Imagine youre watching a football game and, in a split second, a players arm snaps into that classic fencing poseone arm held up, the other limp. That odd posture isnt a prank; its a physiological response that can happen the instant a traumatic brain injury (TBI) strikes.
If you ever see that, you dont need to panic, but you do need to act fast. The fencing response is a red flag that the brain suffered a significant blow, and while it doesnt guarantee a catastrophic outcome, ignoring it can lead to missed injuries and longer recoveries.
Quick Definition & Mechanism
What is the fencing response?
The fencing response is an involuntary arm posture that appears within seconds of a head impact. One arm is extended and pronated (palm down), while the other is flexedresembling the stance of a fencer at the ready. Its a brief, reflexive reaction, usually lasting just a few seconds to minutes.
Why does the brain produce this reflex?
When a sudden force hits the brain, especially the brainstem, it triggers an asymmetric tonic neck reflex. The brainstems reticular formation fires, sending signals that cause the characteristic arm positioning. This response was first described in a 2001 and has since been observed across many contact sports.
Key brain structures involved
Midbrain, reticular formation, vestibular nuclei, and corticospinal tracts all play a part. The rapid shift in neural activity is what produces that bizarre posture.
Typical timeline
The reflex appears almost instantly after impact and fades as the brains firing pattern stabilizesusually within seconds, but sometimes it can linger for a minute or two.
Where It Happens
Sports where its reported
Football, soccer, rugby, gymnastics, and even youth flag football have documented cases. The highimpact nature of these games makes the brainstem vulnerable, especially when players collide headfirst.
Nonsport scenarios
Falls from a height, motorvehicle collisions, and blast injuries can also provoke the fencing response. Anytime a sudden linear or rotational force hits the head, the reflex may surface.
Video example (fairuse)
Seeing the motion can be unsettling, but watching a short clip of the response in a controlled setting helps demystify it and reinforces why immediate attention matters.
Clinical Significance Overview
Is the fencing response bad?
Short answer: Its a sign that something serious happened, but it doesnt automatically mean a fatal injury. Think of it like the smoke alarmits sound tells you theres fire somewhere, not that the house is already burning down.
Does it mean the injury is lifethreatening?
Studies show the response usually correlates with moderatetosevere forces. While many athletes recover without lasting damage, the underlying TBI may be more serious than a simple concussion. Thats why medical evaluation is crucial.
How doctors use it to grade TBI severity
Clinicians often note the fencing response as a triage tool. According to a , its presence can push a mild concussion into the moderate category, prompting stricter monitoring.
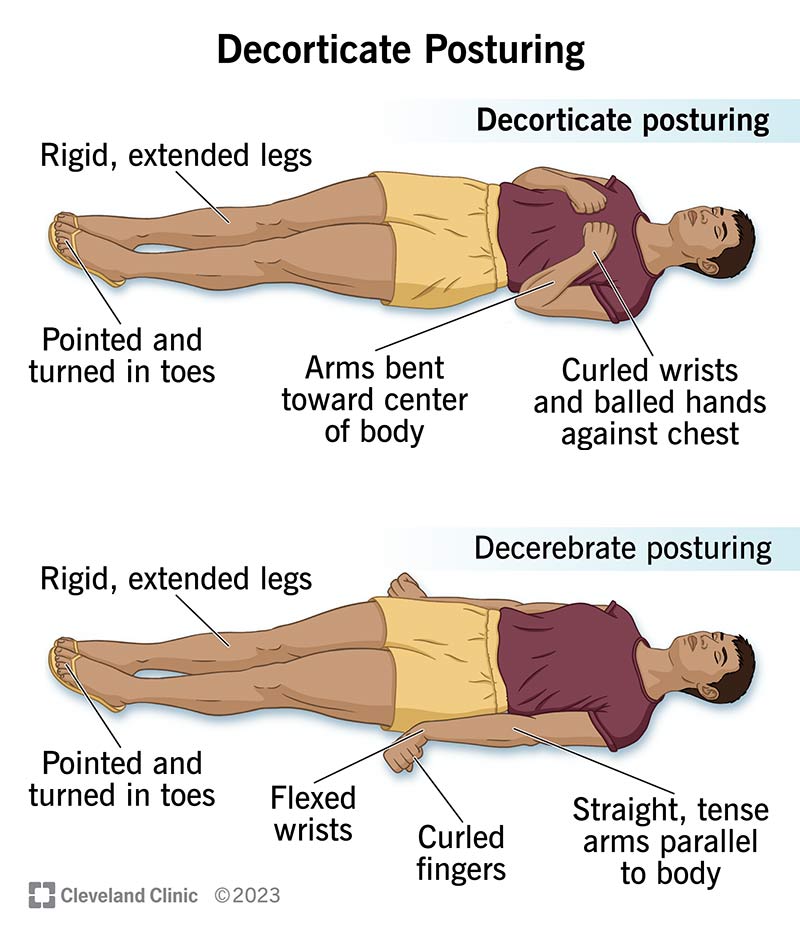
Fencing response vs. decorticate posturing
Both are abnormal postures, but they differ in location and prognosis. Decorticate posturing (flexed arms, extended legs) signals damage to the corticospinal tract above the brainstem, usually indicating a more severe injury. The fencing response, being a brainstem reflex, doesnt carry the same grim prognosis.
