Ever caught yourself thinking that the occasional wheeze is just a bad day for your lungs? I used to, toountil a doctor explained that my breathlessness was actually driven by type2 inflammation in asthma. That tiny phrase turned my whole treatment plan upside down.
Knowing exactly what type2 inflammation in asthma looks like helps you and your clinician pick the right medicines, avoid unnecessary sideeffects, and finally feel a bit more in control of those sudden attacks.
Understanding the Basics
Definition what is type2 inflammation in asthma?
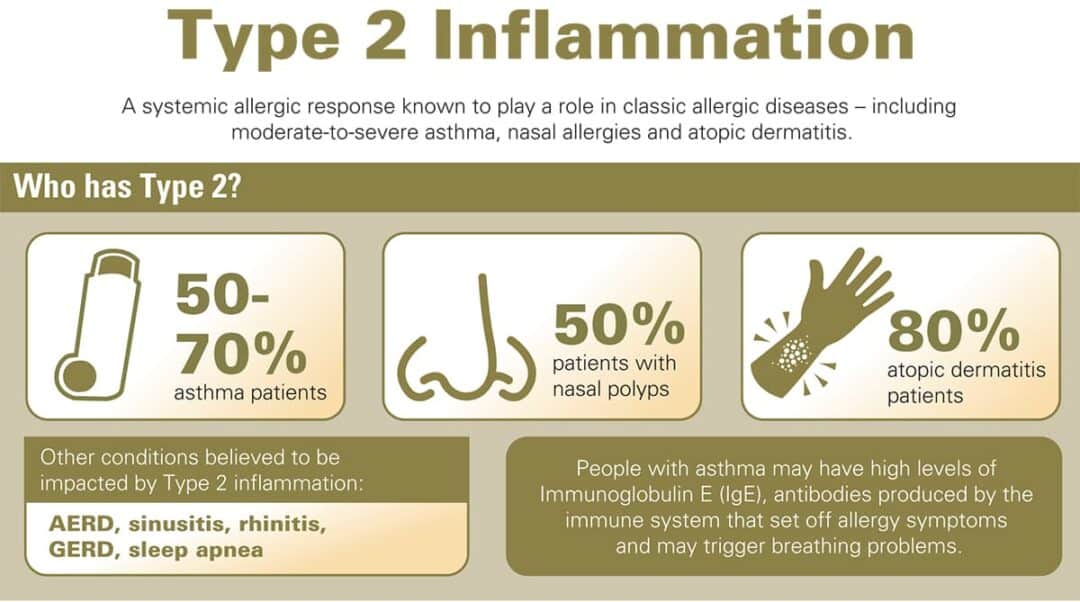
In plain language, type2 inflammation is a specific immune response that makes the airways extrasensitive and swollen. Its driven by a group of immune cellsmainly Th2 lymphocytes, eosinophils, and mast cellsthat release cytokines such as IL4, IL5, and IL13. These chemicals tell the body to produce more IgE antibodies and recruit eosinophils, the badboy white blood cells that love to cause trouble in the lungs.
The immune players eosinophils, mast cells, Th2 cells & cytokines
If you picture your immune system as a neighborhood watch, the Th2 cells are the overenthusiastic volunteers who keep ringing the alarm bell for anything that looks even slightly allergyy. Their favorite calls are IL4 (which tells Bcells to make IgE), IL5 (which recruits eosinophils), and IL13 (which drives mucus production). The eosinophils then flood the airway walls, releasing enzymes that irritate tissue and narrow the passages.
Visual aid simple diagram of the type2 pathway
Consider adding a quick sketch: allergens Th2 cells IL4/5/13 eosinophils & IgE airway swelling. A graphic like this (credit an openaccess source) makes the cascade crystal clear for visual learners.
Quick fact box Did you know?
5070% of people with asthma show a type2 signature according to the Allergy & Asthma Network. That means most of us could benefit from tailored therapies if we know we belong to this group.
Type 2 vs Type 1
Core differences in immune response
While type2 relies on Th2 cytokines, type1 inflammation follows a Th1 pathway, dominated by interferon (IFN) and neutrophils. Think of type1 as the firefighter response that attacks viruses and intracellular bugs, whereas type2 is the allergyalarm that overreacts to harmless particles.
