Did you know that a single injection every few weeks can cut your asthma attacks by more than half? If youve been wrestling with daily inhalers, steroids, or constant flareups, monoclonal antibody asthma treatments might be the gamechanger youve been waiting for.
What Are Monoclonal Antibodies?
Definition and Simple Science
Think of monoclonal antibodies as custommade lock picks that jam the specific doors an overactive immune system tries to open in your lungs. Instead of a blanket suppression like steroids, these labsgrown proteins zero in on the culpritsIgE, interleukin5 (IL5), IL4, or IL13blocking the alarm that triggers inflammation.
Why They Matter for Severe Asthma
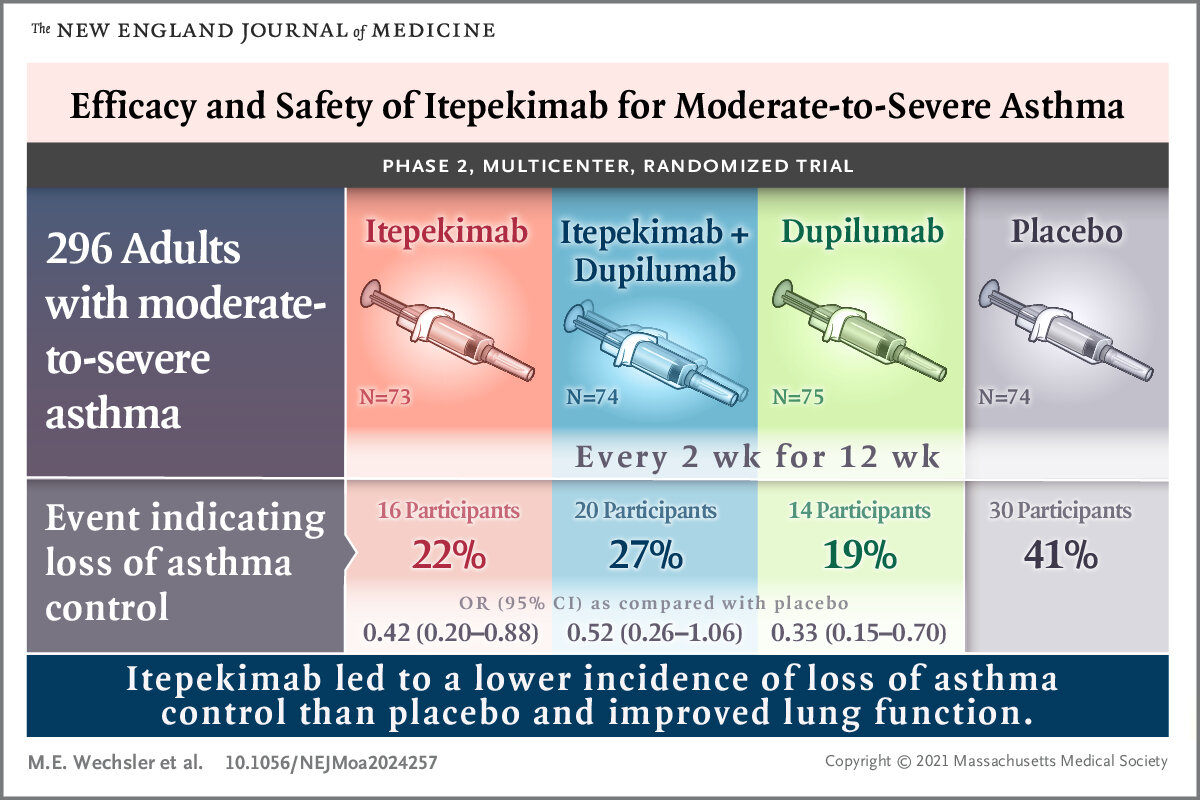
For people with moderatetosevere asthma, standard inhalers often arent enough. Studies show that more than 60% of patients on monoclonal antibody therapy experience fewer emergency visits and a noticeable dip in daily symptoms. In short, they give you back time that would otherwise be spent reaching for your rescue inhaler.
