Understanding COVID Dysautonomia
How does COVID trigger dysautonomia?
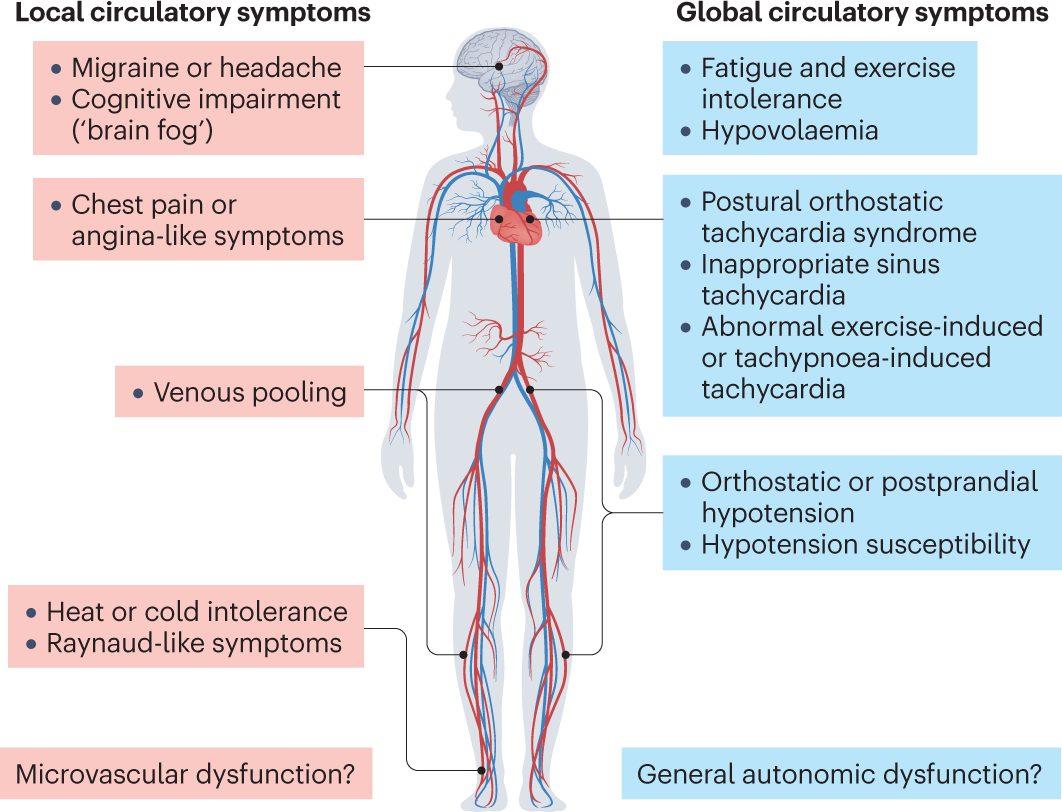
COVID19 can inflame the vagus nerve and other parts of the autonomic nervous system, throwing off the balance that normally keeps your heart rate, blood pressure, and digestion in sync. A review in explains that lingering inflammation and autoimmune reactions are the main culprits.
Is it the same as POTS?
Postural Orthostatic Tachycardia Syndrome (POTS) is one form of dysautonomia that shows up a lot after COVID, but not every case fits the textbook POTS definition. notes that many patients have overlapping symptomsrapid heart rate, dizziness, and fatigueyet their test results can differ.
| Feature | POTS | Other COVIDRelated Dysautonomia |
|---|---|---|
| Heartrate rise on standing | 30 BPM (40 BPM if under 19) | Variable, sometimes <30 BPM |
| Blood pressure drop | Often normal | Can be low, leading to fainting |
| Duration | Monthstoyears | Often improves within 612 months |
| Treatment response | Betablockers, fludrocortisone | Similar meds + lifestyle tweaks |
Spotting Common Symptoms
Top warning signs you shouldnt ignore
Everyones experience is a little different, but these symptoms show up again and again on Reddit threads and in clinical reports:
- Racing or irregular heartbeat (palpitations)
- Lightheadedness or feeling like you might faint when you stand
- Shortness of breath that isnt explained by lung issues
- Unexplained chronic fatigue
- Sudden changes in temperature perception (feeling hot or cold)
- Digestive ups and downs, such as nausea or diarrhea
Can symptoms appear weeks or months later?
Absolutely. Postviral dysautonomia can linger silently and then flare up weeks after the initial infection. A study of 1,200 longCOVID patients found that 22% reported new autonomic symptoms emerging after a threeweek quiet period.
Red flags when to call emergency services
If you ever experience chest pain, severe shortness of breath, sudden loss of consciousness, or a rapid heart rate over 130BPM at rest, treat it as an emergency. These could signal a cardiac issue rather than isolated dysautonomia.
Recovery Timeline Overview
Typical recovery milestones
Most folks notice improvement within the first three months, but the road can be bumpy:
- Weeks14: Symptoms may peak; rest and hydration are crucial.
- Months23: Light activity and gentle tilttraining often start reducing dizziness.
- Months46: Many patients report a 3050% drop in symptom severity.
- Beyond 6months: A smaller group continues to have lingering issues and may need specialist care.
Factors that influence how long it lasts
Age, severity of the original COVID infection, preexisting health conditions, and whether you were vaccinated before falling ill all play a role. For instance, several Reddit users noted that those who received a booster before getting COVID seemed to bounce back a bit quicker.
Can it become permanent?
While most improve with proper care, a minority experience chronic dysautonomia that persists for years. Ongoing research, such as the objective functional outcomes study in , suggests that early intervention improves longterm odds.
Doctor Diagnosis Guide
Key tests doctors use
When you walk into a clinic with these symptoms, a physician will likely order:
- Tilttable test to see how your blood pressure and heart rate react to standing.
