Quick Answers
Does a nerve injury trigger ALS?
Most of us have heard a horror story about a car accident or a sports injury that supposedly caused ALS. The short answer? A nerve injury can raise the odds, but its not a direct causeandeffect switch. Researchers think the injury may start a cascade of inflammation or misfolded proteins that, over years, increase the chance of motorneuron degeneration. As atypical Rett syndrome explains in other neurodevelopmental contexts, the link is still correlational, not causal.
How big is the ALS nerve injury risk?
If youre picturing a 100fold jump, youre overestimating. A large cohort study found that people with a major peripheral nerve injury had about a 1.3 to 1.5times higher risk of being diagnosed with ALS later in life . Put that in perspective: ALS itself affects roughly 2 in 100,000 people each year, so the absolute increase is still modest.
Which injuries matter most?
Not every bump or bruise is equal. The strongest signals come from:
- Severe limb trauma fractures, deep lacerations, or prolonged nerve compression.
- Repetitive strain think chronic carpal tunnel or tennis elbow that keeps the nerve irritated for months.
- Head or brain injury although typically discussed under traumatic brain injury, some studies show a spillover effect on spinal nerves.
Minor sprains or bruises havent shown a reliable connection.
Redflag symptoms to watch
Sometimes the nervous system mixes signals, and that can be confusing. Here are the signs that deserve a doctors look:
- Unexplained muscle weakness that doesnt improve with rest.
- Fasciculations (tiny muscle twitches) that appear in multiple regions.
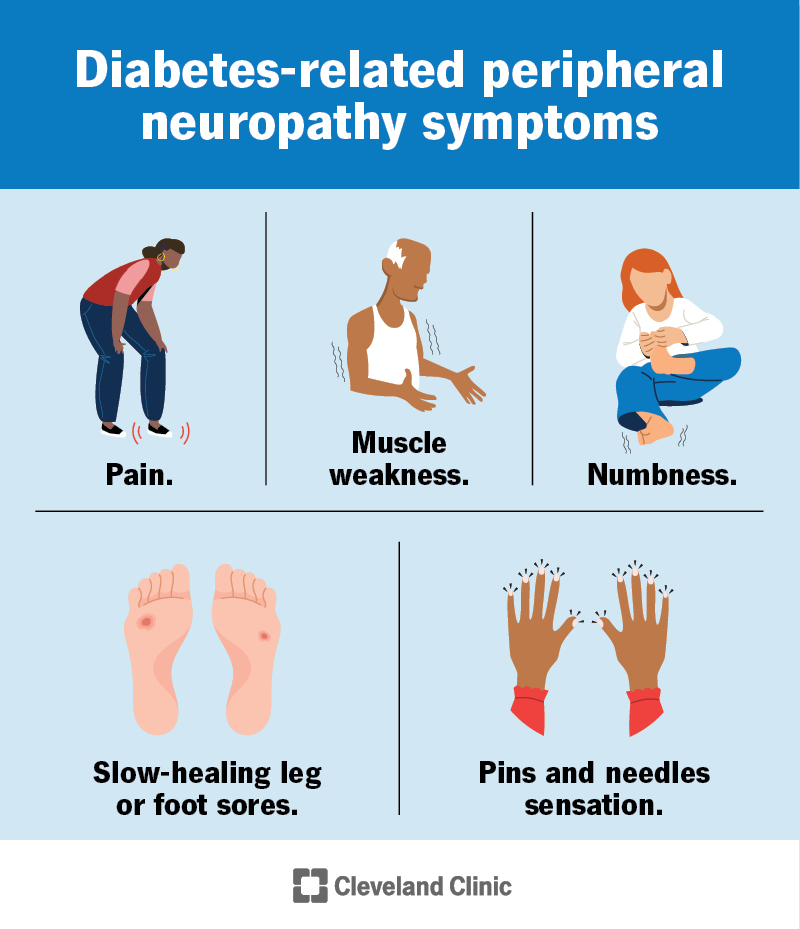
- Persistent numbness or tinglingespecially if its in the feet or hands and lasts beyond three months after the injury.
- Burning sensations that feel different from ordinary postinjury pain.
Pure sensory loss (just numbness without weakness) is rare in classic ALS, so if you have only that, other conditions are more likely. Still, keeping a symptom diary helps your neurologist see the whole picture.
When might ALS appear?
Latency is key. Most studies report a window of 5 to 12 years between a serious nerve injury and an ALS diagnosis. One 10year rule paper even suggests that the risk climbs a bit higher when the injury occurs a decade or more before symptom onset. In short, you wont see ALS the day after a sprained ankle, but the injury could be a subtle piece of a larger puzzle.
Science Overview
Inflammation Theory
Think of your body as a welltuned orchestra. A major nerve injury is like a sudden, dissonant chord that sends stress signals throughout the system. Cytokines such as IL6 and TNF flood the bloodstream, and over time that chronic inflammation may damage motor neurons. A 2020 article in Journal of Neuroinflammation highlighted how peripheral inflammation can cross the bloodbrain barrier, potentially nudging dormant ALS pathways into action.
PrionLike Propagation
Another fascinating idea is that misfolded proteinsthink of them as rogue LEGO brickscan travel along nerves, seeding other cells. After a nerve injury, the affected axon may become a highway for these rogue proteins, spreading the problem toward the spinal cord. This prionlike spread is still under investigation, but it offers a mechanistic bridge between trauma and neurodegeneration.
