But every treatment has a flip side, and the decision isnt just about numbers. Its about how the sideeffects might feel in your daily life, how long youd be on hormone injections every three months, and whether refusing hormone therapy is an option youre comfortable with. Below, I break down the science, the realworld experience, and the practical questions most men (and their loved ones) ask when they hear radiation+hormone therapy.
Quick Summary
Survival & Disease Control
Large randomized trials consistently report 8year diseasespecific survival around 98% for men who receive both radiation and ADT, compared with roughly 99% for radiation alone in lowrisk groups. The real win shows up in highrisk patients: a 20year study from Harvard Health found a 40% reduction in metastasis when ADT is added.
When It Stops Working
If hormone therapy stops shrinking the tumorwhat doctors call castrationresistant prostate cancerPSA levels start climbing again. At that point, options shift to secondgeneration antiandrogens, chemotherapy, or clinical trials.
SideEffect Snapshot
- Radiation: urinary urgency, mild bowel irritation, temporary erectile dysfunction.
- Hormone therapy: hot flashes, loss of libido, bone thinning, mood changes, and metabolic shifts.
| Outcome | Radiation Alone | Radiation+Hormone Therapy (ADT) |
|---|---|---|
| 8yr diseasespecific survival | 99% | 98% |
| 20yr metastasis risk (highrisk) | 40% | |
| Typical sideeffects | GU irritation, fatigue | Hot flashes, bone loss, sexual changes |
Why Combine Them?
Biology Behind the Duo
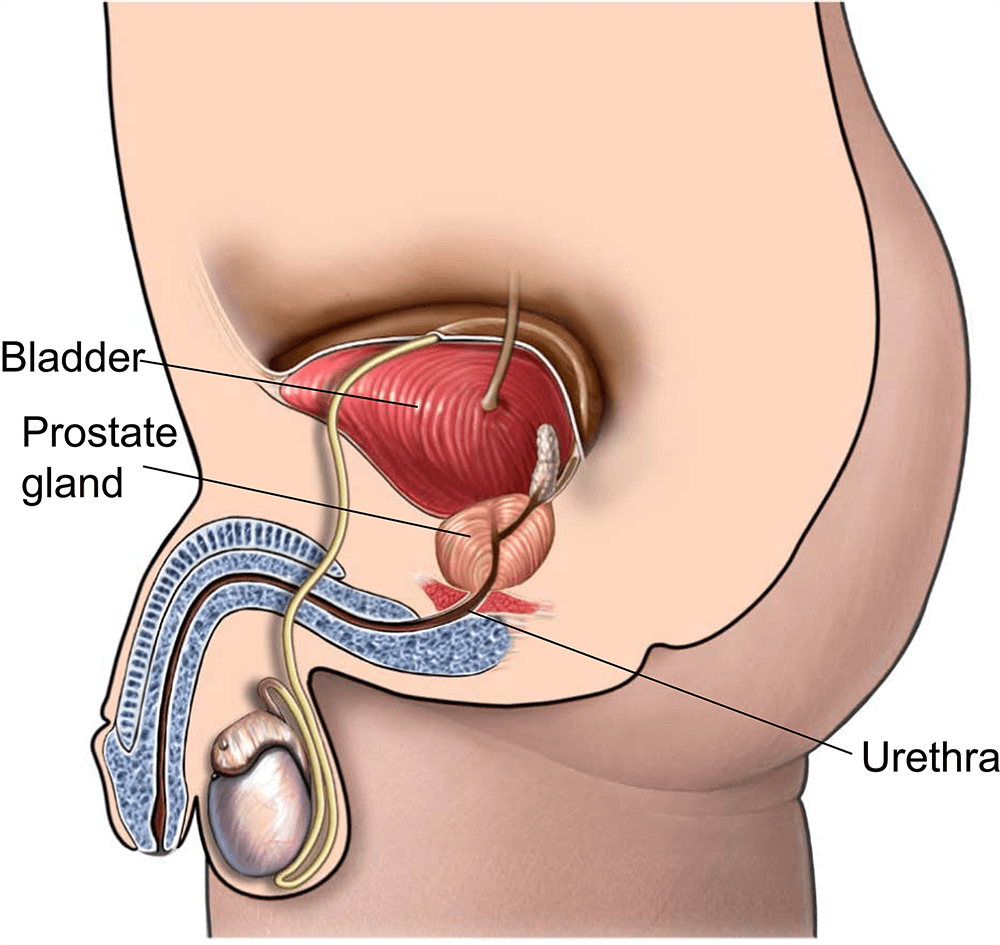
Hormone therapy reduces testosterone, which in turn shrinks the tumor and makes cancer cells more vulnerable to radiation. Think of it like dimming the lights before you take a photothe radiation (the flash) hits a less defended target.
