Hey there, friend. If youve been feeling your heart pound like a drum after battling COVID19, youre definitely not alone. The short answer? Most folks notice a big improvement within 312months, yet a solid sliceabout 2040%may keep feeling that rapid beat for a year or more. Below, well walk through whats happening, why it matters, and what you can actually do to feel better.
Fast Answer Summary
In a nutshell, postCOVID tachycardia usually eases up within a few months, but the road can stretch out to over a year for some. Early lifestyle tweaks and, when needed, targeted medication can shave weeks or even months off that timeline.
What Is Tachycardia
Definition & Common Types
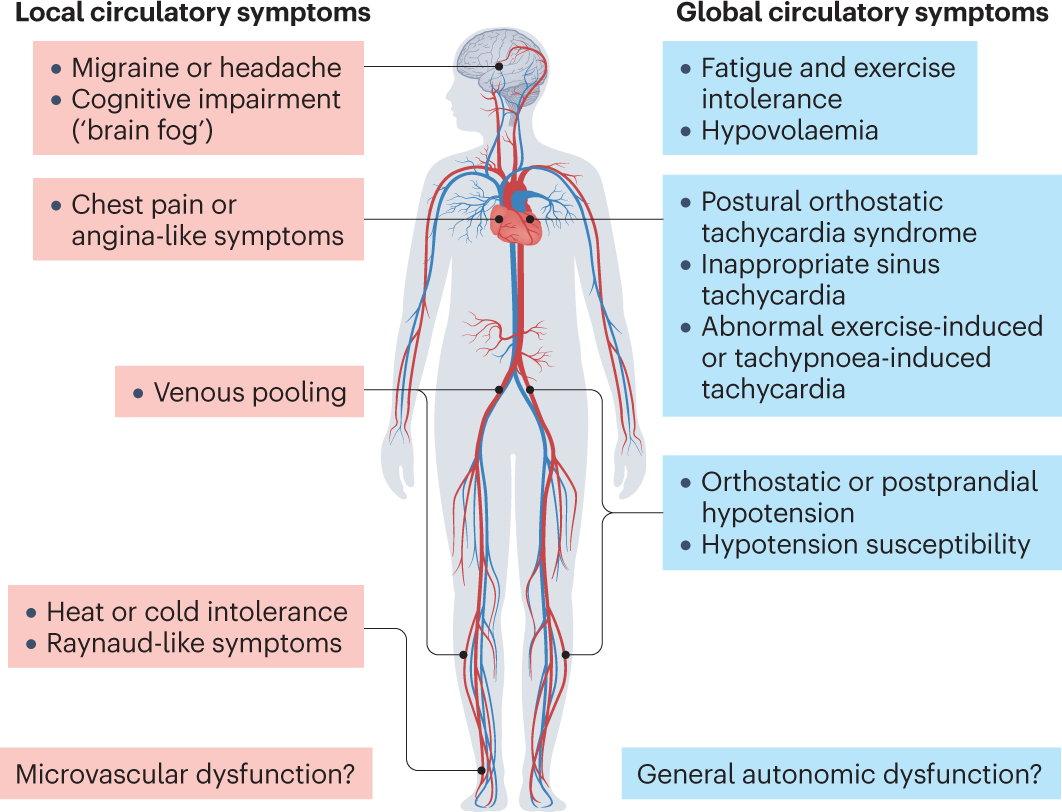
Tachycardia simply means a heart rate thats faster than normalgenerally over 100 beats per minute (bpm) while youre at rest. After COVID, you might see three flavors:
- Sinus tachycardia: the hearts normal pacemaker is racing.
- Inappropriate sinus tachycardia (IST): the rate stays high without an obvious trigger.
- POTS (Postural Orthostatic Tachycardia Syndrome) after COVID: a dramatic jump in heart rate when you stand up.
Why It Happens
The virus can stir up inflammation, poke at the autonomic nervous system, and leave you deconditioned after weeks of bedrest. Think of it like a car thats been parked for monthsit needs a gentle revup before it runs smoothly again. This explains why you might also hear terms like tachycardia during COVID or postviral tachycardia in discussions.
How COVID Triggers It
Researchers believe three main culprits are at play:
- Inflammatory response: cytokines can shortcircuit the hearts rhythm control.
- Autonomic dysfunction: the nerves that tell your heart when to speed up or slow down get confused.
- Physical deconditioning: weeks of reduced activity makes the heart work harder to pump the same amount of blood.
Expert Insight
According to published in Nature (2021), about onethird of patients with lingering symptoms reported persistent tachycardia, underscoring the need for awareness.
Typical Duration Timeline
Average Timeframe
When scientists followed people with postCOVID tachycardia, the median symptom duration landed around 23 weeks (roughly five to six months). In fact, a 2025 analysis of 132 patients found that 75% felt a notable drop in heartrate spikes by the end of the first year.
Comparison Table
| Study | Sample Size | Median Symptom Duration | % Fully Recovered by 12mo |
|---|---|---|---|
| PostCOVID Exertional Tachycardia (2025) | 132 | 23weeks | 75% |
| AAFP Management of POTS after Long COVID | 7080% | ||
| BMJ Review on Orthostatic Tachycardia |
Factors That Stretch the Timeline
Not everyone recovers at the same speed. Things that can keep the tachycardia ticking longer include:
- Preexisting POTS or other autonomic issues
- Older age or severe initial COVID infection
- Low baseline fitness level
- Underlying health conditions such as hypertension or thyroid problems
RealWorld Example
Take Anna, a 34yearold teacher who finished her COVID isolation feeling her heart at 110bpm at rest. She kept a daily log for nine months, noting that gentle walking increased her rate only modestly after the third month. By month ten, her resting rate settled around 85bpm and she could jog again. Stories like Annas are common on threads, where people share timelines, setbacks, and victories.
