Quick answer: Most lung collapses (pneumothorax) show up within the first 24hours after a needle biopsy, but a delayed collapse can sneak in up to 72hours later. If you feel sudden sharp chest pain, shortness of breath, or a new cough anytime in those first three days, call your doctor right away early detection usually means a simple, nonsurgical fix.
Why this matters: A biopsy gives doctors the tissue they need to diagnose cancer or infection, yet the same needle that gives answers can also create a tiny air leak. Knowing the timing, the warning signs, and the steps to protect yourself can turn a scary whatif into a manageable plan.
Why Collapse Happens
What Is a Pneumothorax?
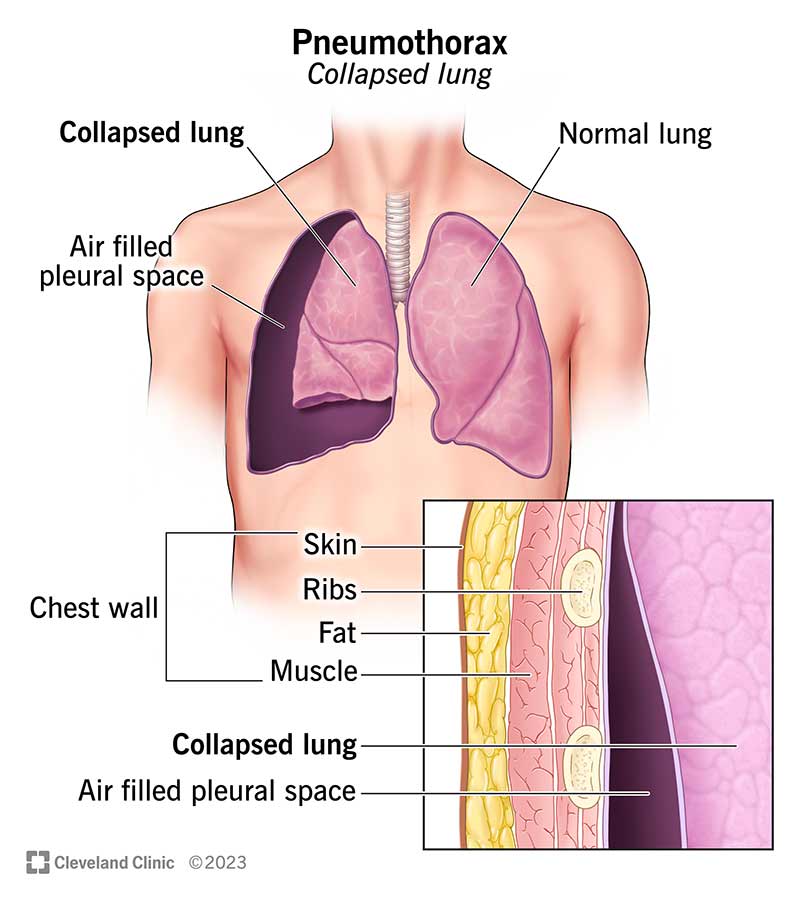
A pneumothorax is simply air that slips into the space between your lung and the chest wall (the pleural cavity). When that air builds up, it pushes the lung flat, making it hard to breathe. A partial collapse might feel like a mild ache, while a complete collapse can feel like an instant pressure bomb.
How the Biopsy Creates an Air Leak
During a transthoracic needle biopsy the doctor threads a thin needle through the chest wall to reach the lung nodule. That needle carves a tiny tunnel; if the tunnel doesnt seal itself, air can escape from the lung into the pleural space. The most common pathways are:
- Needletrack leak the needle leaves a clean channel.
- Alveolar rupture a fragile air sac bursts when the needle pushes through.
Data Snapshot
| Study / Source | % With Pneumothorax | % Requiring Chest Tube |
|---|---|---|
| PMCID3966161 (2023) Pneumothorax after transthoracic needle biopsy | 30% | 510% |
| MedlinePlus (2024) | 28% | 3% |
| Kaiser Permanente (2024) | 33% | 7% |
Timing of Collapse
Immediate (06Hours)
Air that leaks straight away shows up on the first postprocedure chest Xray. Youll probably feel a sudden, stabbing chest pain and rapid breathing. This is why most hospitals keep you under observation for a few hours right after the biopsy.
Early (624Hours)
Even if the first Xray looks clean, a small leak can slowly fill up. Most watchfulwaiting patients are rescanned at around the 12hour mark. If the air pocket is tiny, the lung often reseals itself without any intervention.
Delayed (2472Hours) The Critical Window
This is the period that worries many patients the most. A tiny tear might not let enough air out at first, but as you move, cough, or take deep breaths, the leak can widen. Symptoms that pop up a day or two later a new cough, lightheadedness, or a feeling of tightness often point to a delayed pneumothorax.
Rare LateOnset (>72Hours)
Cases beyond three days are uncommon, but they do happen, especially in people with underlying emphysema or who continue to smoke after the procedure. A handful of case reports describe collapses as late as a week, usually after a vigorous activity or a strong coughing fit.
Risk Factors
PatientSpecific Risks
Age matters. Older adults (70years) tend to have stiffer lungs and less elastic tissue, so a small leak can linger longer. A history of smoking also slows healing; nicotine impairs the tiny blood vessels that would normally seal the needle track.
ProcedureSpecific Details
Using a largergauge needle or making multiple passes increases the chance of an air leak. Lesions located in the upper lobes are a touch riskier because the chest wall is thinner there, giving the needle less cushion.
PostProcedure Behaviors
Smoking after lung biopsy Even a single cigarette can raise the pressure inside your lungs, nudging air out of the tiny tunnel. Studies from the show that patients who smoke within 24hours have a 2fold higher odds of a pneumothorax.