Evidence from Trials
One landmark trial () followed men for eight years and confirmed the survival boost. Another longterm analysis from Harvard (, 2025) highlighted the metastasis reduction.
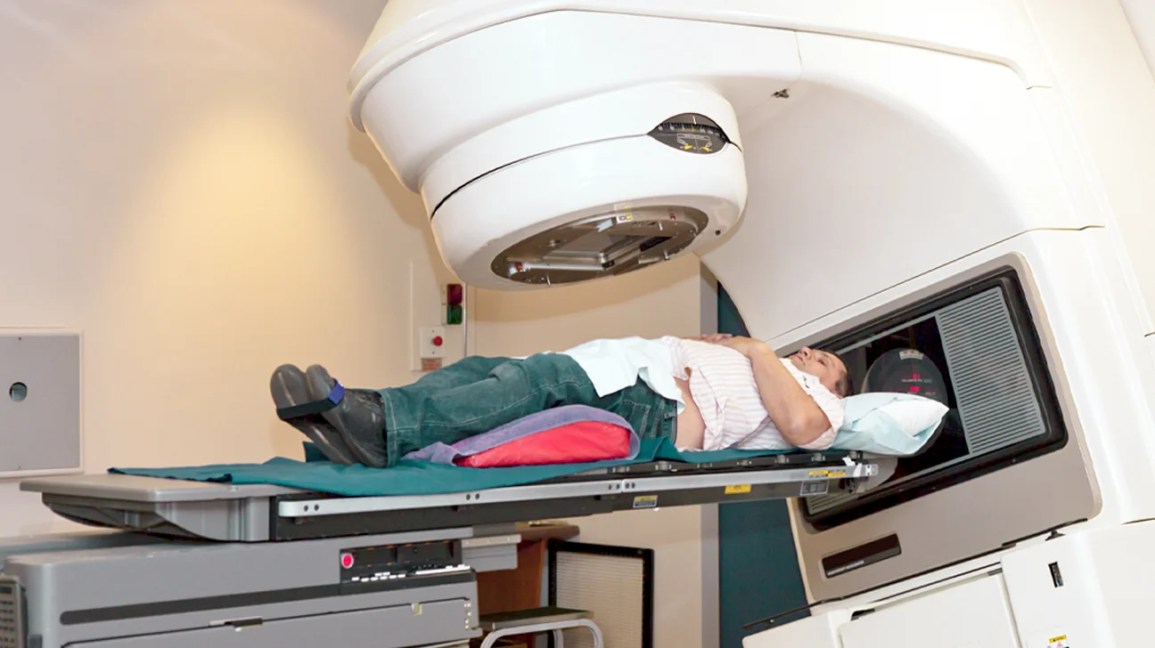
Modern Radiation Techniques
Todays radiation isnt the oldschool, onceaday grind. You have options like stereotactic body radiation therapy (SBRT) that deliver high doses in just five sessions, or doseescalated external beam radiation (EBRT) that push the total dose to 78Gy for tougher disease.
Who Benefits the Most?
HighRisk Disease
If your Gleason score is8or higher, PSA is above20ng/mL, or the tumor has extended beyond the prostate (T3T4), the combined approach is strongly recommended. Studies show the biggest survival bump here.
IntermediateRisk Disease
For Gleason 7 or PSA 1020ng/mL, shortterm ADT (typically 46months) paired with radiation often provides a modest benefitenough to tip the scales in favor of cure without overcommitting to longterm hormone sideeffects.
LowRisk Disease
When the cancer is lowgrade (Gleason6, PSA<10), radiation alone usually does the trick. Some men still choose ADT for peace of mind, but its not a medical necessity.
DecisionMaking Checklist
- PSA level
- Gleason score
- Stage on MRI or biopsy
- Overall health (bone density, heart health)
- Personal preferences regarding sideeffects
What the Treatment Looks Like
Radiation Options & Schedule
| Modality | Typical Sessions | Total Dose (Gy) | Key Advantage |
|---|---|---|---|
| EBRT (conventional) | 2040 | 7078 | Widely available |
| SBRT | 5 | 3640 | Short treatment course |
| Brachytherapy (seed implant) | 1 (implant) | 145 (lowdose) | Precise dose to prostate |
So, how many radiation treatments for prostate cancer? It depends on the methodconventional EBRT can be 2040 visits, while SBRT slashes that to just five.
Hormone Therapy (ADT) Details
- Injection forms: Luteinizing hormonereleasing hormone (LHRH) agonists or antagonists given every 13months. This is the prostate cancer injections every 3 months you might have heard about.
- Oral antiandrogens: Apalutamide, enzalutamide, etc., often added later. For discussion of specific drugs and their role, see anti-androgens prostate cancer for more detail.