- 24hour Holter monitor tracks heart rhythm over a full day.
- Autonomic function panel measures sweat, heart rate variability, and more.
- Blood work looks for markers of inflammation or autoimmunity.
When to ask for a specialist referral
If basic tests are inconclusive but you still feel off, consider asking for a referral to a neurologist or cardiologist who specializes in autonomic disorders. They can run more detailed tests, such as quantitative sudomotor axon reflex testing (QSART).
Managing Dysautonomia Effectively
Medical treatment options
Doctors often start with lowdose medications to steady your autonomic system:
| Medication | Purpose | Typical Dose | Common Sideeffects |
|---|---|---|---|
| Betablockers (e.g., propranolol) | Reduce heartrate spikes | 1040mg daily | Fatigue, cold hands |
| Fludrocortisone | Increase blood volume | 0.1mg daily | Swelling, high blood pressure |
| Ivabradine | Slow heart rate without affecting blood pressure | 57.5mg twice daily | Visual disturbances |
Lifestyle tweaks that make a difference
Small daily habits can shift the balance dramatically:
- Hydration & salt: Aim for 23L of water and 35g of extra salt (unless you have kidney issues).
- Compression garments: Kneehigh stockings help keep blood from pooling in your legs.
- Gradual upright training: Start with a few minutes of standing, then slowly increase the time each day.
- Sleep hygiene: Keep a consistent bedtime and consider a slightly elevated head of the bed.
Sample 4week homerehab plan
Feel free to adapt this to your own schedule:
- Week1: Focus on hydration and gentle stretching while seated.
- Week2: Add 5minute standing intervals three times a day.
- Week3: Increase standing time to 1015minutes, introduce light walking.
- Week4: Aim for 2030minutes of lowintensity activity (walking, swimming).
Complementary approaches
While evidence is still emerging, many people on longCOVID Reddit forums swear by breathing exercises, mindfulness meditation, and gentle yoga for reducing anxiety and stabilizing heart rate. Just keep expectations realistic and discuss any new practice with your physician.
Risks and Benefits
Potential upside of early treatment
Getting help sooner often translates to faster symptom relief, fewer days off work, and a reduced chance of developing a chronic autonomic disorder.
Possible downsides to watch for
Medication sideeffects, overexertion during rehab, and the emotional toll of chronic illness are real concerns. Thats why a balanced, personalized planone that weighs benefits against risksis essential.
Decisionmaking checklist
- Do I understand the medications purpose and sideeffects?
- Am I comfortable with the lifestyle changes required?
- Do I have a support system (family, friends, online community) to keep me accountable?
- Is my doctor monitoring progress and adjusting the plan as needed?
FAQ Quick Answers
What is dysautonomia after COVID?
Its a disturbance of the autonomic nervous system that emerges after a COVID infection, causing irregular heart rate, blood pressure issues, and other outofcontrol bodily functions.
Can dysautonomia after COVID go away?
For most people, symptoms improve within 36months, especially with proper treatment. A small group may need longerterm management.
Is POTS a form of postCOVID dysautonomia?
Yes, POTS is a common subtype, but not every postCOVID case fits the strict POTS criteria.
How do I know if I have dysautonomia after COVID?
If you experience persistent rapid heartbeat, dizziness when standing, unexplained fatigue, or trouble breathing without lung disease, its worth getting evaluated. For help navigating insurance and assistance programs for rare or expensive therapies that might overlap with autonomic care, resources on Exondys 51 assistance can illustrate how patient support programs workuseful background when discussing coverage for offlabel or specialty treatments.
Does the COVID19 vaccine cause dysautonomia?
Current research shows no direct causal link. However, some people report temporary autonomic symptoms after vaccination, which generally resolve quickly.
Community Voices Insight
What Reddit users are saying
On the r/LongCovid subreddit, a thread titled Living with PostCOVID POTS gathered over 2,000 comments. Many shared that consistent salt intake and compression socks shaved hours off their daily fatigue.
Tips that the community swears by
- Keeping a symptom diary to spot patterns.
- Using an elevated pillow to reduce nighttime blood pressure drops.
- Joining virtual support groups for accountability.
Helpful Resources Guide
Professional organizations
Look to the and the for uptodate guidelines and research summaries.
Support groups & hotlines
Many hospitals now host postCOVID clinics with multidisciplinary teams. Online platforms like the Long COVID Support Group on Facebook also provide a safe space to share experiences.
Quick links youll want to bookmark
- Symptom checklist PDF (downloadable from the articles sidebar).
- 4week rehab plan printable.
- Medication comparison table for easy reference.
Remember, youre not alone in this. Dysautonomia after COVID can feel overwhelming, but with the right information, a supportive community, and a personalized care plan, you can navigate the ups and downs. If you have questions, share them in the comments below or reach out to a healthcare professional. Were all in this together.
FAQs
What are the most common symptoms of dysautonomia after COVID?
Typical signs include rapid heartbeat, dizziness on standing, unexplained fatigue, shortness of breath, temperature intolerance, and digestive issues.
How long does post‑COVID dysautonomia usually last?
Most people improve within 3‑6 months, though some recover faster and a minority may experience symptoms for a year or longer.
Can dysautonomia after COVID be treated with medication?
Yes, doctors often prescribe low‑dose beta‑blockers, fludrocortisone, or ivabradine, combined with lifestyle changes like increased hydration and salt.
What lifestyle adjustments help manage dysautonomia?
Staying well‑hydrated, adding extra dietary salt, wearing compression stockings, gradual upright training, and maintaining good sleep hygiene are key strategies.
When should I seek emergency care for dysautonomia symptoms?
If you experience chest pain, sudden loss of consciousness, severe shortness of breath, or a resting heart rate over 130 BPM, call emergency services immediately.