Spotting Key Symptoms
Common Signs
If your heart is constantly in the fast lane, you might notice:
- Resting pulse >100bpm
- Palpitationslike a fluttering butterfly in your chest
- Dizziness or lightheadedness, especially when standing
- Unexplained fatigue even after short activities
- Occasional chest discomfort (not sharp pain, but a pressure)
RedFlag Situations
Some signals demand immediate medical attention:
- Chest pain that feels crushing or radiates to the arm
- Shortness of breath at rest
- Fainting episodes (syncope)
- Heart rate soaring above 130bpm without exertion
Quick SelfCheck List
Print out this simple checklist (or keep it on your phone) and tick off any items you notice. If three or more show up, its a good idea to book a checkup.
How Its Diagnosed
Clinical Evaluation
Your doctor will start with a thorough historywhen symptoms began, how they fluctuate, what makes them better or worse. A physical exam follows, often paired with a basic ECG (electrocardiogram) to rule out arrhythmias unrelated to COVID.
Diagnostic Tools
- 24hour Holter monitor: captures heartrate trends over an entire day.
- Tilttable test: gold standard for confirming POTS; youre tilted upright while the heart rate is monitored.
- Blood tests: thyroid panel, CBC, and inflammatory markers to exclude other causes.
Clinical Reference
The provides a stepbystep protocol for tilttable testing, which many postCOVID clinics now incorporate.
Effective Treatment Options
Lifestyle First
Before reaching for pills, try these gentle, evidencebacked moves:
- Gradual reconditioning: start with fiveminute walks, add a minute each day. Consistency beats intensity.
- Hydration + Salt: up to 3L of water a day and a pinch of extra salt (if you have no contraindications) can boost blood volume and calm the heart.
- Compression stockings: especially useful for those with orthostatic symptoms.
- Breathing exercises: slow diaphragmatic breathing can activate the parasympathetic nervous system, lowering heart rate.
Medication Options (PostCOVID Tachycardia Treatment)
If lifestyle tweaks arent enough, several drugs have shown promise:
| Medication | Mechanism | Typical Dose | Common Sideeffects |
|---|---|---|---|
| Propranolol | blocker (slows heart) | 1040mg twice daily | Fatigue, cold extremities |
| Ivabradine | Ifchannel blocker (specifically lowers rate) | 57.5mg twice daily | Visual disturbances, mild nausea |
| Midodrine | agonist (raises blood pressure, eases orthostatic rise) | 2.510mg three times daily | Supine hypertension, itching |
Doctors Perspective
We usually start with a lowdose blocker, monitor tolerance, and only add ivabradine if the heart rate stubbornly stays high, says Dr. Maya Patel, an autonomic specialist at a major academic center.
Complementary Therapies
Yoga, mindfulness meditation, and even CBT (cognitivebehavioral therapy) can help manage anxiety that sometimes fuels tachycardia. The mindbody connection isnt a mythstress hormones can spike your heart rate as much as a virus.
Your Recovery Timeline
ShortTerm (03Months)
Expect frequent monitoring. Many people see a 1020% drop in resting heart rate just by staying hydrated and moving a little each day.
MidTerm (312Months)
By the sixmonth mark, a solid majority (>70%) report significant improvement, meaning their daily activities no longer trigger a racing heart. If you havent noticed progress by now, a medication adjustment may be needed.
LongTerm (>12Months)
For the minority whose tachycardia persists beyond a year, chronic management becomes the goal. This often involves a combination of lowdose meds and a refined exercise plan. Keep in mind that long COVID tachycardia can coexist with other lingering symptoms, so a holistic approach works best.
Community Insight
On the community, many users share spreadsheets tracking heart rate, sleep, and activity. Seeing patterns helps them (and their doctors) make smarter treatment tweaks.
Final Key Takeaways
To pull everything together:
- Most people feel a big improvement within 312months, but some may need longer.
- Early lifestyle changeshydration, gentle reconditioning, compressioncan shave weeks off the recovery curve.
- When needed, medications like betablockers or ivabradine are safe and effective under medical supervision.
- Listening to your body, tracking symptoms, and staying in touch with a knowledgeable clinician are the best defenses against a lingering fast heart.
Remember, youre not just a set of numbers on a monitor; youre a whole person navigating a tricky postviral landscape. If youve experienced postCOVID tachycardia, share your story in the commentsyour journey might be the beacon someone else needs. And if you have questions, feel free to ask; were all in this together.
For readers also dealing with swelling or fluid buildup that can accompany heart conditions, consider learning more about heart failure edema as part of a broader recovery plan.
FAQs
How long does post-COVID tachycardia usually last?
Most people experience significant improvement in post-COVID tachycardia within 3 to 12 months, though about 20-40% may have symptoms lasting a year or longer.
What factors can prolong post-COVID tachycardia?
Longer duration is more likely if there are pre-existing autonomic issues like POTS, older age, severe initial COVID illness, lower fitness levels, or underlying conditions such as hypertension or thyroid problems.
What types of tachycardia can occur after COVID-19?
Common types include sinus tachycardia, inappropriate sinus tachycardia (IST), and postural orthostatic tachycardia syndrome (POTS), each differing by heart rate patterns and triggers.
How is post-COVID tachycardia diagnosed?
Diagnosis involves clinical history, physical exam, ECG, 24-hour Holter monitoring, tilt-table testing (especially to confirm POTS), and blood tests to exclude other conditions.
What treatments help with post-COVID tachycardia?
Initial treatment focuses on lifestyle changes like gradual reconditioning, hydration, salt intake, and compression stockings. Medications such as beta-blockers or ivabradine may be prescribed if symptoms persist.