Quick Answer
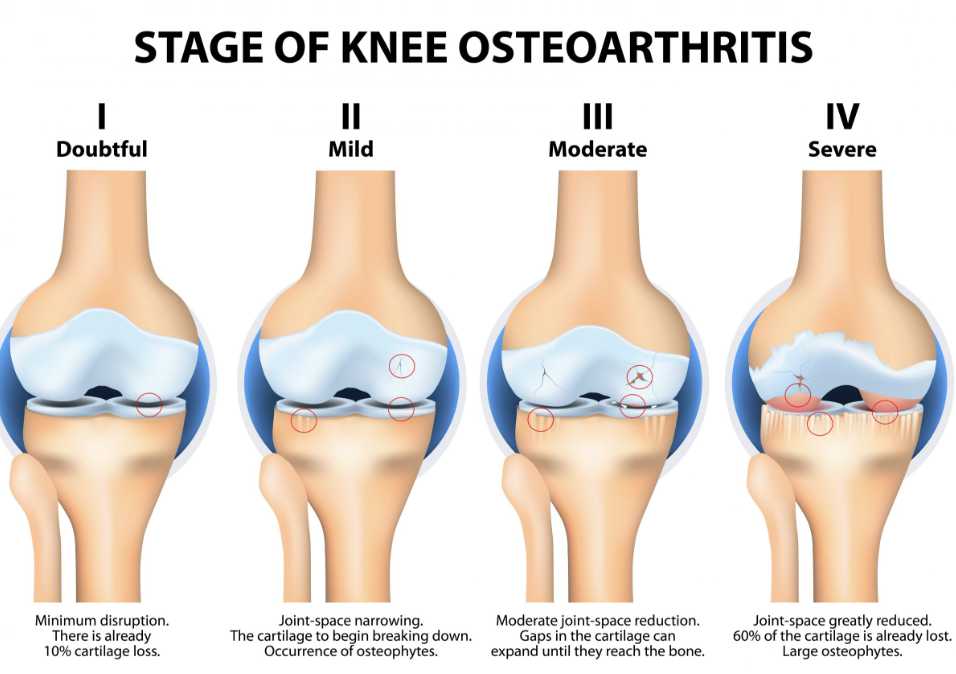
Stage1 Minor (early): Tiny cartilage cracks, occasional stiffness, no clear changes on Xray.
Stage2 Mild: Small osteophytes start to appear, jointspace narrowing is subtle, pain after activity.
Stage3 Moderate: Noticeable cartilage loss, daily aches, limited range of motion, moderate Xray changes.
Stage4 Severe (endstage): Boneonbone contact, severe pain, functional loss; often needs joint replacement.
This snapshot is exactly what Google loves for a featured snippetstraight, concise, and right on point.
Why It Matters
Understanding the four stages isnt just academic; its practical. Imagine youre at a crossroads: keep ignoring the pain and hope it fades, or take a proactive step that could slow the disease. The benefits of stagespecific knowledge are crystal clear:
- Targeted treatment: Early stages respond well to lifestyle tweaks and gentle exercises, while stage4 may require surgery.
- Avoiding over or undertreatment: Misreading the stage can lead to unnecessary medication or, worse, delayed surgery when its truly needed.
- Peace of mind: Knowing exactly where you stand takes the guesswork out of doctor visits.
From my own family, Ive seen both sides. My aunt brushed off her knee pain for years, calling it just arthritis. By the time she finally got an Xray, she was already at stage3, needing a knee replacement. On the flip side, a friend of mine caught her hand OA at stage1 during a routine checkup; she changed her typing posture, kept a healthy weight, and never progressed beyond mild symptoms.
Doctor Classification
Clinical Criteria
Clinicians first listen to your story: how often does the pain appear? How long does it linger? Theyll also check your joints range of motion and look for swelling. Pain scales (010) and functional questionnaires (like the WOMAC) help guide the stage assessment.