Quick List of Approved Options
Heres a rapidfire rundown of the drugs youll hear about in clinics:
- Omalizumab antiIgE
- Mepolizumab antiIL5
- Reslizumab antiIL5 (IV)
- Benralizumab antiIL5R
- Dupilumab antiIL4R (blocks IL4 & IL13)
Who Is Eligible?
Clinical Thresholds
Most guidelines agree that youre a candidate when youve had at least two severe exacerbations in the past year or youre on daily oral steroids (5mg prednisolone) and your blood eosinophils are 150cells/L or higher.
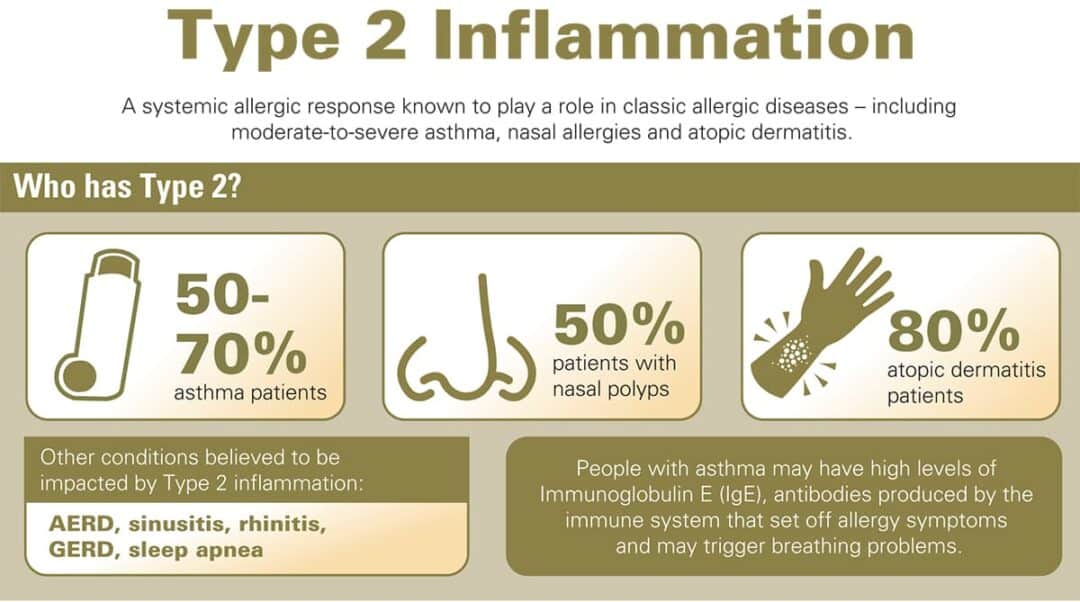
Phenotype Matching
Allergic asthmacharacterized by high IgE levelsusually responds best to omalizumab. On the other hand, eosinophilic asthma (lots of eosinophils in the blood) tends to improve dramatically with drugs that target IL5 or its receptor, such as benralizumab or mepolizumab. Your allergist will run a few simple blood tests and maybe a skin prick test to pin down the right flavor. For those interested in comparing airway management among other respiratory diseases, learning about different airway clearance methods can provide insight into the approaches used for conditions like cystic fibrosis and bronchiectasis.
Patient & Physician Checklist
If youre thinking about a biologic, make sure you have these items ready for your next appointment:
- Recent spirometry results
- Blood eosinophil count
- Allergy test outcomes (if available)
- Medication diary (how many inhaler puffs per day?)