Supporting Data
| Study | Population | Injury Type | Relative Risk | Followup (years) |
|---|---|---|---|---|
| 2023 Cohort (USA) | 12,000 adults | Severe limb fracture | 1.45 | 15 |
| 2020 Neuroinflammation | Animal model | Sciatic nerve crush | inflammatory markers | 2 |
| 2018 Brain Trauma Review | 5,600 veterans | Head injury | 1.30 | 20 |
Counter Evidence & Limitations
Science is rarely black and white. Many variablessmoking, genetics, occupational exposurescan confound the results. No randomized controlled trial exists (ethics would prevent us from assigning people to get injured), so we rely on observational data. That means we must interpret the risk with caution and avoid sensational headlines.
Real Stories
Patient Tale
Meet John, a 58yearold carpenter who broke his right wrist in a fall back in 2010. He thought the lingering pins and needles were just postfracture nerve irritation. Fast forward twelve years, and he began noticing subtle hand weakness and occasional muscle twitches. After a battery of tests, his neurologist diagnosed ALS. Johns story mirrors the latency window we discussed, and it underscores why tracking symptoms over years matters.
Clinician View
Dr. Maya Patel, a boardcertified neurologist at the Neuromuscular Center, says she always asks patients about major injuries that happened a decade or more ago. She adds that the injury history alone doesnt clinch the diagnosis, but it adds a layer of context that can guide us toward earlier testing and, ultimately, earlier support for the patient.
Checklist: What to Bring to Your Appointment
- Dates and details of any serious nerve or head injuries.
- A symptom diary (weakness, tingling, pain).
- Family history of neurodegenerative diseases.
- Current medications and lifestyle factors (smoking, exercise).
Balancing Risks
Why It Matters
Understanding the ALS nerve injury risk isnt about living in fear; its about empowerment. Knowing the connection lets you stay vigilant, catch warning signs early, and have informed conversations with your healthcare team.
LowRisk Reality
Even with a modest relative increase, the absolute chance of developing ALS after an injury remains very lowstill under 1% for the vast majority of people. Its a piece of the puzzle, not the whole picture. So, while you shouldnt dismiss an injury, you also dont need to panic.
Preventive Steps
Here are some everyday habits that may lower overall ALS risk and improve nerve health:
- Stay active regular aerobic exercise supports circulation and reduces inflammation.
- Avoid smoking tobacco compounds are known neurotoxins.
- Protect against head injuries wear helmets during highrisk activities.
- Promptly treat severe limb injuries proper immobilization and rehab can reduce chronic nerve irritation.
Helpful Resources
For deeper dives, consider the ALS Association website, the National Institute of Neurological Disorders and Stroke, and reputable medical journals that publish the latest findings. If you need guidance on navigating treatment assistance or insurance coverage for specialized therapies, resources about Exondys 51 insurance provide examples of how complex coverage questions are handled for high-cost neurologic treatments.
Professional Evaluation
RedFlag Symptoms
If you notice any of the following, schedule a neurology consult sooner rather than later:
- Progressive muscle weakness in one limb or multiple areas.
- Fasciculations that become more widespread.
- Unexplained weight loss or fatigue.
- Persistent numbness or tingling that doesnt improve after injury recovery.
Diagnostic Tools
Neurologists typically use a blend of tests to rule in or out ALS:
- Electromyography (EMG) & Nerve Conduction Studies (NCS) assess electrical activity in muscles and nerves.
- MRI rules out structural causes.
- Blood panels check for metabolic or inflammatory markers.
- Genetic testing (if theres a strong family history).
Appointment Prep
Bring the checklist from the Real Stories section, and be ready to answer questions about:
- Timeline of any major injuries.
- When symptoms first appeared and how theyve changed.
- Lifestyle factors that could influence nerve health.
Being thorough helps the specialist focus on the most relevant exams and avoid unnecessary procedures.
Conclusion
So, whats the bottom line? A serious nerve injury can nudge the odds of ALS upward, but the absolute risk stays low, and many other factors are at play. By staying aware of redflag symptoms, keeping a detailed injury history, and seeking timely professional evaluation, you give yourself the best chance to catch any problem early. Remember, knowledge isnt a guarantee of doomits a tool for empowerment.
If youve experienced a major injury or have questions about ALS, feel free to share your story in the comments. Your experience might help someone else feel less alone, and together we can turn curiosity into confidence.
FAQs
Does a nerve injury directly cause ALS?
No. Current research shows only a correlational link; major nerve injuries may increase the odds but are not a direct cause of ALS.
What is the estimated increase in ALS risk after a severe nerve injury?
Large studies report a 1.3‑ to 1.5‑fold higher risk, which translates to a modest absolute increase given ALS’s rarity (≈2 per 100,000 per year).
Which types of nerve injuries are linked to higher ALS risk?
Severe limb trauma (fractures, deep lacerations), chronic repetitive strain (e.g., long‑standing carpal tunnel), and significant head/brain injuries show the strongest associations.
How long after an injury might ALS symptoms appear?
The typical latency window is 5 to 12 years; some data suggest risk may rise further after a decade following the injury.
What steps can I take to monitor my nerve health after an injury?
Keep a symptom diary, watch for unexplained weakness, muscle twitches, or persistent tingling, and seek a neurology consult promptly if red‑flag signs emerge.