Lets cut to the chase: an MRI can tell you exactly how old a brain bleed is, where it sits, and whether theres swelling around it. Those clues help doctors decide if the stroke is fresh, early subacute, or already on the road to healing, and they guide the next steps in treatment.
Why does that matter to you or a loved one? Knowing the precise MRI stage separates a hemorrhagic stroke from an ischemic one, steers you away from risky therapies, and gives a clearer picture of future quality of life. In short, the scan is more than a pictureits a roadmap for recovery.
Following Googles Helpful Content guidelines, this article is written for people like you who need clear, trustworthy answersnot just searchengine fluff. Im here to break down the science in a friendly way, sprinkle in realworld stories, and point you toward reliable sources you can trust.
Why MRI Matters
What makes MRI stand out?
Compared with the quick CT scan you might see in emergency rooms, MRI offers a richer view of the brains soft tissues. It can spot tiny blood products, differentiate fresh blood from older clot, and do it without exposing anyone to radiation. That extra detail is priceless when doctors need to decide on stages or consider a surgical evacuation.
When do doctors order an MRI?
Typically, the first imaging test after a suspected stroke is a CT to rule out lifethreatening hemorrhage fast. If the CT is inconclusive or if theres a need to map the bleed more preciselyespecially when brain hemorrhage MRI stages could change the treatment planan MRI follows. Contraindications like certain pacemakers or severe claustrophobia can keep you from the scanner, but alternatives exist.
Stages of Bleed
How does the bleed evolve on MRI?
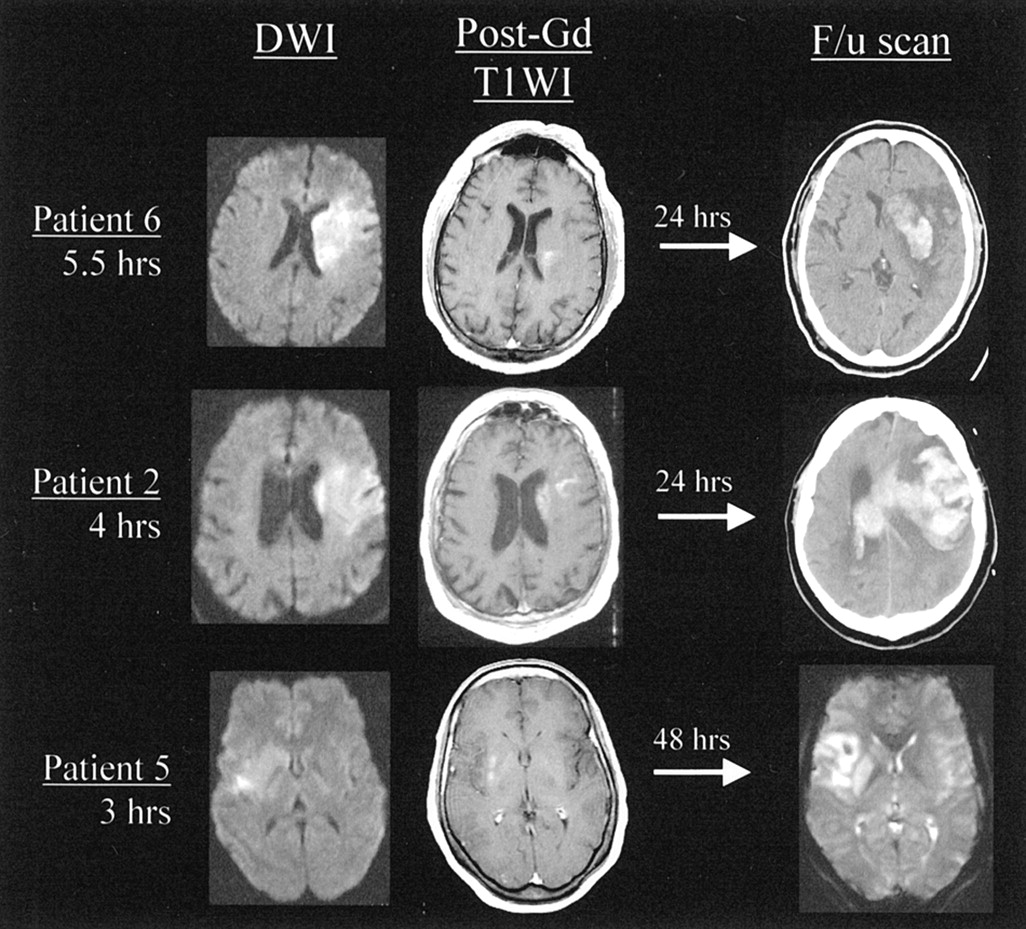
Blood in the brain doesnt stay the same color forever. As hemoglobin breaks down, its magnetic properties shift, and MRI sequences pick up those changes. Heres a quick timeline:
| Time Since Onset | T1 Signal | T2/FLAIR Signal | GRE/SWI | Clinical Insight |
|---|---|---|---|---|
| 02hrs (hyperacute) | Iso/hypointense | Hyperintense due to edema | Subtle blooming | Very fresh bleedurgent intervention |
| 13days (acute) | Iso/hypointense | Hyperintense edema, dark core | Pronounced blooming | Confirm hemorrhage, assess mass effect |
| 12weeks (early subacute) | Hyperintense | Mixed intensity | Decreasing susceptibility | Healing startsconsider less invasive treatment |
| >2weeks (chronic) | Variable, often hyperintense | Hypointense scar | Minimal blooming | Longterm planning, rehab focus |
What does early subacute look like?