- Insurance preauthorization paperwork
Approved Drugs Compared
| Drug | Target | Route / Dosing | Age Approved | Key Benefits | Common Sideeffects |
|---|---|---|---|---|---|
| Omalizumab | IgE | Subcutaneous 150300mg every 24weeks | 6years | Reduces allergydriven attacks | Injectionsite pain, headache |
| Mepolizumab | IL5 | Subcutaneous 100mg every 4weeks | 6years | Steroidsparing effect | Headache, back pain |
| Reslizumab | IL5 | IV 3mg/kg every 4weeks | 18years | Rapid eosinophil drop | Infusion reactions |
| Benralizumab | IL5R | Subcutaneous 30mg every 4weeks (first 3 doses) then every 8weeks | 12years | Nearcomplete eosinophil depletion | Sore arm, nasopharyngitis |
| Dupilumab | IL4R (IL4/13) | Subcutaneous 300mg loading then 300mg every 2weeks | 6years | Improves both asthma & atopic dermatitis | Conjunctivitis, eosinophilia |
Mechanistic Highlights
Each drug blocks a different signal that tells your lungs to swell. AntiIgE (omalizumab) stops the allergy alarm before it even rings. AntiIL5 agents (mepolizumab, reslizumab, benralizumab) silence the traffic that brings eosinophils into the airway. Dupilumab, meanwhile, shuts down two pathways (IL4 and IL13) that drive both inflammation and mucus production. These pathways are also important in chronic respiratory conditions; understanding cystic fibrosis airway clearance provides context for why mucus clearance and immune modulation matter.
RealWorld Evidence
According to a 2023 review in the American Journal of Medicine, patients on benralizumab saw a 71% reduction in severe exacerbations after one year of therapy. Those numbers help turn the abstract idea of biologics work into something you can actually see on a chart.
Key Benefits Explained
Fewer Attacks, Fewer ER Trips
Across multiple trials, monoclonal antibody asthma treatments cut severe exacerbations by 4565%. Thats the difference between a night spent in the emergency department and a peaceful nights sleep.
SteroidSparing Power
Longterm oral steroids can wreak havoc on bone density, mood, and blood sugar. Many patients on biologics can trim their daily prednisolone dose from 20mg down to 5mgor even stop altogetherwithout losing control.
QualityofLife Boost
Validated questionnaires like the Asthma Control Questionnaire (ACQ) and the Asthma Quality of Life Questionnaire (AQLQ) consistently show doubledigit improvements after just three months of therapy. In plain English? You can run, climb stairs, or simply breathe without pausing for a puff.
A Quick Story
Maria, a 34yearold graphic designer, was on 15mg of oral steroids daily and still wheezed at night. After starting benralizumab, her steroid dose dropped to 2.5mg within two months, and the nighttime wheeze vanished. I finally feel like I own my life again, she told her pulmonologist.
Potential Risks Listed
Mild, Common Sideeffects
Most people notice only mild soreness at the injection site, occasional headache, or a brief sore throat. These usually fade within a day or two.
Rare but Serious Events
Very rarely, patients develop anaphylaxis or a condition called eosinophilic granulomatosis with polyangiitis (EGPA). Because these are uncommon, most clinicians will monitor blood counts and lung function regularlyjust to be safe.
Monitoring Recommendations
Before you start, expect a baseline CBC (complete blood count) and spirometry. Followup labs every three months help catch any unexpected changes early. Your specialist will guide you on when to call the office (for example, if you develop a persistent rash or joint pain).
Balancing Act
The good news? For the vast majority, the benefits outweigh the risks. The key is a shared decisionmaking conversation with a qualified allergist or pulmonologist, where you weigh your personal health goals against the possible sideeffects.
Cost & Access Guide
Price Snapshot
In the United States, annual list prices range from $25,000 to $35,000, while in Australia and the UK the outofpocket cost can be dramatically lower thanks to national health coverage. Remember, list price isnt what youll actually payinsurance, copays, and manufacturer assistance programs shrink the bill.
Insurance Pathways
Most private plans require prior authorization. Medicare PartD covers many of these drugs, and many pharmaceutical companies run copayassist programs that can reduce your outofpocket expense to under $100 per month.