Clinical presentation what you feel
People with type2 asthma often notice:
- Wheezing that worsens at night or early morning
- Frequent coughing after exposure to pollen, pet dander, or dust mites
- Quick improvement when using inhaled corticosteroids (ICS)
In contrast, type1driven asthma tends to be more dry less mucus, more bronchial hyperresponsiveness to viral infections, and a weaker response to typical steroids.
Comparison table type2 inflammation vs type1 inflammation asthma
| Feature | Type2 Inflammation | Type1 Inflammation |
|---|---|---|
| Key cytokines | IL4, IL5, IL13 | IFN, TNF |
| Dominant cells | Eosinophils, mast cells | Neutrophils, macrophages |
| Typical triggers | Allergens, highIgE environments | Viral infections, irritants |
| Blood markers | Elevated eosinophils, FeNO | Normal eosinophils, sometimes elevated CRP |
| Preferred meds | Biologics (e.g., Dupilumab), ICS | Macrolides, highdose steroids |
| Prevalence | ~5070% of asthmatics | ~3040% of asthmatics |
Expert quote
According to Dr. Laura Chen, a boardcertified allergist, Identifying a type2 phenotype early lets us intervene with targeted biologics before patients endure years of uncontrolled symptoms.
What Triggers It
Allergens & environmental exposures
Pollen, dustmites, pet dander, and even mold spores are the classic culprits. When these particles land in the airway, they interact with IgE on mast cells, setting off the whole type2 chain.
Viral infections & microbiome shifts
Recent research published in the European Respiratory Journal notes that certain viral infections can tilt the immune balance toward a Th2dominant state, especially in children whose microbiome is still developing.
Genetic & epigenetic factors
Family history matters. Genes like IL33 and TSLP have been linked to an overactive type2 response. Even lifestyle factorslike diet and exposure to pollutantscan switch genes on or off, nudging the immune system toward inflammation.
Realworld case study
Maria, a 28yearold graphic designer, moved from a lowpollen Midwest town to a coastal city with heavy ragweed season. Within weeks she noticed nightly coughing and tighter chest. Blood work revealed a high eosinophil count, confirming a type2 pattern. After adjusting her environment and starting a biologic, her symptoms dropped dramatically.
Symptoms & Diagnosis
Hallmark symptoms of type2driven asthma
Typical red flags include:
- Nighttime wheeze or cough that disrupts sleep
- Rapid response to inhaled steroids
- History of allergic rhinitis, eczema, or food allergies
Biomarkers youll hear about
Doctors often order:
- Blood eosinophil count a value >300 cells/L usually points to type2
- Fractional exhaled nitric oxide (FeNO) high levels indicate airway inflammation driven by IL13
- Total IgE elevated in many allergic patients
Type2 inflammation blood test what the results mean
A typical report might look like this:
Eosinophils: 420cells/L (Reference<300), FeNO: 55ppb (Reference<25), IgE: 210IU/mL (Reference<100). Those numbers suggest a robust type2 response and make you a candidate for targeted therapy.
Sample lab report walkthrough
When you receive the report, focus on three things: (1) absolute eosinophil count, (2) FeNO reading, and (3) any notes about eosinophilic phenotype. Your physician can then match you with the right medication ladder.
Treatment Options Overview
Standard inhaled corticosteroids (ICS) why they work
ICS dampen the whole inflammatory cascade, lowering cytokine production and easing airway swelling. Theyre the firstline for most asthma patients and work especially well for type2 inflammationbut theyre not a cure.
Biologic therapies that target type2 pathways
These are the gamechangers:
- Mepolizumab (antiIL5) reduces eosinophil production.
- Dupilumab (IL4R blocker) blocks both IL4 and IL13, helping a wide range of allergic conditions.
- Benralizumab (antiIL5R) leads to rapid eosinophil depletion.
- Tezepelumab (TSLP inhibitor) works upstream, potentially effective even in mixed phenotypes.
According to a 2022 JACI study, patients on Dupilumab saw a 60% reduction in exacerbations compared with standard care.
Natural & lifestyle adjuncts
While nothing replaces prescription meds, certain lifestyle tweaks can soothe the type2 fire:
- Omega3rich foods (salmon, walnuts) modestly lower eosinophil activity.
