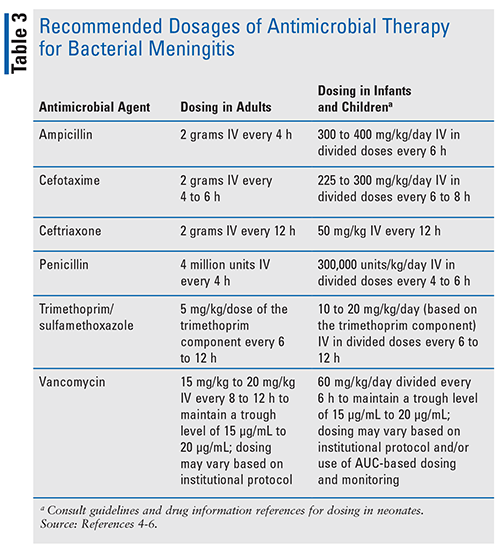
When meningitis strikes, the right medication can mean the difference between a full recovery and a prolonged battle. The drug of choice for meningitis depends on age, the likely pathogen, and local resistance patterns. For most adults its a thirdgeneration cephalosporinampicillin; for children the same drugs are used with weightbased dosing, plus special considerations for neonates.
Below youll find the exact regimens, why theyre recommended, alternatives when resistance is an issue, and how to balance benefits versus sideeffectsall in plain language you can act on right now.
Quick Reference Guidelines
What do the latest IDSA/CDC meningitis treatment guidelines recommend?
Both the 2024 IDSA and 2023 CDC guidelines emphasize a thirdgeneration cephalosporin as the backbone of therapy. In adults, ceftriaxone (2g IV every 12h) is paired with ampicillin (50mg/kg IV every 6h) to coverListeria. In children, cefotaxime (50mg/kg IV every 6h) plus vancomycin (15mg/kg IV every 6h) is standard.
Where can readers download the full guidelines (PDF)?
You can grab the complete directly from the CDC website, and the IDSA recommendations are available in their document.
How do lowresistance regions differ?
In areas where extendedspectrum betalactamase (ESBL) producers are rare, the simple ceftriaxone+ampicillin regimen works well. If local antibiograms show higher resistance, clinicians may add meropenem or TMPSMX as backup options.
Adult Drug Choice
Which antibiotic is firstline for bacterial meningitis in adults?
The goto drug is a thirdgeneration cephalosporinmost often ceftriaxone. It reaches therapeutic levels in the cerebrospinal fluid (CSF) and covers the usual suspects like Streptococcus pneumoniae and Neisseria meningitidis. The typical dose is 2g IV every 12hours, infused over 30minutes.
When is ampicillin added?
Ampicillin comes into play when theres a risk for Listeria monocytogenesthink patients over 50, the immunocompromised, pregnant women, or anyone with a history of Listeria exposure. The dosing is 50mg/kg IV every 6hours (max 2g per dose).
What are the key alternatives if resistance is suspected?
If cultures hint at a resistant strain, you might switch to meropenem (2g IV every 8hours) for broad Gramnegative coverage, or add TMPSMX (10mg/kg IV every 6hours based on the trimethoprim component) for Listeria when ampicillin cant be used.
Oral stepdown options after IV stabilization?
Once the patient stabilizes and CSF cultures are negative, an oral highbioavailability agent can be considered. Fluoroquinolones like levofloxacin (750mg PO daily) or amoxicillin (2g PO every 8hours) are sometimes used, but always check susceptibility first.
Child & Neonate Choices
Firstline regimen for children>1month old
Kids get cefotaxime (50mg/kg IV every 6hours) and vancomycin (15mg/kg IV every 6hours) to cover both typical bacteria and penicillinresistant strains. Dosing is weightbased, so its essential to doublecheck the childs current weight before calculating.
Neonatal (028days) considerations
Newborns are a special case. The classic combo is ampicillin (50mg/kg IV every 12hours) plus gentamicin (5mg/kg IV every 24hours). If Gramnegative rods dominate, cefotaxime can replace gentamicin to avoid nephrotoxicity.
Weightbased dosing calculators
There are free online tools that let you plug in a childs weight and instantly get the correct dose. A quick search for pediatric meningitis dosing calculator will point you to reputable medical sites that host these calculators.
Oral stepdown for kids is it safe?
Evidence from pediatric trials shows that after 48hours of IV therapy, children can often be switched to oral cefdinir (7mg/kg once daily) if theyre improving and the organism is susceptible. Always confirm with the treating physician.
Special Situations & Adjuncts
Tuberculous meningitis drug regimen & duration
TB meningitis requires a fourdrug regimen (isoniazid, rifampin, pyrazinamide, ethambutol) for at least two months, followed by a continuation phase of isoniazid and rifampin for 710months. Its a long haul, but early treatment is crucial.
Viral meningitis when antivirals are indicated
Most viral meningitis cases are selflimiting, but if HSV or VZV is suspected, start acyclovir 10mg/kg IV every 8hours promptly.