Imaging Criteria (Osteoarthritis stages Xray)
Radiographs are the gold standard for visualizing cartilage loss. Most doctors use the KellgrenLawrence grading system, which essentially maps onto the four stages were discussing:
| Stage | JointSpace Width | Osteophytes | Other Features |
|---|---|---|---|
| 1 Minor | >4mm (normal) | None or tiny | Possible mild subchondral sclerosis |
| 2 Mild | 24mm | Small, peripheral | Early narrowing, minimal cysts |
| 3 Moderate | <2mm | Medium, multiple | Significant sclerosis, cyst formation |
| 4 Severe | Boneonbone | Large, bridging | Joint deformity, extensive subchondral changes |
These visual clues give doctors a reliable way to confirm what youre feeling, and theyre what youll see when you search osteoarthritis stages Xray online.
JointSpecific Nuances
While the fourstage framework stays the same, each joint has a unique flavor. Heres a quick cheatsheet you can bookmark:
- Hands: Early OA shows up in the distal interphalangeal (DIP) joints; nodules (Heberdens) appear at stage2.
- Hip: Look for femoral head flattening and narrowing of the joint space on AP pelvis Xray; stage3 often brings groin pain.
- Knee: Classic jointspace narrowing on lateral view; stage4 is when you might feel the grinding sensation.
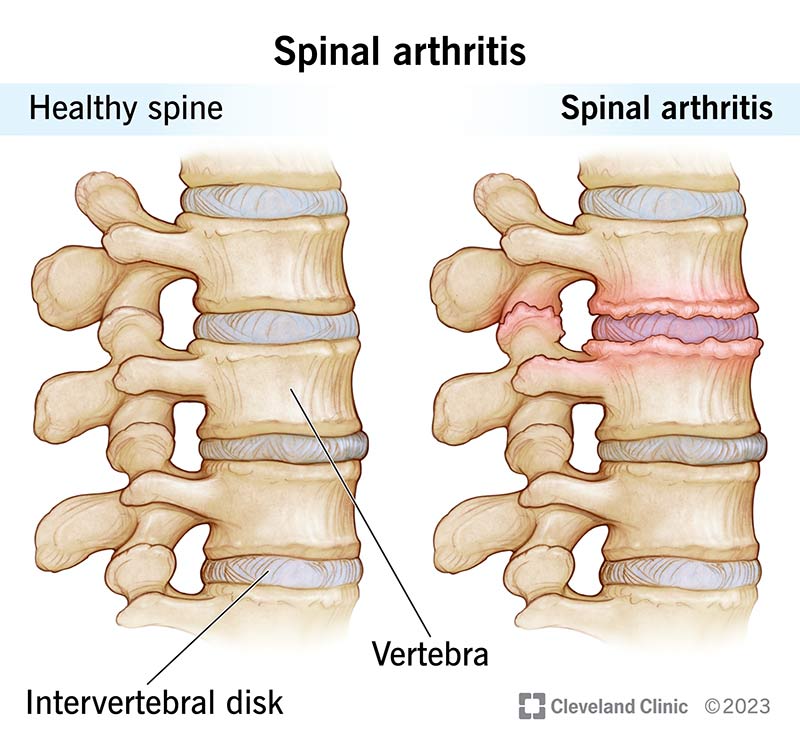
- Spine: Osteophytes (bone spurs) form on the vertebral margins; stage3 often causes reduced flexibility and night pain.
- Shoulder: The humeral head may develop a cystic appearance; stage4 can limit overhead activities dramatically.
Stage Deep Dive
Stage1 Minor (Early)
What you feel: Occasional stiffness that melts away after a few minutes of movement. Pain is rare and usually only after intense activity.
What doctors see: No radiographic changes, but MRI may reveal tiny fissures in the cartilage.
Best moves:
- Light, lowimpact cardio (walking, swimming).
- Strengthening the surrounding musclesthink gentle quad sets and hand grips.
- Weight management; even a 5% bodyweight loss can reduce knee load dramatically.
Stage2 Mild
What you feel: Pain after a walk or after typing for a while. You might notice a faint crepitus (a crackling sound) when you move the joint.
What doctors see: Small osteophytes lining the joint edges, slight narrowing on Xray.