- VitaminD supplementation especially in winter months when levels dip.
- Allergenproof bedding and HEPA air filters cut exposure at the source.
- Regular aerobic exercise improves lung capacity and reduces overall inflammation.
Pros & cons table type2 inflammation treatment options
| Option | Pros | Cons |
|---|---|---|
| Inhaled Corticosteroids | Widely available, inexpensive, effective for many | May cause oral thrush, voice hoarseness; longterm systemic effects at high doses |
| Biologics (e.g., Dupilumab) | Targeted; reduces severe attacks; improves quality of life | High cost; injections every 24 weeks; insurance hurdles |
| Omega3 / VitaminD | Easy dietary changes; low risk | Effects are modest; need consistent intake |
Expert commentary
Dr. Ahmed Patel, a pulmonology fellow, often reminds patients, Watch your eosinophil trend. If it drops below 150cells/L after a biologic, youre likely on the right track.
Balancing Benefits & Risks
Why identifying a type2 phenotype matters
When you know you have a type2 pattern, you can skip the trialanderror stage and jump straight to therapies that actually target your disease. That means fewer ER visits, less reliance on rescue inhalers, and more afternoons spent playing with the kids instead of worrying about breathlessness.
Potential pitfalls overdiagnosis, sideeffects, insurance hurdles
Sometimes clinicians label anyone with mild eosinophilia as type2, leading to unnecessary biologic prescriptionsa costly mistake. Also, biologics can cause injectionsite reactions or, rarely, allergic responses. And lets not forget the paperwork: navigating insurance approval can feel like climbing a mountain.