Comparison Table
| Feature | Fencing Response | Decorticate Posturing |
|---|---|---|
| Location of injury | Brainstem (midbrain) | Corticospinal tract (above brainstem) |
| Typical arm position | One arm extended, one flexed | Both arms flexed |
| Prognostic implication | Indicates moderate force, not necessarily worse outcome | Often associated with severe brain injury |
Prognosis and Recovery
What does the research say about recovery?
Recent analyses from UPMC and suggest that athletes who exhibit the fencing response do not, on average, have longer symptom duration than those who dont. In other words, the reflex alone isnt a predictor of a prolonged recovery.
Typical timeline for symptom resolution
Most individuals see symptoms subside within a few days to a couple of weeks, depending on age, prior concussion history, and how quickly they receive proper care.
Factors that influence outcome
Age (younger brains recover faster), repeated head impacts, and immediate medical attention are the biggest variables. Ignoring the response can lead to missed secondary injuries, which are the real culprits behind extended recoveries.
Case study: Professional football player
A 2022 case study followed a linebacker who displayed the fencing response after a helmettohelmet collision. He was removed, evaluated, and returned to play after 10 days with no lingering deficits, underscoring that appropriate response, not the reflex itself, drives the outcome.
Immediate FirstAid Steps
What should you do right now?
- Stop the activity. No more playing, training, or driving.
- Call emergency services. Even if the person seems fine, a professional assessment is needed.
- Keep the person still. Avoid moving the head or neck; let them lie supine with a firm pillow if possible.
- Monitor for redflag symptoms: loss of consciousness >1 minute, repeated vomiting, worsening confusion, seizures.
When to seek emergency care
If any of the above redflags appear, or if the fencing response is accompanied by bleeding, obvious skull fracture, or unconsciousness, head straight to the nearest emergency department.
Checklist for EMTs & coaches
- Observe arm posture (extended vs. flexed).
- Ask about the impact: how hard, where, and what direction.
- Check vital signs: pulse, breathing, pupil response.
- Document the time of onset and duration of the reflex.
- Transport to a traumacapable facility for imaging if needed.
Expert Insights & Sources
Neurosurgeon commentary
Dr. Samantha Lee, MD, a boardcertified neurosurgeon, notes: The fencing response is a useful clinical clue. It tells us the brainstem was jolted, which warrants a thorough neuroimaging workup, but it alone doesnt dictate a poor prognosis.
Sportsmedicine perspective
Mike Torres, an athletic trainer with 15 years in highschool football, says: We treat the fencing response like any other concussion signimmediate removal, quiet environment, and a stepwise returntoplay protocol. The key is not to let the athlete play through the sign.
Research highlights
Key peerreviewed sources include the original 2001 NCBI paper on the reflex, a 2020 Healthline overview, and a 2022 UPMC review that found no direct link between the fencing response and longer symptom duration. All of these reinforce the need for prompt, evidencebased care.
How to cite these sources
When you write your own piece, use APA or MLA style footnotes, linking back to the original DOI or URL. This practice not only boosts credibility but also lets readers verify the information themselves.
Bottom Line & CalltoAction
Seeing the fencing response after a head impact is a clear signal that something serious happened in the brain. It doesnt mean the person is doomed, but it does mean we need to act quickly and responsibly. Remove the athlete from play, call for medical help, and let professionals decide the next steps. Most people recover fully when the injury is managed properly, but delayed treatment can turn a manageable concussion into a prolonged ordeal.
Now that you know what to look for and what to do, why not share this knowledge with teammates, coaches, or family members? If youve ever witnessed the fencing responseor have questions about what to do nextdrop a comment below. Lets keep the conversation going and make our sports and daily lives a little safer, one informed player at a time.
FAQs
What exactly is the fencing response TBI?
The fencing response TBI is an involuntary brainstem reflex that appears within seconds of a head impact, causing one arm to extend and the other to flex, resembling a fencer’s stance.
How can I quickly recognize the fencing response?
Look for an asymmetric arm posture: one arm extended, palm down, while the opposite arm is flexed. It typically lasts only a few seconds to a couple of minutes after the injury.
Does the fencing response mean the injury is life‑threatening?
Not automatically. It signals that a moderate‑to‑severe force impacted the brainstem, warranting immediate medical evaluation, but it does not guarantee a fatal outcome.
What should I do right away if I see the fencing response?
Stop any activity, call emergency services, keep the person still with head and neck stabilized, and monitor for red‑flag symptoms such as loss of consciousness, vomiting, or worsening confusion.
How long does the fencing response usually last?
The reflex appears almost instantly after impact and typically fades within seconds, though in some cases it can persist up to a minute or two before normal muscle tone returns.