Coughing A violent cough can act like a pressure pump, forcing more air into the pleural space. If you have a lingering cough from a cold, consider a mild cough suppressant (after checking with your doctor) during the first 48hours.
Quick Checklist for Patients
- Dont smoke for at least 24hours (ideally 48hours) after the biopsy.
- Avoid heavy lifting or vigorous exercise for 3days.
- Stay upright; lying flat can encourage air to collect.
- If you notice sudden chest pain, shortness of breath, or a new cough, call your healthcare provider immediately.
What to Do If Your Lung Collapses
Immediate SelfCare (First 24Hours)
Rest on your back with a pillow under your head, and try to breathe shallowly dont force a deep cough. If you have supplemental oxygen prescribed, keep it on. Call emergency services if you feel dizzy, your lips turn blue, or you cant speak full sentences.
Medical Interventions
Most pneumothoraces are observed; the body reabsorbs the air on its own. Only about 510% need a chest tube, which is a thin plastic tube that sucks out the air and lets the lung reexpand. If a tube is placed, the success rate for full reexpansion is around 90%.
In rare, persistent cases surgeons may perform videoassisted thoracoscopic surgery (VATS). According to the , the fiveyear survival after VATS repair of a collapsed lung is over 95% for otherwise healthy adults.
Recovery Timeline After Treatment
| Treatment | Typical Hospital Stay | Full Activity Return |
|---|---|---|
| Observation (no tube) | 02days | 12weeks |
| Chesttube placement | 13days | 24weeks |
| VATS surgery | 25days | 46weeks |
Related Questions People Often Ask
Can a lung biopsy cause cancer to spread?
Current evidence shows that needle biopsies do not increase the risk of tumor seeding in more than 99% of cases. The main concern remains the pneumothorax, not cancer spread.
How long can you live with a collapsed lung?
If untreated, a large pneumothorax can become lifethreatening within hours because the heart and other organs dont get enough oxygen. With prompt medical care, most people recover fully within weeks.
What is the collapsedlung surgery survival rate?
Modern minimally invasive surgery (VATS) boasts a survival rate of over 95% at five years, especially when the patient has no major comorbidities.
Are lung biopsy risks higher for the elderly?
Yes. Patients over 70 experience a slightly higher pneumothorax rate around 35% and they may need a longer observation period. However, the overall outcomes remain excellent when complications are caught early.
Is delayed pneumothorax after lung biopsy common?
Delayed pneumothorax occurs in roughly 5% of cases, most often showing up between 24 and 72hours after the procedure.
RealWorld Stories
Case #1: Immediate Collapse, No Tube Needed
John, 58, a former smoker, felt a sharp ache two hours after his biopsy. A quick Xray showed a 15% collapse. The medical team monitored him, gave supplemental oxygen, and his lung reexpanded on its own after 12hours. He was home the next day, feeling grateful for the early warning signs.
Case #2: Delayed Collapse on Day3, Chest Tube Required
Maria, 72, living with COPD, thought she was fine until the third morning when she woke up short of breath. A repeat Xray revealed a sizeable pneumothorax. A chest tube was placed, and after five days she was discharged with clear instructions on activity restriction. Her experience underscored the importance of staying vigilant during the 72hour window.
How to Reduce Your Risk
Before the Biopsy
- Enroll in a smokingcessation program at least two weeks ahead.
- Use prescribed bronchodilators if you have COPD or asthma.
- Discuss any bloodthinning medications with your doctor; they may be paused.
During the Procedure (Expert Insight)
Interventional radiologists often choose a coaxial needle and limit the number of passes to the smallest amount needed for a diagnostic sample. Realtime CT guidance helps them avoid crossing fissures, which lowers the chance of an air leak.
After the Biopsy
- Ask for a baseline chest Xray immediately after the procedure.
- If youre highrisk (elderly, emphysema, heavy smoker), request a followup Xray at 24hours.
- Follow the no heavy lifting rule for at least three days.
- Stay hydrated and move gently short walks are encouraged, but avoid vigorous activity.
- If you have questions about recovery or related concerns like lung biopsy preparation, discuss them with your care team so you know what to expect before and after the procedure.
Printable PostBiopsy Checklist (download PDF)
Weve prepared a short, printable PDF that lists all the dos and donts for the first 72hours. Keep it on your nightstand so you dont forget anything important.
Conclusion
Understanding that most lung collapses happen within the first 24hours, with a critical watchout period up to 72hours, can turn anxiety into actionable knowledge. A biopsy is a powerful tool that often saves lives, and its risks while real are usually manageable when you know the warning signs and follow simple postprocedure guidelines. Take the steps to quit smoking, avoid heavy exertion, and keep an eye on any new chest symptoms. If anything feels off, reach out to your healthcare team right away. Your lungs have a remarkable ability to heal; with a little vigilance, youll be back to breathing easy in no time.
FAQs
How soon after a lung biopsy can your lung collapse?
Most lung collapses happen within the first 24 hours after a lung biopsy, but a delayed collapse can occur up to 72 hours later.
What are the symptoms of a collapsed lung after biopsy?
Symptoms include sudden sharp chest pain, shortness of breath, new cough, and sometimes lightheadedness or tightness in the chest.
Can a collapsed lung after biopsy heal on its own?
Yes, many small pneumothoraces heal on their own without treatment, but larger collapses may need a chest tube or medical care.
What should I do if I think my lung collapsed after biopsy?
If you have sudden chest pain or trouble breathing, call your doctor or go to the emergency room right away.
How can I reduce my risk of lung collapse after biopsy?
Avoid smoking, heavy lifting, and vigorous activity for at least 72 hours after your biopsy to lower your risk.