- Typical duration: 6months for intermediaterisk, 2436months for highrisk. How long can a man stay on hormone therapy for prostate cancer? Generally up to three years in curative settings, longer in metastatic disease.
Why Some Men Refuse Hormone Therapy
Choosing to skip ADT is sometimes based on concerns about quality of lifeespecially the hot flashes, loss of libido, and bone thinning. In lowrisk cases, foregoing hormone therapy may be reasonable, but you should discuss the tradeoffs with your oncologist.
SideEffects The Good, The Bad, and The Manageable
RadiationRelated Toxicities
Most men experience mild urinary urgency or a feeling of fullness in the bowel that fades after treatment. Erectile dysfunction can happen, but many regain function over time, especially with penile rehab programs.
HormoneRelated Toxicities
Hot flashes are the most commonand they can feel like sudden waves of heat that creep up the chest. Bone health is another biggie; testosterone helps keep bones strong, so longterm ADT can lead to osteoporosis.
When you ask, how long can a man stay on hormone therapy for prostate cancer side effects become a concernmeaning you need regular bone density scans (DEXA), calcium/vitaminD supplements, and possibly bisphosphonates.
Managing the SideEffects
- Hot flashes: Dress in layers, avoid caffeine and spicy foods, try nighttime fans.
- Bone loss: Weightbearing exercise, calcium(1,200mg) + vitaminD(8001,000IU), and talk to your doctor about bisphosphonates or denosumab.
- Sexual health: Open dialogue with your partner, consider PDE5 inhibitors, and explore counseling if mood dips.
RealWorld Stories
Case Study A HighRisk Veteran
John, 70, was diagnosed with Gleason9 disease. His team recommended six months of ADT plus 40Gy EBRT. After treatment, his PSA dropped to <0.1ng/mL and stayed there for eight years. He endured hot flashes for the first six months, but with a support group and a daily walk, he felt empowered.
Patient Quote
The hot flashes were annoying, but knowing I cut my chances of spreading the cancer by 40% kept me going.
Case Study B IntermediateRisk Man Who Declined ADT
Mark, 65, had a Gleason7 tumor. He chose radiation alone after discussing the sideeffects of hormone therapy. Two years later, his PSA remains stable, but a recent MRI showed a tiny area of concern, prompting a discussion about adding shortterm ADT now.
Making the Decision Balance, Trust, and Action
Shared DecisionMaking Framework
Ask yourselfand your doctorthe following:
- What is my cancer risk group?
- How would shortterm hormone therapy affect my daily life?
- Do I have existing bone or heart conditions that could be worsened?
- What support resources are available (support groups, counseling, nutritionists)?
Printable Checklist (Downloadable)
Feel free to copy this list into a notes app:
- Risk category (low, intermediate, high)
- Preferred radiation type (EBRT, SBRT, brachytherapy)
- ADT schedule (4mo, 6mo, 24mo)
- Bone health plan (DEXA scan, supplements)
- Questions for my oncologist
Where to Find Reliable Information
Trusted sources include the National Cancer Institute (NCI), American Cancer Society, and major academic centers like Harvard, Mayo Clinic, and CedarsSinai. Look for uptodate, peerreviewed studies and avoid anecdotal miracle cure blogs.
Conclusion
For men facing intermediate or highrisk prostate cancer, the combination of radiation and hormone therapy offers a powerful chance at curenearly 98% diseasespecific survival at eight years and a substantial drop in metastatic risk. Yet the regimen isnt onesizefitsall; sideeffects, treatment length, and personal values all play a big role. Talk openly with your urologist and radiation oncologist, bring the decisionmaking checklist, and lean on reputable sources. If youve walked this path or have lingering questions, please share your experience in the commentsyour story might be the exact piece of reassurance another reader needs.
FAQs
What is the purpose of combining radiation with hormone therapy?
Combining the treatments shrinks the tumor by lowering testosterone, making cancer cells more vulnerable to radiation and improving survival rates.
Which patients benefit most from radiation plus hormone therapy?
Men with intermediate‑ or high‑risk prostate cancer (Gleason ≥ 7, PSA > 10 ng/mL, or T3‑T4 disease) see the greatest benefit.
How long is hormone therapy usually given with radiation?
Typical durations are 4‑6 months for intermediate‑risk disease and 24‑36 months for high‑risk disease, though individual plans may vary.
What are the common side effects of hormone therapy?
Hot flashes, loss of libido, bone thinning, mood changes, and metabolic shifts are the most frequently reported effects.
Can I avoid hormone therapy and still have good outcomes?
For low‑risk prostate cancer radiation alone is often sufficient; skipping hormone therapy in higher‑risk groups may increase the chance of recurrence.