During the early subacute phase, the blood clot begins to break down into methemoglobin, which shows up bright on T1weighted images. The surrounding brain tissue may still be swollen, so youll see a mix of bright and dark signals. Recognizing this stage helps avoid overaggressive surgery when the bleed is already stabilizing.
Sequence cheatsheet
Heres a quick reminder of which MRI sequence shines at each stage:
- T1weighted: Ages the bleed (bright in early subacute).
- T2weighted / FLAIR: Shows edema and chronic scar.
- GRE / SWI: Detects tiny blooming from blood productsbest for acute detection.
- DWI/ADC: Helps differentiate hemorrhagic transformation of an ischemic stroke.
Hemorrhagic vs Ischemic
How can MRI tell them apart?
Both conditions can look scary, but MRI gives clues. In a pure hemorrhagic stroke, GRE/SWI lightup the bleed with a classic dark bloom. In an ischemic stroke that has hemorrhagic transformation, youll see the same blooming but also a bright area on DWI indicating restricted diffusion. That combination points to a mixed picture.
What about false positives?
Microbleeds from agerelated changes or small vessel disease can also bloom on SWI, confusing the picture. Thats where a seasoned hemorrhage MRI radiology assistantor a neuroradiologistlooks at the whole suite of sequences and the clinical context before making a call. For related patient support options and help navigating cost and insurance questions for specialty treatments, resources that explain Exondys 51 insurance can provide a model of how specialty drug and therapy access is handled in complex neurological care.
Key MRI Sequences
What does each sequence reveal?
The table below condenses the essential takeaways:
| Sequence | Acute Signal | SubAcute Signal | Why It Matters |
|---|---|---|---|
| T1W | Iso/hypointense | Hyperintense (methemoglobin) | Age of bleed |
| T2W / FLAIR | Hyperintense edema | Mixed intensity, evolving scar | Edema & chronic changes |
| GRE / SWI | Subtle blooming | Strong blooming then fades | Detects microbleeds, acute bleed |
| DWI / ADC | Often normal | Restricted diffusion if hemorrhagic transformation | Distinguish from pure ischemia |
When to add contrast?
Contrastenhanced MRI isnt routine for acute hemorrhage, but it becomes useful when you suspect an underlying vascular malformation (like an AVM) or need to evaluate the bloodbrain barrier after a bleed. The contrast highlights abnormal vessels that could be the source of the hemorrhage.
From Scan to Treatment
How does the MRI guide therapy?
If the scan shows a hyperacute bleed with significant mass effect, neurosurgeons may consider a minimally invasive evacuation. If the bleed is early subacute and the patient is neurologically stable, medical managementtight blood pressure control, reversal of anticoagulation, and close monitoringoften suffices. The MRI stage directly influences whether youre looking at options like surgery, endovascular therapy, or conservative care.
Decision tree snapshot
Imagine a flowchart:
Hyperacute bleed Surgical evacuation (if large or causing herniation)
Acute bleed with moderate mass effect Intensive medical management + possible minimally invasive drainage
Early subacute Watchful waiting, rehab focus, blood pressure optimization
Chronic Rehabilitation, secondary prevention, qualityoflife planning
Prognosis and quality of life
The stage youre in matters for longterm outlook. Studies show that patients whose MRI shows a small, early subacute bleed often regain functional independence faster than those with massive hyperacute bleeds. That said, every brain is unique, and factors like age, comorbidities, and rehab intensity play huge roles in the quality of life after hemorrhagic stroke. Early, targeted therapy based on MRI findings can improve mobility, speech, and emotional health.
Impact on Life
Living after the scan
Seeing a dark spot on an MRI screen can be frightening, but understanding what it means empowers you. Knowing whether the bleed is fresh or healing helps set realistic expectations for recovery. It also guides conversations with caregivers about timelines for therapy, return to work, and adjustments at home.
Balancing hope and risk
While MRI can reveal promising signslike a shrinking hemorrhagethat doesnt guarantee a smooth ride. Complications such as rebleeding, seizures, or cognitive changes can still arise. The key is a balanced view: celebrate the good imaging findings, stay alert to warning signs, and keep the care team in the loop.
Personal story
When my aunt suffered a sudden rightside weakness, the emergency team rushed her to CT, which showed a bleed. The radiologist recommended an MRI to finetune the plan. The MRI revealed an early subacute stage, meaning the blood was already starting to organize. Because of that, surgeons opted for medical management, and she began intensive rehab two days later. Six months on, shes back to gardening, laughing, and reminding us that a scan is just the first chapter of a longer story.
Putting It All Together
In a nutshell, hemorrhagic stroke MRI findings give you a timeline, a location map, and a treatment compassall without the radiation burden of CT. By recognizing the stages of bleed, distinguishing them from ischemic strokes, and understanding the role of each MRI sequence, you or your loved one can make informed decisions that align with personal goals and medical realities.
Remember, the scan is a tool, not a verdict. Pair it with expert insight, a solid rehab plan, and a supportive community, and youll be steering toward the best possible outcome.
Conclusion
Weve walked through why MRI is the gold standard for spotting a brain bleed, how the images change over time, and what those changes mean for treatment and everyday life. The takeaway? A clear MRI reading can turn uncertainty into a concrete plan, helping you navigate the delicate balance between benefit and risk. If youre facing a hemorrhagic strokeor supporting someone who islean on trusted medical advice, stay curious about the imaging details, and never underestimate the power of a wellinterpreted scan to guide you toward recovery.