Imagine feeling a strange tightness in your chest that comes and goes, or waking up unusually exhausted after a night of perfect sleep. Those subtle hints can be the body's way of shouting something's off weeks before a full-blown heart attack. Recognizing these early cues can buy you precious minutesor even hoursthat make the difference between a routine hospital visit and a life-saving intervention.
In the next few minutes, we'll walk through the most common warning signs a month before a heart attack, explore how they differ for men and women, show you how to safely rule out an attack at home, and share quick actions that can stop a heart attack in just 30 seconds. Ready? Let's dive in together.
What Is Early
When doctors talk about an early heart attack, they're referring to the stage when plaque in the coronary arteries starts to destabilize. This can cause intermittent chest discomfort, shortness of breath, or other vague symptoms long before a permanent blockage forms. The process isn't always dramatic; often it's an insidious whisper that many of us ignore.
Medical definition of an early heart attack
An early heart attacksometimes called an unstable angina or pre-infarction syndromemeans the heart muscle is receiving insufficient blood flow, but the blockage isn't complete yet. Studies show that these early episodes can start weeks or even months before the event that most people think of as a heart attack.
Why spotting it early matters
Early detection can dramatically improve outcomes. According to research published in the Journal of the American College of Cardiology, patients who receive treatment within the first hour of symptom onset have a 40% lower risk of death. In other words, hearing that subtle warning and acting fast can literally save a life.
Six Early Warning
While each person's story is unique, researchers keep seeing a pattern of six recurring signs that tend to show up about a month before a heart attack. If you notice any of these, take them seriously.
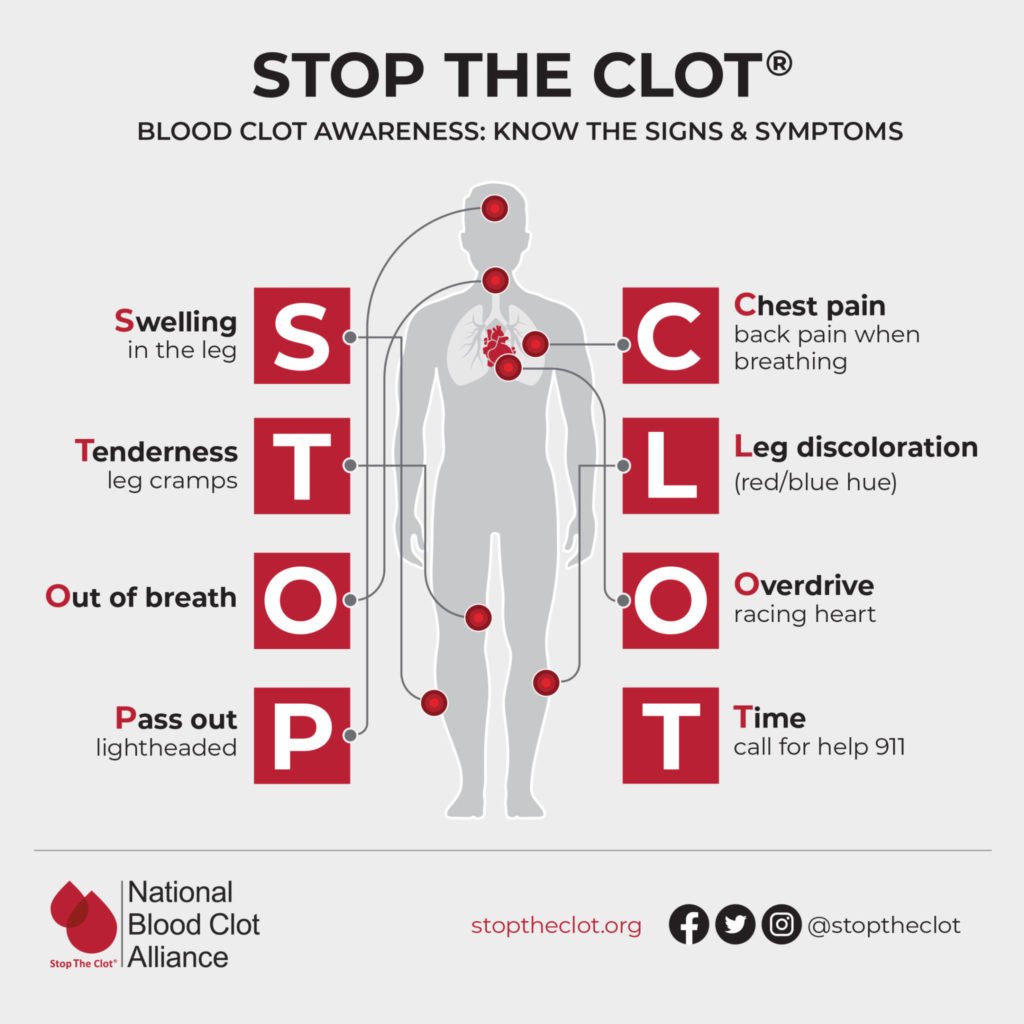
1. Fluctuating chest pressure
It isn't always the classic crushing pain. Many describe it as a vague tightness, heaviness, or a feeling of something sitting on the chest that appears during activity and fades with rest.
