Feeling lightheaded after youve beaten COVID? Chances are your body is sending a subtle alarm: low blood pressurerelated dizziness. Its not just being tired its a real, physiological response that can be unsettling, especially when it shows up out of nowhere.
Below well break down why COVID can tip the balance of your blood pressure, how to spot the warning signs, and what you can actually do today to feel steadier. Think of this as a friendly chat with a buddy whos been through the same fog.
Why It Happens
Autonomic dysfunction the hidden link
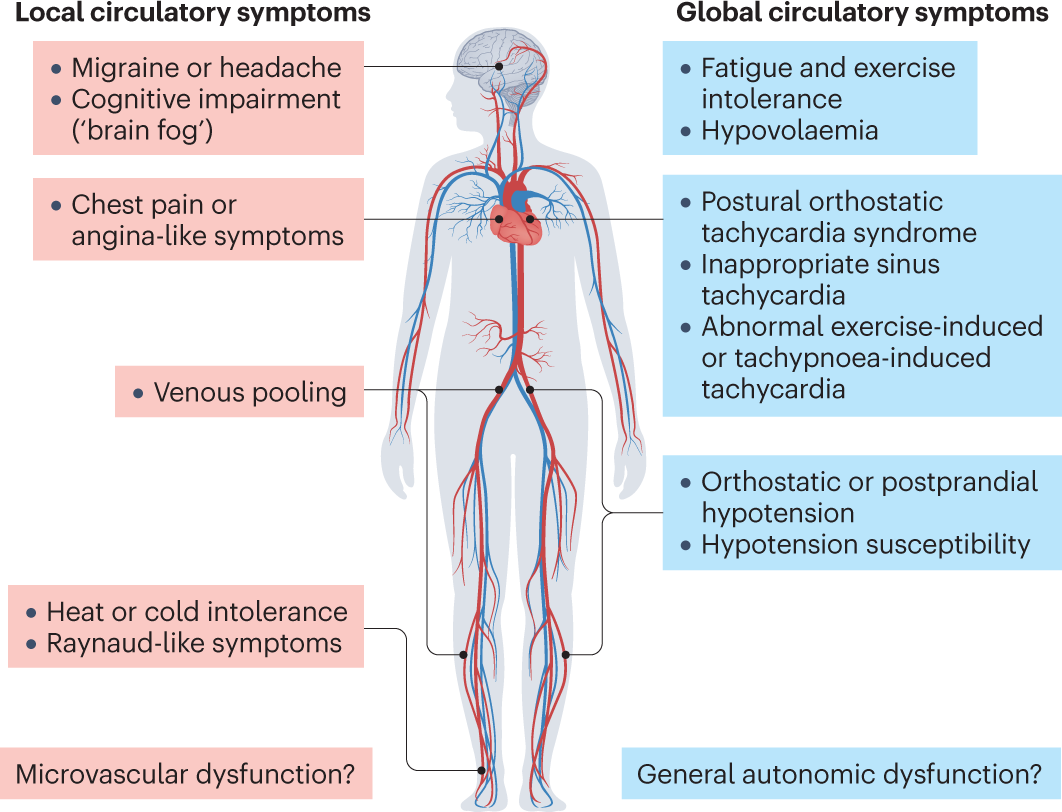
One of the most common culprits behind postCOVID dizziness is autonomic dysfunction. The autonomic nervous system (ANS) is the autopilot that keeps your heart rate, blood vessels, and breathing in sync. When COVID messes with that system, you can end up with a swing between too much and too little sympathetic (fightorflight) activity.
According to , nearly a third of patients reported orthostatic intolerance the fancy term for feeling woozy when you stand up. Thats the lowbloodpressure side of the story.
Inflammation and vascular tone
The virus also triggers a cascade of inflammatory chemicals (cytokines) that can thin the walls of your blood vessels. When vessels are less tight, blood pools in your legs and less returns to the heart, causing a dip in the pressure that reaches your brain. Think of it like a garden hose thats been kinked less water (or blood) reaches the far end.