Patient story Marias journey from generic inhalers to a dupilumab plan
Marias doctor initially prescribed highdose fluticasone, but her symptoms persisted. After a detailed blood test revealed a eosinophil count of 480cells/L, she qualified for Dupilumab. Within three months, her nighttime cough vanished, and she finally felt the breath of relief shed been missing for years.
Practical Action Steps
Talk to your doctor
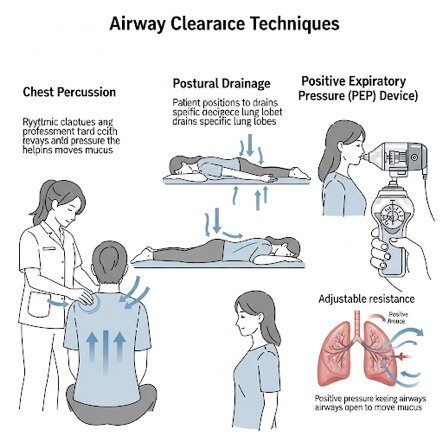
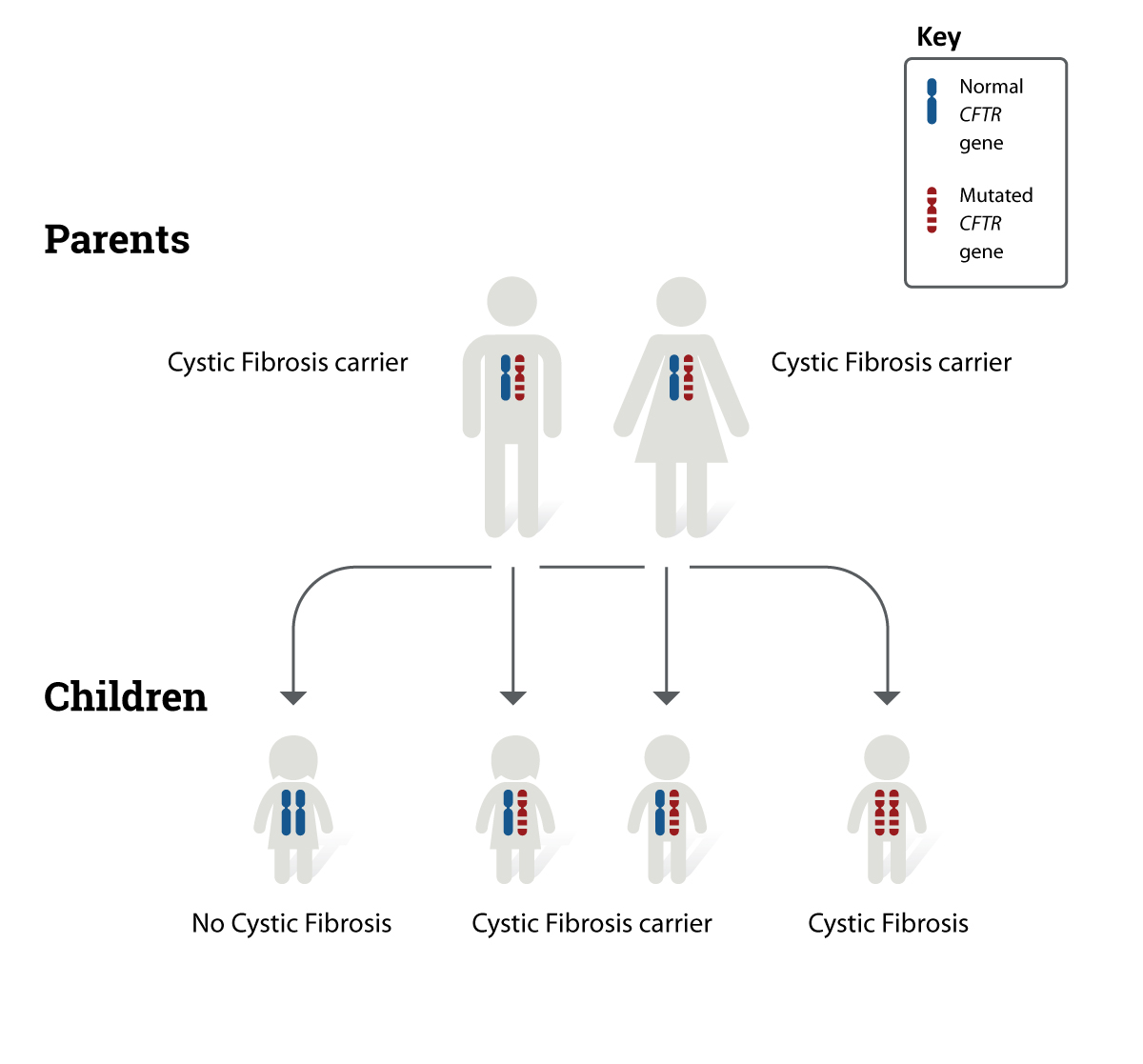
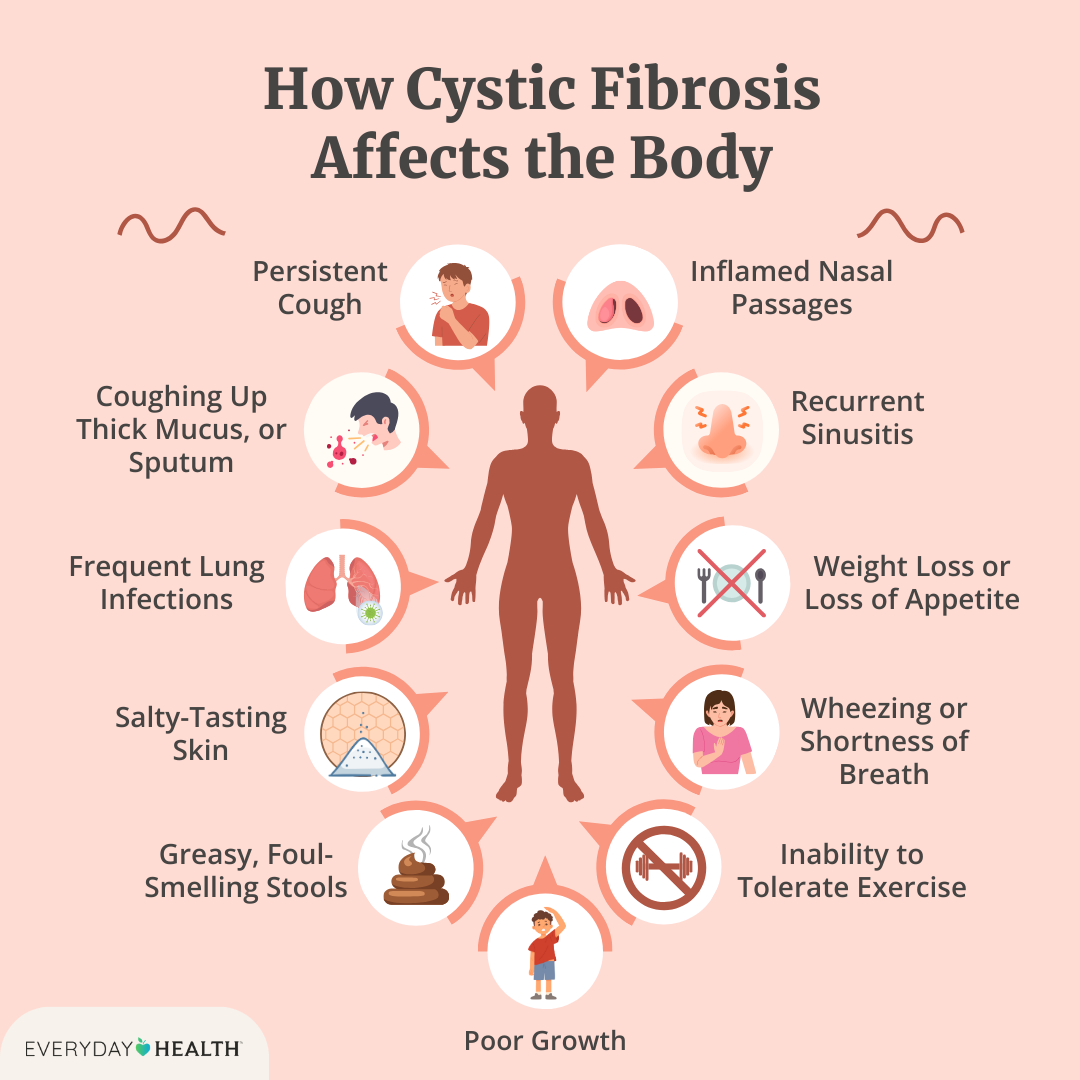
Ask specifically: Can we check my eosinophil count and FeNO to see if I have a type2 phenotype? Knowing the numbers empowers you to make informed decisions. If you or a family member also live with chronic lung conditions like cystic fibrosis, discussing how therapies and airway clearance strategies interact can be helpful; for more on managing relationships and care in that setting see cystic fibrosis relationships.
Lifestyle tweaks
- Keep indoor humidity below 50% to deter mold.
- Use HEPA filters in bedrooms and living rooms.
- Add fatty fish or a highquality fishoil supplement three times a week.
- Track triggers in a simple notebook or phone apppatterns become obvious quickly.
Quickaction checklist
| 1 Review recent labs (eosinophils, FeNO) |
| 2 Note any recent allergen exposures |
| 3 Schedule a followup to discuss targeted therapy options |