Best moves:
- Introduce a structured physiotherapy programfocus on range of motion and gentle resistance.
- Consider overthecounter NSAIDs (ibuprofen or naproxen) for flareups, but discuss longterm use with a doctor.
- Supplements like glucosamine or vitamin D may help, though evidence is mixedtalk to your GP.
Stage3 Moderate
What you feel: Daily aches, morning stiffness that lasts under 30 minutes, and a noticeable reduction in activities you lovelike gardening or playing with grandkids.
What doctors see: Jointspace narrowing less than 2mm, larger osteophytes, subchondral sclerosis, and possible cysts.
Best moves:
- Professional physiotherapy with modalities such as ultrasound or TENS for pain relief.
- Intraarticular injectionscorticosteroids for shortterm flare control, or hyaluronic acid for joint lubrication.
- Bracing or orthotics to offload the affected joint (especially for knee OA).
Stage4 Severe (EndStage)
What you feel: Constant pain that wakes you at night, severe swelling, and an inability to perform basic tasks (walking, dressing, cooking). The joint may feel gritty as bone rubs on bone.
What doctors see: Boneonbone contact, large bridging osteophytes, extensive joint deformity.
Treatment options (Stage4 Osteoarthritis Treatment):
- Joint replacement surgery: Total knee, hip, or shoulder arthroplasty is the most definitive solution.
- Joint fusion: Usually reserved for ankle or smaller joints when replacement isnt feasible.
- Comprehensive painmanagement program: Includes opioids (as a last resort), nerve blocks, and multidisciplinary rehab.
- Assistive devices: Walkers, canes, and custom shoe inserts to improve mobility.
Practical Tools
SelfAssessment Checklist
Print this PDF (link below) and mark the bullet that best describes your symptoms. If you check more than one item in stage2 or higher, its time to schedule a professional evaluation.
Imaging Guide (Infographic)
Visual learners, rejoice! This simple infographic walks you through what to look for on a standard Xray at each stageperfect when you sit with your radiologist.
Trusted Sources
When to Seek Professional Help
Even with stage knowledge, some redflag signs demand immediate medical attention:
- Sudden, severe swelling that doesnt improve within 48 hours.
- Night pain that wakes you up more than once a night.
- Rapid loss of joint functionlike being unable to stand from a chair.
- Signs of infection (fever, warmth, redness).
If any of these show up, call your GP right away. During the appointment, expect a thorough physical exam, possibly new Xrays, and a candid discussion about stagespecific treatment paths.
Conclusion
The four stages of osteoarthritisminor, mild, moderate, and severeserve as a roadmap that can empower you to take the right steps at the right time. By recognizing the signs early, using accurate imaging, and following stageappropriate treatments, you can keep pain in check, maintain mobility, and reserve surgery for when it truly becomes necessary. Remember, youre not alone on this journey; doctors, physiotherapists, and countless people living well with OA are ready to help. osteoporosis physical therapy programs often share many rehabilitation principles useful for OA patients, especially when focusing on strength and balance. What stage do you think youre in? Share your experience in the comments below, or drop a questionlets keep the conversation going and support each other toward healthier joints.
FAQs
What are the 4 stages of osteoarthritis?
The four stages are minor, mild, moderate, and severe, each with increasing cartilage loss and symptoms.
What happens in stage 1 osteoarthritis?
Stage 1 involves minor wear and tear, with little pain and no clear changes on X-ray.
What are common symptoms in stage 2?
Stage 2 brings mild pain, stiffness after activity, and small bone spurs visible on imaging.
How is stage 3 osteoarthritis different?
Stage 3 features noticeable cartilage loss, daily aches, limited motion, and moderate X-ray changes.
What defines stage 4 osteoarthritis?
Stage 4 means severe pain, bone-on-bone contact, and often requires joint replacement surgery.
Can osteoarthritis be reversed?
No, but early treatment can slow progression and manage symptoms effectively.
What treatments are used for each stage?
Treatments range from lifestyle changes and medication in early stages to surgery in severe cases.