PatientAssistance Options
Look for Patient Assistance Programs on the drugs official website. These often provide free medication for qualifying lowincome patients or those without insurance.
CostBenefit Comparison
If an uncontrolled severe asthma patient averages two ER visits a year at $5,000 each, plus daily inhaler costs, the biologics price can actually be a financial win in the long run. A simple spreadsheet can illustrate the breakeven pointsomething many clinics are happy to help you calculate.
Starting Treatment Steps
Get a Specialist Referral
Youll need a pulmonologist or an allergist who can order the necessary labs and submit the insurance paperwork. Dont be shyask for a biologics evaluation when you book your appointment.
Baseline Workup
Bring recent spirometry reports, a full medication list, and any allergy test results. Your doctor will also draw blood to check eosinophils and IgE levels. Additionally, some specialists may recommend therapies such as chest physiotherapy techniques in individuals with overlapping airway clearance issues or chronic mucus production.
Choosing the Right mAb
Imagine a decision tree:
If you have high IgE omalizumab.
If eosinophils >300cells/L consider benralizumab or mepolizumab.
If you also have eczema dupilumab.
First Appointment Experience
Most clinics give a quick demo on how to selfinject (if youre on a subcutaneous drug). The nurse will watch you do a practice dummy injection, then youll leave with a prefilled pen and a simple schedule. It feels a bit like learning to ride a bikeawkward at first, but soon youre cruising.
Quick Reference Table
| Drug | Phenotype | Typical Dose Interval | Annual Cost (US) |
|---|---|---|---|
| Omalizumab | Allergic | Every 24weeks | $30,000 |
| Mepolizumab | Eosinophilic | Every 4weeks | $28,000 |
| Benralizumab | Eosinophilic | Every 4weeks (first 3), then every 8weeks | $32,000 |
| Dupilumab | Type2 (asthma+eczema) | Every 2weeks | $35,000 |
Wrapping It All Up
Monoclonal antibody asthma therapies have turned a oncehopeless situation into a manageable, even thriving, reality for many. They cut attacks, let you ditch highdose steroids, and give you a clearer view of the skyfree of wheezefilled clouds. At the same time, they come with price tags, insurance hurdles, and a handful of sideeffects youll want to watch. The sweet spot is a candid conversation with an asthma specialist who can match your phenotype to the right biologic, line up the paperwork, and guide you through the first injection.
If youve ever felt trapped by your inhaler schedule, consider reaching out to your doctor about whether a monoclonal antibody might be right for you. Have you tried one already? What was your experience? Share your story in the comments, and lets keep the conversation goingbecause breathing easy is something we all deserve.
FAQs
Who qualifies for monoclonal antibody asthma treatment?
Patients with moderate‑to‑severe asthma who have had ≥ 2 severe exacerbations in the past year or who require daily oral steroids (≥ 5 mg prednisolone) and have blood eosinophils ≥ 150 cells/µL are typical candidates.
How are the injections administered and how often?
All approved biologics are given subcutaneously except reslizumab, which is IV. Dosing ranges from every 2 weeks (omalizumab) to every 8 weeks after the loading phase (benralizumab). Most treatments are self‑administered at home after an initial clinic visit.
What are the most common side effects?
Injection‑site pain, mild headache, and occasional sore throat are the most frequent. Rare but serious events include anaphylaxis and eosinophilic granulomatosis with polyangiitis, so regular monitoring is advised.
Do these biologics reduce the need for oral steroids?
Yes. Clinical trials show a 50‑80 % reduction in daily oral‑steroid dose for many patients, and a substantial proportion can stop steroids altogether while maintaining asthma control.
How can I afford the high cost of monoclonal antibody therapy?
Most insurance plans require prior authorization, and many pharmaceutical companies offer copay‑assist or patient‑assistance programs that can lower out‑of‑pocket costs to under $100 per month for eligible patients.