Conclusion
Understanding what type2 inflammation in asthma really means can be a turning point in how you breathe, sleep, and live each day. Its more than a labelits a roadmap that points to the right tests, the most effective medicines, and lifestyle tweaks that actually matter. If you recognize the signs, ask about eosinophils and FeNO, and stay open to both medical and natural strategies, youll be much better equipped to keep asthma under control. Feel free to share your own story or ask questionstogether we can turn confusing jargon into practical, everyday confidence.
FAQs
What is type 2 inflammation in asthma?
Type 2 inflammation in asthma is an immune response involving eosinophils, mast cells, and Th2 cells, leading to airway swelling and increased mucus.
What are common symptoms of type 2 inflammation in asthma?
Symptoms include frequent coughing, wheezing, shortness of breath, and disrupted sleep, often worsening at night or after allergen exposure.
How is type 2 inflammation in asthma diagnosed?
Doctors use blood tests for eosinophils, FeNO breath tests, and IgE levels to identify type 2 inflammation in asthma.
What treatments target type 2 inflammation in asthma?
Treatments include inhaled corticosteroids, biologics like Dupilumab and Mepolizumab, and lifestyle changes to reduce triggers.
Can type 2 inflammation affect other conditions?
Yes, type 2 inflammation is linked to conditions like eczema, nasal polyps, and chronic urticaria, often seen alongside asthma.