Whos most at risk?
- Elderly folks age already reduces vessel elasticity, so a COVIDrelated hit can tip the scales.
- Women some research suggests women experience more severe autonomic symptoms after COVID.
- People with preexisting lowBP conditions if you already run on the lower end, the virus can push you further down.
Spotting the Symptoms
Classic trio: lightheadedness, faint feeling, sudden sweating
If youve ever gotten up from a chair and felt the room spin, thats the classic triad. Sudden sweating, and feeling faint covid is something many Reddit users have shared in the threads. Its not just a random chill its your body trying to compensate for a pressure drop.
Dizziness vs. other causes
| Feature | LowBP Dizziness (PostCOVID) | Other Common Causes |
|---|---|---|
| Trigger | Standing up quickly, prolonged sitting | Innerear infection, medication sideeffects |
| Heartrate response | Increase >20bpm (possible POTS) | No significant change |
| Associated symptoms | Cold clammy skin, fainting | Headache, nausea, ear ringing |
The standtest is a quick selfcheck: take your blood pressure supine, stand up, and measure again after 3 minutes. A drop of 20mmHg systolic or 10mmHg diastolic, accompanied by a heartrate surge, flags orthostatic hypotension.
Redflag warnings
If you ever experience chest pain, prolonged loss of consciousness, or a sudden severe headache, dont wait call emergency services. Those signs are outside the typical postCOVID lowBP pattern and need immediate evaluation.
Getting a Proper Diagnosis
What your doctor will look for
During a postCOVID visit, clinicians usually record orthostatic vitals (lying, sitting, standing). Theyll also ask about the timing of your symptoms, any fever, and how long youve been feeling off.
Useful tests and why they matter
- Tilttable test reproduces the dizziness in a controlled setting.
- 24hour ambulatory BP monitoring catches fluctuations you might miss during a short office visit.
- Basic labs CBC, electrolytes, and thyroid panel rule out anemia or hormonal imbalances.
When selftracking can help
Keeping a simple log of blood pressure, heartrate, and symptom notes can make your next appointment far more productive. Below is a quick template you can copy into a spreadsheet:
| Date | Time | Position | BP (mmHg) | HR (bpm) | Symptoms |
|---|---|---|---|---|---|
| 20250827 | 08:00 | Supine | 120/78 | 68 | - |
| 20250827 | 08:03 | Standing | 95/65 | 92 | Lightheaded, sweaty |
Managing Low Blood Pressure Dizziness After COVID
Lifestyle tweaks that work
Simple habits can make a huge difference:
- Hydration Aim for 23L of water daily, plus electrolytes if you sweat heavily.
- Salt intake An extra 12grams of sodium (think a pinch of sea salt on meals) can raise blood volume.
- Compression stockings These gentle squeezers keep blood from pooling in your legs.
Physical strategies
Gradual position changes are key. Before getting up, sit for a minute, swing your legs gently, then stand. Counterpressure maneuverscrossing your legs or squeezing a handgripalso boost venous return.
Light resistance training (bodyweight squats, wall pushups) performed a few times a week helps the cardiovascular system adapt and reduces orthostatic drops over time.
Medications & when theyre appropriate
For persistent cases, doctors may prescribe:
- Fludrocortisone boosts sodium retention, raising blood volume.
- Midodrine a shortacting vasoconstrictor that tightens blood vessels.
- Betablockers used when a rapid heartrate overcompensates.
Each comes with its own set of pros and cons, so a conversation with a cardiologyautonomic specialist is essential before starting. If you have concerns about how these symptoms relate to broader cardiovascular issues, resources on DI heart failure can help explain overlapping signs and when to seek specialist care.
Complementary approaches
Gentle yoga, slow diaphragmatic breathing, and mindfulness can calm the nervous system and lessen the sudden fightorflight spikes that worsen dizziness. Adequate sleep and a balanced diet rich in B12 and vitaminD also support overall vascular health.