Steroid use (dexamethasone) dosage, timing, evidence
Dexamethasone (0.15mg/kg IV every 6hours, max 10mg) administered before or with the first antibiotic dose can reduce inflammation and improve outcomes, especially in<50yearold adults with pneumococcal meningitis.
Allergy management desensitization vs. switching class
If a patient has a penicillin allergy, you can either desensitize under ICU supervision or switch to a thirdgeneration cephalosporin with a different sidechain, depending on the severity of the allergy.
Doxycycline & TMPSMX Options
Doxycycline meningitis dose (including doxycycline meningitis dose keyword)
Doxycycline can be used when other agents are unsuitable. The recommended dose is 100mg PO or IV every 12hours; it penetrates the CSF reasonably well, especially when the meninges are inflamed.
TMPSMX (Bactrim) indications (e.g., penicillin allergy, Listeria coverage)
Trimethoprimsulfamethoxazole at 10mg/kg IV every 6hours (based on the trimethoprim portion) is a solid fallback for Listeria or as a secondline agent when lactams cant be used.
Safety checklist renal adjustment, photosensitivity, drugdrug interactions
Both doxycycline and TMPSMX can cause photosensitivity, so advise patients to avoid prolonged sun exposure. Adjust TMPSMX dose for renal impairment (eGFR<30mL/min) and watch for interactions with warfarin or certain antiretrovirals.
Risks, Benefits, Monitoring
How to monitor therapeutic response (CSF cultures, clinical scores)
Repeat lumbar puncture 2448hours after starting therapy to check CSF sterility. Track fever curves, mental status, and seizure activity. Tools like the Glasgow Coma Scale help quantify neurologic improvement.
Common adverse effects per drug class (nephrotoxicity, hepatotoxicity, seizures)
Cephalosporins are generally safe but can cause cholestatic liver injury in rare cases. Aminoglycosides like gentamicin are notorious for nephro and ototoxicityregular renal labs and audiograms are a must. Doxycycline may cause esophageal irritation if not taken with water.
When to switch or stop therapy lab thresholds & clinical cues
If CSF cultures turn negative after 48hours and the patient is afebrile for at least 24hours, you can consider stepping down to oral therapy or shortening the IV course. However, always complete the minimum recommended duration (typically 710days for most bacterial meningitis).
Practical Tools & Tables
| Drug | Typical Dose | Route | Age Group | Key Sideeffects |
|---|---|---|---|---|
| Ceftriaxone | 2g | IV q12h | Adults | Gallstones, biliary sludge |
| Ampicillin | 50mg/kg | IV q6h | Adults + Neonates | Allergic rash, renal |
| Cefotaxime | 50mg/kg | IV q6h | Children | Hepatotoxicity (rare) |
| Vancomycin | 15mg/kg | IV q6h | Children | Nephro/ototoxicity |
| Doxycycline | 100mg | PO/IV q12h | All ages (except <8y) | Photosensitivity, GI upset |
| TMPSMX | 10mg/kg (trimethoprim) | IV q6h | All ages | Kidney injury, hyperkalemia |
ResistanceAlert Checklist
Before you start, glance at your hospitals antibiogram:
- Is ESBL prevalence >10%? Consider meropenem.
- Any recent carbapenemresistant isolates? Add TMPSMX.
- Penicillin allergy documented? Use ceftriaxone doxycycline.
Final Takeaway
For most adults and children, a thirdgeneration cephalosporin+ampicillin (or vancomycin for kids) remains the evidencebased drug of choice for bacterial meningitis; alternatives exist for resistant strains or specific allergies. Balancing effectiveness with potential toxicity, and always tailoring therapy to age, weight, and local resistance patterns, is the key to a successful outcome.
Download the printable , use our dosing table, and dont hesitate to discuss any concerns with your healthcare providerearly, appropriate therapy saves lives.
FAQs
What is the first‑line antibiotic for bacterial meningitis in adults?
The recommended first‑line drug is a third‑generation cephalosporin, most commonly ceftriaxone 2 g IV every 12 hours.
When should ampicillin be added to adult meningitis therapy?
Ampicillin is added when Listeria monocytogenes is a concern—typically in patients over 50, the immunocompromised, pregnant women, or those with known Listeria exposure.
What is the standard pediatric regimen for children older than one month?
Children receive cefotaxime 50 mg/kg IV every 6 hours plus vancomycin 15 mg/kg IV every 6 hours to cover typical organisms and penicillin‑resistant strains.
How are antibiotic doses adjusted for neonates (0–28 days)?
The classic neonatal regimen is ampicillin 50 mg/kg IV every 12 hours combined with gentamicin 5 mg/kg IV daily; cefotaxime can replace gentamicin if Gram‑negative rods dominate.
When is dexamethasone recommended in meningitis treatment?
Dexamethasone 0.15 mg/kg IV every 6 hours (max 10 mg) given before or with the first antibiotic dose can reduce inflammation, especially in adults with pneumococcal meningitis.