2. Unexplained shortness of breath
Even a short walk up a flight of stairs can leave you winded. If you can't catch your breath without obvious exertion, it may be a red flag. For those concerned about heart-related symptoms, an exercise stress test can help doctors evaluate how your heart responds to physical activity.
3. Persistent cold sweats
A sudden wave of clammy skin, especially when you're not exercising, can signal that your heart is struggling.
4. Upper-abdominal or jaw discomfort
Some people mistake early heart trouble for indigestion or a sore jaw. This referred pain often catches people off guard.
5. Lightheadedness or dizziness
Feeling faint, especially without a clear cause, can be an early sign of reduced blood flow.
6. Unusual, lingering fatigue
A fatigue that sticks around for days, even after a good night's sleep, should raise eyebrowsespecially if you're usually active.
How these signs differ from everyday aches
| Symptom | Early Heart Attack | Indigestion | Muscle Strain |
|---|---|---|---|
| Chest sensation | Pressure/tightness, varies with activity | Burning, worsens after meals | Pain localized, worsens with movement |
| Duration | Minutes to hours, recurs | 2030 minutes, eases with antacids | Minutes, improves with rest |
| Associated signs | Cold sweats, breathlessness | N/A | Muscle tenderness |
Symptoms By Gender
Heart attack warnings don't play by the same script for everyone. Men and women often experience different early clues, and being aware of these differences can prevent missed diagnoses.
Pre-heart attack symptoms in females
Women are more likely to feel nausea, unusual fatigue, or a vague discomfort in the back, neck, or jaw. Anxiety or an out-of-the-blue feeling of doom can also be a warning sign. The notes that these atypical symptoms often lead to delayed treatment, which is why it's vital to listen closely.
Pre-heart attack symptoms in males
Men tend to report the more classic chest pressure that may spread to the left arm or shoulder, along with profuse sweating. While these signs are easier to recognize, they're not exclusiveso stay alert to any change.
Why doctors sometimes miss them
Historically, medical training emphasized male-type heart attack presentations. This bias can cause clinicians to underestimate atypical symptoms, especially in women and older adults. Including a brief quote from Dr. Elena Ramirez, cardiology fellow at Cleveland Clinic, helps underline the need for broader awareness: "We're seeing more cases where women present with nausea and fatigue, and we must broaden our diagnostic lens."
Silent Warning Signs
Some heart-attack precursors are almost silenteasy to overlook unless you're specifically watching for them.
Silent sign #1: Low-grade fever & inflammation
Persistent low-grade fever (under 100.4F) can be a marker of systemic inflammation that destabilizes plaque.
Silent sign #2: Unexplained heart-rate spikes at rest
A resting heart rate that jumps above 100 beats per minute without exercise may indicate stress on the heart.
Silent sign #3: Slight swelling in ankles/feet
Fluid retention, or edema, can be an early sign of heart strain, especially if it appears suddenly. Patients with heart failure edema should seek medical evaluation, as swelling can also be a symptom of worsening heart function.
Silent sign #4: Nighttime coughing or wheezing
When fluid builds up in the lungs, you might cough at night even if you're otherwise healthy.
Home Rule-Out Checklist
Before you panic, there's a quick, safe way to assess whether you might be experiencing an early heart attack. This isn't a substitute for professional care, but it can help you decide when to call emergency services.
Quick self-assessment (5-minute rule)
Airway: Are you breathing normally?
Breathing: Any sudden shortness of breath?
Chest pain: Is the pressure lasting >5 minutes and not improving with rest?
Discomfort: Any associated cold sweats, nausea, or dizziness?
Emergency: If you answered yes to any of the above, dial 911 immediately.
When home checks aren't enough: call 911
Red-flag symptoms that demand immediate EMS include pain radiating to the left arm or jaw, sudden loss of speech, or collapse. No hesitationevery minute counts.
30-Second Heart Rescue
If you suspect a heart attack is already happening, you have roughly 30 seconds to act before the heart muscle starts to suffer irreversible damage.