LongCOVID Specific Considerations
PostCOVID low blood pressure vs. POTS
Postural Orthostatic Tachycardia Syndrome (POTS) often overlaps with lowBP dizziness. The key distinction is heartrate: POTS typically shows a rise of >30bpm (or >40bpm in teens) upon standing, whereas pure orthostatic hypotension shows a pressure drop with a modest or no heartrate increase.
Will postCOVID POTS go away?
Current evidence suggests many people improve within 612months with a combination of rehab, hydration, and graded exercise. However, a small subset may need longterm management. Ongoing research from UTSW shows that about 40% of patients experience full symptom resolution after a structured longCOVID rehab program.
Community insights lessons from Reddit
Scrolling through threads, I saw a pattern: people who added a salty snack before bedtime reported fewer morning woozy episodes. Others found success with short, frequent meals (instead of three big ones) to keep blood volume steady.
One user wrote, I started a 500ml waterelectrolyte drink before getting up at night, and the faint spells stopped after two weeks. Realworld anecdotes like this give us practical, lowtech ideas that research papers often overlook.
Putting It All Together
Living with postCOVID low blood pressure dizziness can feel like walking on a shifting floor, but the good news is that most of the variables are within your control. Understanding the why (autonomic dysfunction, inflammation, vascular tone) empowers you to target the how (hydration, salt, gentle movement, and smart medical care).
If you notice the classic triadlightheadedness, sudden sweating, and an uneasy faint feelingtake a moment to do a standtest, jot down the numbers, and reach out to your clinician. Theyll likely order a few simple labs and perhaps a tilttable study to rule out anything more serious.
Meanwhile, tiny daily habitsdrinking a glass of water with a pinch of salt when you wake up, slipping on compression socks before a long day, and moving slowly from lying to standingcan add up to noticeable relief.
Remember, youre not alone in this fog. Thousands are navigating the same waters, sharing tips on forums, and working with doctors to reclaim steadier days. So, keep tracking, stay curious, and give yourself credit for each small win.
Conclusion
COVID can shake the autonomic system, leading to low blood pressure dizziness that may linger for weeks or months. By recognizing the symptoms, getting a proper diagnosis, and adopting evidencebased lifestyle tweaks (hydration, salt, gentle exercise, and supportive gear), most people find their balance again. If symptoms persist or you hit redflag warnings, seek medical attention promptly. Feel free to share your story in the comments or ask any lingering questionsyoure part of a community thats learning and healing together.
FAQs
What causes low blood pressure dizziness after COVID?
Low blood pressure dizziness after COVID is often caused by autonomic dysfunction, which disrupts the nervous system’s control of blood vessel tone and heart rate. Inflammation from COVID can also weaken blood vessels, causing blood pooling and drops in blood pressure when standing.
How can I tell if my dizziness is due to low blood pressure post-COVID?
Dizziness from low blood pressure typically occurs when standing up quickly or after sitting for a long time, accompanied by light-headedness, sweating, or faintness. A drop of at least 20 mmHg systolic or 10 mmHg diastolic blood pressure upon standing suggests orthostatic hypotension related to low blood pressure.
What lifestyle changes help reduce COVID-related low blood pressure dizziness?
Increasing hydration, adding moderate salt to your diet, wearing compression stockings, rising slowly from sitting or lying positions, and doing light resistance exercises can improve blood circulation and reduce dizziness episodes.
When should I see a doctor for low blood pressure dizziness after COVID?
Seek immediate medical attention if dizziness is accompanied by chest pain, prolonged unconsciousness, or sudden severe headaches. Otherwise, consult a healthcare provider if symptoms persist or worsen despite lifestyle adjustments.
Can medications help with post-COVID low blood pressure dizziness?
In persistent cases, doctors may prescribe medications like fludrocortisone to boost blood volume or midodrine to narrow blood vessels. Beta-blockers may be used if heart rate is excessively fast. Medication should be managed by a specialist.