours.Could we schedule a quick evaluation?Thank you,[Your Name]
5. Neglecting overall health
Nutrition, sleep, and hydration are silent partners in healing. Antiinflammatory foods (berries, fatty fish, leafy greens) and 78hours of sleep each night help tissue repair.
Pain Management Tips
Medication basics
Start with acetaminophen (5001000mg every 6hours) and a short course of NSAIDs if your doctor approves. Opioids should be tapered as soon as the pain permits.
Physicaltherapy protocols
Key exercises:
- Quad sets tighten the thigh muscle for 5second holds.
- Straightleg raises build strength without stressing the joint.
- Calf pumps improve circulation and reduce swelling.
Videos from reputable orthopedic centers can guide you safely.
Cold/Heat therapy
Ice is your friend for the first two months (15minute sessions, 34 times daily). After week six, alternating with gentle heat (warm towel) can ease muscle stiffness.
What helps nerve pain after knee replacement
Gabapentin, topical lidocaine patches, and a daily 15minute TENS session have shown relief in many patients. Always discuss dosage with your prescriber.
Sleep & nighttime comfort
Elevate the foot with a small pillow, avoid crossing legs, and perform a brief stretch (heel slides) before bed. A cool, dark bedroom also reduces inflammationinducing cortisol spikes.
Mindbody tools
Deepbreathing, guided meditation, or a short journaling habit can lower pain perception. The brains pain pathways are surprisingly pliable.
When to consider advanced interventions
If pain persists despite conservative measures, discuss these options with your surgeon:
- Corticosteroid injection to quell stubborn inflammation.
- Nerve block for targeted relief.
- Revision surgery for component issues.
Helpful Resource Links
For deeper dives, these trusted sites keep their information uptodate:
Conclusion
Recovering from a knee replacement is a marathon, not a sprint. A little ache is normal, but sharp, persistent, or worsening pain is your bodys way of saying stop and check. By staying informed, following your therapists plan, and listening to redflag signs, youll give your new joint the best chance to shine. Have you experienced any of these pain patterns? Share your story in the comments or reach out to your care teamyour experience could help someone else on the same road.
FAQs
What amount of pain is normal after a knee replacement?
During the first 6‑8 weeks it’s typical to feel a moderate ache (VAS 4‑6), some swelling and occasional night‑time throbbing. Pain should steadily decline and be ≤2 on the VAS scale after three months.
When should I contact my surgeon about knee pain?
Call your surgeon if you notice any red‑flag signs: fever >38°C, rapidly increasing swelling or redness, sharp stabbing pain that doesn’t improve with rest or medication, loss of range of motion, or unexplained drainage from the incision.
How can I reduce swelling and pain at home?
Apply ice for 15‑20 minutes 3‑4 times daily, keep the leg elevated above heart level, use compression wraps, and perform gentle range‑of‑motion exercises as prescribed by your physiotherapist.
Why does pain sometimes appear months after surgery?
Late‑onset pain can stem from hidden infection, implant loosening, scar tissue (arthrofibrosis), nerve irritation, or referred pain from the hip or lower back. An evaluation with labs and imaging is usually required.
What treatments are available for persistent post surgery knee pain?
Options include a course of NSAIDs or short‑term opioids, targeted corticosteroid injections, nerve blocks, TENS therapy, gabapentin for neuropathic pain, and in severe cases revision surgery to address component issues.