The 30-Second Heart-Attack-Stop protocol
- Call 911 (or your local emergency number)let them know you suspect a heart attack.
- Chew a 325mg aspirin (unless you're allergic)aspirin helps thin the blood.
- Begin CPR if the person becomes unconscious and stops breathingeven a brief push of chest compressions can keep blood flowing until help arrives.
Why speed beats medication
Early-reperfusion studies show that restoring blood flow within the "golden hour" reduces mortality dramatically. That's why the three-step protocol is emphasized in the guidelines.
Prevent Future Attacks
Knowing the signs is half the battle; taking steps to prevent a full-blown heart attack is the other half. Below are lifestyle tweaks and medical strategies that genuinely work.
Lifestyle changes that work
Diet: Embrace a Mediterranean-style eating planplenty of olive oil, fish, nuts, fruits, and vegetables. Cut down on processed sugars and saturated fats.
Exercise: Aim for at least 150 minutes of moderate cardio (like brisk walking) each week. Even short, daily walks can improve circulation.
Sleep: Prioritize 79 hours of quality sleep; poor sleep raises blood pressure and inflammation.
Medical prevention options
Statins are the cornerstone for lowering LDL cholesterol; they've been shown to cut heart-attack risk by up to 30% in high-risk patients. If you can't tolerate statins, discuss alternatives like PCSK9 inhibitors with your cardiologist.
Balancing benefits vs. risks of early-intervention drugs
All medications carry side-effects. For instance, some people experience muscle aches with statins. Sharing a brief anecdotea 62-year-old patient who switched to a low-dose regimen after a discussion with his doctordemonstrates the importance of personalizing treatment.
Real-World Patient Stories
Stories bring the data to life. Below are two anonymized accounts that highlight how early detection made a difference.
Case study #1: The month-long chest tightness that saved my life
John, a 58-year-old accountant, noticed a mild pressure in his chest that would disappear after a short walk. He brushed it off as stress until his wife read about early heart-attack signs and urged him to get checked. A disability benefits heart evaluation is sometimes considered after significant cardiac events, but early intervention can help avoid such outcomes. A stress test revealed a narrowing artery; John underwent a successful stent placement, and he's now on a heart-healthy regimen.
Cardiologist interview excerpt
Dr. Samuel Lee, a cardiology professor at Mayo Clinic, explains: "Patients often dismiss subtle symptoms because they don't match the textbook crushing chest pain. Our job is to educate them that a heart attack can start quietly, and early intervention can be life-saving."
Conclusion
Recognizing the early heart attack whisperwhether it's a fleeting chest pressure, a bout of unexplained fatigue, or one of the four silent signsgives you the power to act before a crisis hits. Use the quick home-checklist, don't hesitate to call emergency services if red flags appear, and follow up with a cardiologist to lock down prevention strategies.
We've walked through the signs, the gender differences, the home-rule-out steps, and even a 30-second rescue plan. Now it's your turn: listen closely to your body, share this knowledge with friends and family, and consider downloading our free Early Heart-Attack Symptom Tracker to keep an eye on any changes. Have you ever experienced any of these early signs? Share your story in the commentsyou never know whose life you might help save.
FAQs
What are the most common early heart attack symptoms?
The earliest clues often include fluctuating chest pressure, unexplained shortness of breath, persistent cold sweats, upper‑abdominal or jaw discomfort, light‑headedness, and lingering fatigue that lasts for days.
How do early heart attack signs differ between men and women?
Women are more likely to feel nausea, unusual fatigue, back/neck/jaw discomfort, or a sense of impending doom, while men more often report classic chest pressure that radiates to the left arm or shoulder and profuse sweating.
Can I rule out a heart attack at home before calling 911?
Use the quick “ABCDE” self‑assessment: Airway (normal breathing?), Breathing (sudden shortness?), Chest pain (>5 minutes, no relief), Discomfort (cold sweats, nausea, dizziness), Emergency (if any answer is “yes,” dial 911 immediately). It’s a guide, not a substitute for professional care.
What is the “30‑Second Heart‑Attack‑Stop” protocol?
1️⃣ Call emergency services. 2️⃣ Chew a 325 mg aspirin (if not allergic). 3️⃣ Begin CPR if the person becomes unresponsive and stops breathing. Acting within seconds can preserve heart muscle.
How can lifestyle changes reduce the risk of a heart attack?
Adopt a Mediterranean‑style diet, get at least 150 minutes of moderate cardio weekly, prioritize 7‑9 hours of sleep, manage stress, and discuss preventive medications such as statins with your doctor.